Principles of Amputation
Original Editor - Lucy Coughlan as part of the World Physiotherapy Network for Amputee Rehabilitation Project
Top Contributors - Admin, Aicha Benyaich, Tarina van der Stockt, Rachael Lowe, Kim Jackson, Shaimaa Eldib, Tony Lowe, Rucha Gadgil, Lauren Lopez, Sheik Abdul Khadir, Simisola Ajeyalemi, Amrita Patro, Wanda van Niekerk and Jess Bell
Introduction[edit | edit source]
Amputation is the cutting off or the removal of limb/extremity or part thereof,[1] by trauma, prolonged constriction or surgery (see Pathology leading to amputation). As a surgical measure, it is used to control pain or a disease process in the affected limb such as malignancy, infection or gangrene. In some cases, an amputation is carried out on individuals as a preventative surgery for such problems and other people are born with amputations due to congenital disorders (see Paediatric limb deficiency)
Every care should be taken to assure that the amputation is done only when clinically indicated. Amputation should only be considered if the limb is non-viable (gangrenous or grossly ischemic, dangerous, malignancy or infection), or non-functional[2].
A well-planned and executed amputation can remove a painful, dysfunctional limb and allow rehabilitation with a prosthetic limb to a functional, painless state. In this regard, amputation surgery may be considered a reconstructive surgery, with results similar to amputation of an arthritic femoral head and prosthetic replacement (total-hip replacement)[3].
Assessment for Amputation[edit | edit source]
A decision to amputate a limb should be made through discussion with the interdisciplinary team - including the patient - wherever possible; in an emergency situation, the decision should be made based on medical need. There are a number of different investigations that can be carried out to assess the need for amputation; these examinations assess the bones and soft tissues to establish limb viability.
- X-ray – images of bones to view fractures or disease
- Computerised Tomography (CT) scan – detailed images of bone, tissue and blood vessels
- Angiogram – outlines blood vessels
- Doppler ultrasound – occlusion of blood vessels
- Venogram and arteriogram – detailed imaging of blood vessels
These investigations will help the surgeons to find out if the blood supply to the limb is intact. The lower limb is supplied by the popliteal artery which subdivides into the:
- Posterior tibial artery
- Anterior tibial artery
- Fibular artery
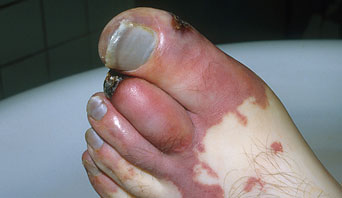
In vascular disease these arteries can become blocked or narrowed over time which reduces the circulation to the legs; this can cause pain, ulceration and blackened areas. If left untreated this can lead to gangrene or infection and amputation is needed to avoid this becoming life-threatening.
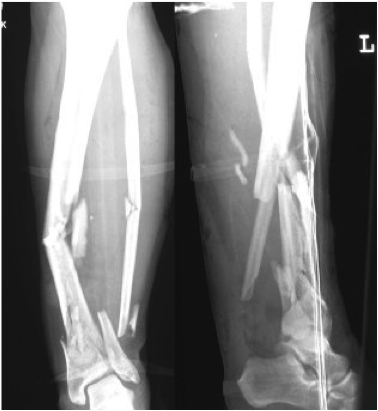
In trauma[4] one or more of these blood vessels may be ruptured beyond repair due to the nature of the injuries sustained – e.g. in a car accident, gunshot wound or blast. In this situation an amputation is performed as the limb does not have any blood supply beyond the level of injury and is therefore deemed non-viable.
