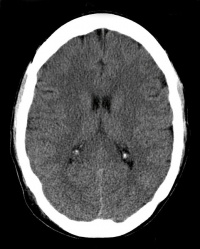
Watershed Stroke/Infarction
Original Editor - Your name will be added here if you created the original content for this page.
Lead Editors
Introduction[edit | edit source]
Watershed cerebral infarctions (WI), also known as border zone infarcts, occur at the border between cerebral vascular territories where the tissue is furthest from arterial supply and thus most vulnerable to reductions in perfusion.[1]
These strokes may often be preceded by specifically precipitating circumstances that induce hypotension and/or hypovolemia (rising from a supine position, exercise, Valsalva's maneuver, administration of antihypertensive drugs, bleeding and anemia)[2].
Epidemiology[edit | edit source]
WI are a frequent clinical entity and are often under-recognised due to slow progression of the presenting symptoms and to the frequent association to seizures.[3]
- Account for 5-10% of all cerebral infarctions
- Tend to occur in the elderly, who have a higher incidence of arterial stenosis and hypotensive episodes, as well as microemboli.[1]
This 10 minute video outlines WI
Mechanism of Injury / Pathological Process[edit | edit source]
It has been proposed that both episodes of hypoperfusion and microemboli from inflamed atherosclerotic plaques play a role in pathophysiology of WI. If low blood flow to watershed areas lasts for longer than a few minutes, the tissues in the watershed areas begin to die, causing a stroke due to low blood volume.
- A typical scenario involves episodes of systemic hypotension, particularly with severe stenosis or occlusion of the feeding arteries (particularly the intracranial and extracranial carotid arteries).
- Clearance of the microemboli (which may form on the surface of inflamed plaques) most likely impair watershed zones due to reduced perfusion.
- A watershed zone infarct in an isolated area is more likely to be secondary to microembolism, particularly in the absence of significant systemic hypotension and/or arterial stenosis. eg In a severe carotid stenosis, lesions are usually ipsilateral to the stenosis.
- Prolonged hypotension, such as during cardiac surgery or cardiac arrest, commonly gives a bilateral pattern in the absence of severe stenosis.
WI are classified thus:
- Cortical (external) border zones infarct
- between ACA, MCA, and PCA territories
- histologically, these can be wedges of cortical and subcortical infarction or cortical laminar necrosis
- Deep (internal) border zones infarct:
- between ACA, MCA, and PCA territories and perforating medullary, lenticulostriate, recurrent artery of Heubner and anterior choroidal arteries[1]
Causes[edit | edit source]
Low Fluid Volume/ Low Blood Pressure. Because the watershed areas are the farthest regions supplied by arterial supply systems, adequate blood flow and blood pressure must be maintained to ensure that enough blood is pumped into these areas. Watershed areas are at high risk during extreme drops of blood pressure.
Common triggers for WI [5]
- Heart attacks, which affect the pumping ability of the heart, potentially cause significantly diminished blood flow to the brain. vulnerable to low blood advanced carotid stenosis,
- Conditions that can cause sudden or severely low blood pressure eg severe dehydration, which results in an overall low volume of fluid in the whole body.
- Severe infections, such as sepsis, an infection that has spread throughout the bloodstream, may cause the blood pressure to drop dramatically
- Profuse bleeding, which may result from major injury and trauma, can cause such a significant amount of blood loss that the brain does not receive enough blood supply to the watershed regions.
Clinical Presentation[edit | edit source]
The symptoms of a watershed stroke are varied include but not limited to [5]
Weakness or paralysis, especially of the legs.
Mood disturbances.
Vision loss in half of their field of vision.
Cause seizures more often than do other types of stroke.
Diagnostic Procedures[edit | edit source]
A watershed stroke can often be diagnosed through a neurological history and physical examination and can often be identified on a brain CT or a brain MRI.
Treatment, Physiotherapy and more see stroke[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Radiopedia Watershed Infarctionhttps://radiopaedia.org/articles/watershed-cerebral-infarction (last accessed 29.12.2019)
- ↑ D'Amore C, Paciaroni M. Border-zone and watershed infarctions. InManifestations of Stroke 2012 (Vol. 30, pp. 181-184). Karger Publishers. Available from:https://www.karger.com/Article/Abstract/333638 (last accessed 29.12.2019)
- ↑ Juergenson I, Mazzucco S, Tinazzi M. A typical example of cerebral watershed infarct. Clinics and practice. 2011 Sep 28;1(4). Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3981431/ (last accessed 29.12.2019)
- ↑ Audiopedia WI Available from:https://www.youtube.com/watch?v=7o_nsFZJIXM (last accessed 29.12.2019)
- ↑ 5.0 5.1 Watershed Stroke Symptoms, Causes, and Treatment dec 2019 Verywell Available from: https://www.verywellhealth.com/what-is-a-watershed-stroke-3146040 (last accessed 29.12.2019)