Syndesmotic Ankle Sprains
Original Editors - Rick Wetherald, Hannah Duncan, Hilary Zachary and James Passmore as part of the Texas State University Evidence-based Practice Project
Top Contributors - James Passmore, Hilary Zachary, Rick Wetherald, Hannah Duncan, Kim Jackson, Kai A. Sigel, Admin, Rachael Lowe, Patrick Bales, Laure Leyers, Simisola Ajeyalemi, 127.0.0.1, Khloud Shreif, Tarina van der Stockt, WikiSysop, Rucha Gadgil, Wanda van Niekerk, Evan Thomas and Naomi O'ReillyDefinition/Description[edit | edit source]
A syndesmotic, or ‘high’ ankle sprain is one that involves the ligaments binding the distal tibia and fibula at the Distal Tibiofibular Syndesmosis. Injuries can occur with any ankle motion, but the most common motions are extreme external rotation or dorsiflexion of the Talus. The dome of the Talus is wider in the anterior than in the posterior, and these movements force apart the medial and lateral aspects of the mortise, respectively the tibial and fibular malleoli. Sufficient distraction of the distal fibula from the tibia can cause strain or rupture of one or more of the following ligaments: the anterior inferior tibiofibular ligament, superficial posterior inferior tibiofibular ligament, transverse tibiofibular ligament, interosseous membrane, interosseous ligament and inferior transverse ligament.[1] Rupture injuries also commonly present with concomitant fractures of either malleolus (lateral being more common) or proximal fibular spiral fracture known as a Maissonneuve fracture. [2]
Epidemiology/Etiology[edit | edit source]
Syndesmotic ankle sprains commonly occur to athletes participating in American football and downhill skiing. Football injuries are usually a result of forced external rotation of the foot while the athlete is prone, as in at the bottom of the pile. The injuries can also result from a blow to the lateral knee while the foot is planted and dorsiflexed, resulting in an eversion or external rotation moment at the talocrural joint.
In downhill ski racing, the boot does not allow dorsi- or plantar-flexion movement, which can result in excessive allowance of talocrural external rotation and injury to the anterior or posterior tibiofibular ligament, as well as the interosseous membrane.
Research has documented that syndesmosis injuries account for 1-11% of all injuries [1]. Incidence among professional American football players is reported to be much higher, up to 29% as documented by Boytim et al ([3])
Characteristics/Clinical Presentation[edit | edit source]
Observationally the Syndesmotic will show significantly less swelling than a lateral ankle sprain, as well as demonstrate a loss of full plantar flexion and an inability to bear weight[2]. Ecchymosis may appear several days post-injury due to the injury of the intereosseuos membrane. A difficulty or inability to toe walk are often noted. History includes chronic pain, prolonged recovery, recurrent sprains, and the formation of heterotopic ossification within the interosseous membrane. [4]The most common MOI is when the foot is in external rotation with excessive dorsiflexion[5].
Differential Diagnosis[edit | edit source]
Because of the occult nature of the high ankle sprain during clinical evaluation it is important to rule out pathologies with a similar mechanism of injury (MOI). First and foremost fractures of the tibia, fibula and/or the talus should be ruled out [6]. Secondly, the clinician should address concerns of a lateral ankle sprain as the mechanism of injury between the two injuries are very similar. Norwig writes “Syndesmotic ankle sprains can usually be distinguished from inversion ankle sprains by a history of an external rotation component.” Other possible pathologies are medial ankle sprain, compartment syndrome, severe joint laxity[2], severe contusion, dystrophic calcification, infection, or tumor. These pathologies should be preferentially ruled out before tx of a syndesmotic ankle sprain begins.
Outcome Measures[edit | edit source]
Examination[edit | edit source]
Hx and MOI: see clinical presentation
- Observation/Gait analysis: Check for discrepancies
- Palpation:
- tenderness proximally over the anterior tibiofibular ligament and proximal along the interosseous membrane [7]
- Palpate the medial and lateral malleoli for existence of a fracture [8]
- Fibula needs to be palpated from distal to proximal, including the proximal tibiofibular joint to rule out Maissoneuve’s fracture . [2]
- Distal Pulses: Ensure pedal pulses are present [8]
- Girth Measurements: Notable swelling of ankle: do Figure 8 girth measurements
Special Testing[edit | edit source]
1. Dorsiflexion External Rotation Stress Test (Kleiger's Test)
- Determines rotator damage to the deltoid ligament or the distal tibiofibular syndesmosis.
- Performed by having the knee flexed by 90 degrees with the ankle in neutral position and appyling an external rotational force to the affected foot and ankle. [6]
- (+) test: Pain in the anterolateral ankle. An indicator of deltoid ligament damage would be if there is a displacement of the talus away from the medial malleolus.
- Interrater kappa= 0.75 (best)- [9]; [2]
2. Squeeze Test
- separation of the tibia and fibula [10]
- Identifies a fibular fracture or syndesmosis sprain.
