Aponeurosis
Original Editor - lucinda hampton
Top Contributors - Lucinda hampton, Ahmed M Diab and Kim Jackson
Introduction[edit | edit source]
Aponeuroses are sheet-like elastic tendon structures that cover a portion of the muscle belly and act as insertion sites for muscle fibers while free tendons connect muscles to bones[1]. They have a role similar to a tendon but here is how they differ:
- An aponeurosis looks quite different than a tendon. An aponeurosis is made of layers of delicate, thin sheaths. Tendons, in contrast, are tough and rope-like. An aponeurosis is made primarily of bundles of collagen fibers distributed in regular parallel patterns, which makes an aponeurosis resilient.
- Aponeurosis has a function of absorbing energy during the movement of the muscle, while Tendon has a function of stretching and contracting during muscle movements.
- It is very rare for the Aponeurosis to get injured as it is situated hidden under many layers of bones and muscles. But Tendon gets injured easily, for it is present in all the injury-prone areas.
- Aponeuroses can act as fascia. Fascia is a fibrous tissue that envelopes muscles or organs, to bind muscles together or to other tissues.[2][3].
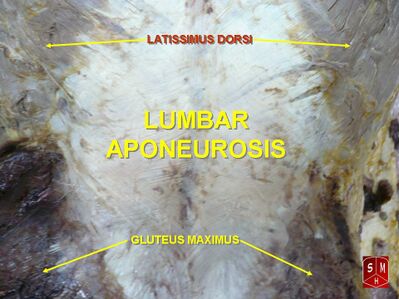
Image 1: Lumbar aponeurosis
We have lots of aponeuroses, some are listed below.
Erector Spinae Aponeurosis[edit | edit source]
The erector spinae aponeurosis (ESA) is a common aponeurosis that blends with the thoracolumbar fascia, with a proximal attachment on the sacrum and the spinous processes of the lumbar vertebrae, for the three erector spinae muscles (iliocostalis, longissimus, and spinalis) and overlying the inferior portion of the erector spinae muscles.[4]
The thoracolumbar fascia (TLF) and the erector spinae aponeurosis (ESA) play significant roles in the biomechanics of the spine. The ESA, at twice the thickness of the TLF, is the thickest dense connective tissue (mean thickness: 1.85 mm) of the paraspinal compartment. [5]
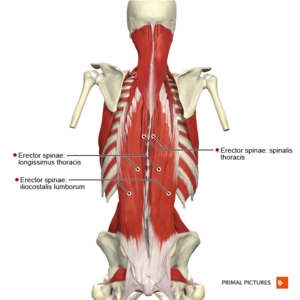
Image 2: Erector Spinae Aponeurosis
Rectus Sheath[edit | edit source]
The Rectus Sheath is an aponeurosis formed by the five muscles of the abdomen. It has an anterior and posterior wall for most of its length. The anterior wall is formed by the aponeuroses of the external oblique and half of the internal oblique. The posterior wall is formed by the aponeuroses of half of the internal oblique and transversus abdominis. About midway between the umbilicus and pubic symphysis, there is only the anterior wall of the rectus sheath and no posterior sheath[6].
Aponeurosis of the External Oblique[edit | edit source]
The aponeurosis of the external oblique is the broad, flat tendinous portion of the external abdominal oblique muscle. The fleshy fibers of the muscle end in the aponeurosis along a line descending vertically from the costochondral joint of the ninth rib then turning laterally just below the level of the umbilicus toward the anterior superior iliac spine. The fibers of the aponeurosis run medially and inferiorly, contributing to the anterior wall of the sheath of the rectus abdominis muscle and decussating with those of the contralateral aponeurosis at the median linea alba. Inferomedially, the aponeurosis is attached to the upper border of the pubic symphysis, the pubic crest, and pubic tubercle.[7]
The aponeurosis of the external oblique is formed of two layers: superficial and deep. The fibres of each layer are perpendicular to those of the other layer.[8]
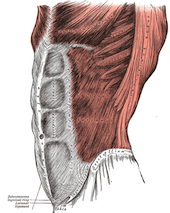
Image 3: Aponeurosis of the External Oblique
Epicranial Aponeurosis[edit | edit source]
The epicranial (or galea) aponeurosis is a tough fibrous sheet of connective tissue that extends over the cranium, forming the middle (third) layer of the scalp. The epicranial aponeurosis also contains vessels that communicate between the deep vascular plexus contained within the subgaleal layer below as well as the superficial vascular plexus in the subcutaneous layer above[9].
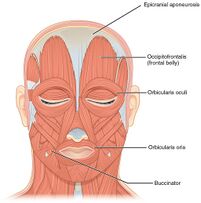
Image 4 : epicranial aponeurosis.
Bicipital Aponeurosis[edit | edit source]
The bicipital aponeurosis is a broad aponeurosis of the Biceps Brachii which is located in the cubital fossa of the elbow and separates superficial from deep structures in much of the fossa.
