Neuropathies: Difference between revisions
Kim Jackson (talk | contribs) m (Added Charcot Marie Tooth Disease to Neuropathies) |
No edit summary |
||
| Line 4: | Line 4: | ||
== Clinically Relevant Anatomy == | == Clinically Relevant Anatomy == | ||
[[File:Neuron Part 1.png|right|frameless|500x500px]] | |||
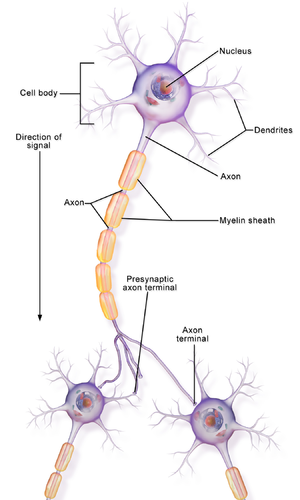
Peripheral neuropathies encompass disorders of peripheral nerve cells and fibers which occur secondary to a wide range of pathologies. These nerves include: cranial nerves; spinal nerve roots & ganglia; nerve trunks & division; nerves of the autonomic nervous system. | |||
Several methods are used to classify peripheral neuropathies including | |||
# Categorizing them as mono-neuropathies, multifocal neuropathies, and poly-neuropathies. | |||
# Further subclassifications can be made separating peripheral neuropathies as axonal, demyelinating, or mixed, which is essential for treatment and management purposes. | |||
The most frequently encountered symptoms of peripheral neuropathy include numbness and paresthesias; pain, weakness, and loss of deep tendon reflexes may accompany these symptoms. | |||
The | Peripheral neuropathies | ||
* Usually develop over months to years, while some may develop more rapidly and be progressive in nature. | |||
* Have a broad range of severity and clinical manifestations as they can affect motor, sensory, and autonomic fibers.<ref name=":2">Hammi C, Yeung B. [https://www.ncbi.nlm.nih.gov/books/NBK542220/ Neuropathy.2019] Available from;https://www.ncbi.nlm.nih.gov/books/NBK542220/ (last accessed 5.9.2020)</ref> | |||
. | |||
== Pathological Process == | |||
The exact pathophysiology of peripheral neuropathy is contingent on the underlying disease. | |||
* Although a wide assortment of distinct diseases can ultimately lead to peripheral neuropathies, the mechanisms in which peripheral nerves suffer injury exhibit similar patterns. | |||
* These reactions include segmental demyelination, along with Wallerian and axonal degeneration<ref name=":2" />. | |||
== Etiology == | |||
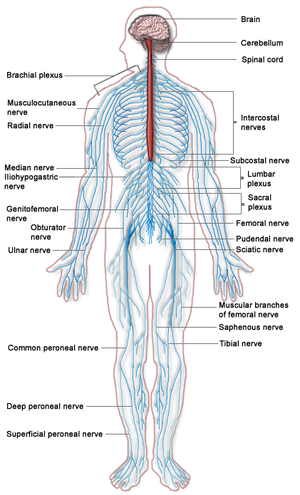
[[File:Nervous system diagram.png|495x495px|right|frameless]]Peripheral neuropathies stem from a variety of origins including metabolic, systemic, and toxic causes. Underlying etiologies to consider include: | |||
* Physical injury e.g. pressure from disc herniation, pressure from a cast, trauma, arthritis. | * Physical injury e.g. pressure from disc herniation, pressure from a cast, trauma, arthritis. | ||
* [[Diabetes]] | * [[Diabetes]] | ||
* Autoimmune diseases e.g. [[Guillain-Barre Syndrome|Guillain-Barre Syndrome]], [https://medlineplus.gov/sjogrenssyndrome.html Sjogren's Syndrome], [[Systemic Lupus Erythematosus|Lupus]], [[Rheumatoid Arthritis|Rheumatoid Arthritis (RA)]] | * Autoimmune diseases e.g. [[Guillain-Barre Syndrome|Guillain-Barre Syndrome]], [https://medlineplus.gov/sjogrenssyndrome.html Sjogren's Syndrome], [[Systemic Lupus Erythematosus|Lupus]], [[Rheumatoid Arthritis|Rheumatoid Arthritis (RA)]] | ||
* | * Nutritional deficiencies (e.g., B1,B6, [[Vitamin B12 Deficiency|B12,]] vitamin E) | ||
* Infections e.g. chicken pox, Varicella zoster virus (shingles), White Nile virus, AIDS, Lyme disease (carried by ticks), Epstein-Barr virus, hepatitis C<ref name=":0">NIH [https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Peripheral-Neuropathy-Fact-Sheet Peripheral neuropathy fact sheet.] Available from: https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Peripheral-Neuropathy-Fact-Sheet (last accessed 18 April 2019)</ref> | * inflammatory conditions (e.g., vasculitis) | ||
[[File: | * Infections e.g. chicken pox, Varicella zoster virus (shingles), White Nile virus, [[HIV/AIDS|AIDS]], [[Lyme Disease|Lyme]] disease (carried by ticks), Epstein-Barr virus, [[Hepatitis A, B, C|hepatitis]] C<ref name=":0">NIH [https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Peripheral-Neuropathy-Fact-Sheet Peripheral neuropathy fact sheet.] Available from: https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Peripheral-Neuropathy-Fact-Sheet (last accessed 18 April 2019)</ref> | ||
