Early-Onset Alzheimer's: A Case Study
Top Contributors - Jeanie Lee, Katerina Jirasek, Kim Jackson, Michele Delfino, Lindsey Gibb, Vince DePaul and Melissa Tan
Abstract[edit | edit source]
Alzheimer's is the most common cause of dementia. It is characterized by a gradual degradation of various physical and cognitive functions[1]. The current fictional case study is about a 42 year old female with early onset Alzheimer’s Disease (EOAD) seeking physiotherapy treatment. Evaluation findings include gait abnormalities, decreased balance and decreased cognition. She presented with forward head posture with slight postural kyphosis and palpable muscle tightness in upper trapezius. Slight weakness in lower extremities (L/E), and decreased shoulder flexion bilaterally. The physiotherapy intervention component includes education, home based exercise programs addressing aerobic and strengthening deficits. Following the physiotherapy intervention, Mrs. S improved her AROM, muscular strength, postural control and gait all the while decreasing overall fatigue and risk of falls. Throughout the treatment plan there were no changes in cognitive function. Mrs. S will continue to be involved in interprofessional care to maintain her quality of life. The physiotherapist’s role in EOAD cases is to maximize independence to help prevent the progression of physical and cognitive decline[2]. In the future, more research must be conducted to determine the adequate frequency, intensity, and duration of treatment for patients with EOAD[3][4].
Introduction[edit | edit source]
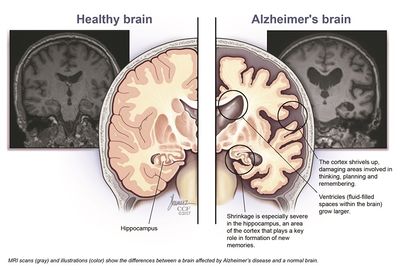
Alzheimer's is “a type of dementia that causes problems with memory, thinking and behaviour. Symptoms usually develop slowly and get worse over time, becoming severe enough to interfere with daily tasks”[1]. Literature shows that physical activity has been repeatedly found to improve the ability of patients with dementia to perform activities of daily living (ADLs)[5]. However, it seems that the frequency, intensity, and duration of exercises prescribed in order to elicit benefits varies widely between studies[5]. On the other hand, research regarding the effects of physical activity on the cognitive function of patients with dementia are inconclusive. A review conducted by McDonnell et al., stated that there is a small effect of aerobic exercise programs on improving cognitive function[6]. However, another review states that an exercise program combining aerobic and strength conditioning evokes no effects on cognitive function[7]. The current case study describes a patient with EOAD who presents with mild difficulties with her ADLs as well as other symptoms such as reduced balance, gait abnormalities, reduced aerobic capacity, and cognitive decline. This report strives to document the changes in the patient’s symptom presentation throughout her involvement in physiotherapy.
Client Characteristics[edit | edit source]
Mrs. S, a 42 year old female with a 1 year history of EOAD presents to the clinic. She previously worked as a full-time administrator at a real estate office. She is recently unemployed due to the worsening of her condition in the last 3 months. Various progressive cognitive symptoms such as memory deficits and confusion have rendered her unfit to continue to work. Mrs. S sought for physiotherapy in order to delay the physical progression of the disease. Her chief complaints include mild difficulties with gait, balance, and being fatigued easily. She noted that she has stumbled and tripped several times in the past 3 months but was fortunately not hurt. She has also noticed the increasing difficulty she is having with fine motor skills such as writing and doing up her buttons when dressing. With the diagnosis of EOAD, the patient is at an increased risk of various secondary conditions such as osteoporosis and falls.
Examination Findings[edit | edit source]
Subjective[edit | edit source]
- Patient Profile (PP): 42 y/o female
- History of Present Illness (HPI): Diagnosed with EOAD 1 year ago, presenting with mild cognitive and physical deficits, not currently receiving treatment interventions from PT.
- Past medical history: Depression
- Medications: Celexa (citalopram) 20mg/day, donepezil (aricept) 10mg/day
- Health Habits: Non-smoker, 1 glass of red wine per week, no other substances
- Family History: Mother passed away from complications of EOAD in 2001
- Social History: Recently resigned from full time position as administrator at a real estate office due to cognitive difficulties. Lives alone in a bungalow with her pet dog. Family lives in the next town over (25 minute drive). Currently spends majority of her day walking her dog and babysitting her neighbours’ kids. Imaging: Magnetic resonance imaging (MRI), Positron Emission Tomography (PET), Single-Photon Emission Computed Tomography (SPECT)
Precautions/Contraindications: Slight confusion with short term memory, risk of agitation, current unemployment, and depression.
