Complications Post Burns
Original Editor - Manisha Shrestha
Top Contributors - Naomi O'Reilly, Manisha Shrestha, Abdulazeez Arowolo, Jess Bell and Chelsea Mclene
Introduction[edit | edit source]
Burn injuries are under-appreciated injuries that are associated with substantial morbidity and mortality. The injuries can be caused by friction, cold, heat, radiation, chemical or electric sources, but the majority of burn injuries are caused by heat from hot liquids, solids or fire. [1] Burn injuries are a significant problem with more than 500,000 people seeking medical treatment, 40,000 resultant hospitalizations, and 4000 deaths per year in the United States. The annual cost of treating these burns is estimated to be in excess of U.S. $ 1 billion, not including the indirect costs of disability and rehabilitation.[2]
Burn injuries can have devastating sequelae that can cause long term morbidity. The best way to minimize complications is to manage burns in a dedicated burns center with immediate full multi-disciplinary involvement. The complication following burn can be
- Early (Acute) or long-term (chronic)
- Local or systemic[3]
Local Complications[edit | edit source]
Burn Wound Infection[edit | edit source]
Burn wound infection is a common cause of morbidity and mortality in burn patients, particularly within disaster and conflict settings. Significant thermal injuries induce a state of immunosuppression that predisposes burn patients to infectious complications as an intact human skin surface is vital to the preservation of body fluid homeostasis, thermoregulation, and the host's protection against infection. Burn patients are also at risk for developing sepsis secondary to pneumonia, catheter-related infections, and suppurative thrombophlebitis. Patient's demographic, burn severity and changes in burn wound care are some of the factors affecting the overall fatality rates from burn wound infection.[4]
Systemic Complications[edit | edit source]
Systemic complications will arise secondary to the large inflammatory response produced by the body in response to the burn injury. Following a burn, there is an enormous production of reactive oxygen species (ROS) which is harmful and implicated in inflammation, systemic inflammatory response syndrome, immunosuppression, infection and sepsis, tissue damage, and multiple organ failure.[2]Systemic effects will typically manifest in patients with burns of >25% total body surface area (TBSA) or often smaller proportions in children.[3]
Burn Shock[edit | edit source]
Burn injuries have been shown to produce systemic effects, including sympathetic stimulation, hypovolemia, renal failure, and myocardial dysfunction. Such effects are referred to as burn shock..
Burn shock is a medical emergency that occurs when the body's tissues and organs are deprived of adequate oxygenated blood, which includes decreased cardiac output, increased vascular resistance, hypovolaemia and hypoperfusion that occur after severe burn injuries have been sustained.[5]Inflammatory and vasoactive mediators such as histamines, prostaglandins, and cytokines are released causing a systemic capillary leak, intravascular fluid loss, and large fluid shifts. These responses occur mostly over the first 24 hours peaking at around six to eight hours after injury.[5]
It is common in burns that involve 30% of the total body surface area. Burn shock occurs due to the interplay of soft-tissue loss, hypovolemia, and systemic mediators and persists as a dangerous pathophysiologic state even after fluid resuscitation has been initiated and hypovolemia is corrected. If left untreated, this state leads to adult respiratory distress syndrome and progressive organ dysfunction.
The possible complications of burns can affect different systems of the body and Physiotherapists of different specializations should be aware of the possible complications. The complications could be respiratory, orthopedics, vascular, Gastrointestinal etc.
Respiratory complications[edit | edit source]
Respiratory complications, particularly those related to inhalation injury, occur as a result of direct cellular damage, alterations in regional blood circulation and perfusion, obstruction of the airways, and the release of pro-inflammatory cytokine and toxin release.[6][7] This may cause reduced functionality of mucociliary clearance and weakening of alveolar macrophages,[8] which places the patient at a high risk of bacterial infection, especially pneumonia.[9][10]
The presence of a smoke inhalation injury, alongside patient age and percentage of body surface area burned, is a major determinant of mortality. Inhalation injury increases the risk of death from a burn injury 3.6-fold. Smoke inhalation injury leads to respiratory complications in 73% and acute respiratory distress syndrome (ARDS) in 20%.[11]
Orthopedic Complications[edit | edit source]
Soft tissue Injury[edit | edit source]
Burn can affect soft tissue injuries like tendon, peripheral nerves which can have long term affect if left untreated and is severe.