There are a number of injury severity scores that may be used in conjunction with clinical investigations to establish the likelihood of limb salvage. Examples of this include:
- Nerve Injury, Ischemia, Soft-Tissue Injury, Skeletal Injury, Shock, and Age of Patient Score (NISSA)[5]
- Limb salvage index (LSI) [6]
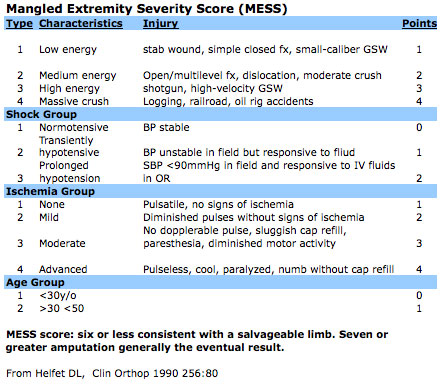
- Mangled Extremity Severity Score (MESS)[7]
Once a decision has been made to remove part of a limb the level of amputation needs to be decided; this can have significant consequences so there are a number of factors to take into account when planning the surgery:
- The boundary of dead or diseased tissue - if the infection or disease is not completely eradicated the patient may need to undergo further operations or treatment so it is important that the amputation is done at a level where this can be achieved.
- Suitability for a prosthesis - if the patient is likely to be a candidate for prosthetic rehab the level of amputation needs to be carefully considered.
- Mobility and function - it is useful to consider the patients’ pre-morbid level of mobility and function.
- Cosmesis - length and shape of stump affect the aesthetic appearance.
Amputation Surgery Terminology[edit | edit source]
Myodesis: The muscle is secured to the bone by suturing the distal tendon via pre-drilled holes to the bone.[8]
- Can be performed on below-knee or above-knee amputation.
- This method prevents deformity of the residual limb by preventing the excessive shift of the muscle during contraction (when this happens it interferes with the muscle control in the prosthesis).[8]
Myoplasty: Attaching sectioned muscles to opposing muscles [9]
Amputations classifications:
Levels of Lower Limb Amputations[edit | edit source]
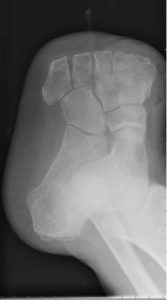
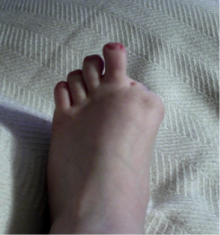
Amputations of the foot[edit | edit source]
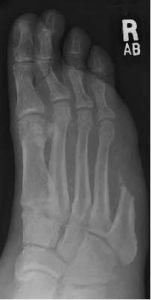
- Toe [8] - amputation through phalanges or disarticulation of metatarsal-phalangeal joint
- this is the most common lower limb amputation[10]
- usually due to ulcers
- great toe amputation affects balance, and ambulation because the late stance phase of gait and push off is disrupted without a first toe/ray to act as the final point of weight transfer
- the second toe acts as lateral support to the great toe and amputation of the second toe may lead to halux valgus
- the transverse arch of the foot get affected with the removal of any toe[8]
- usually amputated through the proximal phalanx [10]
- toe amputations should not be performed through the joint because it will expose the avascular cartilage[10]
- Ray [8]- amputation of the toe and the corresponding metatarsal
- The first ray along with great toe amputations affects balance and gait negatively
- amputation of the 2nd through 4th ray disrupts the transverse arch because the ligamentous structure is removed
- single ray amputations decrease the "structural integrity of the arch"
- when the fifth ray is resected it negatively impacts gait during midstance to terminal stance because it changes the rollover action of the foot[8]
- when there is infection surgeons can leave the wound open[10]
- Transmetatarsal[8] - partial foot amputation through metatarsals
- usually due to wounds in the forefoot due to gangrene or infection[10]
- a guillotine amputation is sometimes done in order to rid the foot of infection
- dorsal split-thickness grafts on the plantar aspect of the foot are used instead of skin grafts because it is more resilient
- the dorsal contact area of the foot is decreased and this leads to an increase of pressure and may result in calluses, ulcers, and wounds
- stance and gait (forward propulsion) is negatively influenced because the lever arm of the foot is shortened
- plantar flexion contracture should be avoided - this may occur because of the gastroc-soleus strength dominance over the dorsiflexors[8]
- if the wound is well healed, the patient can have excellent function[10]
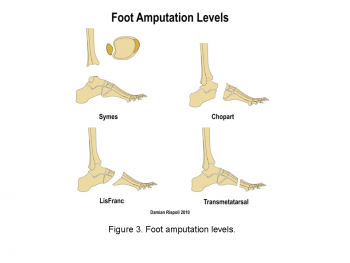
MIDFOOT AND HINDFOOT AMPUTATIONS[8]
- Tarsometatarsal (Lisfranc) - amputation of the forefoot at the tarsometatarsal line.
