Vaginismus: Difference between revisions
No edit summary |
No edit summary |
||
| Line 11: | Line 11: | ||
== Anatomy == | == Anatomy == | ||
[[File:1115 Muscles of the Pelvic Floor.jpg|right|frameless| | [[File:1115 Muscles of the Pelvic Floor.jpg|right|frameless|400x400px]] | ||
Muscles hypothesised to be involved:<ref name=":8">Shafik A, El-Sibai O. [https://www.sciencedirect.com/science/article/abs/pii/S030121150200115X Study of the pelvic floor muscles in vaginismus: a concept of pathogenesis]. European Journal of Obstetrics & Gynecology and Reproductive Biology. 2002 Oct 10;105(1):67-70.</ref> | Muscles hypothesised to be involved:<ref name=":8">Shafik A, El-Sibai O. [https://www.sciencedirect.com/science/article/abs/pii/S030121150200115X Study of the pelvic floor muscles in vaginismus: a concept of pathogenesis]. European Journal of Obstetrics & Gynecology and Reproductive Biology. 2002 Oct 10;105(1):67-70.</ref> | ||
| Line 53: | Line 53: | ||
== Pathophysiology/Mechanism == | == Pathophysiology/Mechanism == | ||
There is a theory that this condition is caused by disorder of the sacral reflex arc conducting the stimulus but further research is needed in this area.<ref name=":8" /> | |||
* '''Primary Vaginismus''' - It is present from the first attempt at penetration and occurs when the woman has never been able to have penetrative intercourse because of the involuntary contraction of her vaginal muscles.<ref name=":9">Jeng CJ, Wang LR, Chou CS, Shen J, Tzeng CR. [https://www.tandfonline.com/doi/abs/10.1080/00926230600835189 Management and outcome of primary vaginismus]. Journal of sex & marital therapy. 2006 Dec 1;32(5):379-87.</ref><ref name=":10">McGuire H, Hawton KK. [https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD001760/abstract Interventions for vaginismus]. Cochrane Database of Systematic Reviews. 2001(2).</ref>Often the etiology is of idiopathic origin. | * '''Primary Vaginismus''' - It is present from the first attempt at penetration and occurs when the woman has never been able to have penetrative intercourse because of the involuntary contraction of her vaginal muscles.<ref name=":9">Jeng CJ, Wang LR, Chou CS, Shen J, Tzeng CR. [https://www.tandfonline.com/doi/abs/10.1080/00926230600835189 Management and outcome of primary vaginismus]. Journal of sex & marital therapy. 2006 Dec 1;32(5):379-87.</ref><ref name=":10">McGuire H, Hawton KK. [https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD001760/abstract Interventions for vaginismus]. Cochrane Database of Systematic Reviews. 2001(2).</ref>Often the etiology is of idiopathic origin. | ||
| Line 68: | Line 67: | ||
!Features | !Features | ||
|- | |- | ||
|Total vaginismus | |Total vaginismus <ref name=":11"> | ||
|Unable to tolerate vaginal penetration | |Unable to tolerate vaginal penetration | ||
|- | |- | ||
| Line 75: | Line 74: | ||
|- | |- | ||
|Primary/Lifelong vaginismus | |Primary/Lifelong vaginismus | ||
| | |Present from the first attempt at penetration; has never had pain-free intercourse) | ||
|- | |- | ||
|Secondary Vaginismus | |Secondary Vaginismus | ||
|Vaginismus occurs after sexual intercourse has previously been normal/pain free | |Vaginismus occurs after sexual intercourse has previously been normal/pain-free | ||
|- | |- | ||
|Situational Vaginismus | |Situational Vaginismus | ||
| Line 123: | Line 122: | ||
In 1978 Lamont<ref name=":16" /> described the first four grades and a grade 5 was later added by Pacik<ref name=":3" /><ref name=":4" />. The Lamont grades were based on the patient's conduct during gynaecological examination and history taking whereas the Pacik grade 5 takes into account the severe fear and anxiety seen in the patient while performing the examination. | In 1978 Lamont<ref name=":16" /> described the first four grades and a grade 5 was later added by Pacik<ref name=":3" /><ref name=":4" />. The Lamont grades were based on the patient's conduct during gynaecological examination and history taking whereas the Pacik grade 5 takes into account the severe fear and anxiety seen in the patient while performing the examination. | ||
{| class="wikitable" | {| class="wikitable" | ||
|+ | |+ | ||
| Line 146: | Line 143: | ||
|Generalized retreat as in level 4 plus visceral reaction, which may result in any one or more of the following: palpitations, hyperventilation, sweating, severe trembling, uncontrollable shaking, screaming, hysteria, wanting to jump off the table, a feeling of becoming unconscious, nausea, vomiting, and even a desire to attack the doctor | |Generalized retreat as in level 4 plus visceral reaction, which may result in any one or more of the following: palpitations, hyperventilation, sweating, severe trembling, uncontrollable shaking, screaming, hysteria, wanting to jump off the table, a feeling of becoming unconscious, nausea, vomiting, and even a desire to attack the doctor | ||
|} | |} | ||
Checking the Degree of vaginal muscle hypertonus/spasm<ref name=":4" /> | Checking the Degree of vaginal muscle hypertonus/spasm<ref name=":4" /> | ||
Revision as of 21:29, 3 August 2022
Introduction[edit | edit source]
Vaginismus is a sexual pain disorder that is characterized by difficulties and pain with vaginal insertion (e.g. during sexual intercourse, or when using a tampon) as well as significant fear and anxiety associated with penetration.[1][2] [3] This results in the avoidance of sexual intercourse, vaginal exams and tampon use and causes significant distress and reduced quality of life for the individual experiencing it.[1][2][4][5][6]
It has traditionally been referred to as an involuntary contraction or hypertonic state of the pelvic floor muscles (PFMs) due to actual or anticipated pain associated with vaginal penetration, causing women to feel pain, fear and anxiety with penetration attempts.[1][7] However, there is a strong psychological component associated with its presentation and it has therefore been described as a psychosexual dysfunction.[2] Awareness of this psychological pain driver is paramount to the management of this condition.
