Lumbar Differential Diagnosis: Difference between revisions
No edit summary |
No edit summary |
||
| Line 4: | Line 4: | ||
Low back pain is a common presenting condition in physiotherapy clinics. The physiotherapy assessment aims to screen for serious spinal conditions and identify impairments that may have contributed to the onset of the pain, or which increase the likelihood of an individual developing persistent pain. These include '''biological factors''' (eg. weakness, stiffness), '''psychological factors''' (eg. depression, fear of movement and catastrophisation) and '''social factors''' (eg. work environment).<ref>M.Hancock. Approach to low back pain. RACGP, 2014, 43(3):117-118.</ref> | Low back pain is a common presenting condition in physiotherapy clinics. The physiotherapy assessment aims to screen for serious spinal conditions and identify impairments that may have contributed to the onset of the pain, or which increase the likelihood of an individual developing persistent pain. These include '''biological factors''' (eg. weakness, stiffness), '''psychological factors''' (eg. depression, fear of movement and catastrophisation) and '''social factors''' (eg. work environment).<ref>M.Hancock. Approach to low back pain. RACGP, 2014, 43(3):117-118.</ref> | ||
Once [[An Introduction to Red Flags in Serious Pathology|serious spinal pathology]] and specific causes of back pain have been ruled out, an individual is classified as having non-specific low back pain. If no serious pathology is suspected, there is no indication for x-rays or MRI diagnostic imaging unless the results of imaging may change / guide the management protocol.<ref>Hall AM, Aubrey-Bassler K, Thorne B, Maher CG. [https://www.bmj.com/content/372/bmj.n291.full Do not routinely offer imaging for uncomplicated low back pain.] bmj. 2021 Feb 12;372.</ref><ref>Almeida M, Saragiotto B, Richards B, Maher C. Primary care management of non-specific low back pain: key messages from recent clinical guidelines. Med J Aust 2018; 208 (6): 272-275</ref> | Once [[An Introduction to Red Flags in Serious Pathology|serious spinal pathology]] and specific causes of back pain have been ruled out, an individual is classified as having non-specific low back pain. If no serious pathology is suspected, there is no indication for x-rays or MRI diagnostic imaging unless the results of imaging may change / guide the management protocol.<ref>Hall AM, Aubrey-Bassler K, Thorne B, Maher CG. [https://www.bmj.com/content/372/bmj.n291.full Do not routinely offer imaging for uncomplicated low back pain.] bmj. 2021 Feb 12;372.</ref><ref>Almeida M, Saragiotto B, Richards B, Maher C. Primary care management of non-specific low back pain: key messages from recent clinical guidelines. Med J Aust 2018; 208 (6): 272-275</ref> | ||
90% of patients presenting to primary care with low back pain are classified as having [[Non Specific Low Back Pain|non-specific low back pain]].<ref>Traeger A, Buchbinder R, Harris I, Maher C. Diagnosis and management of low-back pain in primary care. CMAJ. 2017 Nov 13;189(45):E1386-E1395.</ref><ref>Koes BW, Van Tulder M, Thomas S. Diagnosis and treatment of low back pain. Bmj. 2006 Jun 15;332(7555):1430-4.</ref> Non-specific low back pain is defined as "low back pain not attributable to a recognizable, known specific pathology<ref>Otero-Ketterer E, Peñacoba-Puente C, Ferreira Pinheiro-Araujo C, Valera-Calero JA, Ortega-Santiago R. [https://www.mdpi.com/1660-4601/19/16/10145 Biopsychosocial Factors for Chronicity in Individuals with Non-Specific Low Back Pain: An Umbrella Review]. International Journal of Environmental Research and Public Health. 2022 Aug 16;19(16):10145.</ref> (eg, infection, [[Skeletal Metastases|tumor]], [[osteoporosis]], [[Lumbar Spine Fracture|lumbar spine fracture]], [[Congenital Spine Deformities|structural deformity]], inflammatory disorder, [[Lumbar Radiculopathy|radicular syndrome]], or [[Cauda Equina Syndrome|cauda equina syndrome]])."<ref>Balagué, Federico, et al. "Non-specific low back pain." The Lancet 379.9814 (2012): 482-491. Level of evidence 1A</ref> | 90% of patients presenting to primary care with low back pain are classified as having [[Non Specific Low Back Pain|non-specific low back pain]].