Foot drop
Original Editor - Abbey Wright
Top Contributors - Abbey Wright, Lokiru Paul, Kim Jackson, Admin and Lucinda hampton
Introduction[edit | edit source]
Foot drop also known as drop foot is not a disease, but rather a commonly encountered symptom of a neurological, anatomical, or muscular problem. Foot drop is inability to lift the forefoot due to the weakness of dorsiflexors of the foot.[1] Ankle and foot dorsiflexors, namely the tibialis anterior, extensor digitorum longus, and extensor hallucis longus, help clear the foot during the swing phase of walking and control plantar flexion of the foot on heel strike.[2] Weakness in the ankle and foot dorsiflexors results in an equinovarus deformity. Sometimes referred to as steppage gait, which is a tendency of a person walking with an exaggerated flexion of the hip and knee to prevent the toes from catching on the ground during swing phase. Foot drop can therefore hinder walking and increase the risk of tripping and falling. [3]
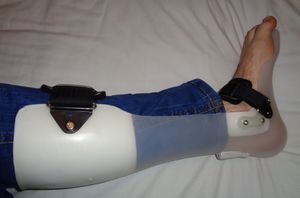
Image to R shows common brace (AFO) for foot drop.
Clinically Relevant Anatomy[edit | edit source]
The common peroneal nerve is the smaller and terminal branch of the sciatic nerve which is composed of the posterior divisions of L4, 5, S1, 2. The nerve can be palpated behind the head of the fibula and as it winds around the neck of the fibula.[4]
Commonly, with damage to the common peroneal nerve, there will be weakness of tibialis anterior and other key dorsiflexors of the foot.
Etiology[edit | edit source]
Lesion site localization of foot drop can be challenging because it may be a presentation of a range of pathologic conditions that localize along the full course of upper and lower motor neuron pathways which often overlap in clinical presentation.[5][6] The Mechanism of injury can be divided into three groups.
1. Compression disorders: Entrapment syndromes of the fibular nerve at various locations along its anatomical pathway can lead to compressive neuropathy. The common fibular neuropathy at the fibular head is the most common mononeuropathy affecting the leg.[7] The fibular nerve being so superficial near the head of the fibula, makes it vulnerable to pressure palsies. Weight loss, prolonged bedridden status, tight casts, space-occupying lesions, and bone metastasis involving the fibular head can be other contributing factors. Compression of the fibula head during surgery e.g. tourniquet[8]
Sciatic nerve compression between the two heads of the piriformis muscle leading to foot drop has been reported.
Compression palsies in the ICUs have been known to occur because of protracted bed rest. It is approximated that 10% of patients that stay in the ICU for a period longer than four weeks are expected to develop paresis of the fibular nerve. Critical illness polyneuropathy involving multiple motor and sensory nerves can also present with foot drop.[5] Depending on the extent of involvement, weakness can be bilateral. Patients with diabetes are more vulnerable to these compression neuropathies.
Another common cause of foot drop is Lumbar radiculopathy. L5 radiculopathy is the most common lumbar radiculopathy and results from lumbar disc herniation or spondylitis in the spine.[6]
Compression of the L5 nerve from disc herniations and bony (osteophytes or sacral ala) or ligamentous (sacroiliac ligament and lumbosacral band) compression is known to occur.[7]
2.Traumatic Injuries: They often occur associated with orthopedic injuries such as TKA[8],Fracture to tibial plateau[9], Patellar dislocations (33% chance of nerve damage)[10], Ankle inversion injury.[11]Sciatic neuropathy commonly resulting from either a traumatic injury of the hip or secondary to surgery is the second most common mononeuropathy of the lower extremity and typically presents with foot drop.[12]Lumbosacral plexopathies, resulting from traumatic injury, a complication of abdominal or pelvic surgery, or a complication of neoplasm or radiation therapy is less common cause of foot drop.
3.Neurologic Disorders:
Charcot–Marie Tooth (CMT) is one of the most commonly inherited congenital demyelinating peripheral neuropathy. It affects both motor and sensory nerves. The incidence is 1 in 25000. One of the main symptoms is foot drop and wasting of the lower leg muscles, giving a typical “stork leg” appearance.[13]
Stroke[14] can present as hemiplegia of which foot drop is part of this presentation. Other signs of upper motor neuron involvement such as increased muscle tone, hyperreflexia, and circumduction of the lower extremity during ambulation, are also seen. Depending on the location of ischemia, aphasia can be present.
