Varicose Veins
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton and Kim Jackson
Introduction[edit | edit source]
Varicose veins, usually referred to as Chronic venous insufficiency (CVI), is a common medical condition with major socioeconomic impact.
- Typically refers to lower extremity edema, skin trophic changes, and discomfort secondary to venous hypertension.
- Prevalent disease process.
- Disability-related to chronic venous insufficiency attributes to diminished quality of life and loss of work productivity.
- Its pathology is based on venous hypertension on the lower extremities (usually the cause is incompetent valves).
- Left untreated it is usually progressive and leads to the post-phlebitic syndrome and venous ulcers[1].
- Prevalence in adult population is estimated to be 5–30%.
- The severity of chronic venous disease is closely related to the magnitude of venous hypertension.
- Treatment options for CVI include medical, interventional, surgical and physical treatments.[2]
- Compression stockings have poor compliance.
- Many patients elect to undergo surgery and the outcomes do vary.[2]
Etiology[edit | edit source]
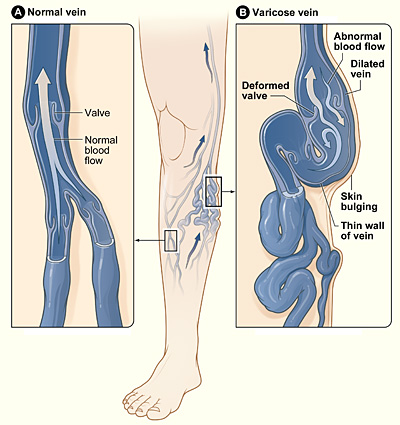
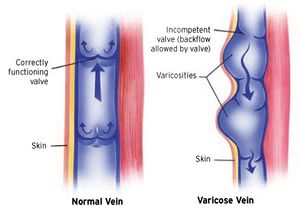
CVI originates from the failure of the venous valves in the saphenous veins, which results in retrograde flow and stasis, or pooling, of venous blood in the branches of the saphenous veins. The normal ambulatory venous pressure in the extremity is regulated by the function of the valves.
- If the valves no longer function this can translate into elevated ambulatory venous pressure and can produce symptoms.
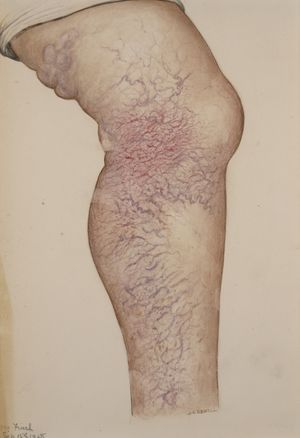
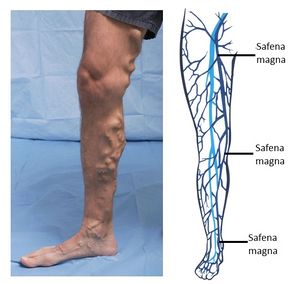
- The associated symptoms, including dilated visible veins at the skin surface (varicose veins, reticular veins, and telangiectasias), swelling, aching, heaviness, skin discoloration, and potential ulcer formation. A poor calf pump mechanism may worsen venous reflux.
Risk Factors: Family history; Female sex; Increased age; Multiple pregnancies; Standing for long periods; Obesity; History of DVT[3]
Epidemiology[edit | edit source]
- Early stages of venous reflux may occur in as many as 25% of women and 15% of men.
- Later stages of venous reflux, such as venous ulceration, may occur in 5% of the population (Rabe 2016).
- Varicose veins are seen globally and influenced by activity and lifestyle.
- Overall, varicose veins are more common in women than men[3].
Symptoms[edit | edit source]
Symptoms and signs of CVI include hyperpigmentation, stasis dermatitis, pain, cramping, chronic edema and venous ulcers.
- Edema begins in the perimalleolar region and ascends up the leg.
- Sense of discomfort in legs is often referred to as weight or pain after standing for a long time and it is relieved by leg elevation.
- Cutaneous changes include skin hyperpigmentation with hemosiderin deposition and eczematous dermatitis.