<ref>Traeger A, Buchbinder R, Harris I, Maher C. Diagnosis and management of low-back pain in primary care. CMAJ. 2017 Nov 13;189(45):E1386-E1395.</ref><ref>Koes BW, Van Tulder M, Thomas S. Diagnosis and treatment of low back pain. Bmj. 2006 Jun 15;332(7555):1430-4.</ref> Non-specific low back pain is defined as "low back pain not attributable to a recognizable, known specific pathology<ref>Otero-Ketterer E, Peñacoba-Puente C, Ferreira Pinheiro-Araujo C, Valera-Calero JA, Ortega-Santiago R. [https://www.mdpi.com/1660-4601/19/16/10145 Biopsychosocial Factors for Chronicity in Individuals with Non-Specific Low Back Pain: An Umbrella Review]. International Journal of Environmental Research and Public Health. 2022 Aug 16;19(16):10145.</ref> (eg, infection, [[Skeletal Metastases|tumor]], [[osteoporosis]], [[Lumbar Spine Fracture|lumbar spine fracture]], [[Congenital Spine Deformities|structural deformity]], inflammatory disorder, [[Lumbar Radiculopathy|radicular syndrome]], or [[Cauda Equina Syndrome|cauda equina syndrome]])."<ref>Balagué, Federico, et al. "Non-specific low back pain." The Lancet 379.9814 (2012): 482-491. Level of evidence 1A</ref> | ||
| Line 10: | Line 10: | ||
Non-specific low back pain is usually categorised into 3 subtypes: acute, sub-acute and chronic low back pain.<ref>Hock M, Járomi M, Prémusz V, Szekeres ZJ, Ács P, Szilágyi B, Wang Z, Makai A. [https://www.mdpi.com/1660-4601/19/19/12024 Disease-Specific Knowledge, Physical Activity, and Physical Functioning Examination among Patients with Chronic Non-Specific Low Back Pain.] International Journal of Environmental Research and Public Health. 2022 Sep 23;19(19):12024.</ref> This subdivision is based on how long the individual has had low back pain. Acute low back pain is an episode of low back pain that has been present for less than 6 weeks, sub-acute low back pain has been present for between 6 and 12 weeks and chronic low back pain has been present for 12 weeks or more.<ref>Burton AK, Tillotson KM, Main CJ, Hollis S. Psychosocial predictors of outcome in acute and subchronic low back trouble. Spine (Phila Pa 1976). 1995 Mar 15;20(6):722-8.Level of evidence 3C</ref> | Non-specific low back pain is usually categorised into 3 subtypes: acute, sub-acute and chronic low back pain.<ref>Hock M, Járomi M, Prémusz V, Szekeres ZJ, Ács P, Szilágyi B, Wang Z, Makai A. [https://www.mdpi.com/1660-4601/19/19/12024 Disease-Specific Knowledge, Physical Activity, and Physical Functioning Examination among Patients with Chronic Non-Specific Low Back Pain.] International Journal of Environmental Research and Public Health. 2022 Sep 23;19(19):12024.</ref> This subdivision is based on how long the individual has had low back pain. Acute low back pain is an episode of low back pain that has been present for less than 6 weeks, sub-acute low back pain has been present for between 6 and 12 weeks and chronic low back pain has been present for 12 weeks or more.<ref>Burton AK, Tillotson KM, Main CJ, Hollis S. Psychosocial predictors of outcome in acute and subchronic low back trouble. Spine (Phila Pa 1976). 1995 Mar 15;20(6):722-8.Level of evidence 3C</ref> | ||
== Diagnosis versus Classification == | == Diagnosis versus Classification == | ||
Diagnosis is typically looked at as a pathoanatomical model, whereas the goal of classification systems is to guide treatment | Diagnosis is typically looked at as a pathoanatomical model, whereas the goal of classification systems is to guide treatment, so that clinicians don't treat all cases of back pain the same. If a patient does not have a clear diagnosis, they are referred to as having [[Non Specific Low Back Pain|non-specific low back pain.]] | ||
== Imaging == | == Imaging == | ||
For more information on referring for imaging, please see [[Practical Decision Making in Physiotherapy Practice]], but to summarise: | |||
* | * imaging is needed if red flags are present or if there is no improvement with conservative care within 6 weeks. If you are unsure about a red flag, you can often treat a little to see if they improve. | ||
