Diversity of Private Physiotherapy Practice
This article is currently under review and may not be up to date. Please come back soon to see the finished work! (19/05/2020)
Top Contributors - Sonja Murphy, Alexandra Di Florio, Emma Casey, Kieran McKinnon, Kim Jackson, Katy Holmes, Michelle Lee, Aoife Birthistle, 127.0.0.1 and Rachael Lowe
Introduction [edit | edit source]
Physiotherapy is an internationally recognised profession, where the physiotherapist works with service users to identify and encourage their ability to maximise their movement and function while ensuring treatment is patient centred, effective and ethical [1]. A physiotherapist has professional autonomy, allowing the physiotherapist to have the ability and freedom to use their professional judgement regarding assessment, diagnosis, treatment and care within their scope and limits of knowledge and competence [2]. The World Confederation for Physiotherapy (WCPT) define physiotherapy as:
“Physical therapy is concerned with identifying and maximising quality of life and movement potential within the spheres of promotion, prevention, treatment/intervention, habilitation and rehabilitation. This encompasses physical, psychological, emotional, and social wellbeing. Physical therapy involves the interaction between the physical therapist, patients/clients, other health professionals, families, care givers and communities in a process where movement potential is assessed and goals are agreed upon, using knowledge and skills unique to physical therapists [3].”
Physiotherapists can work in a variety of environments from hospitals, private practice clinics, community based rehabilitation centres, outpatient clinics, to schools and workplaces [3]. The scope of physiotherapy is not limited to the role played in a clinic surrounding patient care, but also includes influencing public health strategies, advocating patient health, teaching, research, and helping to develop health policies [3]
The movement from treating acute to chronic conditions due to the ageing population, the cost constraints this shift has on public services, along with the impact of technology are effecting the delivery of healthcare internationally [2], and in turn impacting on the physiotherapy profession. The Canadian Physiotherapy Association state that a change in the scope of practice and development of the physiotherapy profession is associated with this shift of treatment in healthcare; for example practices such as ordering X-rays and screening for orthopaedic surgery which were considered advance practices are now becoming under the scope of practice [4]. The recognition of advanced practitioners in specific areas such as pain and oncology is another development emerging as a result of changes in population and the demands on the healthcare system, therefore broadening the scope of physiotherapy [4].
This plays an important role in the development of private physiotherapy practices, as well as changing physiotherapy roles and broadening the scope of practice. Many people are unaware of the diverse nature of physiotherapy practice as it extends to neurological, oncological, respiratory, and occupational rehabilitation and is not limited to strictly musculoskeletal conditions. Hence, there is a need for increased awareness of these other specialities available to the public and to those who wish to work in these areas.
Neurological Physiotherapy[edit | edit source]
Neurological Physiotherapy is a specialist area of physiotherapy which can often be seen in private practice. It focuses on the treatment of individuals with neurological conditions and disorders that impact the functioning of the brain, spinal cord, and nerves. Stroke, multiple sclerosis, spinal cord injury and Parkinson’s are common neurological conditions [5]. It also includes conditions of the peripheral nervous system such as Guillain Barre Syndrome. Disturbances in the communication of messages between the brain and the body can result in the loss of movement, sensation, co-ordination, and balance. Other aspects of bodily function, such as perception, speech, memory, cognition, and behaviour may also be affected. Due to the complexity of neurological disorders management often involves working as part of a multidisciplinary team including speech and language therapists, occupational therapist, dieticians, nurses, and doctors.[6] A number of interventions are used, often incorporating a selection of the following as appropriate [6]
- Stretching
- Strengthening
- Balance re-education
- Gait re-education
- Joint mobilization
- Electrical stimulation
- Postural exercise
- Spasticity management
- Advice/Education on lifestyle, fatigue management, and exercise
Conditions often seen by physiotherapists in private practice include:
See Neurological Physiotherapy in Private Practice for more detailed overview
Benefits of Private Physiotherapy for Neurological Conditions.[edit | edit source]
A major benefit to private physiotherapy is on achievement of a client’s short term goals, focus shifts immediately to longer term maintenance and progression through a combination of neurophysiotherapy and the use of functional electrical stimulation machines, neuro pilates, personal training, and massage therapy. With the choice of longer and more frequent treatment sessions privately, patients can really experience benefits. Receiving regular physiotherapy can not only impact patients physically, but also psychologically, building patient and family members confidence, positivity, hope, and belief. The video [7] below describes the physical and psychological benefits private physiotherapy brings to the lives of people with a neurological condition and their family members.
Occupational Rehabilitation[edit | edit source]
Vocational or Occupational rehabilitation refers to the services that help enable an individual with a health problem to remain at or return to work by addressing barriers in psychological, functional, cognitive or emotional areas. The emphasis in this type of rehabilitation is on restoring functional abilities in order to work or to perform other occupation related activities rather than treating a specific clinical condition. There is strong evidence that sick absences and disability management services are cost effective with reduction in sick absence by 20-60%[8] . Musculoskeletal disorders are a huge contributor to work related illness and absence from the workplace. Musculoskeletal disorders make up one in eight approved absences from work and the average time on leave being 10 weeks[9]. The estimated number of individuals within the UK who are impacted each year is 2 million with an estimated total of 40 million days of work missed[9]. This equates to roughly 12 billion dollars per year in sickness and absence costs to the UK economy.