The bicipital aponeurosis originates from the distal insertion of the biceps brachii. While the tendon of the biceps inserts on the radial tuberosity, the aponeurosis reinforces the cubital fossa, and helps to protect the brachial artery and the median nerve running underneath[10].
Palmar Aponeurosis[edit | edit source]
The palmar aponeurosis (PA) of the hand is a continuation of the flexor retinaculum, consisting of a sheet of connective fibers that converge near the distal wrist crease and radiate to the bases of the fingers. The PA attaches to muscles, ligaments, digital sheaths and a forearm tendon (palmaris longus).
The function of palmar aponeurosis is mechanical. It firmly attaches to the palmar skin allowing it to:
- Cup
- Improve the grip
- Protect underlying tendons and muscles
Slow thickening and shortening of the palmar aponeurosis is a condition known as Dupuytren’s Contracture. It is more common in folks with Northern European ancestry.[11][12] (see Palmar Aponeurosis)
Image 5: Dupuytren’s Contracture.
Plantar Aponeurosis[edit | edit source]
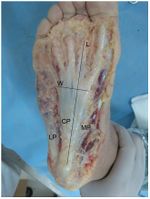
The plantar aponeurosis (PA) originates from the calcaneal tubercle and extends to the forefoot. The aponeurosis consists of a medial, central and lateral part. See Biomechanics of Plantar Fasciitis.
Function of the PA is to
- Support the foot arch [13], elevateing the foot’s medial longitudinal arch,
- Regulates movement about the ankle
- Distributes forces evenly across the foot during loading.
Image 6: Plantar Aponeurosis
References[edit | edit source]
- ↑ Arellano CJ, Gidmark NJ, Konow N, Azizi E, Roberts TJ. Determinants of aponeurosis shape change during muscle contraction. Journal of biomechanics. 2016 Jun 14;49(9):1812-7. Available:https://pubmed.ncbi.nlm.nih.gov/27155748/ (accessed 15.12.2021)
- ↑ Study.com Aponeurosis Available: https://study.com/academy/lesson/aponeurosis-definition-function.html (accessed 15.12.2021)
- ↑ Ask any difference Aponeurosis and tendon Available:https://askanydifference.com/difference-between-aponeurosis-and-tendon/ (accessed 15.12.2021)
- ↑ IMAIOS Erector spinae aponeurosis - Aponeurosis musculis erectoris spinae Available:https://www.imaios.com/en/e-Anatomy/Anatomical-Parts/erector-spinae-aponeurosis (accessed 15.12.2021)
- ↑ Creze M, Soubeyrand M, Timoh KN, Gagey O. Organization of the fascia and aponeurosis in the lumbar paraspinal compartment. Surgical and Radiologic Anatomy. 2018 Nov;40(11):1231-42.Available: https://pubmed.ncbi.nlm.nih.gov/30171298/(accessed 15.12.2021)
- ↑ Varacallo M, Scharbach S, Al-Dhahir MA. Anatomy, Anterolateral Abdominal Wall Muscles.Available:https://www.ncbi.nlm.nih.gov/books/NBK470334/ (accessed 19.12.2021)
- ↑ The free dictionary Aponeurosis of EO Available: https://medical-dictionary.thefreedictionary.com/aponeurosis+of+external+oblique+(muscle)(accessed 15.12.2021)
- ↑ Dommerholt J. Functional atlas of the human fascial system. Journal of Bodywork and Movement Therapies. 2015 Oct 1;19(4):679-80.Available:https://www.sciencedirect.com/topics/medicine-and-dentistry/aponeurosis (accessed 15.12.2021)
- ↑ Radiopedia galea Aponeurosis Available:https://radiopaedia.org/articles/galea-aponeurotica (accessed 15.12.2021)
- ↑ IMAios Bicipital aponeurosis; Lacertus fibrosus - Aponeurosis musculi bicipitis brachii; Aponeurosis bicipitalis; Lacertus fibrosus Available:https://www.imaios.com/en/e-Anatomy/Anatomical-Parts/bicipital-aponeurosis-lacertus-fibrosus (accessed 16.12.2021)
- ↑ Outlander Anatomy Plantar Aponeurosis Available: https://www.outlanderanatomy.com/fun-fact-palmar-aponeurosis/(accessed 16.12.2021)
- ↑ Ombregt L. A system of orthopaedic medicine-E-Book. Elsevier Health Sciences; 2013 Jul 25.Available: https://www.sciencedirect.com/topics/medicine-and-dentistry/aponeurosis(accessed 14.12.2021)
- ↑ Chen DW, Li B, Aubeeluck A, Yang YF, Huang YG, Zhou JQ, Yu GR. Anatomy and biomechanical properties of the plantar aponeurosis: a cadaveric study. Plos one. 2014 Jan 2;9(1):e84347.Available: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3879302/(accessed 15.12.2021)