Anterior Cruciate Ligament (ACL) Rehabilitation
Original Editors - Rachael Lowe Lieselot Longe
Top Contributors - Laura Ritchie, Riccardo Ugrin, Admin, Lieselot Longe, Evan Thomas, George Prudden, Habibu Salisu Badamasi, Kim Jackson, Tony Lowe, Scott Buxton, Claire Knott, Tarina van der Stockt, Bisoffi, Ilkje De Vlieger, Falcone Tseng, WikiSysop, Simisola Ajeyalemi, 127.0.0.1, Rucha Gadgil, Wanda van Niekerk, Jess Bell, Aminat Abolade, Naomi O'Reilly, Ines Corthals and Saeed Dokhnan
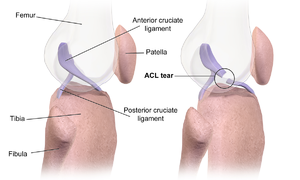
Introduction[edit | edit source]
The anterior cruciate ligament (ACL) is a key structure in the knee joint kinematics, as it resists anterior tibial translation and rotational loads. The ACL provides approximately 85% of the total restraining force of anterior translation. It also prevents excessive tibial medial and lateral rotation, as well as varus and valgus stresses[1]. Despite of that its primary role is a proprioceptive function due to the presence of mechanoreceptors in the ligaments[2]. Because of that an ACL injury might therefore be regarded as a neurophysiological dysfunction and not as a simple peripheral musculoskeletal injury.[3][4] As a consequence of its complex role in the kinematics of the knee, when an ACL injury occurs there are both clinical signs and subjective instability and therefore a comprehensive rehabilitation program is needed[5]. Injuries to the ACL are relatively common knee injuries among athletes[6] and females are two to eight times more likely to sustain an ACL injury than their male counterparts[7][8].
The injuries can range from mild (such as small tears/sprain) to severe (when the ligament is completely torn)[9]. When an ACL has a complete rupture and there are clinical and subjective signs of instability, a surgical reconstruction is needed. However it is not self-evident that an ACL Reconstruction will automatically lead to a return to preinjury activity level.
ACL rehabilitation is both for conservative and surgical option.
Please see these pages for relevant ACL Injuries
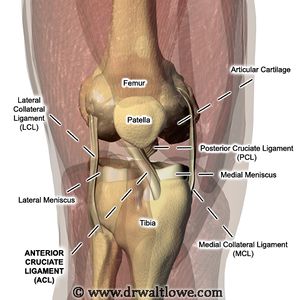
Clinically Relevant Anatomy[edit | edit source]
The anterior cruciate ligament (ACL) is a band of dense connective tissue which courses from the femur to the tibia. The ACL arises from the posteromedial corner of the medial aspect of the lateral femoral condyle in the intercondylar notch and inserted anterior to the intercondyloid eminence of the tibia, blending with the anterior horn of the medial meniscus. The ACL courses anteriorly, medially, and distally across the joint as it passes from the femur to the tibia. As it does, it turns on itself in a slight outward (lateral) spiral.
The density of blood vessels within the ligaments is not homogeneous. In the ACL, an avascular zone is located within the fibrocartilage of the anterior part where the ligament faces the anterior rim of the intercondylar fossa[10]. The coincidence of poor vascularity and the presence of fibrocartilage is also seen in gliding tendons in areas that are subjected to compressive loads, plays a role in the poor healing potential of the ACL.[11]
Please see these pages for relevant anatomy: Anterior Cruciate Ligament (ACL) and Anterior Cruciate Ligament (ACL) - Structure and Biomechanical Properties
General Considerations[edit | edit source]
ACL rehabilitation has undergone considerable changes over the past decade. Intensive research into the biomechanics of the injured and the operated knee have led to a movement away from the techniques of the early 1980's characterized by post operative casting, delayed weight bearing and limitation of Range of Motion (ROM), to the current early rehabilitation program with immediate training of ROM and weight bearing exercises[5].
The ACL rehabilitation is both for conservative and surgical options. Conservative treatment of an ACL injury could be the best choice for sedentary patients. Indeed patient age, sportive activities and foremost subjective instability symptoms in daily life activities should be considered when deciding for or against ACL reconstruction[12][13]. In those cases a physiotherapic program of complete re-gain of ROM, a comprehensive program of reinforce and restore of proprioception and a normal gait pattern training could be the best rehabilitation protocol. However if symptomatic instability of the knee is not reduced after physiotherapy nor after adjustment of activity, anterior cruciate ligament reconstruction is recommended. This might prevent multiple interventions because of further meniscal and cartilage damage[14].
It is useful to remember that injuries to the ACL rarely occur in isolation. The presence and extent of other injuries may affect the way in which the ACL injury is managed. Indeed the mechanism of injury can damage also the Medial Collateral Ligament (MCL) or the meniscus. Other associated injuries could be microfractures or bone contusions, both with or without chondral injuries.[15][16]In those cases the ACL Rehabilitation program must be not standardize and consider the comorbidity.
The major goals of general rehabilitation of the ACL-injured knee:
- Gain full ROM of the knee
- Repair muscle strength and proprioception
- Gain in good functional stability
- Reach the best possible functional level (walking, running, jumping...)
