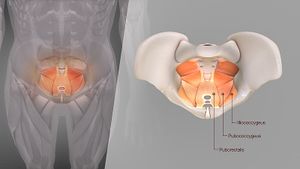
Genitourinary Syndrome
Top Contributors - Khloud Shreif, Temitope Olowoyeye and Lucinda hampton
Introduction[edit | edit source]
Genitourinary syndrome of menopause GSM a new alternative terminology for vulvovaginal atrophy was first introduced in 2014 by consensus between the International Society for the Study of Women’s Sexual Health and the North American Menopause Society, it is a chronic condition that affects women after menopause[1].
It is a chronic progressive condition that describes the changes resulting from the decrease in estrogen level[2] after menopause on the vulvovaginal and lower urinary tract. The majority of women may be affected after menopause but about 15%of women may have symptoms pre-menopause, and many women consider it a normal process with the aging process and they do not seek help or consider it a condition that needs help so it remains underdiagnosed and they need medical awareness of their conditions[3]. GSM symptoms might progress over time if left untreated.
Pathophysiology[edit | edit source]
The vagina, vestibule, urethra, and trigone of the bladder contain receptors a and b for estrogen. However, both receptors can be found in premenopausal women but during menopause, only b receptors can be found. So the level of estrogen in the urogenital tract will be decreased and will affect the contractility and elasticity of organs. The stratified squamous vaginal epithelium is estrogen-responsive, there will be changes in the vaginal epithelium thickness, blood flow, atrophy of smooth cells of the vagina, loss of tissue elasticity, and the vaginal mucosa will be fragile and pallor. The labia minora consists of elastic fibers, dense connective tissue, and erectile tissue, there will be a loss in the size of the labia minora, a decrease in the subcutaneous fat of labia majora, reduction in pubic hair, addition, there will be a change in the microbial environment of the vagina and an increase in vaginal PH[4][5].
That causes trauma and irritation during sex. Plus changes at the level of the genital system the contractile ability of the ureteral sphincter, and contractile coordination of pelvic floor muscle will be decreased[4][5].
Clinical Presentation[edit | edit source]
More than 45% of postmenopausal women report some types of GSM, those with dryness and painful intercourse are the most common[4]. In about 50% of post-menopausal women, the manifestations are mild and nonspecific and all GSM symptoms don't need to occur. Irritation, burning, and itching of the vulva or vagina are common symptoms of GSM, and they are reported in 63.3% of women with GSM[6]. Symptoms of GSM appear to have a greater impact on the quality of life (QOL) especially in sexually active women, confidence, and intimacy with their partner. Other signs and symptoms include:
- Vaginal dryness.[2]
- Dyspareunia (20% to 59%).
- Decrease or loss of arousal, orgasm, or desire.
- Vaginal vault prolapse.
- Post-coital bleeding.
- Incontinence (stress or urge).
- Recurrent urinary tract infection UTI (8%-11%)[4].
- Dysuria (7%- 13%).
- Urethral prolapse.[2][3][5]
- Idiopathic overactive bladder.
- Interstitial cystitis[4][3].
Diagnostic Procedures[edit | edit source]
There are no specific or necessary diagnostic procedures to diagnose GSM and it depends on the exclusion of other causes with similar symptoms such as chronic pelvic pain, vulvodynia, or dermatological conditions, but the measurement of vaginal pH,[2] and assessment of vaginal maturation index (VMI)[2] by taking a vaginal smear there will be an increase in parabasal cells and reduction in superficial cells are the most objective evaluation methods for GSM[1].
Outcome Measures[edit | edit source]
Vulvovaginal Symptoms Questionnaire.
Day-to-Day Impact of Vaginal Aging (DIVA) Questionnaire[7].
Management / Interventions[edit | edit source]
The management of the genitourinary syndrome of menopause will depend on symptomatic relief and it is important first to exclude any other possible causes especially if there is vaginal bleeding it will be important to exclude cancer.
Medical management[edit | edit source]
Non-hormonal therapy:
- Vaginal lubricants
- Vaginal moisturizers
- Oral ospemifene (Selective Estrogen Receptor Modulator (SERM).
- A small dose of DHEA intravaginally (prasterone)[9].
Hormonal therapy:
- Estrogen it will be delivered in two forms;
Systemic delivered oral, transdermal (patch or gel), or subcutaneous.
Vaginal systemically delivered estrogen with a low dose has a beneficial effect on the genital tissues[1][10].
Physical Therapy Management[edit | edit source]
Laser therapy
Its mechanism depends on the absorption of waves by the lamina propria of the vagina which is made mainly of water, the absorbed energy allows the affected tissues to be covered by another healthy one (proliferation) that will prevent pain, and help in rapid recovery this stage lasts for about 30 days. This absorbed and transmitted heat to water will help to stimulate collagen-producing fibroblasts (remodeling) and it lasts for 30–40 days. However, although it is effective for women with GSM low data is supporting its long-term efficacy. any laser device with FDA approval can be used. the recommended sessions from previous studies for micro ablative fractional carbon dioxide (CO2) laser, are usually used for three sessions at five- to six-week intervals, but sessions can be up to 5 sessions for more benefits[11][9]. A recent prospective cohort study found it was effective for treating symptoms associated with GSM; vaginal burning, dryness, and dyspareunia, and these improvements last for 6-12 months after treatment[12].