According to DSM-V classification Vaginismus has been classified under "Genito-pelvic pain/Penetration disorder".[8]
The quality of evidence regarding vaginismus is low as there are very few Randomized Controlled trials (RCT) done. Therefore its etiology, pathology and treatments lacks good quality literature.
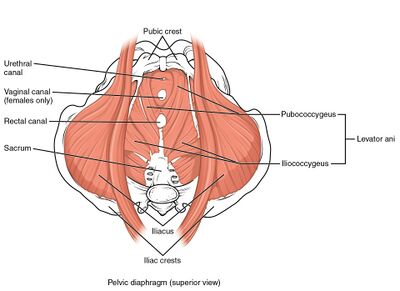
Anatomy[edit | edit source]
Muscles hypothesised to be involved:[9]
- Levator ani
- Puborectalis (with deep external anal sphincter)
- Bulbocavernosus muscle (with external anal sphincter)
Prevalence and Incidence[edit | edit source]
It is difficult to determine the prevalence of vaginismus due to the stigma and embarrassment experienced by people with sexual disorders which results in reduced help-seeking behavior in individuals with this condition.[3][10] Therefore, those studies that report a prevalence (e.g. 1-6% in the general population[11]) likely underestimate the true prevalence of the condition in the population.[3][10] Estimates of prevalence may be more accurate in more specialised settings e.g. 30% in primary care settings [12] and 42% in specialized clinics for female sexual disorders.[13][14]
Etiology[edit | edit source]
Several psychosocial and organic factors have been proposed to be associated with the development of vaginismus but further research is needed to support these associations. These factors are thought to contribute to the anxiety, fear, muscle hypertonicity/spasm and pain associated with vaginismus.
Organic Pathologies[2][15][edit | edit source]
- Hymen/congenital abnormalities
- Local infections
- Trauma associated with childbirth
- Genital injury/surgery or radiotherapy
- Vaginal lesions and tumours
- Vestibulodynia
- Vaginal atrophy
- Pelvic congestion
- Endometriosis
- Irritation of the vagina
Psychosocial Factors [2] [3] [16][edit | edit source]
- Psychological/physical/sexual trauma or abuse
- Strict sexual/religious upbringing
- Negative family messaging and personal views around sexuality
- Facing difficulties in relationship.
- Fear of first-time sex (pain, bleeding, tearing, ripping, penis too large, vagina too small, sexually transmitted diseases, fear of pregnancy)
- Fear of gynecological examinations
- A maternal influence involving grandmothers, mothers, twins, and sisters. The influence is due to merely hearing about the difficulties faced by them and the patient may manifest it as a subsequent fear of penetration.
Quality Of Life[edit | edit source]
This condition influences the quality of life. In the most serious form it can result in an unconsummated marriage, and sterility and thus further result in the couple leading a separate life.[7] It is correlated with poor sexual quality of life[6] and even the male partners may have important effects on the development, maintenance and exacerbation of vaginismus (in lifelong vaginismus (LLV)).[17] Common psychological symptoms seen are depression, anxiety, low self-esteem, insecure attachment styles, histrionic/hysterical traits and an inability to describe own emotions.[15]
Pathophysiology/Mechanism[edit | edit source]
There is a theory that this condition is caused by disorder of the sacral reflex arc conducting the stimulus but further research is needed in this area.[9]
- Primary Vaginismus - It is present from the first attempt at penetration and occurs when the woman has never been able to have penetrative intercourse because of the involuntary contraction of her vaginal muscles.[18][19]Often the etiology is of idiopathic origin.
