Baastrup Syndrome
Original Editors - Fien Selderslaghs, Mirabella Smolders, Matthias Steenwerckx, Wout Theys as part of the Vrije Universiteit Brussel Evidence-Based Practice Project
Top Contributors - Sofie Bourdinon, Scott Cornish, Nikki Rommers, Admin, Arno Vrambout, Kim Jackson, Lucinda hampton, Fien Selderslaghs, Uchechukwu Chukwuemeka, Vidya Acharya, Ceulemans Lisa, Aarti Sareen, 127.0.0.1 and WikiSysop
Introduction[edit | edit source]
Baastrup syndrome (also referred to as kissing spines) is a cause of low back pain characterized by interspinous bursitis and other degenerative changes of the bones and soft tissues where adjacent spinous processes in the lumbar spine rub against each other.[1] It was first described by Christian Baastrup, a Danish radiologist, in 1933[2].
Kissing Spine mainly affects the lumbar area of the spine, with L4-L5 being the most frequently affected level [3], but it has also been reported in the cervical spine.[4]
Epidemiology /Etiology[edit | edit source]
Baastrup Syndrome tends to be more common in the elderly. Literature suggests repetitive lumbar spinal movements in the sagittal plane predispose injury of the posterior elements of the spine. Chronic flexion and extension strain the interspinous ligament, affecting the neighbouring spinous processes. These shearing movements result in further architectural distortion, flattening, sclerosis, and cyst formation in the opposing surfaces resulting in pain. [2]
Other suggested risk factors are:[5] [3]
- Excessive lordosis which results in increased mechanical pressure
- Repetitive strains of the interspinous ligament with subsequent degeneration and collapse
- Traumatic injuries
- Tuberculous spondylitis
- Bilateral forms of congenital hip dislocation
- Obesity
- Pediatric patients[6]: It is a very rare finding in pediatric patients with pediatric athletes susceptible due to physical and repetitive motions that contort the spinal column where adjacent vertebrae touch. Also, gymnasts are at an increased risk of developing “kissing spine disease” due to repeated spinal extension and flexion movement.[2]
Characteristics/Clinical Presentation[edit | edit source]
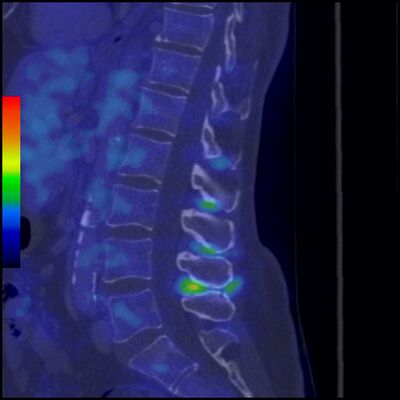
Patients with Baastrup syndrome typically show an excessive lordosis.[3] [7] Patients with Kissing Spine often complain about back pain, more specifically, midline pain that radiates distally and proximally, increasing on extension and reducing on flexion.[8] [3] This abnormal contact between adjacent spinous processes can lead to neoarthrosis and the formation of an adventitious bursa. This can be seen pathologically on MRI. [9] [10] [11]
Baastrup’s disease can result in intraspinal cysts secondary to an interspinous bursitis which may, in rare cases, cause symptomatic spinal stenosis and neurogenic claudication [9]
Diagnostic Procedures[edit | edit source]
Baastrup Syndrome cannot be diagnosed by simply assessing the lumbar spine, imaging modalities are required to prevent misdiagnosis. [3]
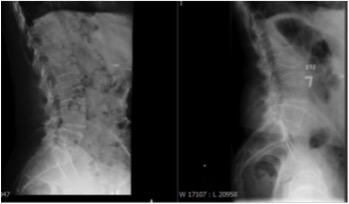
- CT and Xrays: Often shows close approximation and contact of adjacent spinous processes (kissing spines). Resultant enlargement, flattening, and reactive sclerosis of opposing interspinous surfaces
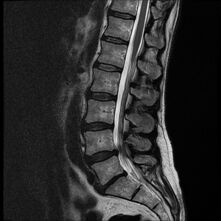
- Magnetic Resonance Imaging MRI: May demonstrate interspinous bursal fluid and posterocentral epidural cyst(s). MRI can be very helpful in determining whether there is resulting posterior compression of the thecal sac.