- Decrease the risk for re-injury
- (Return to sport)
Phases of ACL rehabilitation[edit | edit source]
The physiotherapy intervention could be divided in phases:
- Acute Stage
- Pre-surgical Stage or Conservative Treatment
- Post-surgical Stage
- Return to sport
Acute Stage[edit | edit source]
After an ACL injury, regardless of whether surgery will take place or not, physiotherapy management focuses on regaining range of movement, strength, proprioception and stability. In the acute stage PRICE or PEACE AND LOVE should be used in order to reduce swelling and pain, to attempt full range of motion and to decrease joint effusion. Appropriate anti-inflammatory medications are used to help control pain and swelling[5].
The indication of use crutches and eventually a knee immobilizer could be appropriate in some patients. However extended use of the knee immobilizer should be limited to avoid quadriceps atrophy[14].
The neuro-muscular inhibition of the quadriceps caused by intrarticular effusion may have a negative effect on the strengthening. In any case exercises should encourage range of movement, initial strengthening of the quadriceps and hamstrings, and eventually proprioception[5][14]. In fact, strength and proprioceptive alterations occur in both the injured and uninjured limb[17]. To assist pre-operative optimisation, the following guidelines are recommended in the acute and early sub acute stages post injury:[18][19] [20]
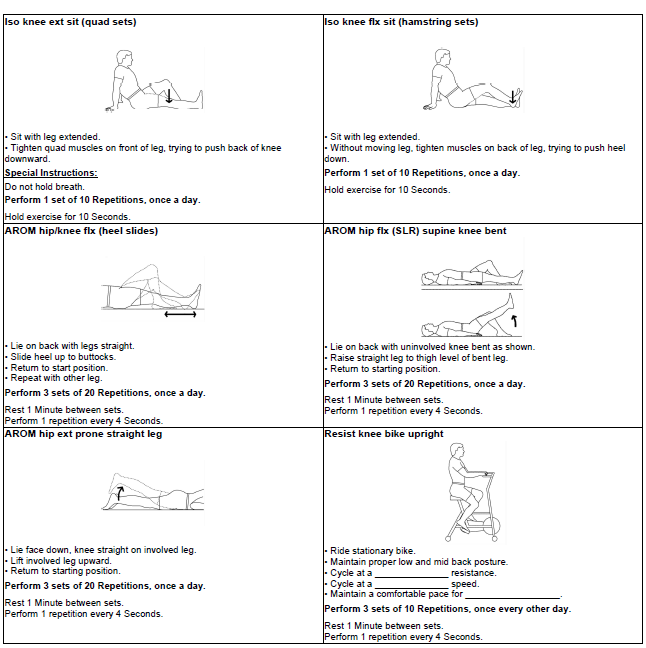
- Full extension is obtained by doing:
- Passive knee extension: the physiotherapist can provide the passive knee extension both with manual therapy and teaching exercises adding leverage to gently force extension,
- Patellar self-mobilisations,
- Heel Props,
- Prone hang exercise,
- Static quads/SLR;
- Bending (Flexion) is obtained by doing:
- Passive knee bend: the physiotherapist can provide the passive knee flexion both with manual therapy and teaching exercises adding leverage to gently force flexion,
- Knee flexion in prone (gentle kicking exercises),
- Wall slides,
- Heel slides;
- Knee flexion/extension in sitting;
- Ankle DF/PF/circumduction;
- Glutes medius work in side lying;
- Gluteal exercises in prone;
- Weight transfers in standing (forwards/backwards, side/side).
It is also demonstrated that Neuromuscular Electrical Stimulation (NMES) combined with exercise is more effective in improving quadriceps strength than exercise alone[21].
It could be useful also to consider taping to provide stability and to encourage reduction in swelling[22].
There is not a clear-cut transition from the Acute stage to the Pre-operative stage, each stage could last some days or several months before surgery. Didactically the end of the acute stage occurs when the patient regains the full range of motion of the knee in extension and at least 110 degrees of flexion or a near-normal gait pattern.
Before Surgical Stage[edit | edit source]
THE HIGHEST INCIDENCE OF KNEE STIFFNESS OCCURS IF ACL SURGERY IS PERFORMED WHEN THE KNEE IS SWOLLEN, PAINFUL, AND HAS A LIMITED RANGE OF MOTION.
The risk of developing a stiff knee after surgery can be significantly reduced if the surgery is delayed until the acute inflammatory phase has passed, the swelling has subsided, a normal or near normal range of motion (especially extension) has been obtained, and a normal gait pattern has been reestablished[23]. However actual guidelines[14] [5]concord that the indication for a reconstruction is persistent instability of the knee with complaints of giving way. This diagnosis is difficult to make in an acute situation. The guidelines recommend that ACLR should not be performed in the first weeks after trauma, in order to minimize the risk of operating on an asymptomatic patient.
As soon as the Acute Stage is over, it is important to prepare the knee for surgery as well as possible to optimise the outcome. The focus needs to be on strength and proprioception. Despite this, the physiotherapist must keep the injured knee in a quiescent state improving range of motion with minimal swelling.