The Role of Physiotherapy[edit | edit source]
Physiotherapists are particularly useful to employers and companies because of their skills and experience needed to perform workplace
assessments to help identify and treat the potential cause of injury. Not only does this assist with treating an existing patient, but also with identifying the cause can help reduce the likelihood of another staff member in the same role being injured.
Physiotherapists are able to carry out a variety of tasks that can be beneficial for employers and employees, which include:
- Identifying probable cause of injury
- Developing safe and SMART orientated return to work programmes including exercises to help with work conditioning
- Developing safe and realistic restrictions to prevent further injury when returning to work
- Reducing the likelihood of further injury by addressing areas such as posture, manual handling techniques, ergonomics and workplace practices [10].
There are also benefits to those who are sick or disabled to stay at work where health status permits which include:
- Helps promote recovery within rehabilitation process.
- Minimizes the side effects of long-term sickness absence, which can include physical, mental and social effects.
- Reduces long term incapacity.
- Helps people feel like they contribute to society, maintain their independence, and have autonomy.Improves quality of life [11]
One of the main therapy tools occupational physiotherapists utilize are work hardening exercises that either simulate or mimic tasks that are functional and would normally be performed within an individual’s work setting. Work hardening exercise protocols utilize graded exercise progression to improve physical, psychological and emotional tolerance to exercise that will translate to improve work feasibility. In order to meet a work hardening exercise protocol, its components must address three key elements, which include:
- Exercises that are chosen to help restore deficits in neurological, musculoskeletal or cardiopulmonary function
- Clearly stated intent to improve a patient’s work status
- Clearly stated connection between job demands and the intervention
Work hardening protocols can also include behavioural approaches, pain management, and condition education along with return to work advice.
Within the UK, private physiotherapy companies are providing services to employers to help make the work place safer and help those who are requiring physiotherapy services return to work faster. Many of these companies including are doing this by preventing employees from missing time at work through job analysis, ergonomic assessments, health screening and functional evaluation of employees. One of the benefits for employees who have access to private occupational health services is the quick appointment service with some patients even being seen within less than two days of booking. Along with quick appointment times, physiotherapists working privately can provide more flexible scheduling to meet individual needs. Among other benefits of choosing private occupational services include:
- On site physiotherapy – large-scale companies can benefit from onsite physiotherapy since it allows for direct communication with management staff. Management can be kept up to date with the progress of employees with their consent to assist with scheduling and planning. Along with the direct contact with management, Human resource departments can be kept up to date on current data to better understand causes of absence. With onsite physiotherapy, a therapist can provide services on specified days per week depending on the number of employees required to see and at the request of the employer.
- Health promotion – physiotherapists are able to provide workshops for business or companies that are tailored to the department and the demands placed on the employees themselves. These topics include specific manual handling skills to reduce the risk of injuries, promoting good physical health and being fit for the work demands, which refers to the bodies ability to cope with the specific task.
- Data analysis – private occupational health companies provide data analysis services that allow for better allocation of money and resources for the prevention of further sick absence. The data can be categorized to reflect specific areas including musculoskeletal, medical or psychosocial causes. Having data on sick absence allows for resources to put towards prevention in areas with the most need allowing a shift from a rehab to prehab approach to employee health.
Oncology Physiotherapy[edit | edit source]
So you're interested in working privately as an oncology physiotherapist. This section was developed to give a brief view of the role the physiotherapist has in both the NHS and the private setting. Firstly will give an overlook into the prevalence of cancer in Scotland, followed by the waiting times in the NHS, service evaluation in the NHS and how the services compare in the private sector. Hopefully this will trigger some thought into the current and emerging career pathways physiotherapy has to offer.
Lets first look at the role of the physiotherapist in oncology.
The role of the physiotherapist in Oncology[edit | edit source]
Physiotherapists working in oncology help people that have been diagnosed with cancer, are undergoing treatment, have survived cancer, and also can be involved in palliative care. The CSP has argued for the need for specialist oncology physiotherapists. Physiotherapists can also advise on physical activity after cancer diagnosis. Research has suggested that exercise can decrease the risk of the cancer arising [12].
The physiotherapist has a role in lymphedema[13], mobilisation, managing cancer related fatigue, [14] and even managing fitness for work [15]. These roles are similar whether physiotherapists are working in the NHS or in a private setting. Services that physiotherapists will be involved in can include outpatient's cancer rehab and a musculoskeletal cancer service. Patients can also self refer and so would avoid GP visits whether it is private or within the NHS.
To read more into the opinion of the CSP for the need for more specialist oncological physiotherapists please click here [16].
Reflection Questions:
1. Does the role of an oncological physiotherapist still interest me?
2. Do I want to further investigate if working in the private sector in this area would interest me?
If you have answered "yes" to the above questions, continue reading below. If not return to the mind map in the introduction section and select another speciality that may be of interest.
Next let us look at the prevalence of cancer in Scotland to understand this population group.
Prevalence of cancer in the UK[edit | edit source]
More than 2 out of 5 people living in Scotland will develop some form of cancer. Lung cancer is the most common cancer currently in Scotland according to the data published by the NHS National services Scotland in October 2016[17]. The second highest rate is breast cancer followed by colorectal. In males prostate cancer remains the highest risk while in females, the highest risk is breast cancer. In the UK alone there are currently 2 million cancer survivors. This statistic is projected to increase 3% per annum [18]
Public perceptions of NHS cancer services[edit | edit source]
The Scottish government and MacMillan cancer support compiled a report from a cancer patients experience survey [19]. The main findings showed that the majority of people (94%) said that they had a good experience overall, 84% were linked with a cancer nurse specialist and 87% felt that they were treated with dignity and respect at all times. However, the report did highlight areas of which patient experience could be improved. This included diagnosis where 28% were not informed of the option to bring a family member or friend into the room when hearing their diagnosis, 25% were not made fully aware of what was wrong with them, and one third of patients were not given written information about the type of cancer they had.
