Angina
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Kim Jackson, Temitope Olowoyeye and Aminat Abolade
Introduction[edit | edit source]
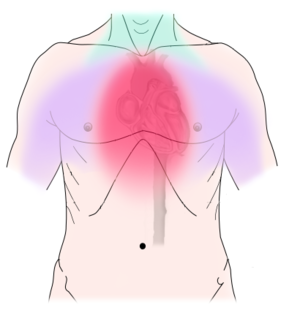
Angina pectoris (commonly known as Angina) is a disease marked by brief sudden attacks of chest pain or discomfort caused by deficient oxygenation of the heart muscles usually due to impaired blood flow to the heart Image on R: Diagram of discomfort caused by coronary artery disease. Pressure, fullness, squeezing or pain in the center of the chest. Can also feel discomfort in the neck, jaw, shoulder, back or arm
- Chest pain may be accompanied by other symptoms (such as nausea, shortness of breath, or pain in the neck, shoulder, jaw, arm, or back). Angina pectoris typically occurs concurrently with coronary heart disease and is often precipitated by physical exertion or emotional stress[1].
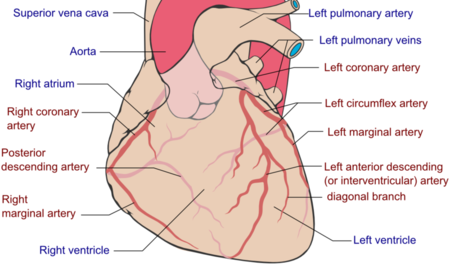
- The main cause of angina pectoris is CAD or coronary artery disease. But this condition can be derived from the heart failure, cardiac arrhythmias and Anaemia.
- Coronary artery disease is a leading cause of death worldwide. The World Health Organization (WHO) reported that CAD was responsible for approximately nine million deaths in 2016.[2]
Medical professionals now differentiate Angina into three types:
- Stable angina (most common)
- Unstable angina
- Variant (Prinzmetal’s) angina.
Because angina is so closely related to other cardiovascular conditions, correctly diagnosing the disease requires precision.[3]
Stable Angina[edit | edit source]
Stable angina occurs:
- When the heart is working harder than usual - eg while exercising, doing yard work, eating a large meal, going out in cold weather[4] or experiencing emotional stress. These situations are considered to be triggers for stable angina.
- In a pattern - the pattern includes how often the angina attacks occur, what triggers it and how severe the attack is. There isn’t a set pattern that applies to every person with angina – each person’s pattern may be a little different, but the fact that there is a pattern is what makes it stable rather than unstable.
- For short periods of time - the pain associated with a stable angina attack usually goes away after a few minutes of rest or after taking a medication for angina. Most stable angina attacks last for between 1 and 15 minutes[5].
Unstable Angina[edit | edit source]
Unstable angina occurs:
- At random - an unstable angina attack can happen at any time, even when a person is at rest. It can occur with or without physical exertion.
- In no particular pattern - unstable angina is unpredictable, and the attacks may vary widely in how often they occur, what triggers them and how severe the pain is. In general, however, unstable angina attacks tend to be more severe and occur more often than those of stable angina.
- For longer periods of time - resting or taking angina medicine does not always relieve the pain associated with an unstable angina attack, which usually lasts more than 15-20 minutes. Emergency treatment should be sought immediately since unstable angina may indicate that a heart attack may happen soon.[5]
Prinzmetal’s Angina[edit | edit source]
Unlike typical angina – which is often triggered by exertion or emotional stress – Prinzmetal’s angina almost always occurs when a person is at rest, usually between midnight and early morning.[6] These attacks can be very painful.
- Prinzmetal angina may also be referred to as: Variant angina
- Prinzmetal’s angina is rare, representing about two out of 100 cases of angina, and usually occurs in younger patients than those who have other kinds of angina.
- Causes of Variant (Prinzmetal) Angina - the pain from variant angina is caused by a spasm in the coronary arteries.
The coronary arteries can spasm as a result of:
- Exposure to cold weather[4]
- Stress
- Medicines that tighten or narrow blood vessels
- Smoking
- Cocaine use[7]
Complications[edit | edit source]
The complications angina include:
Medical Management[edit | edit source]
In spite of enormous improvements in technology and skills in percutaneous revascularization over the last two decades, medical treatment remains a very important modality of management for angina.