* | * imaging is recommended if it will change the course of treatment<ref>Al-Hihi E, Gibson C, Lee J, Mount RR, Irani N, McGowan C. [https://bmjopenquality.bmj.com/content/11/1/e001539.abstract Improving appropriate imaging for non-specific low back pain.] BMJ Open Quality. 2022 Feb 1;11(1):e001539.</ref> | ||
* | * a lot of imaging findings correlate with low back pain. This doesn’t mean everyone with imaging findings has pain, but often the more findings there are, the higher the chance the person has pain. We can still help these people though! | ||
== Differential Diagnosis == | == Differential Diagnosis == | ||
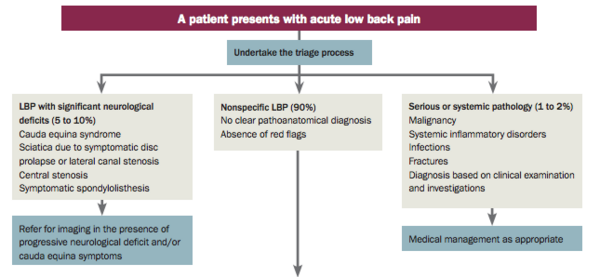
Initially, you should complete a | Initially, you should complete a comprehensive [[Lumbar Assessment|lumbar assessment]]. Once this is complete, you then triage the patient, as explained in the Lumbar Assessment page, by the image below: | ||
[[File:LBP Triage.png|frameless|600x600px]] | [[File:LBP Triage.png|frameless|600x600px]] | ||
You will need knowledge of [[Red Flags in Spinal Conditions|Red Flags]] and conditions that can cause neurological deficits, such as those listed below (see linked pages for more information). | |||
*[[Specific Low Back Pain]] | *[[Specific Low Back Pain]] | ||
| Line 37: | Line 36: | ||
* Thoraco-Lumbar Junction Syndrome | * Thoraco-Lumbar Junction Syndrome | ||
Physiotherapists have valuable assessment skills and clinical reasoning skills when an individual has an unclear presentation. A few key factors to consider when looking at a differential diagnosis:<ref name=":0">Rainey N. Differential Diagnosis Course. Physiopedia Plus. 2023.</ref> | |||
* [[Neurological Assessment|Neurological testing]] isn't an exact diagnosis but it gives a very good indication of where the problem lies, how to treat the patient and what to avoid to prevent injury or flare up.<ref name=":0" /> | * [[Neurological Assessment|Neurological testing]] isn't an exact diagnosis but it gives a very good indication of where the problem lies, how to treat the patient and what to avoid to prevent injury or flare up.<ref name=":0" /> | ||
Revision as of 10:27, 22 February 2023
Top Contributors - Jess Bell, Carin Hunter, Jorge Rodríguez Palomino and Ewa Jaraczewska
Introduction[edit | edit source]
Low back pain is a common presenting condition in physiotherapy clinics. The physiotherapy assessment aims to screen for serious spinal conditions and identify impairments that may have contributed to the onset of the pain, or which increase the likelihood of an individual developing persistent pain. These include biological factors (eg. weakness, stiffness), psychological factors (eg. depression, fear of movement and catastrophisation) and social factors (eg. work environment).[1]
Once serious spinal pathology and specific causes of back pain have been ruled out, an individual is classified as having non-specific low back pain. If no serious pathology is suspected, there is no indication for x-rays or MRI diagnostic imaging unless the results of imaging may change / guide the management protocol.[2][3]
90% of patients presenting to primary care with low back pain are classified as having non-specific low back pain.[4][5] Non-specific low back pain is defined as "low back pain not attributable to a recognizable, known specific pathology[6] (eg, infection, tumor, osteoporosis, lumbar spine fracture, structural deformity, inflammatory disorder, radicular syndrome, or cauda equina syndrome)."[7]
Non-specific low back pain is usually categorised into 3 subtypes: acute, sub-acute and chronic low back pain.[8] This subdivision is based on how long the individual has had low back pain. Acute low back pain is an episode of low back pain that has been present for less than 6 weeks, sub-acute low back pain has been present for between 6 and 12 weeks and chronic low back pain has been present for 12 weeks or more.[9]
Diagnosis versus Classification[edit | edit source]
Diagnosis is typically looked at as a pathoanatomical model, whereas the goal of classification systems is to guide treatment, so that clinicians don't treat all cases of back pain the same. If a patient does not have a clear diagnosis, they are referred to as having non-specific low back pain.