- Performed by squeezing the tibia and fibula together above the injury.
- (+) test: Pain will be reproduced along the fibular shaft if it’s a fibular fracture and the distal tibiofibular jt for syndesmosis sprain.
- interrater= 0.5 (moderate). [9]
3. Cotton Test
- Assess for syndesmosis instability with diastasis.
- Performed: steadying the distal leg with one hand while grasping the plantar heel with the opposite hand and moving the heel directly from side to side [2]
- (+) test: Any lateral translation would indicate syndesmotic instability [11]
4. Fibular Traslation Test
- Beumer et al. (2011): 77% Sensitivity, 88% Specificity
Medical Management[edit | edit source]
Imaging is still considered the diagnostic standard and should be sought as quickly as possible to rule out any expected fractures and to aid in restoring normal anatomy. A one millimeter lateral displacement of the fibula results in a reduction in the available area of tibiotalar contact in weight bearing by 42%[12] One can easily see how such a “minor” yet misdiagnosed injury can lead to a lifetime of chronic sprains. Plain films are the bare minimum suggested, but due to the complexity of the structures and tissues, a CT scan is recommended for bony detail, MRIs give an accurate picture of the ligamentous injury, and they are the imaging gold standard for this injury. They are surpassed in accuracy only by arthroscopy. [2] Images should be done in a bilateral fashion to better determine an injury from a natural joint gap or overlap. Syndesmotic ankle sprains without diastasis are considered to be stable and are treated symptomatically. These patients are told to weightbear as tolerated. Those patients who exhibit a sprain with latent diastasis, where the reduction of the tibiofibular joint can be documented with CT or MRI, do not necessarily need surgery. Patients with these findings are often treated with immobilization in a non-weightbearing cast or walking boot for 4 to 6 weeks. Patients with a high syndesmotic ankle sprain that demonstrate diastasis of the syndesmosis without a fibular fracture require surgery. Surgical stabilization should be performed immediately. Surgical repair that includes open repair of torn ligaments and closed treatment of the ligaments with open or percutaneous insertion of a transverse syndesmosis screw has been shown to have favorable results.[2]
Physical Therapy Management[edit | edit source]
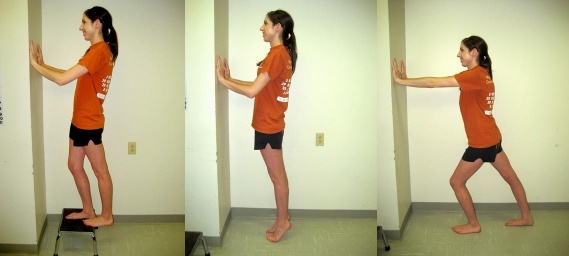
1.) Calf Stretch with Step 2.) Calf Strengthening Exercise 3.) Lunging Calf Stretch
Goals:
- First two weeks: ROM, decrease pain and swelling, protect ligaments against further injury
- Week 3 and onward: Restore normal ROM, strengthen ligaments and supporting muscles, training to improve endurance and balance [13](Level of evidence 5)
- Most important long-term goal is to prevent re-injury! [14](Level of evidence 1A)
Patient Education:
- Surgeon/PT’s recommended weightbearing protocol
- Caution against vigorous physical activity until full weight bearing and dynamic balance has normalized. [8](Level of evidence 3A)
- Gait training with crutches or boot/brace [2](Level of evidence 1A)
- Fall risk [8]
Assistive Devices:
- Crutches- must be maintained until normal, pain free gait is obtained [7]
- Walking boot or stirrup brace for unstable injuries [2]
Modalities:
- RICE (rest, ice, compression, elevation) initially for 15 min 3x a day.[13](. However, Bleakley et al suggested that there is little evidence to support the use of RICE, although it is a widely accepted treatment
- Non-steroidal anti-inflammatory drugs and comfrey ointment have been shown to improve short-term recovery following acute ankle sprain. [15]
Therapeutic Exercise/ Neuromuscular Re-education:
- First two weeks: AROM flexion, ankle alphabet, dorsiflexion/plantarflexion and inversion/eversion with theraband
- Weeks 3-4: Standing Stretch, seated dorsiflexion stretch with theraband, double heel raise progressing to single heel raise, and dorsiflexion stretching on step stool [13]
- Progressive weightbearing and treadmill gait training to promote normal gait pattern. [7][8]
- Neuromuscular Re-education: ankle proprioception, postural reflexes and balance
Ex: Single-leg stance, disk or balance pad training, aquatic therapy
- Progress to jogging, cycling, agility, jumping, and sport-specific drills. [8](Level of evidence 3A)
- Modify exercises to avoid hyperdorsiflexion (stresses mortise joint), subtalar eversion, and loaded external rotation. [7]
Manual Therapy:
- Passive accessory movement of the talocrural and subtalar joints and passive stretching may help stiffness. [8](Level of evidence 3A)
- Green et al: those subjects who used RICE with manual therapy were more likely to reach this normal ROM within the first 2 weeks of the ankle sprain than those who received RICE alone. [16]
- Collins et al: Subjects showed immediate ROM gains when Mulligan’s movement with mobilization was applied in the sub-acute sprains and in patients with recurrent sprains. [17]
- Landrum et al: Reported that one 30-second A-P talocrural joint mob immediately increased ankle dorsiflexion ROM after prolonged mobilization. [18]
**The recovery for Syndesmotic Ankle Sprain is often twice that of a typical ankle sprain!**
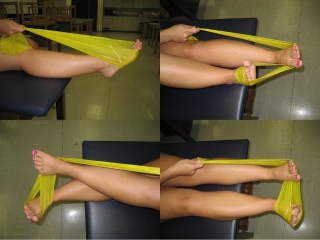
1.) Theraband Plantarflexion 2.) Theraband Dorsiflexion
3.) Theraband Inversion 4.) Theraband Eversion
Clinical Bottom Line[edit | edit source]
Syndesmotic ankle sprains, while less common than other ankle pathology, are an important consideration during the evaluation of leg pain. This injury is more common in athletes after forced external rotation and dorsi flexion of the foot. It may present with concomitant bony and ligamentous injury. While surgical intervention is rarely indicated in the absence of fracture, conservative PT management can aide in a faster recovery.