Waiting times for NHS cancer treatment services[edit | edit source]
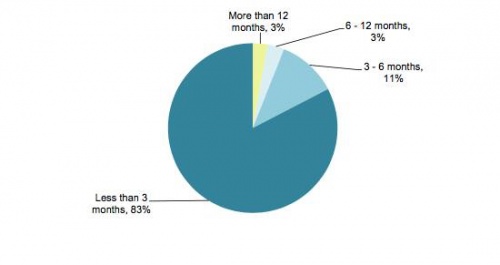
The picture below illustrates the waiting times for seeing their GP after they thought that something may be wrong. Most people see there GP in a timely manner with 83% waiting less than 3 months.
The HEAT standard was developed to ensure quick and timely diagnosis and treatment for those suspected of cancer. It aims to have 95% of patients diagnosed with cancer to begin treatment within 31 days of decision to treat and 95% of those referred urgently with a suspicion of cancer to begin treatment within 62 days of receipt of referral [20].
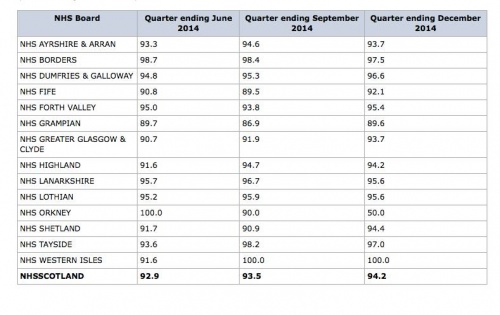
This table below shows the figures for starting treatment within the HEAT standard for NHS Scotland:
We can see that in NHS Scotland performs well in December 2014 at 94.2% were refered within 62 days of receipt of referral. To read further into the HEAT standard clickhere.
NHS and oncological services:[edit | edit source]
To get an understanding of the differences between oncology services in the NHS and the private sector we will provide some information on the services the NHS provides first before looking at private.
Much of the imput the NHS is involved in is in the acute stage. The role of they physiotherapist is intially after cancer treatment, surgery or in the palliative setting. The NHS is continually involved in research to better understand the needs of patients. We saw this earlier in the section when the Scottish government looked at the public's perception of NHS services where patients experiences of using the service is taken in order to improve the service. In a review conducted by Olsen et al[21], the time to care in lung cancer services was examined. This review included studies within the UK and Ireland as well as other countries such as the USA and Australia. Within the UK, in 5 out of 11 studies, the median time from diagnosis to treatment exceeded the NHS National Cancer Plan target of one month. In a day surgery a key outcome for the study in relation to the role of the physiotherapist is the identification of the best time to give patients information about exercise. As a result of the increase in cancer survivors as indicated earlier, there is an increased need for physiotherapy input for a multitude of issues such as mobility. The NHS increasingly work with MacMilllan cancer support to tackle such issues. See below a video on the role of rehabilitation in cancer and how physiotherapist have a huge impact in improving people’s quality of life
Cancer services within private practice[edit | edit source]
Physiotherapists may also work in private hospitals or clinics. The role of a Physiotherapist in a private hospital is similar to those that may work on a ward in the NHS. The Spire Roding hospital [22] is an example of a private hospital that offers private oncology physiotherapy treatments.
Prices include:
Physiotherapy first treatment £80 (one hour)
Physiotherapy £52 (30 mins)
Lymphoedema massage £30 (30 mins) £45 (60 mins)
Physiotherapists can also refer patients into private hospitals for an appointment with a consultant. An example of this can be seen within the Princess Grace Hospital. Waiting times may be shorter to see the consultant than in the NHS and so may attract patients to use their services rather than the NHS. The hospital offers a fixed price treatment. This means that there are no hidden cost after treatment if the patient needs to stay longer for example. Also, people who have health insurance may be covered and so could utilise the facilities of a private hospital instead of going through the NHS. There are hospitals run by insurance companies sure as the Bearwood hospital run by BMI which has access to physiotherapy services directly. Physiotherapists who work here can also refer quickly within the hospital if necessary. Companies such as Aviva include physiotherapy as part of the cover for cancer care. They have no limit on the amount of rehabilitation needed which may give people longer treatment than they may have received in the NHS. This may enable patients to receive further input, if needed, to return to work and daily activities so that patients can return to baseline.
It is important to note that when working in private clincs or practices Physiotherapists will still have to conform to CSP and HCPC guidelines. There may be varying working hours in these types of settings that may suit a newly graduated physiotherapist. When applying for jobs, see what type of further education oppertunites the company offers for improving you knowledge and CPD.
Further resources[edit | edit source]
If oncological physiotherapy is the area that you feel most suited to then we receommend you read these additional resources to gain further knowledge.
Association of chartered physiotherapists in oncology and palliative care [23]
Follow ACPOPC on twitter to get up to date news and research in the field
1. Patients with cancer can sometimes feel as though they are treated as a set of cancer symtoms rather than an individual. What can you do as a physiotherapist in oncology to make a cancer patient feel respected and cared for with a holistic approach?