- Secondary Vaginismus - It is seen following physical or psychological trauma, infection, menopausal changes, or other pelvic pathologies. The patient has previously been able to have coitus but now is no longer able to be penetrated, because of the involuntary muscle spasms. It may be situational and is often associated with dyspareunia.[18][19]
Classifications[edit | edit source]
| Classification | Features | |||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
Total vaginismus Cite error: Closing </ref> missing for <ref> tag
Assessment[edit | edit source]History[edit | edit source]A thorough medical and psycho-sexual history needs to be taken. The Female Sexual Function Index (FSFI) or alternatively Vaginal Penetration Cognition Questionnaire (VPCQ) can be used. Clarify the patient's history of penetration, pain rating and anxiety rating. Pain and anxiety can be scored by the patient for tampons, cotton-tipped applicators, fingers, gynaecological examinations, dilators, and intercourse. It is important to rule out other causes of sexual pain such as herpes virus or lichens sclerosis. Vulvodynia, vestibulodynia and dyspareunia should be considered as differential diagnoses.[16] It can be difficult to differentiate vaginismus from dyspareunia. However, the level of fear, distress, avoidance of sexual intercourse and muscle tension is much higher in those with vaginismus.[2] [3] The following topics are important to include in the subjective history:[1]
Examination[edit | edit source]If the patient is willing and comfortable to move forward with an internal pelvic exam, the clinician should assess the level of muscle tone and trigger points within the pelvic floor musculature as well as the general functioning of these muscles. The Lamont grading system can be utilized to diagnose the severity of vaginismus .[4] [5] [16] [22] This scale is based on the patient's response to the internal pelvic exam (The Lamont Scale - What Is It?, 2016; Figure 1. The Lamont Scale. Descriptions of Lamont Grades 1À4., n.d.).[4][5][16][22] In 1978 Lamont[23] described the first four grades and a grade 5 was later added by Pacik[16][24]. The Lamont grades were based on the patient's conduct during gynaecological examination and history taking whereas the Pacik grade 5 takes into account the severe fear and anxiety seen in the patient while performing the examination.
Checking the Degree of vaginal muscle hypertonus/spasm[24]
Diagnosis[edit | edit source]Diagnosis is based on the history and symptoms of the patient. Documenting the amount of pain and anxiety with various forms of vaginal penetration is helpful in understanding a patient's perception of penetration pain. The diagnosis of vaginismus is made by a history of severe pain during intercourse or intercourse being impossible which feels like "hitting a brick wall" or "there is no hole down there" is indicative of vaginal spasm of the opening of the vagina and is often diagnostic of severe vaginismus, which is an important differentiation from dyspareunia, vulvodynia and vestibulodynia.[16] This history and the inability to tolerate gynaecological examinations are two important diagnostic features of severe vaginismus.[16] Patients with vaginismus may have an aversion to pelvic touch related to the fear of pain and behavioural avoidance and may not permit pelvic examination, cotton-tipped testing, and EMG evaluation.[16] Patients who score themselves as "10's" (severe pain and severe anxiety) with all forms of penetration have much more difficulty incorporating the suggestion of therapy.[16] Differential Diagnosis[edit | edit source]As per evidence, the unwillingness or inability to experience/attempt vaginal penetration has been recommended to differentiate vaginismus from dyspareunia and provoked vestibulodynia.[25] Extreme fear and anxiety towards penetration of any object in the vagina is a crucial diagnostic factor. The conditions which can be differentially diagnosed from vaginismus are;
Prognosis[edit | edit source]Patients who are able to tolerate some forms of penetration and who have lower pain and anxiety scores tend to be easier to treat in that they are able to cooperate with the proposed treatment. Hence their prognosis is also better when compared to other higher grades of vaginismus. Management[edit | edit source]The management of vaginismus needs to be multimodal to address the physical, emotional and psychological contributors to its presentation and should ideally include a multidisciplinary team consisting of a gynaecologist, physiotherapist and a psychologist/sex therapist.[20] Non-Surgical Management[edit | edit source]Therapy/Counseling[edit | edit source]Psychotherapy for vaginismus aims to address the anxiety, depression, fear avoidance and relational stressors associated with the conditions.[16]Options include;[2][16]
The therapy can be conducted in an individual or couple format. In individual therapy, the treatment is to identify and resolve underlying psychological problems that could be causing the disorder. In couples therapy, the disorder is designed as a problem for the couple and the treatment inclines to aim at the couple’s sexual history and any other problems that may be occurring in the relationship. Cognitive Behavioural Therapy[edit | edit source]There are two methods used for CBT;
Pharmacological Therapy[edit | edit source]There are three main types of pharmacological treatment for vaginismus;
Pelvic Physiotherapy[edit | edit source]A pelvic floor physiotherapist can help to restore function by treating altered PFM tone, improving PFM functioning, and reducing the pain and anxiety associated with penetration.[2]
The use of interferential current for the treatment of vaginismus is still under trial.[30] Surgical Management[edit | edit source]Removal of hymenal remnants-Hymenectomy.[16] Combination Treatment of Sacral Erector Spinae Plane Block and Progressive Dilatation is under trial.[31] References[edit | edit source]
|