References[edit | edit source]
- ↑ 1.0 1.1 Norkus S, Floyd RT, The Anatomy and Mechanisms of Synedesmotic Ankle Sprains. J Athletic Training. 2001;36:68-73
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 2.9 5. Clanton T. Syndesmotic ankle sprains in athletes. International SportMed Journal. 2003;4 (4):1-10. 6
- ↑ Boytim MJ, Fischer DA, Neumann L. Syndesmotic ankle sprains. Am J Sports Med. 1991;19:294–298
- ↑ Nussbaum E, Hosea T, Sieler S, Incremona B, Kessler D. Prospective Evaulation of Syndesmotic Ankle Sprains Without Diastasis. The American Journal of Sports Medicine. 2001;29 (1): 31-35.
- ↑ Lin CF, Gross ML, Weinhold P. Ankle syndesmosis injuries: anatomy, biomechanics, mechanism of injury, and clinical guidelines for diagnosis and intervention. JOSPT. 2006; 36(6):372-384. 3. Fincher L. Early Recognition of Syndesmotic Ankle Sprain. Athletic Therapy Today. 1999; 42-42.
- ↑ 6.0 6.1 Norwig JA. Injuring Management Update: Recognizing and Rehabilitating the High Ankle Sprain. Professional Jrnl of Athletic Trng Ther. 1998, July; 12-13.
- ↑ 7.0 7.1 7.2 7.3 Fincher L. Early Recognition of Syndesmotic Ankle Sprain. Athletic Therapy Today. 1999; 42-42.
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 8.6 Dressendorfer R. Clinical Review: Syndesmotic Ankle Sprain. CINAHL. 2009.
- ↑ 9.0 9.1 Alonso A, Khoury L, Adams R. Clinical tests for Ankle Syndesmosis Injury: reliability and prediction of return to function. JOSPT. 1998; 27(4):276-84
- ↑ Starkey C, Ryan JL. Evaluation of Orthopedic and Athletic Injuries. Philadelphia, PA: FA Davis; 1996. pp. 86–95
- ↑ Magee D. Orthopedic Physical Assessment. 4th Edition. St. Louis, Missourie: Saunders Elsevier; 2006
- ↑ Pajaczkowski A. Rehabilitation od distal tibiofibular syndesmosis sprains: a case report. <i>JC CA<i/> 2007; 51(1):42-49
- ↑ 13.0 13.1 13.2 Recovering from an ankle sprain. Harvard Women’s Health Watch. 2007 Feb; 14(6):4-6.
- ↑ Bleakley CM, McDonough SM, MacAuley DC. Some conservative strategies are effective when added to controlled mobilization with external support after acute ankle sprain: a systematic review. Aust J Physiother. 2008;54(1):7-20.
- ↑ Dolan, MG (2009) Clinical Research Review: Conservative Strategies in Ankle Sprain Management 14(5):8-10.
- ↑ Green T, Refshauge K, Crosbie J, Adams A (2001) A randomized controlled trial of a passive accessory joint mobilization on acute ankle inversion sprains. Physical Therapy 81: 984-994
- ↑ Collins N, Teys P, Vicenzino B (2004) The initial effects of a Mulligan’s movilisation with movement technique on dorsiflexion and pain in subacute ankle sprains. Manual Therapy 9: 77-82.
- ↑ Landrum EL, Kelln BM,, Parente WR, Ingersoll CD, Hertel J. Immediate effects of anterior-to-posterior talocrural joint mobilization after prolonged ankle immobilization: a preliminary study. J Man Manip Ther 2008;16(2):100-105