- Mid-tarsal (Chopart) - amputation between the talus and the calcaneus proximally and the cuboid and the navicular distally.
- Ankle disarticulation (Symes) – amputation through the ankle joint
- these 3-type of amputations are mainly performed in children to preserve the length of the residual limb and to keep the epiphyseal plate intact
- equinus varus foot deformity is possible due to the following: a gastrox-soleus and dorsiflexor imbalance, as well as a shortened lever arm
- surgical techniques to prevent this deformity include Achilles Tendon lengthening and the "reattachment of the peroneal and anterior tibial muscles to the more advantageous biomechanical position"
Advantages
- Range of prosthetic options such as insoles, toe fillers or ankle-foot orthosis (exception for ankle disarticulation)
Disadvantages
- May need further surgery in future
- Can lead to skin breakdown and joint pain
- Cosmesis might be not accepted by the patient
Read more:
Transtibial / Below Knee Amputation (BKA)[edit | edit source]
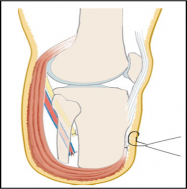
This amputation is done through the tibia and fibula, measurements are taken and flap lines marked out. The surgeon dissects through the skin to then isolate and ligate the nerves and blood vessels. In order to minimise the risk of neuropathic pain (see complications) the nerves are dissected on tension so the end will retract back into the tissues where they can heal away from the stump end. The tibia is dissected using an oscillating saw – optimum length of residual bone is approximately 12-17cm[11]; the tibia should be beveled at approximately 45° to remove the sharp anterior edge, the fibula should ideally be approx. 1-2 cm shorter than the tibia on a perpendicular axis. Preferred flap technique of surgeon is then used to close the wound and create functional stump - options include skew flap, long posterior flap, sagittal flap or medial flap.
Advantages[8]
- Preservation of the knee joint leads to less energy expenditure and better proprioception than an above knee amputee
- Candidates for patella tendon bearing prosthesis
- Near the normal level of function (more energy expenditure than a non-amputee)
- Decreased mortality rate and increases the likelihood for ambulation of the older person when compared to the above-knee amputation population
Disadvantages
- The risk of knee flexion contractures (see complications)
- May need ‘bone bridge’ surgery due to distal fibula pain (see complications)
This video shows one example of how a transtibial amputation can be performed.
Read more:
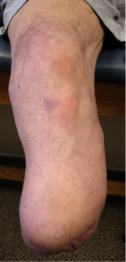
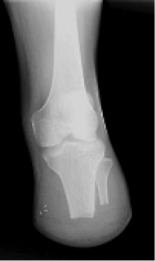
Knee Disarticulation Amputation (KDA) / Through Knee Amputation[edit | edit source]
Amputation done through the knee joint
Advantages
- Long lever prevents contractures and allows consequently the movement control[8]
- Maintains muscle length and strength
- Preserves growth plates in children
- Candidates for end bearing prosthesis
- Conserve condyles and the patella
- Proprioception and better distribution of pressure[8]
Disadvantages
- Bulky prosthesis (see complications)
- Poor cosmesis as knee mechanism is distal to the knee joint (see complications)
- More demanding surgical procedure with the risk of increased wound complications[8]
Read more:
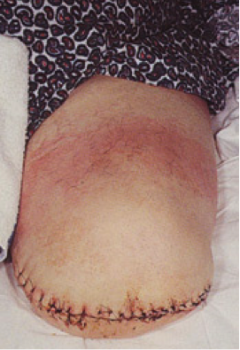
Transfemoral (TF)/ Above Knee Amputation (AKA)[edit | edit source]
This amputation is done through the femur, measurements are taken and flap lines marked out. The surgeon dissects through the skin to then isolate and ligate the nerves and blood vessels. In order to minimise the risk of neuropathic pain (see complications) the nerves are dissected on tension so the end will retract back into the tissues where they can heal away from the stump end. The femur is dissected on its perpendicular axis using an oscillating saw.