2. Open communication is key to positive patient experiences in healthcare. What aspects of communication do you feel are important when dealing with a young newly diagnosed cancer patient?
3. Anxiety and depression are commonly seen in cancer patients, impacting patient's effort and motivational levels in physiotherapy. How would you, as a physiotherapist alter your treatment to cope with the emotional turmoil associated with cancer?
Respiratory Physiotherapy[edit | edit source]
This section has been developed to explore the emerging role physiotherapists can play in the private setting for patients suffering from a range of different respiratory illnessess, and will concentrate on chronic obstructive pulmonary disorder (COPD).
So what exactly does a respiratory physiotherapist do?
Respiratory physiotherapists treat a wide range of conditions. These range from COPD and cystic fibrosis, to post surgical patients in intensive care and high dependency units in hospitals. The services of a respiratory physiotherapist can be utilized at any stage of the disease progression, ranging from early diagnosis through to care at the terminal stage.
Aims of Respiratory Physiotherapy[edit | edit source]
One of the main cornerstones of respiratory physiotherapy has been to aid in the removal of secretions. This area of physiotherapy has now developed to include a wide variety of different techniques to help problems associated with respiratory function, including:
• Maintaining/increasing exercise tolerance
• Reducing breathlessness and the work of breathing
• Educating the patient on their condition and improving their knowledge
• Improve their capability to engage in daily functional activities
Reflection Questions:
1. Does the role of a respiratory physiotherapist still interest me?
2. Do I want to further investigate if working in the private sector in this area would interest me?
If you have answered "yes" to the above questions, continue reading below. If not return to the mind map in the introduction section and select another speciality that may be of interest.
Prevalence of Lung Disease[edit | edit source]
Lung disease is believed to affect approximately 12.7 million people in the UK [24] ranging from asthma, COPD and other long-term respiratory illnesses. COPD is the fifth leading cause of death in the UK, beaten only by cardiovascular disease and cancer [25]
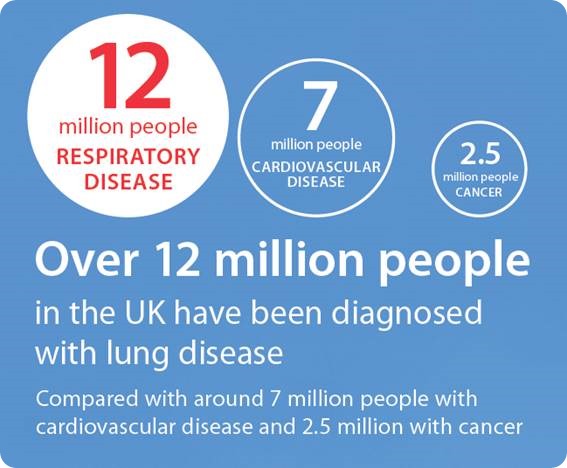
Figure 1: British Lung Foundation, viewed October 2016
Each year, lung diseases are responsible for a large number of hospital admissions. In 2011, 694,000 patients were admitted, with 6,120,400 bed-days due to lung disease [24]. Figure 1 demonstrates the different number of people diagnosed with lung disease compared to cardiovascular disease and cancer.
Research has suggested that the prevalence of lung disease in the UK is growing. For example, the diagnosis of COPD has increased by approximately 27% in the last 10 years, from under 1600 to 2000 people per 100,000 These figures[24]demonstrate that lung disease is a potentially massive burden on the NHS, with interventions needed to address the treatment plans for these patients.
Pulmonary Rehabilitation[edit | edit source]
Pulmonary rehabilitation is a non-pharmacological program designed to help patients with chronic respiratory disease. There are numerous different components of this rehabilitation, such as exercise training, disease education and behavioral interventions [26]. It has been shown to significantly improve symptoms associated with chronic respiratory diseases, such as dyspnea, as well as increasing exercise capacity [27]
Pulmonary rehabilitation classes generally last from between 6-8 weeks, with 1-2 sessions a week. People with a variety of respiratory conditions can attend, with the most common condition being COPD. It consists of a group exercise program, followed by an educational talk to increase their knowledge regarding their respiratory disease. The sessions are supervised by a health professional. To be allowed to attend a pulmonary rehabilitation class with the NHS, their GP or district nurse must first refer patients, if they are deemed suitable.
Hospitalisation due to exacerbations of COPD cause the NHS a huge economic burden, with an annual cost of £810 to £930 million. It results in 1.4 million GP visits a year, as well as 1 million bed days a year [26]. Pulmonary rehabilitation has been proven to help prevent flare ups of COPD, thus helping reduce the burden of these illnesses on the NHS.
Potential Barriers to Pulmonary Rehabilitation[edit | edit source]
However, although there are obvious benefits associated with pulmonary rehabilitation, it is not without its downside. Due to the need to be referred to these classes, it increases the waiting time for the attendance of classes. Issues with patient compliance have also been documented. Attendance is as low as 50% [28], with 23-31% of patients failing to complete the course. Due to patients not showing up for classes, this prevents other patients from accessing this service, hindering them in their rehabilitation and increasing waiting list times for the classes.
A recent study highlighted a few problems associated with pulmonary rehabilitation classes provided by the NHS. Patient interviews drew attention to a number of different issues with these rehabilitation classes. Some found transport and parking to be an issue, whilst others found the timing of the classes and the day of the week to not suit them [29]. Accessing physiotherapy privately would offer them the opportunity to discuss other options with the physiotherapist, allowing patients more autonomy with the timing and location of their classes. As people may be working full time, this gives them the choice to obtain physiotherapy outside of their working hours, helping progress their rehabilitation.