Clinical Presentation[edit | edit source]
Typical presentation of foot drop can be noted when testing the foot and ankle in isolation, however, in a clinical setting, it may be identified initially through gait assessment.
Foot and Ankle[edit | edit source]
- When testing the foot and ankle a positive test for foot drop is NO active dorsiflexion in a non weight bearing position.
- It is important to test passive ROM to ensure the ankle is not stiff.
- See foot and ankle examination page for a full assessment of the foot and ankle.
Gait Assessment[edit | edit source]
- Gait should be assessed in any clinical setting.
- Foot drop gait can manifest in different ways varying from patient to patient.
- Some patients may increase the amount of hip flexion they produce on the effected side therefore, clearing the floor more effectively:
- [15]
- Other patients may circumduct the hip and drag the forefoot along the floor:
Pain[edit | edit source]
- Neurogenic pain can be experienced from damage to the common peroneal nerve.
- This pain can be present over the lateral aspect of the knee as well as the dorsal part of the foot.
- Sensory changes can also be experienced indicating nerve damage to the therapist.[17]
Diagnostic Procedures[edit | edit source]
- Subjective History: emphasis on any knee trauma, recent spinal/peripheral limb surgery or family history of neurological disease
- Assessment of ankle dorsiflexion
- Neurological exam[17]
- Gait assessment
- Electromyography (EMG) / Nerve conduction studies[18][11]
Outcome Measures[edit | edit source]
- Foot and ankle disability index
- Functional gait analysis
- Stanmore assessment of foot drop[19]
- Hand dynamometry of the dorsiflexors in the foot using the Oxford scale
Management / Interventions[edit | edit source]
Following palsy of the common peroneal nerve, the main residual symptom can be foot drop due to the disruption to L4/5 muscle groups which perform dorsiflexion.
This has been shown to resolve in two-thirds of patients by one-year post-injury. [8]
Pain should also be addressed if the patient is experiencing neuropathic pain by use of appropriate analgesia. [17]
Splinting[edit | edit source]
One way to improve function while the foot drop resolves is the use of splinting.
A solid ankle-foot orthoses (AFO) or foot-up splint can be used to keep the foot in plantar-grade.
These work to increase the amount of dorsiflexion the foot is held in during gait and can prevent falls as the toes do not get caught on the floor.
Exercise[edit | edit source]
Physiotherapy interventions normally are focused on graded exercises to encourage active dorsiflexion and muscle recruitment. These exercises have been shown to prevent atrophy and speed up recovery but more research is needed.[8]
In neurologically impaired patients such as Charcot‐Marie‐Tooth disease improved with strengthening exercises to tibialis anterior, however, other neurological diseases like muscular dystrophy strength training was not found to be effective at reducing the foot drop. [20]
Preventing contractures and stiffness is also an important maintenance goal of physiotherapy as this is likely in neurological disease patients more so than after trauma to the knee.
Electro-stimulation of the affected muscle groups has also been shown to improve recovery times.[8]
Surgery[edit | edit source]
Direct repair of the common peroneal nerve is possible for surgical intervention however, this has been shown to have poor outcomes with residual foot drop leading to further surgery.[21]
In extreme cases tibialis posterior can be transposed to regain active dorsiflexion by using the tendon not innervated by the common peroneal nerve, this surgery has been shown to be more successful than nerve repair.[9][21][19]
Surgery has been shown to be successful at improving active dorsiflexion strength and reduced use of AFOs.[22]
Differential Diagnosis[edit | edit source]
- L5 radiculopathy[18]
- Upper motor neuron lesion
- Chronic/persistent pain[23]
- Sciatic nerve injury[17]
Resources[edit | edit source]
References[edit | edit source]
- ↑ Stewart JD. Foot drop: where, why and what to do?. Pract Neurol. 2008 Jun. 8 (3):158-69. [QxMD MEDLINE Link].
- ↑ Gage JR. An overview of normal walking. Instr Course Lect 1990;39:291–303.
- ↑ Stevens F, Weerkamp NJ, Cals JW. Foot drop. BMJ 2015;350:h1736.
- ↑ Palastanga N & Soames R Anatomy and Human Movement, Structure and Function. 6th ed. China: Elsevier(Churchill Livingstone) Limited; 2012.
