Anticoagulants
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton
Introduction[edit | edit source]
Anticoagulant are drugs that, when aded to blood, prevents it from clotting. Anticoagulants do this by suppressing the synthesis or function of various clotting factors that are normally present in the blood. These drugs are frequently used to prevent the formation of blood clots (thrombi) in the veins or arteries or the enlargement of a clot that is circulating in the bloodstream[1]. Anticoagulants are very effective in preventing life-threatening conditions eg stroke, pulmonary embolism and myocardial infarction.
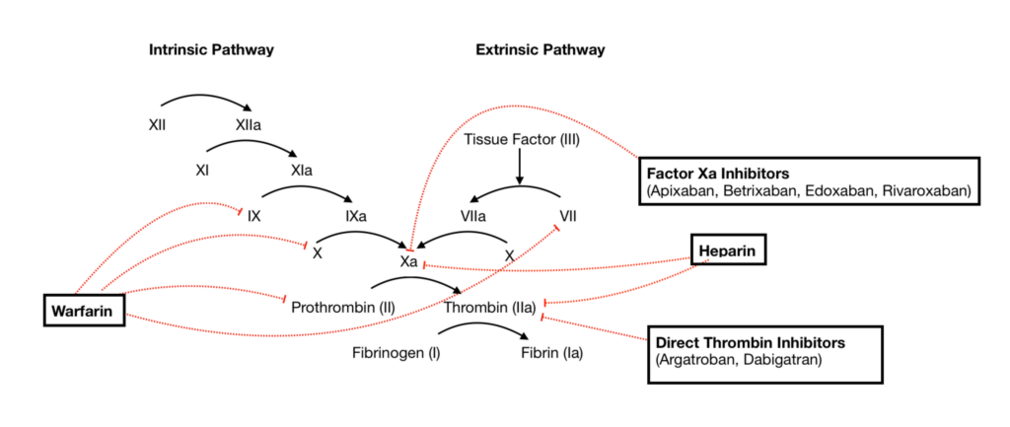
Anticoagulants come in many different forms, including injections, intravenous (IV) drugs, and oral medications, with treatment options increasing markedly over the past 10 years with the development and wide-scale availability of oral direct thrombin inhibitors and oral direct factor Xa inhibitors. Factor Xa participates in both the intrinsic and extrinsic pathways of blood coagulation). [2][3]
Clotting factors: Clotting factors are enzymes in normally present in the blood in inactive forms (all proteins, except factor IV) within the clotting cascade necessary to form cross‐linked fibrin. They were numbered in the order they were discovered.[4]eg Factor I: Clotting factor I is also known as fibrinogen, factor II is also known as prothrombin, factor IV in the clotting cascade refers to calcium, factor X is also known as Stuart factor or Stuart Prower factor.[5]
Types of Anticoagulants[edit | edit source]
Anticoagulants generally are of two types: heparin, which is given by injection, and derivatives of coumarin or indandione, which are administered orally.
- Heparin is used mainly in hospitalized patients. Heparin is an injectable anticoagulant that activates antithrombin III, which inhibits thrombin and factor Xa, factors necessary in the final stages of blood clotting cascade. There are two types of heparins: high molecular weight heparins and low molecular weight heparins.
- Coumarin derivatives are oral anticoagulants that prevent vitamin K from acting as a cofactor in the hepatic synthesis of the vitamin K-dependent coagulation factors II, VII, IX, and X (as well as the anticoagulants, proteins C and S)[6]. Derivatives of coumarin include eg Warfarin, an extremely effective anticoagulant but there are a few problems. It can interact with certain foods and can it cause serious interactions with many commonly used medicines. Regular blood monitoring (international normalized ratio-INR) is done to check for effectiveness and safety[7]
- Synthetic indandione derivatives, oral anticoagulant, a group of synthetic anticoagulants that resemble the coumarins in structure and activity and work by a similar mechanism of action.[1]
- Factor Xa inhibitors, a type of anticoagulant that work by selectively and reversibly blocking the activity of clotting factor Xa, preventing clot formation. They effect factor Xa within the blood and within a preexisting clot, and do not affect platelet aggregation. Used for the treatment and prevention of DVTs and acute PE, and to reduce the risk of stroke and embolism in people with nonvalvular atrial fibrillation.
- Thrombin inhibitors are anticoagulants that bind to and inhibit the activity of thrombin hence preventing blood clots. Thrombin inhibitors inactivate free thrombin and also the thrombin that is bound to fibrin. Used to prevent arterial and venous thrombosis and can be used to prevent and treat deep vein thrombosis or used as prophylaxis in atrial fibrillation to avoid thromboembolism[8].
Indications[edit | edit source]
Include, but not limited to:
- Deep vein thrombosis (DVT), a blood clot in the leg veins
- Pulmonary embolism (PE), a blood clot in the pulmonary blood vessels
- Acute coronary syndrome, a blood clot in the coronary arteries that causes heart attacks
- Prosthetic heart valves
- Stroke
- Left ventricular thrombus, a blood clot in the heart
- Acute limb ischemia, a blood clot in a leg artery
- Acute mesenteric ischemia, a blood clot in the artery feeding the bowel
- Atrial fibrillation, an irregular and unusually rapid heartbeat
- Hypercoagulable state, conditions that cause thick blood
Physiotherapy Implications[edit | edit source]
People on anticoagulants are also at risk for severe bleeding, especially internal bleeding, when they’re injured. Seek immediate medical attention if a client has any kind of fall where they hit the floor or an object, even if you don’t have a cut or wound they may have internal bleeding. People who take anticoagulants have a high risk of internal bleeding, especially in their brain, from falls and injuries[9].
References[edit | edit source]
- ↑ 1.0 1.1 Britannica Anticoagulants Available:https://www.britannica.com/science/anticoagulant (accessed 20.7.2022)
- ↑ Dictionary net. Factor Xa Available:http://www.dictionary.net/factor%20xa (accessed 20.7.2022)
- ↑ DeWald TA, Washam JB, Becker RC. Anticoagulants: pharmacokinetics, mechanisms of action, and indications. Neurosurgery Clinics. 2018 Oct 1;29(4):503-15. Available:https://www.sciencedirect.com/sdfe/pdf/download/eid/1-s2.0-S1042368018308660/first-page-pdf (accessed 20.7.2022)
- ↑ Steven W. Salyer PA‐C, ... Michael K. Shafé, in Essential Emergency Medicine, 2007 Available: https://www.sciencedirect.com/book/9781416029717/essential-emergency-medicine (accessed 21.7.2022)
- ↑ Phaa.com Clotting factors Available:https://www.phaa.com/clotting-factors-list-names-and-how-clots-form.htm (accessed 21.7.2022)
- ↑ Schaefer C, Peters PW, Miller RK, editors. Drugs during pregnancy and lactation: treatment options and risk assessment. Academic Press; 2014 Sep 17. Available: https://www.sciencedirect.com/science/article/pii/B9780444520722500136 (accessed 20.7.2022)
- ↑ Study.com What is Coumarin? Synthesis and Structure Available:https://study.com/academy/lesson/what-is-coumarin-structure-synthesis-derivatives.html (accessed 20.7.2022)
- ↑ Drugs.com Anticoagulants Available: https://www.drugs.com/drug-class/anticoagulants.html (accessed 21.7.2022)
- ↑ Cleveland Clinic Anticoagulants Available: https://my.clevelandclinic.org/health/treatments/22288-anticoagulants (accessed 20.7.2022)