Another possible barrier for attendance of these classes was the environment in which they were held, which can potentially be intimidating to patients. A study carried out by Hogg et al.[30] discovered that being surrounded by fit and healthy people was disconcerting to people suffering from respiratory disease.
One patient interviewed felt intimidated by the other so-called 'healthy' users of the gym. 
If people were offered their own rehabilitation classes in a more private discreet setting, offering them the opportunity to feel comfortable in their surroundings, patient compliance with the programme could potentially increase.
As pulmonary rehabilitation classes generally only last between 6-8 weeks, patients aren’t able to avail of these services after the program has finished, instead relying on themselves to continue their exercises. It can be argued that if patients have enough motivation to proceed with these classes, thus increasing their quality of life and ability to carry out functional activities, they will be willing to pay the extra cost of the rehabilitation.
Another point of interest highlighted in the study by Hogg et al.[30] showed that some participants were worried about carrying out their rehabilitation without the comforting presence of medical staff.
Without a doubt pulmonary rehabilitation classes provided by the NHS are an invaluable resource, but this extra comfort provided by physiotherapists after their course has concluded would encourage patients to continue in their rehabilitation and to not halt their progess.
What services are available at the moment?[edit | edit source]
The cost of private respiratory physiotherapy consultations and treatments range from £50 - £80 per treatment. There are a range of different respiratory physiotherapy services available in the private sector. For example, BUPA offer coverage for respiratory conditions ranging from pulmonary rehabilitation classes, hydrotherapy and pilates for breathing disorders.
By registering with the CSP website on the Physio2u page [31] respiratory physiotherapists can advertise their services to the public.
Health Considerations for Patients[edit | edit source]
As patients suffering from respiratory disease, they may have a wide range of different delibitating symptoms.
It is important for physiotherapists to keep this in mind when treating their own patients.
A service specification carried out by the NHS outlined a few recommendations for pulmonary rehabilitation. The healthcare provider running the classes must have knowledge of the diagnosis, recent spirometry results, relevent medical history, MRC dysponea score, oxygen saturation if possible, recent relevent clinical tests and drug management [32]
For more information regarding this service, including more comprehensive examinations, staffing and equipment, please click here [33]
The next stage: Setting up your own private practice[edit | edit source]
If you are still considering working in or setting up a private practice, below are a number of areas and points to be considered before entering this field. This section will detail different models of private practice as discussed in the CSP’s “Thinking of Private Practice: A guide for physiotherapists” [34], including financial, equipment and marketing matters.
What are the options for working in private practice?[edit | edit source]
• Treating the occasional private patient – any chartered physiotherapist can accept private business from a self-referring patient, or on referral from any other professional.
• Working as a support worker in a private practice - it is possible for Associate members to work as self-employed private practitioners. To remain within the scope of practice of a CSP Associate member, it is essential that your work is delegated to you by a registered physiotherapist, which requires a formal arrangement between you and a physiotherapist. In private practice this will need to be determined by the written “contract-for-services” that you will create as the legal basis for the operation of your services.
• Becoming a partner in an existing practice - if you are considering becoming a partner or entering into a directorship, legal and financial advice should always be sought and a formal partnership or directorship agreement will need to be established.
• Purchasing an existing practice – it is possible to purchase an existing practice that is already up and running with its own equipment and clientele. Businesses are often advertised in CSP’s Frontline publication, Physio First’s in Touch Journal as well as in local papers.
• Setting up a new practice - a practice can be owned by a sole proprietor, by a partnership of two or more people, or by Directors of a Limited Company. Each of these scenarios will have different tax and legal implications, and these should be considered before choosing which is the most appropriate for your circumstances.
What are the different types of practice?[edit | edit source]
• Partnership
For this type of practice, two or more people share the risks, costs and responsibilities of being in business. Partners do not enjoy any protection if the business fails. Each partner is self-employed and takes a share of the profits.
• Sole Trader
A sole trader runs their business as an individual. You are responsible for all aspects of the business and you pay personal tax on the profits of your business. You will be personally liable for any debts incurred, meaning that this could be a risky option for businesses that need a lot of investment.
Advantages: independence, any profits made go to you.
Disadvantages: lack of support, unlimited liability, and personal responsibility for any business debts.
• Limited companies
Limited companies exist in their own right and company finances are distinct from the personal finances of their owners. Shareholders are not responsible for the company’s debts unless they have given guarantees however, they may lose any money they have invested if the company fails.
What types of referrals will be received in private practice?[edit | edit source]
• GP referrals – there are a number of factors that may impact upon referrals from GP’s such as the GP being responsible for purchasing physiotherapy services for their community. It is important here to highlight that GPs do not directly commission health services in Wales, Scotland or Northern Ireland. As a physiotherapist you may need to apply to the GP directly to become capable of providing physiotherapy services to a particular community.
• Self referral – this will be the majority of the type of patients you will see in private practice as they are the most important market segment for independent practitioners. Evidence from self referral pilot studies by the Department of Health has delineated that people who self-refer to physiotherapy take fewer days off work and are 50% less likely to be off work for longer than one month when compared with people referred from other pathways.
• Health insurance companies – there are two choices for practitioners:
Patients pay for services directly to the practice and are advised to follow up with their insurance company.