- ↑ 5.0 5.1 Baima J, Krivickas L. Evaluation and treatment of peroneal neuropathy. Curr Rev Musculoskelet Med 2008;1(2):147–153.
- ↑ 6.0 6.1 Stewart JD. Foot drop: where, why and what to do? Pract Neurol 2008;8(3):158–169.
- ↑ 7.0 7.1 van Zantvoort A, Setz M, Hoogeveen A, van Eerten P, Scheltinga M. Chronic lower leg pain: entrapment of common peroneal nerve or tibial nerve. Unfallchirurg. 2020 Jan;123(Suppl 1):20-24. [PubMed] [Reference list]
- ↑ 8.0 8.1 8.2 8.3 8.4 Park JH, Restrepo C, Norton R, Mandel S, Sharkey PF, Parvizi J. Common peroneal nerve palsy following total knee arthroplasty: prognostic factors and course of recovery. The Journal of arthroplasty. 2013 Oct 1;28(9):1538-42
- ↑ 9.0 9.1 Baima J, Krivickas L. Evaluation and treatment of peroneal neuropathy. Current reviews in musculoskeletal medicine. 2008 Jun 1;1(2):147-53.
- ↑ Henrichs A. A review of knee dislocations. Journal of athletic training. 2004 Oct;39(4):365.
- ↑ 11.0 11.1 Brief J M, et al. Peroneal Nerve Injury with Foot Drop Complicating Ankle Sprain A Series of Four Cases with Review of the Literature. Bulletin of the NYU Hospital for Joint Diseases. 2009;67(4):374-7
- ↑ Distad BJ, Weiss MD. Clinical and electrodiagnostic features of sciatic neuropathies. Phys Med Rehabil Clin N Am. 2013 Feb;24(1):107-20. [PubMed] [Reference list]
- ↑ Pisciotta C, Shy ME. Neuropathy. Handb Clin Neurol. 2018;148:653-665. [PubMed] [Reference list]
- ↑ Everaert DG, Stein RB, Abrams GM, Dromerick AW, Francisco GE, Hafner BJ, Huskey TN, Munin MC, Nolan KJ, Kufta CV. Effect of a foot-drop stimulator and ankle–foot orthosis on walking performance after stroke: a multicenter randomized controlled trial. Neurorehabilitation and neural repair. 2013 Sep;27(7):579-91.
- ↑ Steppage Gait. Judy Mishriki Available from: https://www.youtube.com/watch?v=TijuPg8_JhY [last accessed 02/09/2013]
- ↑ Alaine Wambe MD. Right slap gait/steppage gait/foot drop in a post operative patient. Available from: https://www.youtube.com/watch?v=EjPUpKUbZSg [last accessed 11/03/2019]
- ↑ 17.0 17.1 17.2 17.3 Baima J, Krivickas L. Evaluation and treatment of peroneal neuropathy. Current reviews in musculoskeletal medicine. 2008 Jun 1;1(2):147-53.
- ↑ 18.0 18.1 Masakado Y, Kawakami M, Suzuki K, Abe L, Ota T, Kimura A. Clinical neurophysiology in the diagnosis of peroneal nerve palsy. The Keio journal of medicine. 2008 Jun 25;57(2):84-9.
- ↑ 19.0 19.1 Lingaiah P, Jaykumar K, Sural S, Dhal A. Functional evaluation of early tendon transfer for foot drop. Journal of Orthopaedic Surgery. 2018 Sep 19;26(3):2309499018799766.
- ↑ Sackley C, Disler PB, Turner‐Stokes L, Wade DT, Brittle N, Hoppitt T. Rehabilitation interventions for foot drop in neuromuscular disease. Cochrane Database of Systematic Reviews. 2009(3).
- ↑ 21.0 21.1 Özkan T, Tuncer S, Ozturk K, Aydin A, Ozkan S. Tibialis posterior tendon transfer for persistent drop foot after peroneal nerve repair. Journal of reconstructive microsurgery. 2009 Apr;25(03):157-64.
- ↑ Hove LM, Nilsen PT. Posterior tibial tendon transfer for drop-foot: 20 cases followed for 1–5 years. Acta Orthopaedica Scandinavica. 1998 Jan 1;69(6):608-10.
- ↑ Brewer RB, Gregory AJ. Chronic lower leg pain in athletes: a guide for the differential diagnosis, evaluation, and treatment. Sports Health. 2012 Mar;4(2):121-7.