RICE and electrotherapy can be applied during several weeks ahead of the surgery in order to obtain full range of motion and to decrease joint effusion. The patient should also have a normal gait pattern: because of that it is useful analyse the motion of the leg both in the swing phase of walking and in the one-leg-standing phase . Thus will help the patient to regain faster motion and strength after the surgery[24].
The length of this pre-surgical stage can last a few days or several weeks. Because of this, the role of the physiotherapist is also to maintain the compliance of the patient. For this reason, the rehabilitation program must have measurable weekly objectives to improve muscular strength and conditioning, to gain range of motion and to get better on proprioception. This will provide new goals to be reached week by week: the compliance for treatment will be maintained by the patient achieving these goals[25].
During the pre-surgical stage is it important to offer different way to reinforce muscular strength and proprioception. Because of that it could be a good solution to give to the patient two different plans of exercises to do in the gym and at home. However it is very important to give to the injured knee sub-maximal loads to avoid knee swelling or re-injuring caused by lack of proprioception.
- Obtain and mantain full range of motion in extension and keep improving range of motion in flexion with minimal swelling;
- Develop muscle strength: Once 110 degrees of flexion has been achieved work may begin to work on muscular strength. Examples of exercises are:
- Swimming (avoid breaststroke),
- Low impact exercise machines such as an elliptical cross-trainer, Stationary Bicycle and treadmill,
- Leg press machine,
- Leg curl machine or Leg Extension machine, (see Open-Kinetic-Chain below)
- Weight bearing exercises such as squats, lunges, steps up, (see Closed-Kinetic-Chain exercises below);
- Improve proprioception:
- One-leg- standing exercise
- One-leg standing exercise adding balance cushions or cues for the arms (throwing or catching a ball, reaching targets...)
- One-leg standing exercise in different planes (frontal, sagittal)
- Preparation for controlled jumps;
- Keep the compliance to rehabilitation program high[25];
- Mental preparation: Patient must know what to expect of the surgery and understand the rehabilitation phases after surgery.[18][26]
After Surgery[edit | edit source]
Please see these page for relevant ACL Rehabilitation: Acute Management after Surgery
ACL Reconstruction has undergone considerable changes over the past decade.Various tissues/graft have been used to anatomically reconstruct the torn ACL. The most commonly used are autografts (patellar bone & hamstring) and sometimes allografts (taken from cadavers). The process of "ligamentization" of the grafts needs precautions in terms of loading and physical requests.[27] However it seems indicated that the remodeling of the new ACL is a process that continues for 9 years or more. Furthermore, it seems to be a process of adaptation rather than full restoration.[28] Despite this there are no substantial differences in the physiotherapic approach during After Surgery Stage between grafts.
Consider pain, swelling, muscular contracture, limitation in range of motion and abnormal gait patterns as indicators for having a good outcome. In the After Surgery Stage three factors are important:
- Early terminal knee extension equal to the contralateral side,
- Early weight bearing,
- Closed and Open Kinetic Chain strengthening exercises.
Early knee extension establishes the foundations for the entire rehabilitation program.
The incidence of knee flexion contracture with associated quadriceps weakness and extensor mechanism dysfunction following ACL reconstruction has significantly decreased with accelerated knee extension immediately after surgery.
In accordance with the ACL Rehabilitation Guidelines a good physiotherapic program is dependent on achieving goals week by week.
Week 1[edit | edit source]
- Regular icing and elevation are used to reduce swelling[29][30][31]. Eventually medications or pain-killers according to MD to attempt rehabilitation goals.
- The goal is full extension and 70 degrees of flexion by the end of the first week.
- Use a knee brace and crutches in agreement with the surgeon and only if needed. Infact the wearing of a knee brace has no additional treatment value after an ACL reconstruction[32]. The use of the knee brace is progressively reduced by authors.[24][19] Postoperative rehabilitative bracing either in extension or with the hinges opened for ROM does not offer significant advantages over no bracing.[33] The need for postoperative functional bracing and for consensus involving the duration of the bracing in many rehabilitation protocols comes into question. Harilainen et al have compared the effects of functional bracing after ACL reconstruction with patellar graft against not bracing post- operatively. No significant difference in functional outcome, degree of stability, or isokinetic muscle torque was detected at 1 and 2 yrs postoperatively between the two groups[34]. In a similar study, Risberg et al found no significant differences in knee-joint laxity, range of motion, muscle strength, functional knee tests, or pain. [33]
- Multidirectional mobilizations of the patella should be included for at least 8 weeks. Other mobilization exercises in the first 4 weeks are passive extension of the knee (no hyperextension) and passive and active mobilization towards flexion.
- Strengthening exercises for the calf muscle, hamstring and quadriceps (vastus medialis) can be performed supine or prone.
- Isometric quadriceps exercises are safe from the first postoperative week 1[35]
Early weight bearing appears beneficial and may decrease patellofemoral pain. Early motion is safe and may help avoid problems with later arthrofibrosis. Continuous passive motion is not warranted to improve rehabilitation outcome in patients. Minimally supervised physical therapy in selected motivated patients appears safe without significant risk of complications[5].
| ACL Reconstruction: Rehab Program Seminar[36] | Heel Raises For ACL Reconstruction[37] |
Week 3-4[edit | edit source]
- There is no evidence that icing and elevation is useful after Week 1.
- The first goal is maintain full extension and increase degrees of flexion week by week.