OR
Practitioners complete insurance claim forms to be reimbursed for services by the insurance company. The majority of insurance companies will use a GP or specialist as a pathway to a physiotherapist. Some companies however, will accept claims for patients who self-refer. It is important to note that some insurance companies may limit the number of sessions reimbursed per course of treatment.
• Commercial intermediary companies – these companies handle the management of claims for insurers. For instance, for a person who has been in a car accident, their insurance company may pass their details to a commercial intermediary company who may then:
Arrange for a referral to a physiotherapist.
Pass the details to a legal representative.
Some of these companies offer inducements (CAUTION!!!) and many will limit the number of sessions and insist upon certain pathways and protocols to be used.
Starting a Private Practice[edit | edit source]
Reflection Questions:
1. Am I still interested in private practice?
2. If "yes", what aspects of private practice are appealing to me and why? What are the potential barriers holding me back from starting a private practice?
There are a number of points for consideration below to be contemplated before venturing further:
Experience[edit | edit source]
As a private physiotherapist it is imperative that you have the necessary skills for assessment, diagnosis and treatment. In private practice it is your responsibility to keep updated with continuing professional development (CPD) and deciding when and how time will be allocated to your CPD.
Status of Employment[edit | edit source]
If you are offered a position on a self-employed basis, you should ensure that you receive a written “contract for services”, which summarises the proposed relationship and arrangements. If you are hired as an employee then you should receive a “contract of employment” that outlines the main terms and conditions of employment. In either case, you should be absolutely clear about what is contained in the contract as it should summarise the relationship between you and the Practice Owner/Employer and set out the expectations for all involved. As a CSP member working in private practice as an employee, you will have a range of employment rights and obligations in a similar way to those that would apply if you were employed in any other workplace or organisation. Should you encounter difficulties in the workplace you can contact the Society’s Employment Relations and Union Services (ERUS) staff for advice.
If you are working on a self-employed basis, you are not covered by the same employment rights that apply to employees. There are therefore only limited areas in which ERUS is able to assist such members; these include access to some aspects of ERUS legal services, support with responding to a complaint made against them to the HPC, and initial assistance in determining their employment status if this is unclear. However, self-employed CSP members who are also members of Physio First will be able to access further advice.
Professional Conduct and Responsibilities[edit | edit source]
The CSP’s Code of Members' Professional Values and Behaviour [35] outlines the professional values and behaviour that all CSP members must adhere to regardless of whether you are working in the NHS or private practice. It is your responsibility as a CSP member to comply to the regulatory requirements, the law and the requirements of your employing organization (where appropriate).
Business Planning[edit | edit source]
Before setting off on this venture, it is advised that you seek advice, develop a business plan and evaluate risk. A business plan can also form the basis of any developments in the future. You should consider the following issues:
• Demand for your service
• Competition
• Marketing
• Charge for services
• Who will buy your services
• Extra costs involved
• Facility and equipment
• Insurance
For further details on business plans and how to develop them, please click here [36]
Fees[edit | edit source]
In terms of cost for services, it is good business practice to give an indication of fees and the likely number and frequency of treatments before a programme commences. "Cash sales" means all income from your main business activity which is received at the conclusion of a course of treatment. Your cash sales income will be from patients paying your fees out of their own pocket and from patients covered by health insurance who will pay you and then claim the cost from the insurance company after the treatment has been completed. If a patient needs a course of treatment (more than one appointment), you may decide to charge them after each treatment rather than at the end of the course to improve your cash flow. Income from patients that are covered by health insurance but who will pass you the claim forms at the end of the treatment for you to claim from the insurance company will be "cash from debtors".
Expenditure, Finance and Running Costs[edit | edit source]
There are some costs that may not initially be considered but are imperative to the successful running of a private practice.
• Wages – this will be wages for staff hired by the practice or for services required from other professionals e.g. other physiotherapists, physiotherapy assistants, receptionist/secretary, accountant, solicitor.
• Stationery – pens, appointment and treatment cards, headed notepaper, brochures etc. will be needed and should be professionally produced.
• Uniforms and equipment - private practices may or may not provide uniforms. Within private practices it is typically the responsibility of the owner to provide the equipment and this can vary depending on contracts and the physiotherapist’s role in the private practice. In the case of a self employed physiotherapist, their uniform needs to be provided at their own expense as does any equipment they deem necessary in treatment provision.
• Bills - this can include internet and telephone, property rent, electricity and heating, advertising, security systems etc.
Insurance[edit | edit source]
The extent of insurance required by any private practitioner is dependent on a number of factors and circumstances. Members of the CSP are covered for professional liability. The CSP has produced information papers on Scope of Physiotherapy Practice [37]in the UK, and separately on the CSP professional liability insurance (PLI) scheme [38] Both documents provide the information needed in this area. Working in private practice, you may need some or all of the following types of insurance:
• Professional liability insurance
• Public liability
• Insurance to cover risks with equipment
• Employer’s liability insurance
• Loss of earnings
• Premises
Value added Tax (VAT)[edit | edit source]
HPC registered physiotherapists are exempt from registration for payment of VAT for the provision of physiotherapy treatment even if their turnover is in excess of the statutory limit. This also means that the practitioner may not recover VAT on items of expenditure. However, if activities like consultancy and medico-legal work are carried out, these do not count towards the VAT limit, and VAT-registered practitioners may reclaim VAT on expenditure made in providing these services. This however is only usually the case in practices that specialise in these areas.