Objective[edit | edit source]
Vitals: HR: 80 bpm, BP: 120/80 mmHg, RR= 20 bpm.
Observation: Forward head posture (protracted) along with slight increased postural kyphosis. Palpable muscle tightness in upper trapezius. Patient appears to be slightly deconditioned.
- Cervical AROM= slightly limited in extension
- Shoulder AROM= bilateral shoulder flexion decreased.
- All other UE AROM= WNL
- U/E sensation intact
- L/E AROM= limited trunk extension, all other WNL
- L/E sensation intact
Isometric break test (IBT):
- Upper extremities: strong, pain free, and good motor control.
- Lower extremities: slightly weak, pain free, and good motor control.
Coordination Tests:
- Finger to nose: smooth and controlled, with slight dysmetria bilaterally
- Finger opposition: mild bilateral impairment in coordination
Self-reported outcome measures:
- Functional Activities Questionnaire (FAQ): Score of 13/30
- Generalized Anxiety Disorder (GAD-7): 8/21
- Patient Health Questionnaire (PHQ-9): 10/27
Outcome measures:
- Mini-mental State Examination (Mental Health Outcome Measures for Physiotherapists in Clinical Practice): score of 20/30
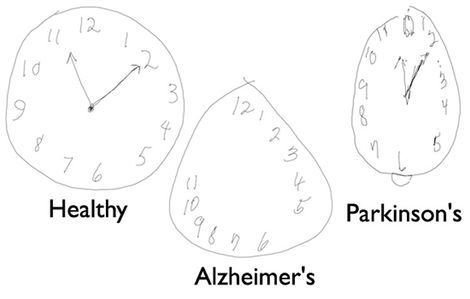
- Clock drawing test: score of 2/5 on the Shulman Method
- Timed Up and Go Test (TUG): 13 seconds
- Mini-Balance Evaluation Systems Test (BESTest): Score of 21/28.
Clinical Impression[edit | edit source]
Major clinical findings identified during the subjective interview were the patient’s history of falls, gait abnormalities, and decreased cognition due to the progression of her condition. This is affecting her ADLs, sleep quality and quantity, as well as her interaction with others. She was no longer able to work due to cognitive and physical changes. These factors, in combination with her condition, appear to be negatively impacting her functionality which was once at a high level prior to her diagnosis. This is reflected in her FAQ score of 13/30 indicating impaired function and possible cognitive impairment[8]. Both her GAD-7 score of 8/21 and her PHQ-9 score of 10/27 reflect mild, probable generalized anxiety that will require clinical judgement from a physician for intervention[9][10]. The patient’s cognitive baseline is assessed using the MMSE and the clock drawing test with scores of 20/30 and 2/5 respectively. Both tests support her diagnosis of mild EOAD[11][12].
The difficulty with balance is indicated by a TUG score of 13 seconds which suggest an increased risk of falls[13]. The weakness she is experiencing in her L/E and difficulty with postural control and dual gait tasks are demonstrated within the Mini-BESTest reflecting a score of 21/23[14]. Tasks of poor performance that indicate physiotherapy intervention include: reactive postural control during compensatory stepping when making corrections to forward, backward, and lateral external perturbations. There were also marked difficulties in dynamic gait when asked to speed up, turn head when walking, execute a pivot turn, and when stepping over obstacles. Fine motor skills as assessed through the finger-to-nose test, and finger opposition indicate mild dysmetria.
Problem List[edit | edit source]
- Decreased postural control: due to weakness with external perturbations
- Decreased balance: instability during gait, especially during dual tasks
- Decreased L/E muscle strength and proprioception
- Reduced aerobic capacity
- Decreased fine motor control and coordination
- Memory impairment: difficulty remembering instructions and task components
- Increased fatigue secondary to depression
Intervention[edit | edit source]
Patient Goals[edit | edit source]
- Improve reactive postural control to external perturbations in the Mini-BESTest taking no more than 2 steps to recover balance within 2 months
- Improve TUG score from 13sec to 10sec within 8 weeks to surpass the cutoff for independent mobility
- Increase lower extremity strength on IBT by 1 point within 2 months
- Improve the accuracy of movements on the finger to nose coordination test
- Be able to walk and count by 2’s without hesitation and stopping within 8 weeks to improve motor coordination and cognition
Treatment Plan[edit | edit source]
| Frequency | Intensity | Time | Rationale | |
|---|---|---|---|---|
| Education
1) Cognitive strategies 2) Relaxation techniques 3) Importance, instructions and how to manage risks associated with exercises 4) When to seek medical attention |
As early on as possible | As appropriate | Ongoing | 1) Compensation strategy for cognitive decline and memory issues. E.g. writing out lists, setting reminders, etc.