* [[Chemotherapy Side Effects and Syndromes|Chemotherapy]] agents | |||
* Medications (antibiotics, cardiovascular medications) | |||
* Tumors (secondary to compression or associated [[Paraneoplastic Syndrome|paraneoplastic]] syndromes) | |||
* Inherited conditions (e.g., [[Charcot-Marie-Tooth Disease: A Case Study|Charcot-Marie-Tooth]] disease, familial amyloidosis) | |||
* Trauma/injury | |||
* [[Multiple Myeloma|Multiple myeloma]] and its treatments | |||
* Monoclonal gammopathy of undetermined significance (MGUS) | |||
In some cases, a direct cause may not be apparent<ref name=":2" /> | |||
== Epidemiology == | |||
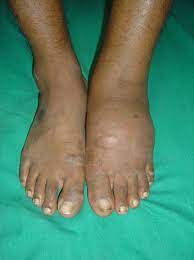
* [[File:Diabetic foot.jpg|right|frameless]]Approx. 2.4% of the population is affected by peripheral nerve disorders | |||
* Prevalence increases to 8.0% in older populations. | |||
* Diabetic neuropathy occurs in approximately 50% of individuals with chronic type 1 and type 2 diabetes. | |||
* Globally, [[Body Pain|leprosy]] remains a common cause of peripheral neuropathy, with the highest prevalence in South East Asia. | |||
* The most common genetic sensorimotor polyneuropathy is Charcot-Marie-Tooth disease, specifically, type 1a. | |||
* The most common mononeuropathy is [[Carpal Tunnel Syndrome|carpal tunnel syndrome]].<ref name=":2" /> | |||
== Clinical Presentation == | == Clinical Presentation == | ||
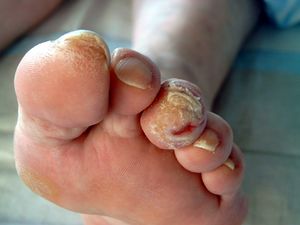
* [[File:Offene_Wunde_bei_einem_diabetischen_Fußsyndrom.jpg|thumb|An example of foot damage due to sensory loss]] The clinical presentation of peripheral neuropathy widely varies depending on the underlying disease process. | |||
* Patients may complain of symptoms initially starting in their digits, progressing to their proximal limbs. | |||
* Symptoms range and include changes in sensation, weakness, atrophy, pain, numbness, and even autonomic disturbances. | |||
<br> | * Clinically, these symptoms may resemble that of myelopathies, radiculopathies, autoimmune disease, and diseases of muscles. | ||
* Motor nerve damage will cause muscle weakness, painful cramps, fasciculations (uncontrolled muscle twitching visible under the skin) and muscle atrophy | * Advanced disease may progress to reduced or absent deep tendon reflexes, stocking-glove pattern sensory loss, muscle wasting, and weakness<br> | ||
** Motor nerve damage will cause muscle weakness, painful cramps, fasciculations (uncontrolled muscle twitching visible under the skin) and muscle atrophy | |||
* Sensory nerve damage causes various symptoms because sensory nerves have a broad range of functions. Damage to large sensory fibers affects the ability to feel vibrations and touch. The client may feel as if she/he is wearing gloves and stockings. This damage may contribute to the loss of reflexes (along with motor nerve damage). Loss of position sense presenting with e.g. balance problems. The damage of “small fibers” (without myelin sheaths) affects the transmission of pain and temperature sensations which interferes with the ability to feel pain or changes in temperature. This causes [[Neuropathic pain|neuropathic pain,]] which can erode a person's [[Quality-Adjusted Life Year|quality of life.]] | ** Sensory nerve damage causes various symptoms because sensory nerves have a broad range of functions. Damage to large sensory fibers affects the ability to feel vibrations and touch. The client may feel as if she/he is wearing gloves and stockings. This damage may contribute to the loss of reflexes (along with motor nerve damage). Loss of position sense presenting with e.g. balance problems. The damage of “small fibers” (without myelin sheaths) affects the transmission of pain and temperature sensations which interferes with the ability to feel pain or changes in temperature. This causes [[Neuropathic pain|neuropathic pain,]] which can erode a person's [[Quality-Adjusted Life Year|quality of life.]] | ||
