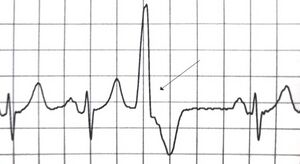
Ventricular Extrasystole
Original Editor - Elyssa Abou Jamra
Top Contributors - Elyssa Abou Jamra, Kim Jackson and Lucinda hampton
Introduction[edit | edit source]
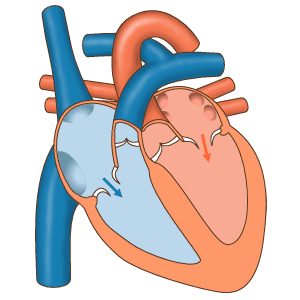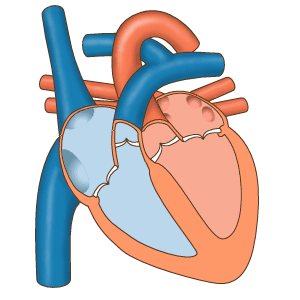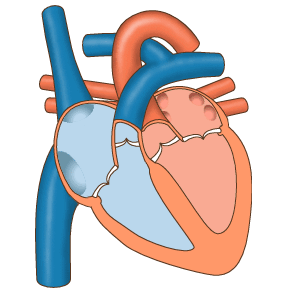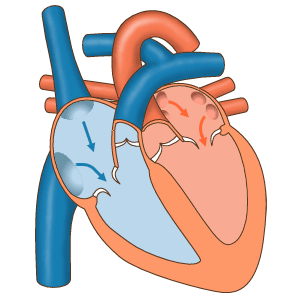
Premature ventricular contractions (PVCs) are early depolarizations of the myocardium originating in the ventricule. During a premature ventricular contraction (PVC), the heartbeat is initiated by the Purkinje fibers rather than the SA node. [1] [2]
- In the vast majority of cases, PVCs have no known cause and occur spontaneously. [1]
- The most common forms of premature ectopic ventricular impulse formation are ventricular extrasystoles and ventricular tachycardia. [3]The manifestation of the ectopic rhythm may be an expression of underlying disease. [4]
- Overall, the presence of PVCs in young people is a benign finding but in older patients with underlying heart disease, there is a risk of ventricular arrhythmias and cardiac arrest.[1]
Epidemiology[edit | edit source]
PVCs are common among the general population.
- The estimated prevalence ranges from 1% to 4% on electrocardiogram and 40% to 75% on a 24 or 48-hour Holter monitor.
- Young and healthy adults have shown a highly similar frequency rate of PVCs in contrast to the older segments of the general population[1].
Etiology[edit | edit source]
Common known etiologies include:
- Excess caffeine consumption, excess catecholamines (released in response to emotional or physical stress),[5] high levels of anxiety, and electrolyte abnormalities.
- Specific electrolyte:
- low blood potassium
- low blood magnesium
- high blood calcium.
- Alcohol, tobacco, and illicit drugs
- Patients suffering from sleep deprivation
- There are numerous cardiac and non-cardiac pathologies that are causative,examples:
- Any structural heart disease that alters conduction pathways due to tissue alterations
- Non-cardiac examples :
Patient populations with higher risks of cardiovascular disease and clinically poor cardiovascular markers have a higher occurrence of PVCs.[6]
Pathophysiology[edit | edit source]
There are three mechanisms for the development of the disease: disruption of automatism, trigger activity, circular passage of the excitation wave (re-entry).[7]
Assessment[edit | edit source]
History:
- Detailed history of the presenting symptom - including onset, duration, associated symptoms and recovery.
- Check for other cardiac symptoms including chest pain, breathlessness, syncope or near syncope (eg, dizziness), and arrhythmia symptoms (eg, sustained fast palpitations).
- If there is history of syncope, note that:
- Exertional syncope should always raise alarm of a sinister cause.
- Rapid recovery after the syncopal event, without confusion or drowsiness, is characteristic of cardiac syncope.
- Family history - for early cardiac disease or sudden death.
- Previous cardiac disease or coronary heart disease (CHD) risk factors.
Symptoms[edit | edit source]
In most cases there are no complaints. To a lesser extent, the following symptoms arise:
- uneven heartbeat;
- weakness and dizziness;
- lack of air;
- pain in the chest is located in an atypical location;
- the ripple can be very pronounced, so it is felt by the patient[7].[8]
Diagnosis
It starts with listening to the complaints of the patient, an objective examination, listening to the activities of the heart. Next an instrumental study. The main diagnostic method is electrocardiography.
ECG signs of ventricular extrasystole:
- prematurely appears QRS complex;
- in its form and magnitude the extraordinary complex QRS differs from other, normal;
- In front of the QRS complex, formed by the extrasystole, there is no tooth P;
- after an incorrect QRS complex, an compensatory pause is always observed - an elongated insulin segment located between extraordinary and normal abbreviations.
Holter monitoring of ECG - is often prescribed to patients with severe left ventricular failure or with an unstable occurrence.