Imaging[edit | edit source]
For more information on referring for imaging, please see Practical Decision Making in Physiotherapy Practice, but to summarise:
- imaging is needed if red flags are present or if there is no improvement with conservative care within 6 weeks. If you are unsure about a red flag, you can often treat a little to see if they improve.
- imaging is recommended if it will change the course of treatment[10]
- a lot of imaging findings correlate with low back pain. This doesn’t mean everyone with imaging findings has pain, but often the more findings there are, the higher the chance the person has pain. We can still help these people though!
Differential Diagnosis[edit | edit source]
Initially, you should complete a comprehensive lumbar assessment. Once this is complete, you then triage the patient, as explained in the Lumbar Assessment page, by the image below:
You will need knowledge of Red Flags and conditions that can cause neurological deficits, such as those listed below (see linked pages for more information).
- Specific Low Back Pain
- Cauda Equina Syndrome
- Lumbar Radiculopathy
- Disc Herniation
- Spinal Stenosis
- Spondylolisthesis
- Piriformis Syndrome
- Sacroiliac Joint Pain (not dysfunction)
- Osteoarthritis
- Sciatica
- Thoraco-Lumbar Junction Syndrome
Physiotherapists have valuable assessment skills and clinical reasoning skills when an individual has an unclear presentation. A few key factors to consider when looking at a differential diagnosis:[11]
- Neurological testing isn't an exact diagnosis but it gives a very good indication of where the problem lies, how to treat the patient and what to avoid to prevent injury or flare up.[11]
- If you are considering an extremity as the source of lower back pain or symptoms, the likelihood of it being the extremity is far less if the extremity has a full, pain free range of motion when tested.[11]
- In a study by Rastogi Ravi, et al[12], it shows that current spinal pain raises the the pre-test probability of the extremity being from a spinal source from 10% to 19% overall.
- According to the table below, a high percentage of people reporting pain in their hip, thigh or leg have a spinal source of their pain.
| Regions | Extremity Source Frequency (%) | Spinal Source Frequency (%) | Total |
|---|---|---|---|
| Hip | 9 (29.0%) | 22 (71.0%) | 31 |
| Thigh/Leg | 5 (27.8%) | 12 (72.2%) | 18 |
| Knee | 58 (74.4%) | 20 (25.6%) | 78 |
| Ankle/Foot | 34 (70.8%) | 14 (29.2%) | 48 |
| Shoulder | 44 (52.4%) | 40 (47.6%) | 84 |
| Arm/Forearm | 2 (16.7%) | 10 (83.3%) | 12 |
| Elbow | 14 (56.0%) | 11 (44.0%) | 25 |
| Wrist/Hand | 16 (61.5%) | 10 (38.5%) | 26 |
| Total | 182 (56.5%) | 140 (43.5%) | 322 |
Pathoanatomical Approach Compared to a Signs and Symptoms Approach:[edit | edit source]
Pathoanatomical approach means that you are treating to improve anatomy while a signs and symptoms approach means you test signs and ask for symptoms, treat, and then retest to assess for progress.