Outcome Measures[edit | edit source]
The following tests can be used to objectively determine the progress and efficacy of treatment:
Medical Management[edit | edit source]
The main goal of any therapy is to reduce lower back pain as well as return to normal ADLs. The treatment of Baastrup’s syndrome is an ongoing topic of debate. Both conservative and surgical treatment can be utilized, but an accurate diagnosis of the disease is necessary for determining the appropriate treatment.[12]
Local steroid injection into the interspinous processes/ligament region may often ease the back pain 8. Surgical options include interspinous process decompression devices.[1][13]
An interspinous processes spacer (also known as a decompression spacer or interspinous posterior device) is a device implanted between spinous processes to open narrowed exiting foraminal nerve channels to treat lumbar radiculopathy caused by spinal stenosis. The process of implantation is usually minimally invasive and performed under local anaesthesia. [14]
Physical Therapy Management[edit | edit source]
Examination[edit | edit source]
Diagnosis of Baastrup’s disease is verified with clinical examination and imaging studies.[3]
Symptoms include:
- Low back pain with midline distribution that exacerbates when performing extension relieved during flexion and is exaggerated upon finger pressure at the level of the pathologic interspinous ligament.
- Rotation and lateral flexion are very painful. [3]
- The pain can be described as a sharp or deep ache, often worse during physical activities that increase lumbar lordosis or compression of these structures.[15]
Throughout the physical examination, the physiotherapist uses active and passive techniques to evoke complaints.
- Active spinal extension can reproduce the symptoms.
- The stork test is very beneficial in the examination of this disease.[15]
- When the patient bends forward, relief is also gained.[16]
Treatment[edit | edit source]
The main goal is the reduction of pain as well as hyperlordosis and to improve spinal function. Once the pain is managed, physical therapy management can begin, involving education, strengthening and stretching of the abdominal and spinal muscles.[9] [19]
- Treating hyperlordosis is a key aspect, hence strengthening of the core muscles is recommended, along with postural education and hip flexor stretches. [20]
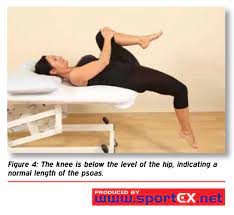
- When the abdominal muscles are weak, the hip flexors are mainly responsible for shaping the lumbar spine.[21] Furthermore the rectus femoris muscle is a continuation of the hip flexor complex so it is important to stretch rectus femoris muscle muscles. The hip flexors can become shorter through long-term sitting or resting. When these muscles shorten, it can affect the function of the gluteal and the spinal muscles.[22] The stretch below is one example of how to lengthen these muscles. Resting the weight on the knee and the front foot, push the hips forward until a stretch is felt, keeping the trunk upright. Maintain this position for at least 20 seconds, and repeat this 3-5 times on each side.[21]
Figure 6: Stretching the hip flexors [21]
- Motion of the gluteus maximus muscle during the flexion-extension cycle is decreased in patients with chronic low back pain, which is why strengthening of gluteus maximus muscle should be part of the physical management program [23]
- Physical therapy is also suggested to help reduce the neuromuscular damage that is provoked by the disease and other treatments such as heat therapy, ergotherapy and muscle relaxation techniques can be helpful [9]
Clinical Bottom Line[edit | edit source]
Kissing spines is characterised by the close approximation and contact of adjoining spinous processes. It is often treated with injections as pain relief in the first instance. Physical therapy should include stretching and strengthening exercises to reduce the mechanical pressure on the spine and any hyperlordosis. Baastrup’s syndrome is still relatively unknown and is often misdiagnosed and consequently treated incorrectly. [24]
Baastrup syndrome is more common in the lumbar spine with L4-L5 being the most affected region.[3] People who are most likely to suffer from Kissing Spine are particularly elderly patients with degenerative disc disease or hyperlordosis. Both of these conditions may lead to chronic contact between adjacent spinous processes. [25]
References[edit | edit source]
- ↑ 1.0 1.1 Radiopedia. Basstrup Syndrome. Available from:https://radiopaedia.org/articles/baastrup-disease-1?lang=us (accessed 29 August 2022)
- ↑ 2.0 2.1 2.2 Ali AA, Jacobs BM, Gandhi A, Brooks M. Baastrup’s Disease in Pediatric Gymnasts. Children. 2022 Jul 8;9(7):1018.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 Filippiadis DK, Mazioti A, Argentos S, Anselmetti G, Papakonstantinou O, Kelekis N, et al. Baastrup's disease (kissing spines syndrome): a pictorial review. Insights Imaging. 2015 Feb;6(1):123-8. doi: 10.1007/s13244-014-0376-7.
- ↑ Rajasekaran S, Pithwa YK. Baastrup's disease as a cause of neurogenic claudication: a case report. Spine (Phila Pa 1976). 2003 Jul 15;28(14):E273-5.
- ↑ Kacki S, Villotte S, Knüsel CJ. Baastrup's sign (kissing spines): A neglected condition in paleopathology. Int J Paleopathol. 2011 Oct;1(2):104-110. doi: 10.1016/j.ijpp.2011.09.001.