- Try to genuinely increase the stance phase in an attempt to walk with one crutch. With good hamstring/quadriceps control, the use of crutches can be reduced earlier.
- Strengthening exercises for the calf muscle, hamstring and quadriceps (vastus medialis) can be performed sitting using a stationary bicycle or light weights . The progress of the exercise depends on pain, swelling and quadriceps control.
- Starting eccentric quadriceps training (in CKC) from 3 weeks after ACLR is safe and contributes to a bigger improvement in quadriceps strength than concentric training[38]
- In some patient with good hamstring/quadriceps control it is possible to genuinely attempt some exercise in Closed Kinetic Chain (half-squats, hip hinges, calfs, step up...). Usually those exercise are performed by patients who trained for a long period in a good pre-surgical stage program.
Quadriceps strength is enhanced with early extension and weight bearing. The combination of early knee extension, early weight bearing, and closed kinetic quadriceps strengthening allows the patient to progress through the post-operative rehabilitation period at a rather rapid pace without compromising ligamentous stability.[18]
Week 5[edit | edit source]
- Passive mobilizations should normalize motility but flexion should not yet be thorough.
- Tonification of hamstrings and quadriceps can start with more intensity both in open and close chain exercises. The exercises should be started on light intensity (50% of maximum force) and now progressively increased to 60-70%. The closed chain exercises should be built from less responsible positions (leg presses, step) to more congested starting positions (ex.squad). The progress of the exercise depends on pain, swelling and quadriceps control.
- Proprioception and coordination exercises can evolve if the general strength is good. This includes balance exercises on boards and toll.
Postoperative phase 1 ( 1-5 weeks)[edit | edit source]
Possible example for exercises to teach self-mobilisations of the knees and strength for quadriceps and hamstrings:
| Week 1: Self Mobilization[39] | Week 3: Strengthening exercises and gait training[40] | Week 5: Strengthening exercises [41] |
| Week 10: Forward, backward and lateral dynamic exercises[42] | Week 12: Forward, backward and lateral dynamic exercises[43] | Week 15: Sprinting, jumping, cutting [44] |
Week 10[edit | edit source]
- The progression of loading is the fundamental from now on.
- The proprioception and coordination exercise could be more specific to the individual sporting needs of the patient. If the patient does not wish to return to sport these exercises fulfill his ADL needs (climbing stairs, walking uphill or downhill, skating, swimming...)
- Forward, backward and lateral dynamic movements can be included as well as isokinetic exercises[19].
Month 3[edit | edit source]
- After 3 months the patient can move on to functional exercises such as running and jumping.
- As proprioceptive and coordination exercises become more intense, faster changes in direction are possible. To stimulate coordination and control through afferent and efferent information processing, exercises should be enhanced by variation in visible input, surface stability (trampoline), speed of exercise performance, complexity of the task, resistance, one or two-legged performance, etc.[19].
Month 4-5[edit | edit source]
- The final goal is to maximize endurance and strength of the knee stabilizers, optimize neuromuscular control with plyometric exercises and to add the sport-specific exercises.
- Acceleration and deceleration, variations in running and turning and cutting manoeuvres improve arthrokinetic reflexes to prevent new trauma during competition.[20]
Return to Activities[edit | edit source]
- Before returning to driving its recommended patient can safely activate the brake in a simulated emergency. Typically, this will be at approximately 4–6 weeks after right-sided ACLR and approximately 2–3 weeks after leftsided ACLR.[45]
- Before returning to running, its recommended for the patients, to achieved 95% knee flexion range of motion (ROM), Full extension ROM, no effusion/trace of effusion. no limb symmetry index (LSI)>80% for quadriceps strength, LSI>80% eccentric impulse during counter movement jump, pain-free repeated single-leg hopping (‘pogos’), pain-free aqua jogging and alter-G running.[45]
Return to Sport[edit | edit source]
An ACL injury leads to static and functional instability that causes changes in motion patterns and an increased risk of osteoarthrosis. In many cases, an ACL injury results in a premature end to a career in sports. [46]
|
ACL Return to Sport: Hop Test|[47] |
Strength and power deficits after surgery may be a risk factor for future injuries and may set athletes up for failure when they try to return to their prior performance levels. Researchers suggest that the surgically repaired leg should perform at least 90% as well as the uninjured leg before you return to sport[48]. Three hopping tests can be used as part of a comprehensive physical and functional examination to help ensure not just a speedy, but a safe return to sport after ACL reconstruction. These 3 tests are sensitive enough to measure side-to-side differences and can be used during more advanced recovery phases after surgery to help ensure that the athlete’s exercise program is successful in returning the injured leg at least to the level of the uninjured leg[48].
Athletes who undergo ACL reconstruction should be informed that postoperative participation in level I sports increases the 2-year knee reinjury rate more than four times. A later return to level I sports and more symmetrical quadriceps strength prior to return decreases this rate significantly[49].
As strength and conditioning grow, the mechanism of previous injury can guide the last phases of rehabilitation: an ACLR due to an indirect mechanism of injury could point the focus on coordination exercises between ankle-knee-hip, or on core-stability, or on sport specific gesture.