Fractures[edit | edit source]
Fracture associated with burn are usually present following injuries from falls caused by the electrical shock, such as long bone fractures, spinal fractures, or joint dislocations (classically posterior shoulder dislocations). [12]The historical standard of care for the treatment of fractures in association with burns has been external fixation. More recent data suggest that if patients are adequately resuscitated and stable, internal fixation of orthopaedic injuries within the first forty-eight hours after injury is associated with improved healing rates and a lower incidence of infection. Surgical incisions can be safely extended into burnt tissue to provide adequate operative exposure and fracture reduction. [13]
Complications that occur in patients with fractures associated with burns include infection, nonhealing incisions, delayed union, nonunion, stiffness, and scar formation.
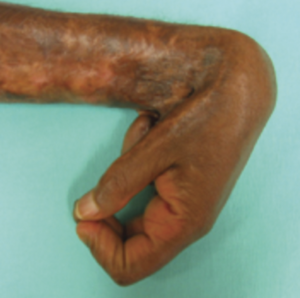
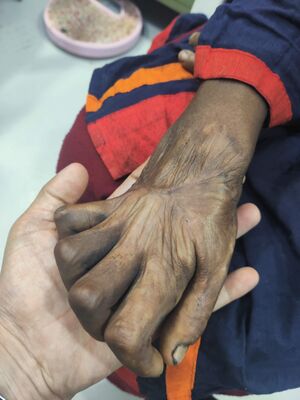
Joint Contracture[edit | edit source]
Joint contracture is often a long term complication associated with burns, and patients with tendon injury, and burn areas involving joint are more likely to have joint contracture. The optimal method to treat joint contractures in burn patients is to take a preventative approach that includes the provision of adequate analgesia, early active range-of-motion exercises, proper positioning during acute care and timely plastic surgery consultation with regard to the excision of scar tissue.
Heterotrophic Ossification[edit | edit source]
Heterotophic Ossification, also referred to as ectopic ossification and myositis ossificans, is the formation of pathological bone in muscle or soft tissue, which if severe can lead to ankylosis and impaired function. It usually presents around the joint, predominantly in the hip, with the first signs including swelling around the joint, reduced range of motion, with or without fever, spasticity and pain, which are similar clinical signs to those of fracture and deep venous thrombosis. Ultrasound, CT Scan or Bone Scan are used to provide a definitive diagnosis of heterotopic ossification, although blood tests may also give some indication. In general, surgical excision of heterotopic bone is effective, but, to minimize the rate of recurrence, excision should be delayed until twelve months or more after injury, when maturation is complete.
Compartment Syndrome[edit | edit source]
Compartment Syndrome, common both following burns or crush injuries, is a condition in which there is increased pressure within a closed osteofascial compartment, resulting in impaired local circulation. Electrical, circumferential, and full-thickness burns all are associated with an elevated risk of compartment syndrome. Prompt escharotomy or fasciotomy should be performed if patients exhibit increasing analgesic requirements or have elevated compartment pressures. Without prompt treatment, acute compartment syndrome can lead to ischemia and eventually, necrosis, often resulting in the need for amputation if not adequately managed.[14]
Gastrointestinal Complications[edit | edit source]
These include paralytic ileus, Curling’s ulcer, and bacterial translocation. Early enteral feeding often mitigates complications, aiming to maintain body weight and endocrine homeostasis[3]
Endocrine Complications[edit | edit source]
Direct fluid loss from the burns, third space losses, and kidney injury can lead to electrolyte imbalance, commonly results in initial hypernatraemia; subsequent hypokalaemia, hypomagnesaemia, hypocalcaemia, and hypophosphataemia
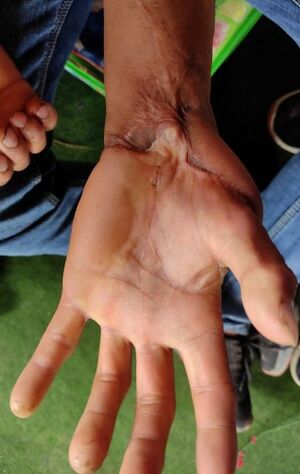
Skin Complications[edit | edit source]
Hypertrophic Scarring, Keloid Formation and Contractures are unfortunately quite common following burn injury, and occur more frequently within low resource, disaster and conflict settings where access to ongoing treatment may be impacted. Scarring following burn injury and its accompanying aesthetic and functional sequelae still pose major challenges.