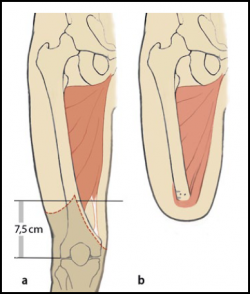
The optimum length of the residual bone is approximately 7.5-10cm proximal to the superior border of the patella. Very short trans-femoral stumps often end up in abduction because there is an imbalance between the adductor and abductor muscles. There is a significantly higher level of energy expenditure on the part of an amputee. It varies between 60% and 110% so lower levels of activity and mobility would be expected[4].
With a transfemoral amputation, the distal attachments of the thigh muscles are lost, in order to preserve their function and length, a myodesis may be performed to anchor the adductor (and sometimes hamstring) muscles to bone. The hamstrings and quadriceps may then be sutured together over the distal end of the femur – a technique called a myoplasty. It is a myoplasty of the antagonist muscles to help pad the end of the stump to perform Gottchaltk myodesis (adductor magnus trans-osseously fixed and covering the distal femoral end)
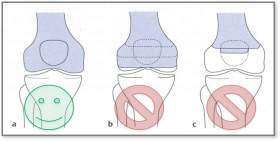
Advantages and Disadvantages
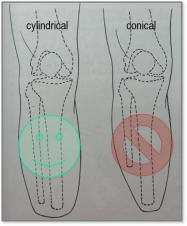
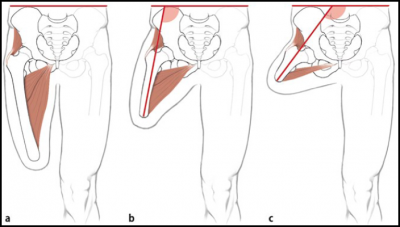
For Long stump (a)
- best lever
- better muscular balance while preserving the strength of the adductors
- energy efficient
- candidate for ischial tuberosity bearing prosthesis
Medium-length stump (b)
- reduced strength of the adductors
- increased flexion and abduction
- increased energy expenditure
Short stump (c)
- weak adductor muscles, causing a severe imbalance
- the position of the stump often ends up in flexion and abduction
- causes massive energy expenditure (effort) and the prosthesis can be heavy
Read more:
- Transfemoral Amputation: Surgical Procedures
- The Transfemoral Amputation Level, Part 2, Surgery and Postoperative Care
Other Types of Amputation in the Lower Limb[edit | edit source]
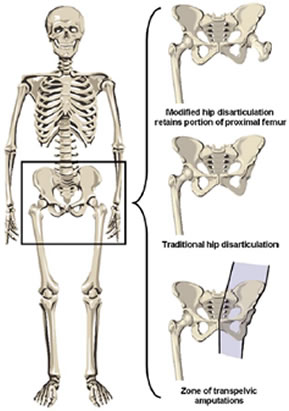
Hip Disarticulation[edit | edit source]
Hip disarticulation is amputation of the whole lower limb through the hip joint. A traditional hip disarticulation is done by separating the ball from the socket of the hip joint, while a modified version retains a small portion of the proximal (upper) femur to improve the contours of the hip disarticulation for sitting. A hip disarticulation results most often from trauma, tumors and severe infections, such as necrotizing fasciitis (commonly referred to as flesh-eating bacteria). Less often, it results from vascular disease and complications of diabetes. [12] Many are wheelchair users but can be considered for ischial tuberosity bearing prosthesis. The risks for wound complications and mortality with this type of amputation is very high.[8]
Hemi-pelvectomy (Hindquarter)[edit | edit source]
Amputation of the whole lower limb and ipsilateral hemi-pelvis[13] This type of amputation is most rare. They are likely to be a wheelchair user, some are considered for a trunk and contralateral ischial tuberosity weight-bearing prosthesis
Read more:
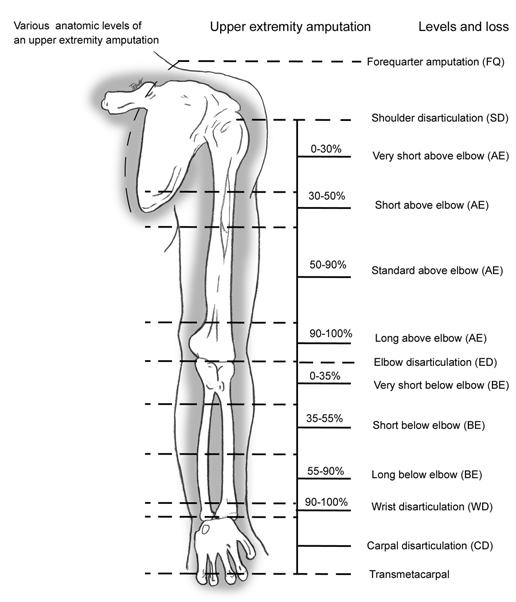
Upper Limb Amputations[edit | edit source]
54% of all upper limb amputations are as a result of trauma; in comparison, only 3% of lower limb amputations are as a result of trauma. Upper limb amputations are seen more rarely than lower limb amputations.