- This fibrotic process produces lipodermatosclerosis and there are risks of cellulite, leg ulcers and delayed wound healing.
- In addition, chronic venous insufficiency contributes to the development of lymphedema[2]
Treatment[edit | edit source]
There are many treatment options such as medical, pharmacological and conservative methods used in CVI.
Conservative Treatments (see physiotherapy)
Surgical Treatment
- Traditional surgical treatment consisted of ligation and stripping of the greater saphenous vein with avulsion of tributary veins.
Endovascular Treatment
- In the United States, surgical vein ligation and stripping has largely been replaced by catheter-based endovenous thermal ablation (EVTL). EVTL is performed with either laser or radiofrequency as the source of the heat energy. The EVTL procedure is typically performed under ultrasound guidance and with a local anesthetic.
Supplemental Procedures
- In addition to treating the venous reflux within the saphenous veins, many patients will also have visible superficial veins including reticular veins, "spider veins" in lay terminology. In addition to being unsightly, may also be painful to local pressure. Liquid sclerotherapy involves the injection of a dilute medication (sclerosant) into the superficial telangiectasias and reticular veins. Phlebectomy involves the removal of larger superficial varicose veins through small 2 mm to 3 mm incisions. Laser therapy is only used to treat the spider veins and is not useful for varicose veins.[3]
Physiotherapy[edit | edit source]
The most important step includes patient education to obtain better outcomes after treatment. Training the patient about the changes in lifestyle is important. The control of weight, care of the limbs and optimum exercises to keep the calf muscles and ankle joint supple are among the strategies.
Treatment includes:
Compression stocking (CS):
- Relies on the use of compression therapy, which is considered the “gold standard,” provided by means of elastic stockings, bandages and pneumatic compression devices. Patient education is essential. CVI is a chronic disease that needs a life-long care. So patients with CVI should encourage to maintain a normal body weight, exercise daily (a walking program is especially good) and wear compression garment throughout the day[2]
- Most patients obtain adequate symptom relief by using long-term graduated compression stockings, and through leg elevation and oral pain medications. For compression rates the recommended graduation is 20-30 mmHg and in more severe cases can be elevated to 30-40 mmHg. Stockings when worn daily are the ideal treatment for patients who do not want surgery. They do work but the heat and hot weather can reduce compliance[3].
Structured exercise program
- CVI causes ankle immobility due to storage of fibrotic tissue. Because of immobility, the calf muscle pump cannot be activated and venous blood does not return to the heart. Presence of any abnormality in pump functions of calf muscle plays a significant role in the development of CVI. In patients with CVI, progressive exercise program have been used to rehabilitate the muscle pump function and improve symptoms
- A normal walking motion is required for activation of the calf muscular pump. It has been found that exercise program twice a week increased the angle of dorsiflexion and plantar flexion in those with CVI[2]
Complete Decongestive Therapy (CDT)
Intermittent pneumatic compression (IPC)[2]
- Skin-taping increases the circulation in the region by creating convulsions that cause the dermis to rise up. Kinesio Tape (frequently used in edema, hematoma and wound healing) has been used as an alternative to compression therapy in patients with venous insufficiency in recent years. Kinesio Tape has not been proven to have a positive effect on venous insufficiency.[2]
References[edit | edit source]
- ↑ Patel SK, Surowiec SM. Venous insufficiency.Available from:https://www.ncbi.nlm.nih.gov/books/NBK430975/ (last accessed 24.10.2020)
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Özdemir ÖÇ, Surmeli M. Conservative management of chronic venous insufficiency. Clinical physical therapy. 2017 May 31.Available from:https://www.intechopen.com/books/clinical-physical-therapy/conservative-management-of-chronic-venous-insufficiency (last accessed 25.10.2020)
- ↑ 3.0 3.1 3.2 3.3 Antani MR, Dattilo JB. Varicose Veins. InStatPearls [Internet] 2019 Nov 28. StatPearls Publishing.Available from:https://www.ncbi.nlm.nih.gov/books/NBK470194/ (last accessed 25.10.2020)