Please see these pages for relevant Return to Play in Sports
Open versus Closed Kinetic Chain Exercise[edit | edit source]
Closed kinetic chain exercises (CKC) and Open kinetic chain exercises (OKC) play an important role in regaining muscle (quadriceps, hamstrings) strength and functional knee stability.
- CKC exercises became more popular than OKC exercises in ACL rehabilitation. Some clinicians believed that CKC exercises were safer than OKC exercises because they place less strain on the ACL graft. Besides, they also believed that CKC exercises are more functional and equally effective as OKC exercises. Bynum et al. (1995) concludes that CKC exercises are safe, effective, and sacrifice some important advantages over OKC exercises. [50]
- A study that compared the amount of anterior tibial displacement in the ACL-deficient knee during (1) resisted knee extension, an OKC-exercise and (2) the parallel squat, a CKC-exercise, concluded that the ACL-deficient knee had significantly greater anterior tibial displacement during extension from 64° to 10° in the knee extension exercise as compared to the parallel squat exercise[51].
- But in one study no difference in strain was found on the intact ACL between OKC and CKC exercises[52].
- Currently, ACL grafts may respond more like the intact ACL. Therefore they argue, both types of exercise could be done safety[19].
- However a study that examined the effect of OKC and CKC exercises on functional activity concludes that both OKC and CKC programs lead to an equal long-term good functional outcome[53].
- In another study, group 1 carried out quadriceps strengthening only with CKC while group 2 trained with CKC plus OKC exercises starting from week 6 after surgery[54] It seemed that the addition of OKC quadriceps training after ACL reconstruction results in a significantly stronger quadriceps without reducing knee joint stability at 6 months and also leads to a significantly higher number of athletes returning to their previous activity earlier and at the same level as before injury. The authors conclude that the combination of OKC and CKC exercises is more effective than CKC exercises alone[55].
- The use of a bone-patella-tendon-bone autograft has a greater chance of giving anterior knee pain than the use of a hamstring autograft. Because of that the type of autograft can guide the physiotherapist choosing the right period in which insert OKC sitting-leg-extension. It would be earlier in case of hamstring graft, and some week later in case of the patellar tendon graft. Guidelines are agree about insert OKC exercises not before 4 weeks after surgery[5][14].
- In any case it is important to follow the progression of loads for the knee to not provoke pain or laxity. A more recent systematic review[56] of RCTs comparing OKC vs CKC exercises in patients post-ACLR has found that:
- There is no or insufficient evidence to demonstrate difference between OKC & CKC for pain scores or joint laxity
- the former could be explained by (1) lack of sensitivity with used questionnaire, (2) statistical power of analysis was insufficient, or (3) there is actually no difference in pain experienced by patients undertaking OKC vs CKC
- "There is weak evidence that open chain exercises are better for improving knee extensor strength, this is countered by weak evidence for better active knee flexion in closed chain activities."
- There is no or insufficient evidence to demonstrate difference between OKC & CKC for pain scores or joint laxity
Open-Kinetic-Chain exercises:[edit | edit source]
Characteristics[edit | edit source]
- Non-weight bearing
- Movement occurring at a single joint: isolation movements that promote more shearing forces[51]
- Distal segment free to move
- Resistance is usually applied to the distal segment
Open-Kinetic-Chain Knee-Extension exercises[edit | edit source]
These exercises seems to have a controversial role in ACL rehabilitation programs, because some research showed that OKC-extension exercises from 60° to 0° flexion, markedly increase anterior tibial translation in the ACL-deficient knee, as well as ACL graft strain in the reconstructed knee.[24] Despite these findings, OKC-extension exercises aren’t excluded in ACL-rehabilitation programs, because the same research had shown that OKC-extension exercises from 90° to 60° of flexion could be done safe, without increasing anterior tibial translation or ACL graft strain.[24]
In short, OKC-extension exercises in ACL rehabilitation programs could be done safe in a ROM from 90° to 60° flexion and are furthermore useful to train the quadriceps isolated.
Open-Kinetic-Chain Knee-Flexion exercises[edit | edit source]
OKC-flexion exercises play an important part in the rehabilitation process because research showed that there is no anterior tibial translation or ACL graft strain during these exercises. Besides, they result in isolated hamstrings muscle contraction.[50]
Closed-Kinetic-Chain Knee exercises[edit | edit source]
Characteristics[edit | edit source]
- Weight bearing
- Movement at several joints: compound movements that generally incur compressive forces[51]
- Distal segment fixed to a surface: the extremity remains in constant contact with the immobile surface, usually the ground[57]
- Resistance may be applied both proximally and distally: the entire limb is loaded[57].
Closed-Kinetic-Chain Knee exercises[edit | edit source]
CKC exercises play an important role in ACL rehabilitation because they result in a hamstrings-quadriceps co-contraction that reduces tibiofemoral shear forces. Besides, research showed that during CKC exercises body weight provides tibiofemoral joint compression, that also reduces tibiofemoral shear forces .[51]
CKC exercises have several advantages compared with OKC exercises
- Increase stability in the knee joint (more joint compression)
- Functional load
- Strong coordinative training
- Minimal shear force
- Less stress on the ACL
- Training of the entire extension chain [58]
- No selective muscle training
- Weakest link in the chain is feeling the most "overload" and the corresponding largest trainings effect
- Fewer complications such as patellofemoral symptoms
- CKC-exercises are earlier to apply than OKC-exercises
Other Considerations[edit | edit source]
In a retrospective, cross-sectional analysis conducted by Culvenor et al.[59]. 30% of patients had patellofemoral pain (PFP) 12-15 months following ACLR using a hamstring graft. Those who were 27 and older were 2.6 times more likely to report PFP. Patellofemoral cartilage lesions, mensical tears (both assessed by arthroscopy), pre-injury activity level, time from injury to surgery and sex were not predictors of post-operative PFP.