The goals of medical treatment are relief of symptoms, prevention of further progression of atherosclerotic heart disease and reduction in the incidence of acute coronary syndrome and mortality.[11]
Treatment includes
- Lifestyle changes — Changes include weight loss for obese patients, therapy to quit smoking, medications to lower high cholesterol, a program of regular exercise to lower high blood pressure, and stress reduction techniques.
- Nitrates, including nitroglycerin — Nitrates are medications that widen blood vessels (vasodilators).
- Statins, such as atorvastatin (Lipitor), rosuvastatin (Crestor) and simvastatin (Zocor, generic versions)
- Beta-blockers, such as atenolol (Tenormin) and metoprolol (Lopressor, Toprol-XL)
- Aspirin — helps to prevent blood clots from forming inside narrowed coronary arteries.
- If lifestyle changes and drugs fail to ease angina or when the risk of heart attack is great, your doctor may recommend balloon angioplasty or coronary artery bypass surgery.[12]
Physiotherapy Management[edit | edit source]
Angina can inhibit individual’s ability to carry out normal activities of daily living such as walking around, shopping or climbing stairs. Physiotherapy can help to minimise angina, improve cardiovascular fitness and reduce the risk of further cardiac complications.
Treatment for an individual with angina may include:
- Cardiovascular exercise
- Fitness and stamina
- Flexibility and range of movement
- Core Stability and dynamic balance work
- Weight management
- Lifestyle changes[13]
See also Cardiac Rehabilitation
References[edit | edit source]
- ↑ Merriam webster angina pectoris Available from:https://www.merriam-webster.com/dictionary/angina%20pectoris (last accessed 10.8.2020)
- ↑ Regmi M, Siccardi MA. Coronary Artery Disease Prevention. InStatPearls [Internet] 2019 Sep 24. StatPearls Publishing. Available from:https://www.ncbi.nlm.nih.gov/books/NBK547760/ (last accessed 6.8.2020)
- ↑ Worldwide clinical trial Angina Available from:https://www.worldwide.com/therapeutic-areas/cardiovascular-disease/angina/ (last accessed 10.8.2020)
- ↑ 4.0 4.1 Marchant B, Donaldson G, Mridha K, Scarborough M, Timmis AD. Mechanisms of cold intolerances in patients with angina. Journal of the American College of Cardiology. 1994 Mar 1;23(3):630-6.
- ↑ 5.0 5.1 Symptomfind Angina Available from:https://www.symptomfind.com/health/stable-and-unstable-angina/ (last accessed 10.8.2020)
- ↑ Ghadri JR, Ruschitzka F, Lüscher TF, Templin C. Prinzmetal angina. QJM: An International Journal of Medicine. 2014 May 1;107(5):375-7.
- ↑ Heart Organisation Angina Available from:https://www.heart.org/en/health-topics/heart-attack/angina-chest-pain/prinzmetals-or-prinzmetal-angina-variant-angina-and-angina-inversa (last accessed 10.8.2020)
- ↑ 8.0 8.1 8.2 Ziccardi MR, Hatcher JD. Prinzmetal Angina. InStatPearls [Internet] 2022 Jul 18. StatPearls Publishing.
- ↑ 9.0 9.1 9.2 Goyal A, Zeltser R. Unstable angina. InStatPearls [Internet] 2022 May 2. StatPearls Publishing.
- ↑ Gillen C, Goyal A. Stable Angina. InStatPearls [Internet] 2021 Dec 21. StatPearls Publishing.
- ↑ Chatterjee D. Medical management of angina: treatment of associated conditions and the role of antiplatelet drugs. Available from:https://www.escardio.org/Journals/E-Journal-of-Cardiology-Practice/Volume-15/Medical-management-of-angina-treatment-of-associated-conditions-and-the-role-of-antiplatelet-drugs (last accessed 10.8.2020)
- ↑ Drugs.com Angina Available from:https://www.drugs.com/health-guide/angina.html (last accessed 10.8.2020)
- ↑ physiouk Angina Available from:https://www.physio.co.uk/what-we-treat/cardiovascular/angina.php (last accessed 10.8.2020)