The Calgary-Cambridge Guide to the Medical Interview - Gathering Information on the Biomedical History
Introduction[edit | edit source]
Information gathering involves the collection of clinically relevant facts and history, in combination with the exploration of patient experience, concerns and ideas regarding their condition [1]. It is therefore important to follow a biopsychosocial approach throughout the medical interview: different patients may have similar sets of biomedical information, but each individual clinical presentation will be greatly influenced by the psychosocial background of the patient [2][3][4]. The aim of information gathering is to gain enough clinical data to be able to form a hypothesis of potential cause of symptoms, and to test the hypothesis to reach a diagnosis [5]. In this document, the gathering of biomedical information will be investigated, underpinned by a functional and psychosocial consideration. Clinical reasoning and hypothesis generation as a product of information gathered during the medical interview, will firstly be discussed.
| "Taking a patient history is like playing detective, ‘searching for clues, collecting information without bias, yet staying on track to solve the puzzle"[1]. |
|---|
Clinical Reasoning and Hypothesis Generation[edit | edit source]
Clinical reasoning is defined as a process of analyzing acquired clinical data in combination with patient preferences, professional judgement, and scientific knowledge, with the goal of structuring meaning, developing objectives, and implementing health management strategies in the management of a patient[5][6]. According to the research findings[5], clinical reasoning in physical therapy is conceptualized as integrating cognitive, psychomotor and affective skills. It is contextual in nature and involves both therapist and client perspectives. It is adaptive, iterative and collaborative with the intended outcome being a biopsychosocial approach to patient/client management.
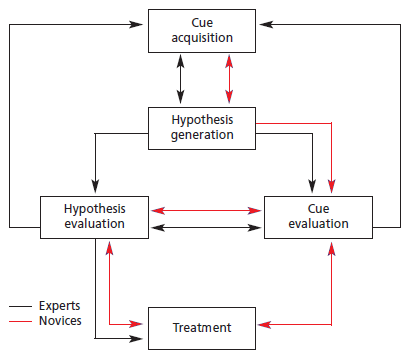
A sound hypothesis depends on good quality clinical reasoning, using as much as possible clinically relevant information gained during the patient interview[7]. Physiotherapists often apply clinical reasoning to arrive at a working hypothesis by utilizing either a hypothetico-deductive model, or pattern recognition, or a combination of the two [8].
In a hypothetico-deductive model, hypotheses are generated from all observations, after which clinical data gained is tested to arrive at the most likely hypothesis. Pattern recognition is generally used by more experienced physiotherapists. It refers to the formation of a hypothesis from typical symptom and disease presentations noted, and subsequent data exploration to confirm or negate the hypotheses[6].
The use of the International Classification of Function and Disability and Health model (ICF) can help the physiotherapist to better understand the context of the presenting patient during the process of clinical reasoning and hypothesis generation. It aids to organize information in a practical and logical manner, while also integrating environmental, social, and psychological factors in the understanding of the person and condition[6]. Furthermore, the use of the ICF as an outcome measure allows for the standardization of patient impairment and provides a concrete, comparable benchmark by which to measure the effect of management.
The International Classification of Function, Disability and Health (ICF)[edit | edit source]
The ICF is a classification system that describes the different components of the functioning of a person with any health condition. It was approved by the World Health Organization (WHO) in 2001, as a universally accepted conceptual model and taxonomy of human functioning[7].
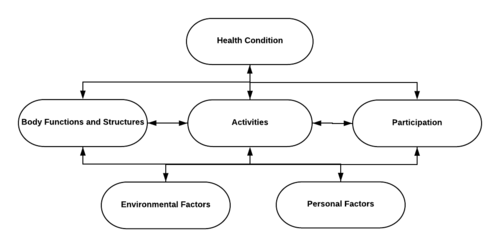
The ICF describes human functioning as an interaction between body functions and structures, activities, and participation, together with the effect of psychological and environmental influences (Figure 1). The model is built on biopsychosocial principles which regard the patient as a holistic, psychological being within a specific environment. Disability is described according to impairment of body functions/structure, limitations in activities, and restrictions in participation[9]. A systematic review[10] shows that biopsychosocial interventions with a clear focus on psychosocial factors (understanding pain, unhelpful thoughts, coping styles, and goal setting) seemed more effective than education/advice and were found to be as effective as physical activity interventions in patients with chronic low back pain. Physiotherapists need sufficient training and resources (manual, supervision, and informative resources) to provide a cognitive‐behavioral intervention effectively.[10]
Body functioning and structures refers to physiological processes and anatomic structures, and any abnormality of these is referred to as an impairment.
Activity refers to the execution of tasks or actions and represents the individual’s perception of function. The inability to perform normal activities is referred to as limitations.