After our assessment, we should consider the asterisk signs that we have made note of throughout our examination and use these to help decide how to treat using a "signs and symptoms" treatment approach.
An asterisk sign is also known as a comparable sign. It is something that you can reproduce/retest that often reflects the primary complaint. It can be functional or movement specific. It is used to measure if symptoms are improving or worsening.
Differentiating between Hip and Lumbar Pain:[edit | edit source]
In this video you can see a live patient examination differentiating between hip and lumbar pain:
| Syndrome | Findings | Assessment/Plan |
|---|---|---|
| Facet syndrome | History and physical examination:
Radiological findings (not indicated on intial evaluation):
|
Differential diagnosis:
Treatment:
|
| Sacro-iliac joint syndrome | History and physical examination:
Radiological findings (not indicated on intial evaluation): – Differential diagnosis:
|
Functional disturbance:
Treatment:
|
| Myofascial pain syndrome | History and physical examination:
Radiological and histological findings:
|
Local treatment:
|
| Functional instability | History and physical examination:
Radiological findings:
|
|
| Disease | Findings | Further Evaluation | Treatment |
|---|---|---|---|
Fracture
|
|
Imaging studies:
Laboratory testing:
|
Conservative:
Surgical:
Prevention:
|
| Massive disc herniation |
|
|
Surgical:
|
| Bacterial infection (spondylitis/ spondylodiscitis, epidural or paravertebral abscess) |
|
|
The indication for conservative vs. operative treatment (debridement, filling of defects, instrumentation) depends on:
|
| Tumor |
|
Imaging studies: local at first, then staging studies to rule out instability (SINS):
Laboratory tests:
|
Neurologic deficit present:
Neurologic deficit absent:
Conservative:
|
| Disease | Findings | Further Evaluation | Treatment |
|---|---|---|---|
| Disk herniation |
|
Imaging studies: (DD herniation vs. stenosis vs. tumor)
Neurological/electrophysiological testing:
|
Depending on the clinical findings:
|
| Spinal canal stenosis /
degenerative instability |
|
Abnormally flexed posture of trunk imaging studies:
Neurological/electrophysiological testing:
|
Depending on the clinical findings:
|
| Axial spondylitis and
seronegative spondylo - arthropathy |
Inflammatory back pain syndrome
|
Imaging studies:
|
|
Deformities
|
Clinical features:
|
Early detection in children!
|
Depending on the patient’s age and on the cause and severity of the deformity:
|
| Herpes zoster |
|
Lumbar puncture and CSF examination:
|
|
| Diabetic radiculopathy |
|
|
Pharmacotherapy:
|
| Neuroborreliosis |
|
Lumbar puncture and CSF examination:
|
|
| Spinal ischemia |
|
|
|
Key to abbreviations:
- CBC: complete blood count
- CRP: C-reactive protein
- CT: computerized tomography
- EMG: electromyography
- ESR: erythrocyte sedimentation rate
- MRI: magnetic resonance imaging
- SINS: spinal instability in neoplastic disease
- SSEP: somatosensory evoked potentials
- AB: antibodies
- CT: computerized tomography
- CSF: cerebrospinal fluid
- DD: differential diagnosis
- ENG: electroneurography
- EMG: electromyography
- MRI: magnetic resonance imaging
- NCS: nerve conduction study
- NSAID: nonsteroidal anti-inflammatory drug
- PDA: peridural anesthesia
- SSEP: somatosensory evoked potentials
- SSNRI: selective serotonin-norepinephrine reuptake inhibitor
- TCA: tricyclic antidepressant
Additional Resources[edit | edit source]
Physiopedia Pages:[edit | edit source]
- Low Back Pain
- Lumbar Assessment
- Low Back Pain Guidelines
- Differentiating Inflammatory and Mechanical Back Pain
- Non Specific Low Back Pain
- Specific Low Back Pain
Podcast Links:[edit | edit source]
- The Back Pain Podcast: Piriformis syndrome
- The Back Pain Podcast: Is my pain from my sacroiliac joint?