2) Manage stress and anxiety 3&4) Increase adherence to exercise program, ensure safety and effectiveness |
| Brisk Walking | Begin at 80min/wk and progress to
>150min/wk |
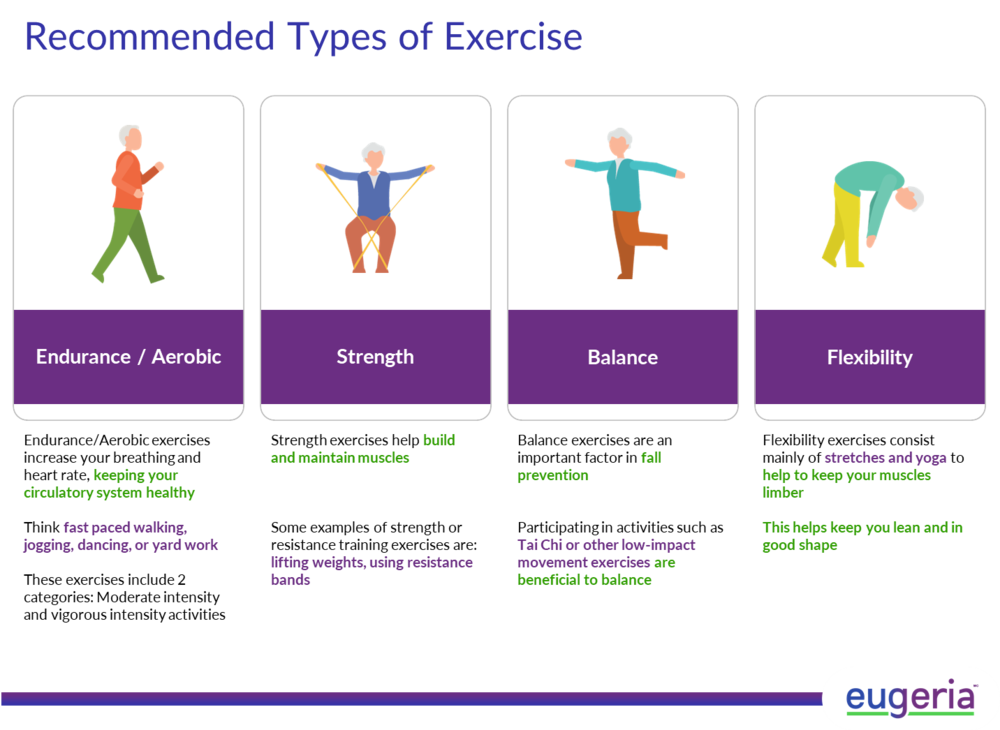
Moderate intensity | Bouts of 10mins or more, accumulating 150min/wk | Mrs. S presents with reduced aerobic capacity, increased fatigue and gait abnormalities, therefore mild difficulties with ADLs. A meta-analysis showed that aerobic exercise alone has a positive effect on improving ADLs and cognitive function[3] |
| Balance training
(e.g. tandem stance, heel and toe walking) |
2-3 x/ week | within limits of stability | 3 set of 10 steps | On several occasions, Mrs. S stumbled and tripped but luckily was not hurt. An individualized exercise program with close supervision that comprises balance amongst other components can help to prevent falls and its associated consequences[15] |
| L/E strengthening
(kitchen sink exercises e.g. heel raises, hip abduction and extension, half squats) |
2-3 x/week | 60% of 1 RM | 3 set of 10 reps with 1 minute rest
Tempo: 1:0:1 seconds |
On objective examination, Mrs. S appeared to have decreased L/E muscle strength and proprioception. To address this a combination of aerobic and non-aerobic exercise can improve physical function outcomes such as the TUG, functional reach, and performance oriented mobility assessment, as well as cognitive outcomes such as MMSE[4] |
| Dual task training
(walking while counting by 2’s) |
2x/week | light intensity | 3 sets of 30 seconds | To address impairments in Mrs. S cognitive function and motor control |
| Fine motor task
(finger opposition, finger to nose) |
Daily | N/A | 3 sets of 10 reps | Enhance ADLs and occupational tasks such as doing up buttons and writing |
Medical and lifestyle management are areas of practice addressed within the interprofessional care team. Pharmacological agents will manage cognitive function and behavioural symptoms[16]. In addition, consuming a healthy diet, such as the Mediterranean Diet (MeDi) diet may help slow cognitive decline in individuals with Alzheimer’s disease[17].