** Autonomic nerve damage affects the axons in small-fiber neuropathies. Common symptoms include, excess sweating, heat intolerance, inability to expand and contract the small blood vessels that regulate blood pressure, and gastrointestinal symptoms.<ref name=":0" /> | |||
* Autonomic nerve damage affects the axons in small-fiber neuropathies. Common symptoms include, excess sweating, heat intolerance, inability to expand and contract the small blood vessels that regulate blood pressure, and gastrointestinal symptoms.<ref name=":0" /> | |||
== Diagnostic Procedures == | == Diagnostic Procedures == | ||
[[File:Blood testing.jpg|right|frameless]] | |||
Evaluating patients with neuropathy involves a detailed history and physical including a review of current and past medications. Although there are no standard laboratory or imaging studies to test for peripheral neuropathies, the following studies may aid in the diagnosis and help narrow down the underlying cause of the neuropathy (e.g., inflammatory, infectious, metabolic) | |||
* [[Blood Tests|Blood tests]], checking for e.g. toxins, vitamin deficiencies, [[diabetes]] | * [[Blood Tests|Blood tests]], checking for e.g. toxins, vitamin deficiencies, [[diabetes]] | ||
* Imaging test e.g. [[CT Scans|CT scans]], [[MRI Scans|MRI scans]] | * Imaging test e.g. [[CT Scans|CT scans]], [[MRI Scans|MRI scans]] | ||
* Nerve function tests, checking nerve conduction. | * Nerve function tests, checking nerve conduction. | ||
* Nerve biopsy, looking for abnormalities | * Nerve biopsy, looking for abnormalities | ||
* Skin biopsy, looking for reduction in nerve endings<ref name=":1">Mayo clinic. [https://www.mayoclinic.org/diseases-conditions/peripheral-neuropathy/diagnosis-treatment/drc-20352067 Peripheral neuropathy.] Available from: https://www.mayoclinic.org/diseases-conditions/peripheral-neuropathy/diagnosis-treatment/drc-20352067 (last accessed 18 April 2019)</ref | * Skin biopsy, looking for reduction in nerve endings<ref name=":1">Mayo clinic. [https://www.mayoclinic.org/diseases-conditions/peripheral-neuropathy/diagnosis-treatment/drc-20352067 Peripheral neuropathy.] Available from: https://www.mayoclinic.org/diseases-conditions/peripheral-neuropathy/diagnosis-treatment/drc-20352067 (last accessed 18 April 2019)</ref> | ||
== Outcome Measures == | == Outcome Measures == | ||
| Line 50: | Line 72: | ||
* INCAT (inflammatory cause and treatment) score is a measure of activity limitation | * INCAT (inflammatory cause and treatment) score is a measure of activity limitation | ||
* [[Timed Up and Go Test (TUG)|TUG]]; [[10 Metre Walk Test|10 metre walk test]]; [[Grip Strength]]; [[Fatigue Severity Scale|Fatigue Severity Scale;]] [[Patient Specific Functional Scale]]; [[Muscle Strength|Oxford Muscle Strength Scale]]; [[Romberg Test|Romberg Test]]. | * [[Timed Up and Go Test (TUG)|TUG]]; [[10 Metre Walk Test|10 metre walk test]]; [[Grip Strength]]; [[Fatigue Severity Scale|Fatigue Severity Scale;]] [[Patient Specific Functional Scale]]; [[Muscle Strength|Oxford Muscle Strength Scale]]; [[Romberg Test|Romberg Test]]. | ||
== | == Treatment == | ||
Treatment of peripheral neuropathies should focus on the treatment of the underlying disease process. Eg | |||
* Glucose control in diabetic neuropathy, alcohol cessation in alcoholic neuropathy. | |||
* Nutritional deficiencies can have therapy with supplementation of the depleted vitamins or minerals. | |||
Not all peripheral neuropathies are reversible. | |||
* Physical therapy and occupational therapy can aid in the improvement of a patient's overall strength and function. | |||
* Chronic inflammatory demyelinating neuropathy is treated using corticosteroids initially, but can also be treated using intravenous immunoglobulin, plasma exchange, and some immunosuppressant drugs<ref name=":2" />. | |||