Participation refers to life situations in which an individual is actively involved. The inability to engage in normal participation is called participation restrictions.
Environmental and personal factors are collectively known as contextual factors and refer to the influence of surroundings, psychology, and experience of illness on the patient’s health[11].
From a biopsychosocial point of view, the ICF is a model for standardization of function and health which allows for comparison across the spectrum of disability. The inclusion of contextual factors provides a patient-specific representation of function which illustrates why different individuals may be differently affected by a seemingly similar pathology. For example, one patient may walk on a fractured metatarsal for days before having it diagnosed, whereas another patient, with similar biomedical factors and a similar injury, may be in much more distress following the injury. Differences in contextual factors may also influence the recovery and behavior of the individual[11].
Although physiotherapists often successfully treat patients who reach full recovery, we should remember that many conditions are chronic and progressive in nature and that some patients will never be completely asymptomatic, for example, individuals with Parkinson's or cystic fibrosis. Therefore, the focus should be on rehabilitation as a process to help patients reach their optimal physical, psychological, social, occupational and educational potential within the anatomical and physiological capacity available[12]. The ICF aids rehabilitation professionals to gauge the functional capacity of a patient, analyze the source of restrictions and limitations, and compile a realistic management plan accordingly[7].
The consideration of the ICF in the medical interview helps rehabilitation professionals to understand the impact of a health condition on the patient’s functionality and well-being. Emphasis is placed on the functional limitation due to presenting symptoms, instead of only focusing on the specific presentation and behavior of symptoms. Proper comprehension of the bigger context of ill-health will also assist the therapist in realistic goal-setting and provide a better understanding of the patient as a person, as well as his/her experience of the condition and the potential role this experience can play in symptom presentation and/or recovery. Knowledge of a patient’s functional impairment will furthermore assist the physiotherapist to select assessment techniques based on symptom-eliciting functional movements. For this reason, it is strongly recommended that the process of information gathering should be based on the patient’s current functional capacity and the potential effect of the presenting condition/symptoms[13].
Gathering the Biomedical Information[edit | edit source]
The process of investigating biomedical history is highly dependent upon the subspecialty of medicine/allied health involved[14], however, the basic principles remain the same across the spectrum. Some of these factors will be discussed in more detail and include the behavior of the symptoms, red flags, the medical history and a review of other relevant systems [1].
Red flags[edit | edit source]
Red flags are any signs or symptoms that may indicate a possible serious underlying condition that warrants further medical assessment and/or intervention[15] before continuing with the therapeutic management [16]. Although the concept of red flags covers all areas of medicine, specific subspecialties need to assess specific red flags relevant to their field. For example, musculoskeletal physiotherapists treating a lumber condition should clear any signs of cauda equina syndrome and spinal stenosis, and for upper cervical pain/headache and vertigo, vertebrobasilar insufficiency and cervical spine instability should be excluded.
When screening for red flags, is it suggested for the therapist to inform the patient that the relevant questions are only asked to ensure that no potential underlying pathologies are missed. Also, confirm that the prevalence of red flags is mostly low in the general population. This will put potentially catastrophizing patients at ease and prevent unnecessary anxiety regarding questions that may seem irrelevant to the condition. When red flags are indeed identified, share your findings with the patient in a logical manner using easily understandable language, and explain that referral to a specialist is necessary to exclude underlying pathology before continuing with therapy[7].
Behavior of Symptoms[edit | edit source]
A good place to start when taking history is to explore what is the most concerning problem of the patient. A patient-centered approach investigates the patients’ ideas and concerns about their symptoms and their expectations[17]. The majority of patients will not show how anxious they are about their condition thus it's important to ask about what they think regarding their symptoms to get an understanding of their worries and include that in the discussion.
Very often, basic information on symptom behavior is already provided in the initiation of the session and should now be elaborated upon and investigated deeper if necessary. The mnemonic PQRST[18] is a framework developed to be used in information gathering. It can be used to remember five aspects of symptom behavior to be investigated: Palliation/provocation, quality, region/radiation, severity and timing[1]
- Palliation/provocation refers to any factors that may exacerbate/aggravate or improve symptoms. As discussed, an investigation into the patient’s functional limitations due to the presenting symptoms, specifically relating to participation restrictions or activity limitations, usually provide valuable information. Ask about specific movements or positions that may aggravate or alleviate symptoms. Patients may also relate their emotional state to their physical symptoms: allostatic overload (cumulative effect of frequent stressful situations in everyday life) can have a significant adverse effect on physical health [19][13].
- Quality of symptoms, also called the nature of the symptoms, involves the patient's perception of the presenting symptoms which could give clues on the etiology of the presenting condition[1]. Example of questions: “what type of pain is it?” or “Is it a sharp pain, or burning? Or a dull ache?” or “Would you say your cough is dry or wet? Maybe wheezy, or barking?”)[7].