Outcome[edit | edit source]
Following Mrs. S’s initial assessment it was determined she would receive four months of physiotherapy care to address her postural and gait impairments with associated fatigue. Her treatment program consisted of visits two times per week for the first month and one visit every 3 weeks for the last three months. A thorough follow-up assessment was performed.
Within four months her AROM and muscular strength improved slightly and there were no significant changes in vital signs. Mrs. S still presents with forward (protracted) head posture along with a slight postural kyphosis. She had slight improvement in her postural awareness and increased motor control of her scapulothoracic stabilizing muscles.
The scores on her outcome measures are listed below:
- FAQ = 13/30
- GAD-7 = 7/21
- PHQ-9 = 8/27
- MMSE = 20/30
- Clock drawing test = 2/5
- TUG = 10 seconds
- Mini-Best = 24/28
The GAD-7 and PHQ-9 decreased indicating a lower number of symptoms associated with anxiety and depression. This may reflect her increase in confidence with daily tasks, postural control, strength and decreased fatigue. Mrs. S improved on the gait components of the Mini-Best test, increasing her score by a total of three points. Furthermore, her TUG time on reassessment was 10 seconds which decreases her risk of falls. For the MMSE and clock drawing test no significant changes were reported. These tests will continue to be used to monitor the cognitive status over time.
Based on her progress and improvements over the past four months Mrs. S should continue physiotherapy treatment as needed to help manage the progression of the musculoskeletal, postural, and gait impairments secondary to EOAD. It is suggested she visit her family doctor to receive a referral to community balance and healthy aging programs. Mrs. S would benefit from a referral to an occupational therapist for a thorough home assessment, maintenance of mental health status and future need for assistive devices. Ms. S would further benefit from a nutritionist or dietitian who can educate her on proper eating habits such as the MeDi diet which has been shown benefit patients with Alzheimer's[17].
Discussion[edit | edit source]
Mrs. S presented with a history of falls, gait deficits, and decreased cognition. Mrs. S and her physiotherapist developed a list of goals to assist with managing and preventing further progression of her mobility difficulties. After four months of the physiotherapy treatment plan, a thorough follow-up assessments was completed. Improvements where seen in her confidence to perform ADLs and a decrease in stress and anxiety. Furthermore, her L/E strength increased as well as her mobility. Other cognitive symptoms did not change which may be due to the progression of the disease.
There are many cases of EOAD presenting with gait impairments, postural instability, decreased musculoskeletal and memory function found secondary to the disease. The role of a physiotherapist varies depending on the disease progression, but the overall aim is to maximize independence by improving and preserving motor and cognitive function[2]. Although there are similarities in symptoms among patients with EOAD, the treatment plan should be personalized to each individual. However, as the disease progresses, there should be additional emphasis placed on decreasing risk of falls, managing cognitive decline and reducing the burden on family and caregivers[2][4].
As discussed, intervention approaches such as exercise and physical activity are beneficial for those with EOAD. These interventions are also applicable for patients with dementia and aging related cognitive impairments. The research has shown that a combination of both aerobic and strength exercise can improve physical function[4]. Participation in community and home exercise programs consisting of daily exercises and a graded walking program have shown to improve independence with performing ADLs and overall quality of life (QOL)[18]. Through improving functional ability of the patient, research suggests that home exercise programs also provide benefit to their caregivers by reducing physical and emotional burden[18].
Rehabilitation therapy is constantly evolving and so are the needs of each individual with Alzheimer’s Disease. The progression of the disease varies in severity and time for each individual as should their treatment. Further research should be focused on bridging the gap in literature around disease progression and physiotherapy intervention focusing on determining the appropriate frequency, intensity, and duration of treatment for this population[3][4]. The evolution of the research should focus on selecting a study design and methodical approach that will increase the external validity and thus allow for the transfer of knowledge to the EOAD cohort.
References[edit | edit source]
- ↑ 1.0 1.1 Alzheimer's Disease and Dementia. (2019). What Is Alzheimer's?. [online] Available at: https://www.alz.org/alzheimers-dementia/what-is-alzheimers [Accessed 9 May 2019].