- Modern Pain Podcast: Lumbar Stenosis
- The Back Pain Podcast Episode 82: Flexion, Extension, Radicular Pain & Disc Pathology with Adam Meakins and Dr. Mark Laslett
Journal Articles and Books:[edit | edit source]
- Casser HR, Seddigh S, Rauschmann M. Acute lumbar back pain: investigation, differential diagnosis, and treatment. Deutsches Ärzteblatt International. 2016 Apr;113(13):223.
- Casiano VE, Dydyk AM, Varacallo M. Back pain.
References[edit | edit source]
- ↑ M.Hancock. Approach to low back pain. RACGP, 2014, 43(3):117-118.
- ↑ Hall AM, Aubrey-Bassler K, Thorne B, Maher CG. Do not routinely offer imaging for uncomplicated low back pain. bmj. 2021 Feb 12;372.
- ↑ Almeida M, Saragiotto B, Richards B, Maher C. Primary care management of non-specific low back pain: key messages from recent clinical guidelines. Med J Aust 2018; 208 (6): 272-275
- ↑ Traeger A, Buchbinder R, Harris I, Maher C. Diagnosis and management of low-back pain in primary care. CMAJ. 2017 Nov 13;189(45):E1386-E1395.
- ↑ Koes BW, Van Tulder M, Thomas S. Diagnosis and treatment of low back pain. Bmj. 2006 Jun 15;332(7555):1430-4.
- ↑ Otero-Ketterer E, Peñacoba-Puente C, Ferreira Pinheiro-Araujo C, Valera-Calero JA, Ortega-Santiago R. Biopsychosocial Factors for Chronicity in Individuals with Non-Specific Low Back Pain: An Umbrella Review. International Journal of Environmental Research and Public Health. 2022 Aug 16;19(16):10145.
- ↑ Balagué, Federico, et al. "Non-specific low back pain." The Lancet 379.9814 (2012): 482-491. Level of evidence 1A
- ↑ Hock M, Járomi M, Prémusz V, Szekeres ZJ, Ács P, Szilágyi B, Wang Z, Makai A. Disease-Specific Knowledge, Physical Activity, and Physical Functioning Examination among Patients with Chronic Non-Specific Low Back Pain. International Journal of Environmental Research and Public Health. 2022 Sep 23;19(19):12024.
- ↑ Burton AK, Tillotson KM, Main CJ, Hollis S. Psychosocial predictors of outcome in acute and subchronic low back trouble. Spine (Phila Pa 1976). 1995 Mar 15;20(6):722-8.Level of evidence 3C
- ↑ Al-Hihi E, Gibson C, Lee J, Mount RR, Irani N, McGowan C. Improving appropriate imaging for non-specific low back pain. BMJ Open Quality. 2022 Feb 1;11(1):e001539.
- ↑ 11.0 11.1 11.2 Rainey N. Differential Diagnosis Course. Physiopedia Plus. 2023.
- ↑ Rastogi R, Rosedale R, Kidd J, Lynch G, Supp G, Robbins SM. Exploring indicators of extremity pain of spinal source as identified by Mechanical Diagnosis and Therapy (MDT): a secondary analysis of a prospective cohort study. Journal of Manual & Manipulative Therapy. 2022 May 4;30(3):172-9.
- ↑ Rosedale R, Rastogi R, Kidd J, Lynch G, Supp G, Robbins SM. A study exploring the prevalence of Extremity Pain of Spinal Source (EXPOSS). Journal of Manual & Manipulative Therapy. 2020 Aug 7;28(4):222-30.
- ↑ 14.0 14.1 14.2 Casser HR, Seddigh S, Rauschmann M. Acute lumbar back pain: investigation, differential diagnosis, and treatment. Deutsches Ärzteblatt International. 2016 Apr;113(13):223.