* A referral to a pain specialist can be beneficial for those patients who are suffering from neuropathic pain. | |||
* Neuropathic pain, particularly in those suffering from small-fiber neuropathies, do not typically respond to simple analgesics. Instead, effective treatment for pain associated with peripheral neuropathies can be with membrane stabilizers, certain anti-epileptics, and tricyclic antidepressants. | |||
* Transcutaneous electrical nerve stimulation (TENS) is also an option as a noninvasive intervention for pain relief<ref name=":2" />. | |||
Medications used to relieve peripheral neuropathy signs and symptoms include:<ref name=":1" /> | |||
'''Anticonvulsants:''' Gabapentin; Pregabalin; Valproate | '''Anticonvulsants:''' Gabapentin; Pregabalin; Valproate | ||
| Line 60: | Line 91: | ||
'''Others:''' Topical nitrate sprays; Capsaicin cream | '''Others:''' Topical nitrate sprays; Capsaicin cream | ||
== Physiotherapy == | == [[Nerve Injury Rehabilitation|Physiotherapy]] == | ||
[[File:Motionscykel Sjukgym.gif|right|frameless]]The main role of Physiotherapy is to | [[File:Motionscykel Sjukgym.gif|right|frameless]] | ||
[[File:Exercise group.jpg|right|frameless]] | |||
The main role of Physiotherapy is to | |||
* Restore, or maintain muscle strength, and prevent muscle shortening and deformity | * Restore, or maintain muscle strength, and prevent muscle shortening and deformity | ||
* [[Balance]], coordination and functional training. | * [[Balance]], coordination and functional training. | ||
| Line 87: | Line 120: | ||
* [[Thoracic Radiculopathy]] | * [[Thoracic Radiculopathy]] | ||
* [[Ulnar Nerve Entrapment]] | * [[Ulnar Nerve Entrapment]] | ||
== Prognosis == | |||
In those diseases where peripheral nerves suffer damage through Wallerian or axonal degeneration, the prognosis is poorer, as the recovery of the nerve is more challenging. | |||
* For clinical improvement to take place, the axon must regenerate itself, and reinnervate the affected muscle or organ. | |||
* The prognosis of diseases which occur secondary to segmental demyelination is more favorable because remyelination is achieved more quickly, allowing the return of function of the axon. | |||
* Complications of peripheral neuropathies include pain, altered sensation, muscle atrophy, and weakness. Diabetic peripheral neuropathy is infamous for complications including foot ulcers which can lead to gangrenous digits and limbs, sometimes progressing to amputation.<ref name=":2" /> | |||
== References == | == References == | ||
<references /> | <references /> | ||
Revision as of 07:29, 5 September 2020
Top Contributors - Lucinda hampton, Kim Jackson, Candace Goh, Melissa Coetsee, Uchechukwu Chukwuemeka, Manisha Shrestha, Merinda Rodseth, Ahmed M Diab and Sehriban Ozmen
Clinically Relevant Anatomy[edit | edit source]
Peripheral neuropathies encompass disorders of peripheral nerve cells and fibers which occur secondary to a wide range of pathologies. These nerves include: cranial nerves; spinal nerve roots & ganglia; nerve trunks & division; nerves of the autonomic nervous system.
Several methods are used to classify peripheral neuropathies including
- Categorizing them as mono-neuropathies, multifocal neuropathies, and poly-neuropathies.
- Further subclassifications can be made separating peripheral neuropathies as axonal, demyelinating, or mixed, which is essential for treatment and management purposes.
The most frequently encountered symptoms of peripheral neuropathy include numbness and paresthesias; pain, weakness, and loss of deep tendon reflexes may accompany these symptoms.
Peripheral neuropathies
- Usually develop over months to years, while some may develop more rapidly and be progressive in nature.
- Have a broad range of severity and clinical manifestations as they can affect motor, sensory, and autonomic fibers.[1]
.