- Region/Radiation refers to the physical area where symptoms are experienced[1]. The use of a body chart is recommended to indicate the region of symptom presentation. A body chart aids to conceptualize symptoms and assists the therapist to recognize potential patterns that may be specific to certain conditions. It is suggested to ask the patient to indicate the area of symptom experience on his/her body by showing with the hand, after which the physiotherapist plots the area on the body chart, and confirms with the patient whether the correct area is indicated. All areas where symptoms are experienced should be charted and the patient should confirm whether any relationship exists between the different areas in terms of the behavior of the symptoms.
- Severity reflects the intensity of symptoms[1]. Severity should be as concrete as possible, using a numeric value or a standardized score. A well-known example is that of the numeric pain scale where a patient indicates the severity of pain on a scale from 0 to 10 (where 0 is no pain and 10 is excruciating and decapacitating) or the Visual Analogue Scale (VAS) where the patient indicates his level of pain on a line. Depending on the presenting condition, different subjective outcome measures can be used to measure severity: the severity of upper limb dysfunction can for instance be determined by the Disability of Arm, Shoulder and Hand (DASH) questionnaire, or the Dizziness Handicap Inventory (DHI) can be used to express the severity of the experienced dizziness. Patients should be informed that severity is specific and standardized to each patient and is often used as a comparable sign to indicate potential improvement or regression of the condition. In this way, individual variables such as pain threshold are accommodated.
- Timing includes three concepts: Firstly, a timeline from onset to the current presentation should be established, including further exploration of mechanisms, and any regression/progression of the condition since onset. Secondly, enquire about any 24-hour pattern noted (for example, worse at night, or stiffness and pain first thing in the morning). Thirdly, investigate the frequency of symptoms (i.e. intermittent or constant awareness) and whether this has changed since the onset of symptoms[1]. Information on timing assists the therapist to assess etiology, chronicity and/or phase of recovery.
Current Medical History[edit | edit source]
The prevalence of chronic conditions and chronic medication use should be assessed also taking into consideration the duration of the use of chronic medication while considering any co-incidence in symptom timing and medication use, which may indicate that symptoms can possibly be linked to medication [1]. Remain objective, sensitive, and respectful at all times – patients often feel ashamed or stigmatized for certain conditions or medicinal uses. It is also necessary to enquire about habitual substance consumption, such as the use of tobacco, alcohol or marijuana or other narcotics. Create a safe, non-judgmental space when assessing these, since patients are often reluctant to share this type of information with health-care professionals [7]. When the patient seems reluctant, explain that prolonged substance use can influence the healing process, which is why it needs to be taken into account. Even though it is the task of healthcare professionals to educate patients regarding the use of adverse substances, this should rather be incorporated into the management plan than addressing the issue during the interview. Also, ask about regular exercise and note the activity and frequency. Furthermore, enquire about diet, sleep habits, as well as any other preventative medicine used [1].
Previous Medical History[edit | edit source]
Enquire about any physical trauma, hospitalization or injuries throughout the patient’s lifetime, even though the patient may not consider such history as relevant to the presenting condition. Ask about any previous treatment by another medical or rehabilitation professional, and what the patient was treated for[7].
Family History[edit | edit source]
Like with red flags, explain to the patient that an investigation into family history is done routinely and to exclude the possibility of any link to genetic or hereditary diseases. Conditions to look out for include cardiovascular disease, diabetes, chronic respiratory conditions, cancer, and bone diseases. Literature suggests that clinicians should consider the family history of the previous two generations [1]. When hereditary diseases are noted, consider providing some counselling in terms of preventative screening to be performed by a relevant health care practitioner.
Review of the Systems[edit | edit source]
In an ideal world, a complete head-to-toe check-up gives a comprehensive image of the patient's condition, however, this process wouldn't be appropriate for most clinical settings with limited time. The clinician should apply good judgement and clinical reasoning to decide which system review to include in the assessment. For example, for a patient with neck pain, an investigation into possible eye problems will be sensible, but assessing for sexual health disorders will be inappropriate.
Table 1 provides a summary of additional somatic systems to consider in the assessment. It is important to explain to the patients why other systems are investigated to prevent unnecessary anxiety[1].