Those who had PFP did not have reduced range of movement but performed worse at hop distance and single leg tasks. Patients also reported significantly lower quality of life, poor returning sport attitudes and increased kinesiophobia.
PFP is important to consider as maladaptive, fear avoidance patterns of movement perpetuate pain and functional disability by lowering pain experience thresholds. The use of appropriate language during rehab and psychosocial interventions are recommended.
Hamstring strength loss after ACL Surgery[60]
Resources[edit | edit source]
Melbourne ACL Rehabilitation Guide
Knee Stability and Movement Coordination Impairments: Knee Ligament Sprain Revision 2017
References[edit | edit source]
- ↑ Matsumoto, H., Suda, Y., Otani, T., Niki, Y., Seedhom, B. B., Fujikawa, K. (2001). Roles of the anterior cruciate ligament and the medial collateral ligament in preventing valgus instability. J Orthop Sci, 6(1), 28-32.
- ↑ Singh JK, Verma A.Prevention of Anterior Cruciate Ligament (ACL) Injury and Enhance Performance Program. IJRAR-International Journal of Research and Analytical Reviews (IJRAR). 2020 Feb;7(1):715-27.
- ↑ Courtney CA, Rine RM. Central somatosensory changes associated with improved dynamic balance in subjects with ACL deficiency. Gait Posture 2006;24:190–5.
- ↑ Kapreli E, Athanasopoulos S, Gliatis J, et al. ACL deficiency causes brain plasticity: a functional MRI study. Am J Sports Med 2009;37:2419–26.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 van Melick N, van Cingel REH, Brooijmans F, et al Evidence-based clinical practice update: practice guidelines for anterior cruciate ligament rehabilitation based on a systematic review and multidisciplinary consensus British Journal of Sports Medicine 2016;50:1506-1515.
- ↑ Nagano Y, Ida H, Akai M, Fukubayashi T. Biomechanical characteristics of the knee joint in female athletes during tasks associated with anterior cruciate ligament injury. The Knee. 2009 Mar 1;16(2):153-8.
- ↑ Myer GD, Sugimoto D, Thomas S, et al. The influence of age on the effectiveness of neuromuscular training to reduce anterior cruciate ligament injury in female athletes: a meta-analysis. Am J Sports Med 2013;41:203–15
- ↑ Yoo JH, Lim BO, Ha M, et al. A meta-analysis on the effect of neuromuscular training on the prevention of the anterior cruciate ligament injury in female athletes. Knee Surg Sports Traumatol Arthrosc 2010;18:824–30.
- ↑ William E.Prentice, Rehabilitation techniques for sports medicine and athletic training; fourth ed. McGraw Hill publications.
- ↑ Petersen, W., Tillmann, B. (1999). Structure and vascularization of the cruciate ligaments of the human knee joint. Anat Embryol (Berl), 200(3), 325-334.
- ↑ Petersen, W., Tillmann, B. (1999). Structure and vascularization of the cruciate ligaments of the human knee joint. Anat Embryol (Berl), 200(3), 325-334.
- ↑ Konrads C, Reppenhagen S, Belder D, Goebel S, Rudert M, Barthel T. Long-term outcome of anterior cruciate ligament tear without reconstruction: a longitudinal prospective study. Int Orthop. 2016 Nov;40(11):2325-2330.
- ↑ Mall NA, Frank RM, Saltzman BM, Cole BJ, Bach BR Jr. Results After Anterior Cruciate Ligament Reconstruction in Patients Older Than 40 Years: How Do They Compare With Younger Patients? A Systematic Review and Comparison With Younger Populations. Sports Health. 2016 Mar-Apr;8(2):177-81.
- ↑ 14.0 14.1 14.2 14.3 14.4 Meuffels DE, Poldervaart MT, Diercks RL, Fievez AW, Patt TW, Hart CP, Hammacher ER, Meer Fv, Goedhart EA, Lenssen AF, Muller-Ploeger SB, Pols MA, Saris DB. Guideline on anterior cruciate ligament injury. Acta Orthop. 2012 Aug;83(4):379-86.
- ↑ Yoon KH, Yoo JH, Kim KI.J. fckLRBone contusion and associated meniscal and medial collateral ligament injury in patients with anterior cruciate ligament rupture. Bone Joint Surg Am. 2011 Aug 17;93(16):1510-8.
- ↑ Shekhar¹ A, Singh¹ A, Laturkar¹ A, Tapasvi¹ S. Anterior Cruciate Ligament Rupture with Medial Collateral Ligament Tear with Lateral Meniscus Posterior Root Tear with Posterolateral Tibia Osteochondral Fracture: A New Injury Tetrad of the Knee. Journal of Orthopaedic Case Reports. 2020 May;10(3):36-42.