Pathological Process[edit | edit source]
The exact pathophysiology of peripheral neuropathy is contingent on the underlying disease.
- Although a wide assortment of distinct diseases can ultimately lead to peripheral neuropathies, the mechanisms in which peripheral nerves suffer injury exhibit similar patterns.
- These reactions include segmental demyelination, along with Wallerian and axonal degeneration[1].
Etiology[edit | edit source]
Peripheral neuropathies stem from a variety of origins including metabolic, systemic, and toxic causes. Underlying etiologies to consider include:
- Physical injury e.g. pressure from disc herniation, pressure from a cast, trauma, arthritis.
- Diabetes
- Autoimmune diseases e.g. Guillain-Barre Syndrome, Sjogren's Syndrome, Lupus, Rheumatoid Arthritis (RA)
- Nutritional deficiencies (e.g., B1,B6, B12, vitamin E)
- inflammatory conditions (e.g., vasculitis)
- Infections e.g. chicken pox, Varicella zoster virus (shingles), White Nile virus, AIDS, Lyme disease (carried by ticks), Epstein-Barr virus, hepatitis C[2]
- Chemotherapy agents
- Medications (antibiotics, cardiovascular medications)
- Tumors (secondary to compression or associated paraneoplastic syndromes)
- Inherited conditions (e.g., Charcot-Marie-Tooth disease, familial amyloidosis)
- Trauma/injury
- Multiple myeloma and its treatments
- Monoclonal gammopathy of undetermined significance (MGUS)
In some cases, a direct cause may not be apparent[1]
Epidemiology[edit | edit source]
- Approx. 2.4% of the population is affected by peripheral nerve disorders
- Prevalence increases to 8.0% in older populations.
- Diabetic neuropathy occurs in approximately 50% of individuals with chronic type 1 and type 2 diabetes.
- Globally, leprosy remains a common cause of peripheral neuropathy, with the highest prevalence in South East Asia.
- The most common genetic sensorimotor polyneuropathy is Charcot-Marie-Tooth disease, specifically, type 1a.
- The most common mononeuropathy is carpal tunnel syndrome.[1]
Clinical Presentation[edit | edit source]
- The clinical presentation of peripheral neuropathy widely varies depending on the underlying disease process.
- Patients may complain of symptoms initially starting in their digits, progressing to their proximal limbs.
- Symptoms range and include changes in sensation, weakness, atrophy, pain, numbness, and even autonomic disturbances.
- Clinically, these symptoms may resemble that of myelopathies, radiculopathies, autoimmune disease, and diseases of muscles.
- Advanced disease may progress to reduced or absent deep tendon reflexes, stocking-glove pattern sensory loss, muscle wasting, and weakness
- Motor nerve damage will cause muscle weakness, painful cramps, fasciculations (uncontrolled muscle twitching visible under the skin) and muscle atrophy
- Sensory nerve damage causes various symptoms because sensory nerves have a broad range of functions. Damage to large sensory fibers affects the ability to feel vibrations and touch. The client may feel as if she/he is wearing gloves and stockings. This damage may contribute to the loss of reflexes (along with motor nerve damage). Loss of position sense presenting with e.g. balance problems. The damage of “small fibers” (without myelin sheaths) affects the transmission of pain and temperature sensations which interferes with the ability to feel pain or changes in temperature. This causes neuropathic pain, which can erode a person's quality of life.
- Autonomic nerve damage affects the axons in small-fiber neuropathies. Common symptoms include, excess sweating, heat intolerance, inability to expand and contract the small blood vessels that regulate blood pressure, and gastrointestinal symptoms.[2]
Diagnostic Procedures[edit | edit source]
Evaluating patients with neuropathy involves a detailed history and physical including a review of current and past medications. Although there are no standard laboratory or imaging studies to test for peripheral neuropathies, the following studies may aid in the diagnosis and help narrow down the underlying cause of the neuropathy (e.g., inflammatory, infectious, metabolic)
- Blood tests, checking for e.g. toxins, vitamin deficiencies, diabetes
- Imaging test e.g. CT scans, MRI scans
- Nerve function tests, checking nerve conduction.