Radiofrequency
Pelvic Floor Muscle Training (PFMT)
There are recent studies about the effect of PFMT on GSM symptoms in case other options for treatment can not be available. In this study by Mercier in 2019 an intensive PFMT program, divided into three phases to help with gradual progression was used[13], the session was for 1 hour/ week and they had to do a home exercise program 5 times/ week. It was conducted for 12 weeks, After the termination of the study the outcomes showed PFMT can be effective for symptoms with GSM and UI[14]. In 2020, Mercier published a study on the mechanism of action of PFMT on symptoms of GSM. In this study color Doppler ultrasound was used to measure the pulsatility index of the internal pudendal and dorsal clitoral arteries before and after the pelvic floor muscle (PFM) contraction task, a dynamometer was used to assess PFM function, and a Vaginal Atrophy Index for assessment of vaginal elasticity all was measure before and after termination. At the end of the study, there was an improvement in the parameters of blood flow in both arteries, an improvement in PFM contraction, a decrease in the tone of muscles in addition to improvement in skin elasticity[15].
Differential Diagnosis[edit | edit source]
Dermatological conditions related to the vulva; vaginitis, lichen sclerosis, chronic vulvovaginitis, or eczema.
Vulvodynia
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Briggs P. Genitourinary syndrome of menopause. Post reproductive health. 2020 Jun;26(2):111-4.
- ↑ 2.0 2.1 2.2 2.3 2.4 Sarmento AC, Costa AP, Vieira-Baptista P, Giraldo PC, Eleutério Jr J, Gonçalves AK. Genitourinary syndrome of menopause: epidemiology, physiopathology, clinical manifestation and diagnostic. Frontiers in Reproductive Health. 2021 Nov 15;3:779398.
- ↑ 3.0 3.1 3.2 Angelou K, Grigoriadis T, Diakosavvas M, Zacharakis D, Athanasiou S. The genitourinary syndrome of menopause: an overview of the recent data. Cureus. 2020 Apr 8;12(4).
- ↑ 4.0 4.1 4.2 4.3 4.4 Mitchell CM, Waetjen LE. Genitourinary changes with aging. Obstetrics and Gynecology Clinics. 2018 Dec 1;45(4):737-50.
- ↑ 5.0 5.1 5.2 Faubion SS, Sood R, Kapoor E. Genitourinary syndrome of menopause: management strategies for the clinician. InMayo Clinic Proceedings 2017 Dec 1 (Vol. 92, No. 12, pp. 1842-1849). Elsevier.
- ↑ Moral, E., Delgado, J.L., Carmona, F., Caballero, B., Guillán, C., González, P.M., Suárez-Almarza, J., Velasco-Ortega, S., Nieto, C. and writing group of the GENISSE study, 2018. Genitourinary syndrome of menopause. Prevalence and quality of life in Spanish postmenopausal women. The GENISSE study. Climacteric, 21(2), pp.167-173.
- ↑ Huang AJ, Gregorich SE, Kuppermann M, Nakagawa S, Van Den Eeden SK, Brown JS, Richter HE, Walter LC, Thom D, Stewart AL. The day-to-day impact of vaginal aging questionnaire: A multidimensional measure of the impact of vaginal symptoms on functioning and well-being in postmenopausal women. Menopause (New York, NY). 2015 Feb;22(2):144.
- ↑ Mayo Clinic. Dr. Stephanie Faubion - Genitourinary syndrome of menopause. . Available from: http://www.youtube.com/watch?v=4c7F9Bv5pw4 [last accessed 28/10/2022]
- ↑ 9.0 9.1 Palacios S, Combalia J, Emsellem C, Gaslain Y, Khorsandi D. Therapies for the management of the genitourinary syndrome of menopause. Post Reproductive Health. 2020 Mar;26(1):32-42.
- ↑ Kim HK, Kang SY, Chung YJ, Kim JH, Kim MR. The recent review of the genitourinary syndrome of menopause. Journal of menopausal medicine. 2015 Aug 1;21(2):65-71.
- ↑ Athanasiou S, Pitsouni E, Falagas ME, Salvatore S, Grigoriadis T. CO2-laser for the genitourinary syndrome of menopause. How many laser sessions? Maturitas. 2017 Oct 1;104:24-8.
- ↑ Li J, Li H, Zhou Y, Xie M, Miao Y, Wang L, Zhao Y, Ying T, Hu Y, Chen Y, Chen Y. The fractional CO2 laser for the treatment of genitourinary syndrome of menopause: A prospective multicenter cohort study. Lasers in Surgery and Medicine. 2021 Jul;53(5):647-53.
- ↑ Dumoulin C, Morin M, Mayrand MH, Tousignant M, Abrahamowicz M. Group physiotherapy compared to individual physiotherapy to treat urinary incontinence in aging women: study protocol for a randomized controlled trial. Trials. 2017 Dec;18(1):1-4.
- ↑ Mercier J, Morin M, Zaki D, Reichetzer B, Lemieux MC, Khalifé S, Dumoulin C. Pelvic floor muscle training as a treatment for genitourinary syndrome of menopause: A single-arm feasibility study. Maturitas. 2019 Jul 1;125:57-62.
- ↑ Mercier J, Morin M, Tang A, Reichetzer B, Lemieux MC, Samir K, Zaki D, Gougeon F, Dumoulin C. Pelvic floor muscle training: mechanisms of action for the improvement of genitourinary syndrome of menopause. Climacteric. 2020 Sep 2;23(5):468-73.