Income Tax[edit | edit source]
In terms of being able to claim tax relief, you can claim back on the annual subscription to the CSP, the annual HPC registration fee and the Physio First subscription, as well as laundry and uniform costs, in addition to all allowable business expenses. Annual accounts are essential for Inland Revenue purposes, and again the advice of a qualified accountant is recommended, although the Inland Revenue can in many instances give helpful advice.
How do you let people know that you and your practice exist?[edit | edit source]
The simple answer: market yourself! The CSP’s Code of Professional Values and Responsibilities [35]outlines what is and isn’t appropriate in terms of advertising, canvassing and publicity, therefore make sure you thoroughly read this document before you go any further with your marketing. Who you decide to connect with will depend on the specialty of your practice, but as a few suggestions, to make your practice known you can get in contact with GPs, consultants, private hospitals, nursing homes/rest homes, sports clubs etc.
Next Steps[edit | edit source]
This guide, with the help of the CSP’s “Thinking of Private Practice: A guide for physiotherapists” has provided some brief information on the areas you will need to consider as private physiotherapist. Before taking that final step into private practice, it is strongly advised that you talk to some private-practitioners and visit their practices; contact Physio First; and seek business, financial and legal advice.
Conclusion-Future Planning[edit | edit source]
This summary reiterates some of the main points from our learning resource.
The role of a physiotherapist is constantly developing due to the change in healthcare services and provisions. Throughout this wiki we have highlighted some the diversities found within the private sector of physiotherapy such as opportunities within neurological, oncological, respiratory and occupational rehabilitation. We have also demonstrated the many benefits of having these services available to service users. As mentioned above, there are many points to consider before becoming part of the private sector or setting up your own practice.
Throughout the Wiki we have provided further resources to broaden and expand your knowledge in specialities which may interest you. Further guidelines and further steps to establish yourself within the private physiotherapy sector have been discussed.
We would recommend if you are considering a career within private physiotherapy to take a look at the Physio First website [39].
Physio First [39][47][71][71][87]is an organisation that represents physiotherapists working in private practice. Any fully subscribing CSP member who is self-employed in private practice is eligible for membership. In addition, any fully subscribing member of the CSP who is employed by a full member of Physio First is eligible for affiliated membership. If you decide to work in private physiotherapy, it is highly recommended that you join Physio First.
References[edit | edit source]
- ↑ Chartered Society of Physiotherapy. Physiotherapy Framework: putting physiotherapy behaviours, values, knowledge and skills into practice. Chartered Society of Physiotherapy:2013. 40p. Available from: https://v3.pebblepad.co.uk/v3portfolio/csp/Asset/View/6jqbh3GzhGWrrcGqpknwmZzh8Z
- ↑ 2.0 2.1 Higgs, J.,Refshauge, K., Ellis, E.. Portrait of the Physiotherapy Profession. Journal of Interprofessional Care. 2001; 15(1):79-89.
- ↑ 3.0 3.1 3.2 World Confederation for Physical Therapy. Policy statement: Description of physical therapy. World Confederation for Physical Therapy: 2001. 12p. Available from: http://www.wcpt.org/policy/ps-descriptionPT
- ↑ 4.0 4.1 Canadian Physiotherapy Association. Description of Physiotherapy in Canada. Ottawa (CA): Canadian Physiotherapy Association; 2012. 17p. Available from: https://physiotherapy.ca/description-physiotherapy
- ↑ Neurological Alliance of Scotland. Neurological conditions factsheet. Available from: http://www.scottishneurological.org.uk/content/res/Neurological_Conditions_Factsheet.pdf (Accessed 31st October 2016).
- ↑ 6.0 6.1 Neurological Physiotherapy Information Guide and Resource Centre. Neurological physiotherapy. Available from:http://neurologicalphysiotherapy.comfckLR(Accessed 31st October 2016).
- ↑ Challenge Center. Challenge center video 2014. Available from: https://www.youtube.com/watch?v=TDGETLa4Bm8 (Accessed 3rd November 2016).
- ↑ Waddell, G., Burton, K., Kendall, N. Vocational rehabilitation: what works, for whom and when? 2008; 2-303. Available from: https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/209474/hwwb-vocational-rehabilitation.pdf
- ↑ 9.0 9.1 Addley, K., Burke, C., McQuillan, P.. Impact of a direct access occupational physiotherapy treatment service. 2010; 60: 651-653.
- ↑ Physiomed. 2016. Available from: http://www.physiomed.co.uk/pages/physio-med-provides-quality-and-affordable-occupational-physiotherapy-and-ergonomic-solutions
- ↑ NHS Scotland. Getting Vocational rehabilitation working for Scotland: education needs of staff supporting vocational rehabilitation. 2008; 1-37. Available from: http://www.gov.scot/resource/doc/924/0077375.pdf
- ↑ CSP. Physios play key role in cancer care. Available from: http://www.csp.org.uk/frontline/article/physios-play-key-role-cancer-care [Accessed 25th November 2016]
- ↑ Lacomba MT, Sánchez MJ, Goñi ÁZ, Merino DP, del Moral OM, Téllez EC, Mogollón EM. Effectiveness of early physiotherapy to prevent lymphoedema after surgery for breast cancer: randomised, single blinded, clinical trial. Bmj. 2010 Jan 13 Available from: doi 340:b5396, [Accessed 25th November 2016]
- ↑ Donnelly CM, Lowe-Strong A, Rankin JP, Campbell A, Allen JM, Gracey JH. Physiotherapy management of cancer-related fatigue: a survey of UK current practice. Supportive care in cancer. 2010 Jul 1;18(7):817-825.