- ↑ Singh S. Baastrup's disease in the pediatric spine. Asian J Neurosurg. 2016 Oct-Dec;11(4):446. doi: 10.4103/1793-5482.145153.
- ↑ Jang EC, Song KS, Lee HJ, Kim JY, Yang JJ. Posterior epidural fibrotic mass associated with Baastrup's disease. Eur Spine J. 2010 Jul;19 Suppl 2(Suppl 2):S165-8. doi: 10.1007/s00586-009-1262-8.
- ↑ Singla A, Shankar V, Mittal S, Agarwal A, Garg B. Baastrup's disease: The kissing spine. World J Clin Cases. 2014 Feb 16;2(2):45-7. doi: 10.12998/wjcc.v2.i2.45.
- ↑ 9.0 9.1 9.2 9.3 Kwong Y, Rao N, Latief K. MDCT findings in Baastrup disease: disease or normal feature of the aging spine? AJR Am J Roentgenol. 2011 May;196(5):1156-9. doi: 10.2214/AJR.10.5719.
- ↑ Maes R, Morrison WB, Parker L, Schweitzer ME, Carrino JA. Lumbar interspinous bursitis (Baastrup disease) in a symptomatic population: prevalence on magnetic resonance imaging. Spine (Phila Pa 1976). 2008 Apr 1;33(7):E211-5. doi: 10.1097/BRS.0b013e318169614a.
- ↑ Farinha F, Raínho C, Cunha I, Barcelos A. Baastrup's Disease: a poorly recognised cause of back pain. Acta Reumatol Port. 2015 Jul-Sep;40(3):302-3. \
- ↑ Kerroum A, Laudato PA, Suter MR. The steps until surgery in the management of Baastrup's Disease (kissing spine syndrome). J Surg Case Rep. 2019 Jun 28;2019(6):rjz194. doi: 10.1093/jscr/rjz194.
- ↑ Lamer TJ, Tiede JM, Fenton DS. Fluoroscopically-guided injections to treat “kissing spine” disease. Pain Physician. 2008;11:549–54.
- ↑ Radiopedia. Interspinous processes spacer. Available from:https://radiopaedia.org/articles/interspinous-processes-spacer?lang=us (accessed 29 August 2022)
- ↑ 15.0 15.1 DePalma MJ. iSPINE Evidence Based Interventional Spine Care. New York:Demos Medical; 2011, 4-8
- ↑ Hertling D. et al. Management of common musculoskeletal disorders: Physical Therapy Principles and Methods. Lippincott Williams & Wilkins; 2006, 4th edition
- ↑ ladyspinedoc. Available from: http://www.youtube.com/watch?v=ja4omWV9QPM[last accessed 26/2/2024]
- ↑ Iragi board of diagnostic radiology . Baastrup's disease. Available from: http://www.youtube.com/watch?v=wy5mZEPbWT0[last accessed 26/2/2024]
- ↑ Cohen SP, Argoff CE, Carragee EJ. Management of low back pain. BMJ. 2008 Dec 22;337:a2718. doi: 10.1136/bmj.a2718.
- ↑ Scannell JP, McGill SM. Lumbar posture--should it, and can it, be modified? A study of passive tissue stiffness and lumbar position during activities of daily living. Phys Ther. 2003 Oct;83(10):907-17. PMID: 14519062.
- ↑ 21.0 21.1 21.2 Laughlin K. Overcome Neck and Back Pain. Simon & Schuster; 1998, 58-61
- ↑ Konrad A, Močnik R, Titze S, Nakamura M, Tilp M. The Influence of Stretching the Hip Flexor Muscles on Performance Parameters. A Systematic Review with Meta-Analysis. Int J Environ Res Public Health. 2021 Feb 17;18(4):1936. doi: 10.3390/ijerph18041936.
- ↑ Leinonen V, Kankaanpää M, Airaksinen O, Hänninen O. Back and hip extensor activities during trunk flexion/extension: effects of low back pain and rehabilitation. Arch Phys Med Rehabil. 2000 Jan;81(1):32-7. doi: 10.1016/s0003-9993(00)90218-1.
- ↑ Chen CK, Yeh L, Resnick D, Lai PH, Liang HL, Pan HB, et al. Intraspinal posterior epidural cysts associated with Baastrup's disease: report of 10 patients. AJR Am J Roentgenol. 2004 Jan;182(1):191-4. doi: 10.2214/ajr.182.1.1820191.
- ↑ Pinto PS, Boutin RD, Resnick D. Spinous process fractures associated with Baastrup disease. Clin Imaging. 2004 May-Jun;28(3):219-22. doi: 10.1016/S0899-7071(03)00156-6.