Levels of upper limb amputations:
- Fingers
- Partial hand
- Wrist disarticulation
- Transradial
- Elbow disarticulation
- Transhumeral
- Shoulder disarticulation
- Scapulo-thoracic dissociation (forequarter)
There is a range of different prosthetics available for the upper limb; these range from hooks to passive orthotics that might mainly serve an aesthetic purpose to fully mechanical and functional limbs.
Resources[edit | edit source]
- Definitions of amputation related terms from the Amputee Coalition
- Questions to Ask Your Surgeon
References[edit | edit source]
- ↑ Limb Loss Definitions. Fact Sheet. Amputee Coalition 2008. http://www.amputee-coalition.org/resources/limb-loss-definitions/ [accessed 24 Sep 2017]
- ↑ Clinical Practice Guideline for Rehabilitation of Lower Limb Amputation. Department of Veterans Affairs, Department of Defence. 2007
- ↑ Thomas J. Moore. Planning for Optimal Function in Amputation Surgery. Chapter 3 - Atlas of Limb Prosthetics: Surgical, Prosthetic, and Rehabilitation Principles. 2002
- ↑ 4.0 4.1 Devinuwara K, Dworak-Kula A, O'Connor RJ. Rehabilitation and prosthetics post-amputation. Orthopaedics and Trauma. 2018 Aug 1;32(4):234-40.
- ↑ McNamara et al (1994) Severe Open Fractures of the Lower Extremity: A Retrospective Evaluation of the Mangled Extremity Severity Score (MESS). J Orthop Trauma 8: 81-7
- ↑ Russell et al (1991) Limb Salvage Versus Traumatic Amputation A Decision Based on a Seven-part Predictive Index Ann Surg. 213: 473-81
- ↑ Johansen et al (1990) Objective Criteria Accurately Predict Amputation following Lower Extremity Trauma. J Trauma.30: 568-73
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 8.10 8.11 8.12 8.13 Spires MC, Kelly BM, Davis AJ, editors. Prosthetic restoration and rehabilitation of the upper and lower extremity. Demos Medical Publishing; 2013 Dec 19.
- ↑ Burgess EM, Zettl JH. Amputations below the knee. Artif Limbs. 1969 Jan 1;13(1):1-2. Available at http://www.oandplibrary.org/al/1969_01_001.asp? [Accessed 9 Oct 2017]
- ↑ 10.0 10.1 10.2 10.3 10.4 10.5 10.6 10.7 Guest F, Marshall C, Stansby G. Amputation and rehabilitation. Surgery (Oxford). 2019 Feb 1;37(2):102-5.
- ↑ Wheeless’ Textbook of Orthopaedics: Below Knee Amputation. Available at: http://www.wheelessonline.com/ortho/below_knee_amputation
- ↑ Douglas G. Smith. Higher Challenges: The Hip Disarticulation and Transpelvic Amputation Levels. inMotion, January/February 2005, 15(1).
- ↑ Robert E. Tooms and Frederick L. Hampton. Hip Disarticulation and Transpelvic Amputation: Surgical Procedures. Chapter 21A In: Atlas of Limb Prosthetics: Surgical, Prosthetic, and Rehabilitation Principles.