Hypertrophic scarring (HTS) is a major concern in deep partial thickness burn injuries. A scar generally forms within weeks of insult, and studies indicate that a wound that takes longer than 2–3 weeks to heal is characterized by an increased risk of hypertrophic scar formation. The incidence of HTS occurrence following burn injuries has been reported to range from 32 to 94%. This condition can be associated with significant pain and limited movement when present over joints.[15]
A keloid is a growth that rises above the skin surface; it is hard, shiny, and white or pink in color. When healing must take place over a large area, or one that has been skin-grafted, keloids may develop. It is actually a benign tumor, generally harmless except that it may cause uncomfortable itching and may pose a cosmetic problem.
Multisystem Organ Dysfunction[edit | edit source]
Multisystem Organ Dysfunction, a progressive disorder that commonly occurs in acutely ill patients, exists in a continuum with the systemic inflammatory response syndrome (SIRS) that affects most patients with severe burns, with or without an infection with increased risk seen with burn wounds >20 percent total body surface area, increasing age, male gender, sepsis, hypoperfusion, and under-resuscitation.
Specific organ injuries
- Acute lung injury – caused by a combination of burn and smoke inhalation, which can eventually lead to acute respiratory distress syndrome (ARDS)
- Acute kidney injury – multifactorial from a combination of SIRS, hypotension, myoglobinuria, and any iatrogenic nephrotoxic agents
Resources[edit | edit source]
Rehabilitation of Burns Casualties
References[edit | edit source]
- ↑ Jeschke MG, van Baar ME, Choudhry MA, Chung KK, Gibran NS, Logsetty S. Burn injury. Nature Reviews Disease Primers. 2020 Feb 13;6(1):1-25.
- ↑ 2.0 2.1 Nielson CB, Duethman NC, Howard JM, Moncure M, Wood JG. Burns: pathophysiology of systemic complications and current management. Journal of Burn Care & Research. 2017 Jan 1;38(1):e469-81.
- ↑ 3.0 3.1 3.2 TeachMe Surgery. Burns Complications, Rehabilitation, and Reconstruction. Available from: https://teachmesurgery.com/plastic-surgery/burns/burns-reconstruction/ lasted accessed: 28th March 2022
- ↑ Church D, Elsayed S, Reid O, Winston B, Lindsay R. Burn wound infections. Clinical microbiology reviews. 2006 Apr;19(2):403-34.
- ↑ 5.0 5.1 Schaefer TJ, Nunez Lopez O. Burn Resuscitation And Management. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020
- ↑ Kadri SS, Miller AC, Hohmann S, Bonne S, Nielsen C, Wells C, Gruver C, Quraishi SA, Sun J, Cai R, Morris PE. Risk factors for in-hospital mortality in smoke inhalation-associated acute lung injury: data from 68 United States hospitals. Chest. 2016 Dec 1;150(6):1260-8.
- ↑ Reper P, Heijmans W. High-frequency percussive ventilation and initial biomarker levels of lung injury in patients with minor burns after smoke inhalation injury. Burns. 2015; 41:65–70. [PubMed: 24986596]
- ↑ Al Ashry HS, Mansour G, Kalil AC, Walters RW, Vivekanandan R. Incidence of ventilator associated pneumonia in burn patients with inhalation injury treated with high frequency percussive ventilation versus volume control ventilation: A systematic review. Burns. 2016 Sep 1;42(6):1193-200.
- ↑ Mlcak RP, Suman OE, Herndon DN. Respiratory management of inhalation injury. burns. 2007 Feb 1;33(1):2-13.
- ↑ Pruitt BA, McManus AT. The changing epidemiology of infection in burn patients. World journal of surgery. 1992 Jan 1;16(1):57-67.
- ↑ Gill P, Martin RV. Smoke inhalation injury. BJA Education. 2015 Jun 1;15(3):143-8.
- ↑ Bounds EJ, West B, Kok SJ. Electrical Burns.
- ↑ AlQahtani SM, Alzahrani MM, Carli A, Harvey EJ. Burn management in orthopaedic trauma: a critical analysis review. JBJS reviews. 2014 Oct 28;2(10):e4.
- ↑ Torlincasi AM, Lopez RA, Waseem M. Acute compartment syndrome. 2017 [last accessed 16.03.2022]
- ↑ Chiang RS, Borovikova AA, King K, Banyard DA, Lalezari S, Toranto JD, Paydar KZ, Wirth GA, Evans GR, Widgerow AD. Current concepts related to hypertrophic scarring in burn injuries. Wound Repair and Regeneration. 2016 May;24(3):466-77.