- ↑ Chartered Society of Physiotherapy. Information paper: Fitness for work. March 2016.
- ↑ Chartered society of physiotherapy. Physios play key role in cancer care. August 2013; 19(14). Available from: http://www.csp.org.uk/frontline/article/physios-play-key-role-cancer-care. (Accessed 2nd December 2016).
- ↑ Cancer in Scotland (October 2016): Information Services Division, NHS National Services Scotland
- ↑ Maddams J, Utley M, Møller H. Projections of cancer prevalence in the United Kingdom, 2010–2040. British journal of cancer. 2012 Sep 25;107(7):1195-202.
- ↑ NHS Scotland. Scottish Cancer Patient Experience Survey 2015/16. Available from:http://www.gov.scot/Publications/2016/06/3957/downloads. [Accessed 25th November 2015].
- ↑ Scottish Government. Cancer waiting times. Available from: http://www.gov.scot/About/Performance/scotPerforms/NHSScotlandperformance/CWT-LDP [Accessed: 25th November 2016]
- ↑ Olsson JK, Schultz EM, Gould MK. Timeliness of care in patients with lung cancer: a systematic review. Thorax. 2009 Sep 1;64(9):749-56.
- ↑ Spire Roding hospital. 2016. [Accessed 1 December 2016]. Available: http://www.spirehealthcare.com/roding/physiotherapy/-oncology-physiotherapy-treatments/
- ↑ ACPOPC. Association of Chartered Physiotherapists in Oncology and Palliative Care. Available from: http://acpopc.csp.org.uk. (Accessed 2nd December 2016).
- ↑ 24.0 24.1 24.2 British Lung Foundation. Lung disease in the UK. Available from: https://statistics.blf.org.uk/. ( Accessed 18th November 2016).
- ↑ Masoli M, Fabian D, Holt S, Beasley R. The global burden of asthma: executive summary of the GINA Dissemination Committee Report. Allergy. 2004; 59(5): 469-478.
- ↑ 26.0 26.1 Hayton C, Clark A, Olive S, Browne P, Galey P, Knights E, Staunton L, Jones A, Coombes E, Wilson A. Barriers to pulmonary rehabilitation: Characteristics that predict patient attendance and adherence. Respiratory Medicine. 2013; 107(3): 401-407.
- ↑ Nici L, Donner C, Wouters E, Zuwallack R, Ambrosino N, Bourbeau J, Carone M, Celli B, Engelen M, Fahy B, Garvey C, Goldstein R, Gosselink R, Lareau S, MacIntyre N, Maltais F, Morgan M, O'Donnell D, Prefault C, Reardon J, Rochester C, Schols A, Singh S, Troosters T. American Thoracic Society/European Respiratory Society Statement on Pulmonary Rehabilitation. American Journal of Respiratory and Critical Care Medicine. 2006; 173(12): 1390-1413.
- ↑ Keating A, Lee A, Holland A. What prevents people with chronic obstructive pulmonary disease from attending pulmonary rehabilitation? A systematic review. Chron Respir Dis. 2011; 8(2): 89-99.
- ↑ De Sousa Pinto J, Martin-Nogueras A, Morano M, Macedo T, Arenillas J, Troosters T. Chronic obstructive pulmonary disease patients' experience with pulmonary rehabilitation: A systematic review of qualitative research. Chronic Respiratory Disease. 2013; 10(3): 141-157.
- ↑ 30.0 30.1 Hogg L, Grant A, Garrod R, Fiddler H. People with COPD perceive ongoing, structured and socially supportive exercise opportunities to be important for maintaining an active lifestyle following pulmonary rehabilitation: a qualitative study. Journal of Physiotherapy. 2012;58(3):189-195.
- ↑ CSP, List your practice on Physio2u. Available from: http://www.csp.org.uk/your-health/find-physio/list-your-practice-physio2u. (Accessed 2nd December 2016).
- ↑ Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease: GOLD Executive Summary Updated 2003. COPD: Journal of Chronic Obstructive Pulmonary Disease. 2004;1(1):105-141.
- ↑ Anon, (2016). [online] Available at: : /https://www.brit-thoracic.org.uk/document-library/clinical-information/pulmonary-rehabilitation/bts-guideline-for-pulmonary-rehabilitation/ [Accessed 18 Nov. 2016].
- ↑ CSP, 2011. Thinking or Private Practice: A guide for physiotherapists [online]. [Viewed 10 November 2016]. Available from: www.csp.co.uk/publications/thinking-private-practice-guide-physiotherapists
- ↑ 35.0 35.1 CSP, Code of members' professional values and behaviour. 2011. Available from: http://www.csp.org.uk/publications/code-members-professional-values-behaviour. (Accessed 2nd December 2016).
- ↑ CSP, Making the business case. Available from: http://www.csp.org.uk/professional-union/practice/your-business/making-business-case. (Accessed 2nd December 2016).
- ↑ CSP, Scope of practice. Available from: http://www.csp.org.uk/professional-union/professionalism/scope-of-practice. (Accessed 2nd December 2016).
- ↑ CSP, CSP PLI scheme. July 2016. Available from: http://www.csp.org.uk/professional-union/practice/insurance/csp-pli-scheme. (Accessed 2nd December 2016)
- ↑ 39.0 39.1 Physio first, Physio First is changing. Available from: http://www.physiofirst.org.uk. (Accessed 2nd December 2016)