Table 1: Review of the Systems (adapted from Kaufman [1])
| SYSTEM | FACTORS TO CONSIDER |
|---|---|
| Head | Dizziness, headaches, faintness, recent head injury |
| Eyes | Any changes in vision, regular optometric tests |
| Respiratory | Breathing problems, coughing, wheezing, sputum production, allergic rhinitis, chronic sinusitis, earache hearing loss |
| Cardiac | Anemia, hypertension, palpitations |
| Gastrointestinal | Heartburn, irritable bowel syndrome, nausea, changes in regular toileting routine |
| Urogenital/gynaecological | Pain with urination, menstruation-related symptoms, changes in regular toileting routine |
| Muskuloskeletal | Stiffness, cramps, weakness, swelling |
| Neurological | Numbness, tingling, tremors, weakness, coordination, balance |
Conclusion[edit | edit source]
The gaining of biomedical information is regarded as the core of the medical assessment process by many. Although the information gathered is imperative for the formation of a sound hypothesis, the clinical significance of psychosocial factors should not be overlooked. It is recommended to follow a function-based approach in the investigation of biomedical information in order to ensure patient-centered care. Throughout the gaining of information, dynamic clinical reasoning is necessary to develop relevant hypotheses, select the appropriate assessment techniques, formulate a sound diagnosis and ensure a comprehensive and applicable management plan.
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 Kaufman G. Patient assessment: effective consultation and history taking. Nursing Standard. 2008 Oct 1;23(4).
- ↑ Bevers K, Watts L, Kishino ND, Gatchel RJ. The biopsychosocial model of the assessment, prevention, and treatment of chronic pain. US Neurol. 2016 Jan 1;12(2):98-104. DOI:10.17925/USN.2016.12.02.98
- ↑ Parker R, Madden VJ. State of the art: What have the pain sciences brought to physiotherapy?. The South African journal of physiotherapy. 2020;76(1). DOI:10.4102/sajp.v76i1.1390
- ↑ Bolton D, Gillett G. The biopsychosocial model of health and disease: New philosophical and scientific developments. Springer Nature; 2019. DOI:10.1007/978-3-030-11899-0
- ↑ 5.0 5.1 5.2 Huhn K, Gilliland SJ, Black LL, Wainwright SF, Christensen N. Clinical reasoning in physical therapy: a concept analysis. Physical therapy. 2019 Apr 1;99(4):440-56.
- ↑ 6.0 6.1 6.2 Jones M, Edwards I, Gifford L. Conceptual models for implementing biopsychosocial theory in clinical practice. Manual therapy. 2002 Feb 1;7(1):2-9.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 Fourie M. Gathering Information - Underpinning Biomedical History. Plus Course 2020
- ↑ Croskerry P. A model for clinical decision-making in medicine. Medical Science Educator. 2017 Dec 1;27(1):9-13. DOI: 10.1007/s40670-017-0499-9
- ↑ Stucki G, Cieza A, Melvin J. The international classification of functioning, disability and health: A unifying model for the conceptual description of the rehabilitation strategy. Journal of rehabilitation medicine. 2007 May 5;39(4):279-85.
- ↑ 10.0 10.1 van Erp RM, Huijnen IP, Jakobs ML, Kleijnen J, Smeets RJ. Effectiveness of primary care interventions using a biopsychosocial approach in chronic low back pain: a systematic review. Pain Practice. 2019 Feb;19(2):224-41.
- ↑ 11.0 11.1 Johnston M, Dixon D. Developing an integrated biomedical and behavioural theory of functioning and disability: adding models of behaviour to the ICF framework. Health psychology review. 2014 Oct 2;8(4):381-403.
- ↑ Heerkens Y, Hendriks E, Oostendorp R. Assessment instruments and the ICF in rehabilitation and physiotherapy. Medical Rehabilitation. 2006;10(3):1-4.
- ↑ 13.0 13.1 Fava GA, McEwen BS, Guidi J, Gostoli S, Offidani E, Sonino N. Clinical characterization of allostatic overload. Psychoneuroendocrinology. 2019 Oct 1;108:94-101.
- ↑ Johnson P. Assessment and clinical reasoning in the Bobath concept. Bobath Concept. 2009 Jul 3:43.
- ↑ Briggs AM, Fary RE, Slater H, Ranelli S, Chan M. Physiotherapy co-management of rheumatoid arthritis: Identification of red flags, significance to clinical practice and management pathways. Manual therapy. 2013 Dec 1;18(6):583-7.
- ↑ Yusuf M, Finucane L, Selfe J. Red flags for the early detection of spinal infection in back pain patients. BMC musculoskeletal disorders. 2019 Dec;20(1):1-0. DOI:10.1186/s12891-019-2949-6
- ↑ Moulton L. The naked consultation: A practical guide to primary care consultation skills. CRC Press; 2017 Jul 14.
- ↑ Estes ME. Health assessment and physical examination. Cengage Learning; 2013 Feb 25.
- ↑ Butler RK, Finn DP. Stress-induced analgesia. Progress in neurobiology. 2009 Jul 1;88(3):184-202.