Electrophysiological study, two groups of patients. First: no structural changes in the heart, but correction of medical treatment is necessary. Second: organic disorders are present, to assess the risk of sudden death, conduct diagnosis.
Signal-averaged ECG is a new method that is promising in terms of identifying patients with a high probability of occurrence of severe forms of HPI. It also helps in determining the unstable tachycardia of the ventricles[7].
Treatment[edit | edit source]
- Patients who experience asymptomatic PVCs rarely require any treatment (especially true for isolated PVCs). In the emergency room, hypoxic patients need to be provided with oxygen, the electrolyte imbalance should be corrected and drug toxicity should be ruled out. At the same time, an acute MI must be ruled out.
- Those experiencing frequent PVCs or symptomatic PVCs should be evaluated to identify the etiology. In many cases, excess intake of stimulants and/or lower levels of potassium and magnesium is the cause of the PVCs. These patients can be easily managed via minimization of stimulants and/or repletion of electrolytes. The medication classes used to treat frequent and/or symptomatic PVCs include antiarrhythmics, beta-blockers, and calcium channel blockers. Commonly used antiarrhythmics include amiodarone and flecainide.
- Some patients who have very frequent PVCs (e.g., several thousand per day) or symptomatic PVCs refractory to pharmacologic treatment, may be candidates for radiofrequency catheter ablation. [1]
Summary[edit | edit source]
- Ventricular ectopic beats (PVCs) are frequently seen in daily clinical practice and are usually benign.
- Presence of heart disease should be sought and, if absent, indicates good prognosis in patients with PVCs.
- Unifocal PVCs arising from the right ventricular outflow tract are common and may increase with exercise and cause non-sustained or sustained ventricular tachycardia. Catheter ablation is effective and safe treatment for these patients.
- B-blockers may be used for symptom control in patients where PVCs arise from multiple sites. It should also be considered in patients with impaired ventricular systolic function and/or heart failure.
- Risk of sudden cardiac death from malignant ventricular arrhythmia should be considered in patients with heart disease who have frequent PVCs. An implantable cardioverter defibrillator may be indicated if risk stratification criteria are met.
- PVCs have also been shown to trigger malignant ventricular arrhythmias in certain patients with idiopathic ventricular fibrillation and other syndromes. Catheter ablation may be considered in some patients as adjunctive treatment.[10]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Farzam K, Richards JR. Premature Ventricular Contraction. StatPearls [Internet]. 2021 Aug 12. Available: https://www.ncbi.nlm.nih.gov/books/NBK532991/(accessed 28.2.2022)
- ↑ Ahn MS. Current Concepts of Premature Ventricular Contractions. J Lifestyle Med. 2013;3(1):26-33.
- ↑ Leo Schamroth (1980). Ventricular extrasystoles, ventricular tachycardia, and ventricular fibrillation: Clinical-electrocardiographic considerations. , 23(1), 13–32. doi:10.1016/0033-0620(80)90003-1
- ↑ Scherf D, Schott A: Extrasystoles and Allied Arrhythmias. London, William Heinemann, 1953
- ↑ Frigy, Attila; Csiki, Endre; Caraşca, Cosmin; Szabó, István Adorján; Moga, Victor-Dan (2018). Autonomic influences related to frequent ventricular premature beats in patients without structural heart disease. Medicine, 97(28), e11489–. doi:10.1097/MD.0000000000011489
- ↑ Ribeiro WN, Yamada AT, Grupi CJ, da Silva GT, Mansur AJ. Premature atrial and ventricular complexes in outpatients referred from a primary care facility. PLoS One. 2018;13(9):e0204246.
- ↑ 7.0 7.1 7.2 Arrhymia centre Ventricular extrasystoleshttps://arrhythmia.center/en/zheludochkovaya-ekstrasistoliya/ (accessed 28.2.2022)
- ↑ Gorenek, Bulent; Fisher, John D.; Kudaiberdieva, Gulmira; Baranchuk, Adrian; Burri, Haran; Campbell, Kristen Bova; Chung, Mina K.; Enriquez, Andrés; Heidbuchel, Hein; Kutyifa, Valentina; Krishnan, Kousik; Leclercq, Christophe; Ozcan, Emin Evren; Patton, Kristen K.; Shen, Win; Tisdale, James E.; Turagam, Mohit K.; Lakkireddy, Dhanunjaya (2019). Premature ventricular complexes: diagnostic and therapeutic considerations in clinical practice. Journal of Interventional Cardiac Electrophysiology, (), –. doi:10.1007/s10840-019-00655-3
- ↑ Alila Medical Media. Premature Ventricular Contractions (PVCs), Animation . Available from: https://www.youtube.com/watch?v=wBs4fowZmzs [last accessed 22/11/2021]
- ↑ Ng, G A. (2006). Treating patients with ventricular ectopic beats. Heart, 92(11), 1707–1712. doi:10.1136/hrt.2005.067843