- Nerve biopsy, looking for abnormalities
- Skin biopsy, looking for reduction in nerve endings[3]
Outcome Measures[edit | edit source]
The many different presentations of neuropathies lead to a need to client specific outcome measures. Usually related to muscle strength, pain, QOL, and activity limitations. They include:
- The SF-36 is a measure of health status and an abbreviated variant of it, the SF-6D, is commonly used in health economics as a variable in the quality-adjusted life year calculation to determine the cost-effectiveness of a health treatment.[4]
- INCAT (inflammatory cause and treatment) score is a measure of activity limitation
- TUG; 10 metre walk test; Grip Strength; Fatigue Severity Scale; Patient Specific Functional Scale; Oxford Muscle Strength Scale; Romberg Test.
Treatment[edit | edit source]
Treatment of peripheral neuropathies should focus on the treatment of the underlying disease process. Eg
- Glucose control in diabetic neuropathy, alcohol cessation in alcoholic neuropathy.
- Nutritional deficiencies can have therapy with supplementation of the depleted vitamins or minerals.
Not all peripheral neuropathies are reversible.
- Physical therapy and occupational therapy can aid in the improvement of a patient's overall strength and function.
- Chronic inflammatory demyelinating neuropathy is treated using corticosteroids initially, but can also be treated using intravenous immunoglobulin, plasma exchange, and some immunosuppressant drugs[1].
- A referral to a pain specialist can be beneficial for those patients who are suffering from neuropathic pain.
- Neuropathic pain, particularly in those suffering from small-fiber neuropathies, do not typically respond to simple analgesics. Instead, effective treatment for pain associated with peripheral neuropathies can be with membrane stabilizers, certain anti-epileptics, and tricyclic antidepressants.
- Transcutaneous electrical nerve stimulation (TENS) is also an option as a noninvasive intervention for pain relief[1].
Medications used to relieve peripheral neuropathy signs and symptoms include:[3]
Anticonvulsants: Gabapentin; Pregabalin; Valproate
Antidepressants:Amitriptyline; Duloxetine; Venlafaxine
Opioids: Dextromethorphan; Morphine sustained release; Oxycodene; Tapentadol; Tramadol.
Others: Topical nitrate sprays; Capsaicin cream
Physiotherapy[edit | edit source]
The main role of Physiotherapy is to
- Restore, or maintain muscle strength, and prevent muscle shortening and deformity
- Balance, coordination and functional training.
- Pain relief e.g. provision of TENS, massage
- Splints as needed, prevent deformity and contractures
- Education, re-managing conditions, preventing damage and emotional support.
For a comprehensive guide see individual neuropathies below
- AIDS
- Anterior Interosseous Nerve Syndrome
- Axillary Nerve Injury
- Brachial Plexus Injury
- Benediction Hand
- Carpal Tunnel Syndrome
- Charcot Marie Tooth Disease
- Chronic Inflammatory Demyelinating Polyneuropathy (CIDP)
- Cubital Tunnel Syndrome
- Cyclist's Palsy
- Diabetic Neuropathy
- Double Crush Syndrome
- Lumbar Radioculopathy
- Multifocal Motor Neuropathy
- Nerve Entrapment
- Posterior Interosseous Nerve Syndrome
- Sciatic Nerve Injury
- Thoracic Radiculopathy
- Ulnar Nerve Entrapment
Prognosis[edit | edit source]
In those diseases where peripheral nerves suffer damage through Wallerian or axonal degeneration, the prognosis is poorer, as the recovery of the nerve is more challenging.
- For clinical improvement to take place, the axon must regenerate itself, and reinnervate the affected muscle or organ.
- The prognosis of diseases which occur secondary to segmental demyelination is more favorable because remyelination is achieved more quickly, allowing the return of function of the axon.
- Complications of peripheral neuropathies include pain, altered sensation, muscle atrophy, and weakness. Diabetic peripheral neuropathy is infamous for complications including foot ulcers which can lead to gangrenous digits and limbs, sometimes progressing to amputation.[1]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Hammi C, Yeung B. Neuropathy.2019 Available from;https://www.ncbi.nlm.nih.gov/books/NBK542220/ (last accessed 5.9.2020)
- ↑ 2.0 2.1 NIH Peripheral neuropathy fact sheet. Available from: https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Peripheral-Neuropathy-Fact-Sheet (last accessed 18 April 2019)
- ↑ 3.0 3.1 Mayo clinic. Peripheral neuropathy. Available from: https://www.mayoclinic.org/diseases-conditions/peripheral-neuropathy/diagnosis-treatment/drc-20352067 (last accessed 18 April 2019)
- ↑ Wikipedia. SF-36 Available from: https://en.wikipedia.org/wiki/SF-36 (last accessed 19 April 2019)