- ↑ Suter E, Herzog W, Bray R. Quadriceps activation during knee extension exercises in patients with ACL pathologies. Journal of Applied Biomechanics. 2001;17: 87-102.
- ↑ 18.0 18.1 18.2 Dr. P. J. Millett et al. ACL Reconstruction Rehabilitation Protocol. Sports Medicine and Orthopaedic Surgery 2010.
- ↑ 19.0 19.1 19.2 19.3 19.4 S. van Grinsven, R. E. H. van Cingel, C. J. M. Holla, C. J. M. van Loon. Evidence-based rehabilitation following anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 2010; 18:1128–1144
- ↑ 20.0 20.1 Savio L-Y. Woo, Richard E. Debski, PhD, John D. Withrow, Marsie A. Janaushek. Biomechanics of Knee Ligaments. The American Journal of Sports medicine 1999;27:533
- ↑ Kyung-Min KiM, Ted Croy, Jay HerTel, SuSan Saliba. Effects of Neuromuscular Electrical Stimulation After Anterior Cruciate Ligament Reconstruction on Quadriceps Strength, Function, and Patient-Oriented Outcomes: A Systematic Review. JOSPT, 2010;40(7):383-391.
- ↑ Balki S, Göktaş HE, Öztemur Z. Kinesio taping as a treatment method in the acute phase of ACL reconstruction: A double-blind, placebo-controlled study. Acta Orthop Traumatol Turc. 2016;50(6):628-634.
- ↑ Duncan KJ, Chopp-Hurley JN, Maly MR. A systematic review to evaluate exercise for anterior cruciate ligament injuries: does this approach reduce the incidence of knee osteoarthritis? Open Access Rheumatol. 2016 Jan 8;8:1-16
- ↑ 24.0 24.1 24.2 24.3 I Eitzen, H Moksnes, L Snyder-Mackler, MA Risberg. Progressive 5-Week Exercise Therapy Program Leads to Significant Improvement in Knee Function Early After Anterior Cruciate Ligament Injury. JOSPT, 2010;40(11):705-722
- ↑ 25.0 25.1 Della Villa F, Andriolo L, Ricci M, Filardo G, Gamberini J, Caminati D, Della Villa S, Zaffagnini S. Compliance in post-operative rehabilitation is a key factor for return to sport after revision anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2020 Feb;28(2):463-469.
- ↑ Cascio B, Culp L, Cosgarea A (2004) Return to play after anterior cruciate ligament reconstruction. Clin Sports Med 23:395–408
- ↑ Pauzenberger L, Syré S, Schurz M. "Ligamentization" in hamstring tendon grafts after anterior cruciate ligament reconstruction: a systematic review of the literature and a glimpse into the future. Arthroscopy. 2013 Oct;29(10):1712-21.
- ↑ Mayr HO, Stoehr A, Herberger KT, Haasters F, Bernstein A, Schmal H, Prall WC. Histomorphological Alterations of Human Anterior Cruciate Ligament Grafts During Mid-Term and Long-Term Remodeling. Orthop Surg. 2021 Feb;13(1):314-320
- ↑ Everhart JS, Best TM, Flanigan DC. Psychological predictors of anterior cruciate ligament reconstruction outcomes: a systematic review. Knee Surg Sports Traumatol Arthrosc 2015;23:752–62.
- ↑ Wierike SC, van der Sluis A, van den Akker-Scheek I, et al. Psychosocial factors influencing the recovery of athletes with anterior cruciate ligament injury: a systematic review. Scand J Med Sci Sports 2012;23:527–40.
- ↑ Gobbi A, Francisco R. Factors affecting return to sports after anterior cruciate ligament reconstruction with patellar tendon and hamstring graft: a prospective clinical investigation. Knee Surg Sports Traumatol Arthrosc 2006;14:1021–8.
- ↑ Wright R W, Fetzer G B. Bracing after ACL reconstruction: a systematic review. Clin Orthop 2007; (455): 162-8.
- ↑ 33.0 33.1 Rick W. Wright et al. ACL Reconstruction Rehabilitation: A Systematic Review Part I. J Knee Surg. 2008;21(3): 217–224.
- ↑ Harilainen, A. and Sandelin, J. (2006), Post-operative use of knee brace in bone–tendon–bone patellar tendon anterior cruciate ligament reconstruction: 5-year follow-up results of a randomized prospective study. Scandinavian Journal of Medicine & Science in Sports, 16: 14-18.
- ↑ Isberg J, Faxén E, Brandsson S, et al. Early active extension after anterior cruciate ligament reconstruction does not result in increased laxity of the knee. Knee Surg Sports Traumatol Arthrosc 2006;14:1108–15
- ↑ ACL Reconstruction: Rehab Program Essentials Seminar. Available from: http://www.youtube.com/watch?v=Yp4eYFald-g&t=3507s
- ↑ Heel Raises For ACL Reconstruction. Available from: http://www.youtube.com/watch?v=8HjkdVfmRkI&t=56s
- ↑ Gokeler A, Bisschop M, Benjaminse A, et al. Quadriceps function following ACL reconstruction and rehabilitation: implications for optimization of current practices. Knee Surg Sports Traumatol 2014;22:1163–74.