- ↑ 2.0 2.1 2.2 Lord S, Rochester LY. Role of the physiotherapist in the management of dementia. 2017 Feb 24 (pp. 240-248). CRC Press.
- ↑ 3.0 3.1 3.2 Groot C, Hooghiemstra AM, Raijmakers PG, Van Berckel BN, Scheltens P, Scherder EJ, Van der Flier WM, Ossenkoppele R. The effect of physical activity on cognitive function in patients with dementia: a meta-analysis of randomized control trials. Ageing research reviews. 2016 Jan 1;25:13-23.
- ↑ 4.0 4.1 4.2 4.3 4.4 Rao AK, Chou A, Bursley B, Smulofsky J, Jezequel J. Systematic review of the effects of exercise on activities of daily living in people with Alzheimer’s disease. American Journal of Occupational Therapy. 2014 Jan 1;68(1):50-6.
- ↑ 5.0 5.1 Forbes D, Forbes SC, Blake CM, Thiessen EJ, Forbes S. Exercise programs for people with dementia. Cochrane Database of Systematic Reviews. 2015(4).
- ↑ McDonnell MN, Smith AE, Mackintosh SF. Aerobic exercise to improve cognitive function in adults with neurological disorders: a systematic review. Archives of physical medicine and rehabilitation. 2011 Jul 1;92(7):1044-52.
- ↑ Lamb SE, Sheehan B, Atherton N, Nichols V, Collins H, Mistry D, Dosanjh S, Slowther AM, Khan I, Petrou S, Lall R. Dementia And Physical Activity (DAPA) trial of moderate to high intensity exercise training for people with dementia: randomised controlled trial. bmj. 2018 May 16;361:k1675.
- ↑ Teng E, Becker BW, Woo E, Knopman DS, Cummings JL, Lu PH. Utility of the Functional Activities Questionnaire for distinguishing mild cognitive impairment from very mild Alzheimer’s disease. Alzheimer disease and associated disorders. 2010 Oct;24(4):348.
- ↑ Spitzer RL, Kroenke K, Williams JB, Löwe B. A brief measure for assessing generalized anxiety disorder: the GAD-7. Archives of internal medicine. 2006 May 22;166(10):1092-7.
- ↑ Kroenke K, Spitzer RL, Williams JB, Löwe B. The patient health questionnaire somatic, anxiety, and depressive symptom scales: a systematic review. General hospital psychiatry. 2010 Jul 1;32(4):345-59.
- ↑ Pangman VC, Sloan J, Guse L. An examination of psychometric properties of the mini-mental state examination and the standardized mini-mental state examination: implications for clinical practice. Applied Nursing Research. 2000 Nov 1;13(4):209-13.
- ↑ Mendes-Santos LC, Mograbi D, Spenciere B, Charchat-Fichman H. Specific algorithm method of scoring the Clock Drawing Test applied in cognitively normal elderly. Dementia & neuropsychologia. 2015 Jun;9(2):128-35.
- ↑ Podsiadlo D, Richardson S. The timed “Up & Go”: a test of basic functional mobility for frail elderly persons. Journal of the American geriatrics Society. 1991 Feb;39(2):142-8.
- ↑ Leddy AL, Crowner BE, Earhart GM. Utility of the Mini-BESTest, BESTest, and BESTest sections for balance assessments in individuals with Parkinson disease. Journal of neurologic physical therapy: JNPT. 2011 Jun;35(2):90.
- ↑ Jensen LE, Padilla R. Effectiveness of interventions to prevent falls in people with Alzheimer’s disease and related dementias. American Journal of Occupational Therapy. 2011 Sep 1;65(5):532-40.
- ↑ Bishara D, Sauer J, Taylor D. The pharmacological management of Alzheimer's disease. Progress in Neurology and Psychiatry. 2015 Jul;19(4):9-16.
- ↑ 17.0 17.1 Frisardi V, Panza F, Seripa D, Imbimbo BP, Vendemiale G, Pilotto A, Solfrizzi V. Nutraceutical properties of Mediterranean diet and cognitive decline: possible underlying mechanisms. Journal of Alzheimer's Disease. 2010 Jan 1;22(3):715-40.
- ↑ 18.0 18.1 Vreugdenhil A, Cannell J, Davies A, Razay G. A community‐based exercise programme to improve functional ability in people with Alzheimer’s disease: A randomized controlled trial. Scandinavian journal of caring sciences. 2012 Mar;26(1):12-9.