Sulfonylureas in the Treatment of Diabetes Mellitus
Original Editor - Ashton Randolph
Top Contributors - Lucinda hampton, Shanice Rouse, Ashton Randolph and Aminat Abolade
Introduction[edit | edit source]
Sulfonylureas represent a class of medications utilized in the treatment of type 2 diabetes mellitus. When metformin is not sufficient, as indicated by an HbA1c >8.0%, a sulfonylurea can be added. Sulfonylureas can be used as the first drug in lean type 2 patients or in those patients who cannot tolerate metformin.[1]
Mechanism of Action and Administration[edit | edit source]
Sulfonylureas increase the release of insulin through the stimulation of pancreatic beta cells. Sulfonylureas, consequently, are a more potent medication in the earlier stages of type 2 diabetes when a patient has an increased pancreatic beta-cell function[2].
All sulfonylureas are taken orally and bind mainly to albumin after absorption occurs in the intestines. To improve efficacy, medications in this class should be taken about 30 minutes before meals. The dose should be increased gradually until control is adequate (HbA1c <8.0%).
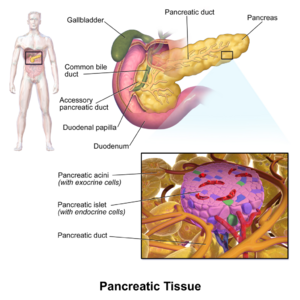
Image 2: Structure of pancreas, revealing the Islet of Langerhans
Adverse Effects[edit | edit source]
The major adverse effects of sulfonylureas are hypoglycaemia (because of its long-acting mechanism) and weight gain.[1]
- The hypoglycemic effects of sulfonylureas can be potentiated by certain drugs including NSAIDs, ACE inhibitors, fluoxetine, monoamine oxidase inhibitors, and beta-adrenergic blocking agents[3].
- Other much less common side effects of sulfonylurea treatment include GI distress and skin reactions[4].
Physiotherapy[edit | edit source]
Physical therapists should be aware of the adverse effects of sulfonylurea treatment as they have important clinical implications. Blood glucose levels should be taken before therapy sessions and after to ensure patient safety. During therapy sessions the therapist should be observant for indications of low blood glucose such as anxiety, confusion, headache, and sweating.[4][5] Patients may need to be scheduled before taking their medicine or after they reach the peak serum level to avoid cases of extreme hypoglycemia.
Education of Client:
- Because hypoglycemia is more likely to occur when there is a caloric deficit, encouraging patients to stick to a meal schedule and eat in the absence of hunger is important to ensure proper insulin and glucose levels.
- Therapists should also encourage patients to eat prior to physical activity to reduce the risk of hypoglycemia[6].
- Patients taking sulfonylureas also should have their renal function and body weight monitored regularly.
- Advice about exercise should take into account the presence of ischaemic heart disease or foot problems.[1]
Back to Pharmacological Management of Diabetes Mellitus[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 NPS medwise The management of type 2 diabetes Available:https://www.nps.org.au/australian-prescriber/articles/the-management-of-type-2-diabetes (accessed 26.9.2021)
- ↑ Costello RA, Shivkumar A. Sulfonylureas. StatPearls [Internet]. 2021 Jun 15.Available:https://www.ncbi.nlm.nih.gov/books/NBK513225/ (accessed 26.9.2021)
- ↑ DiaBeta (glyburide) Tablets USP 1.25, 2.5 and 5 mg. (2009). Bridgewater, NJ: sanofi-aventis U.S. LLC.
- ↑ 4.0 4.1 Ciccone, C. D. (2016). Pharmacology in Rehabilitation.Philadelphia: F.A. Davis Company.
- ↑ Ahrẻn B. Avoiding hypoglycemia: a key to success for glucose-lowering therapy in type 2 diabetes. Vasc Health Risk Manag. 2013; 9: 155-163
- ↑ Type 2 diabetes. (2018, September 15). Retrieved from Mayo Clinic: https://www.mayoclinic.org/diseases-conditions/type-2-diabetes/diagnosis-treatment/drc-20351199