- ↑ Mike Henkelman. ACL Rehab Forum: Therapy - Week 1. Available from: http://www.youtube.com/watch?v=n5AG4eaTS-A [last accessed 04/10/14]
- ↑ Mike Henkelman. ACL Rehab Forum: Therapy - Week 3. Available from: http://www.youtube.com/watch?v=6fGhPKUI0Us [last accessed 04/10/14]
- ↑ Mike Henkelman. ACL Rehab Forum: Therapy - Week 5. Available from: http://www.youtube.com/watch?v=NbFzjZAri-w [last accessed 04/10/14]
- ↑ Mike Henkelman. ACL Rehab Forum: Therapy - Week 10. Available from: http://www.youtube.com/watch?v=uibgRUgKNeQ [last accessed 04/10/14]
- ↑ Mike Henkelman. ACL Rehab Forum: Therapy - Weeks 12-13. Available from: http://www.youtube.com/watch?v=V1hg7sBH67U [last accessed 04/10/14]
- ↑ Mike Henkelman. ACL Rehab Forum: Therapy - Week 15. Available from: http://www.youtube.com/watch?v=NR8pINSvlag [last accessed 04/10/14]
- ↑ 45.0 45.1 Kotsifaki R, Korakakis V, King E, Barbosa O, Maree D, Pantouveris M, Bjerregaard A, Luomajoki J, Wilhelmsen J, Whiteley R. Aspetar clinical practice guideline on rehabilitation after anterior cruciate ligament reconstruction. British Journal of Sports Medicine. 2023 May 1;57(9):500-14.
- ↑ Kvist J. Rehabilitation Following Anterior Cruciate Ligament Injury Current Recommendations for Sports Participation. Sports Medicine 2004: 269-267.
- ↑ Atlantic Physical Therapy Center. ACL level 4 Test. Available from: http://www.youtube.com/watch?v=dEdr3Of8tUk[last accessed 04/10/14]
- ↑ 48.0 48.1 Gregory D. Myer, Laura C. Schmitt, Jensen L. Brent, Kevin R. Ford, Kim D. Barber Foss, Bradley J. Scherer, Robert S. Heidt Jr., Jon G. Divine, Timothy E. Hewett.Utilization of Modified NFL Combine Testing to Identify Functional Deficits in Athletes Following ACL Reconstruction. J Orthop Sports Phys Ther 2011;41(6):377-387.
- ↑ Grindem H, Snyder-Mackler L, Moksnes H, et al Simple decision rules can reduce reinjury risk by 84% after ACL reconstruction: the Delaware-Oslo ACL cohort study British Journal of Sports Medicine 2016;50:804-808.
- ↑ 50.0 50.1 EB. Bynum et al. Open Versus Closed Chain Kinetic Exercises After Anterior Cruciate Ligament Reconstruction: A Prospective Randomized Study. Am J Sports Med. 1995; 23:401-406.
- ↑ 51.0 51.1 51.2 51.3 Graham VL. et al. Electromyographic evaluation of closed and open kinetic chain knee rehabilitation exercises. J Athl Train 1993;28(1):23-30.
- ↑ Keays SL, Sayers M, Mellifont DB, Richardson C. Tibial displacement and rotation during seated knee extension and wall squatting: a comparative study of tibiofemoral kinematics between chronic unilateral anterior cruciate ligament deficient and healthy knees. Knee. 2013 Oct;20(5):346-53.
- ↑ Perriman A, Leahy E, Semciw AI. The Effect of Open- Versus Closed-Kinetic-Chain Exercises on Anterior Tibial Laxity, Strength, and Function Following Anterior Cruciate Ligament Reconstruction: A Systematic Review and Meta-analysis. J Orthop Sports Phys Ther. 2018 Jul;48(7):552-566.
- ↑ Heijne A, Werner S. Early versus late start of open kinetic chain quadriceps exercises after ACL reconstruction with patellar tendon or hamstring grafts: a prospective randomized outcome study. Knee Surg Sports Traumatol Arthrosc. 2007;15:402–414
- ↑ Glass, Rebekah et al. “The Effects of Open versus Closed Kinetic Chain Exercises on Patients with ACL Deficient or Reconstructed Knees: A Systematic Review.” North American journal of sports physical therapy : NAJSPT vol. 5,2 (2010): 74-84.
- ↑ Jewiss D, Ostman C, Smart N. Open versus Closed Kinetic Chain Exercises following an Anterior Cruciate Ligament Reconstruction: A Systematic Review and Meta-Analysis. Journal of Sports Medicine. 2017;2017.
- ↑ 57.0 57.1 Prof. dr. P. Vaes. Tekstboek: Onderzoek en behandeling deel IIA 2016
- ↑ Prof. dr. P. Vaes. Tekstboek: Onderzoek en behandeling deel IIA 2017.
- ↑ Culvenor AG, Collins NJ, Vicenzino B, Cook JL, Whitehead TS, Morris HG, et al. Predictors and effects of patellofemoral pain following hamstring-tendon ACL reconstruction. J Sci Med Sport. 2015.
- ↑ Hamstring strength loss after ACL Surgery. Available from: http://www.youtube.com/watch?v=EtO4TqQcORc&t=287s