Sporting Elbow - Clinical Reasoning and Differential Diagnosis
Top Contributors - Wanda van Niekerk, Kim Jackson, Jess Bell, Robin Leigh Tacchetti and Robin Tacchetti
Introduction[edit | edit source]
The elbow is a complex joint and stability is provided by osseous and soft-tissue constraints. The elbow's relative instability makes it vulnerable to injuries, often caused by sports[1] and these injuries often involve several of the structures associated with the joint.[2] Apart from the clinical history, clinical reasoning and the physical examination are essential to make a diagnosis.
Anatomy of the Elbow[edit | edit source]
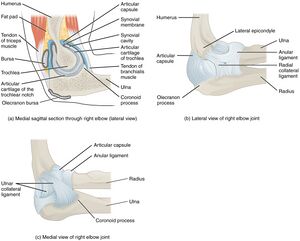
The distal humerus meets the proximal radius and ulna bones to form the elbow joint. It is known as a trochleogingylomoid joint as it can flex and extend as a hinge (ginglymoid) joint, as well as pivot around an axis (trochoid motion) (i.e. pronation and supination). It is an extremely congruent and stable joint.[3][4] The stability of the elbow is provided by the osseous anatomy, capsuloligamentous structure and the musculotendinous units that cross the elbow.[5]
Joints[edit | edit source]
The humerus, radius and ulna articulate to form the three joints that make up the elbow. [2] Table 1 provides an anatomical overview of the elbow. For more detailed information on the specific elbow joints, please read: The Complex Anatomy of the Elbow - Joints
| Humeroulnar Joint | Radiohumeral Joint | Proximal Radioulnar Joint | |
|---|---|---|---|
| Active range of motion norms | Flexion 140°
Extension 0 - 10° |
Flexion 140°
Extension 0 - 10° |
Pronation 80 -90°
Supination 80 -90° |
| Capsular pattern | Flexion and extension | Flexion and extension | Equal limitations of supination and pronation |
| Ligaments | Ulnar collateral ligament
(UCL -anterior oblique bundle; posterior oblique bundle; intermediate bundle; transverse ligament) Lateral ulnar collateral ligament (LUCL) |
Radial collateral ligament (RCL) | Annular ligament
Quadrate ligament Oblique cord Interosseous membrane |
Ligaments and Capsule[edit | edit source]
The Medial Collateral Ligament Complex (MCLC) / Ulnar Collateral Ligament is the most important stabiliser of the elbow and it provides valgus and posteromedial stability. It comprises an anterior and posterior bundle and a supporting transverse ligament (ligament of Cooper). The anterior band is more taught in extension and relaxes into flexion, whereas the posterior band tightens in flexion and releases in extension. Thus, the anterior band is more vulnerable to valgus stress in elbow extension and the posterior band of the anterior medial collateral ligament (AMCL) is more vulnerable to valgus stress in elbow flexion.[7]
The Lateral Collateral Ligament Complex (LCLC) is the primary stabiliser against varus and external rotation stresses. It is formed by the lateral ulnar collateral ligament, the radial collateral ligament and the annular ligament.
The joint capsule surrounds all three joints of the elbow. There is a thickening medially and laterally of the joint capsule that blend with the MCLC and LCLC respectively and this contributes to the stability of the elbow.[8]
For more information, please read: The Complex Anatomy of the Elbow - Ligaments and Capsule
Muscles[edit | edit source]
| Muscle Synergy of the Elbow | |
|---|---|
| Flexion | Primary Flexors:
Secondary Flexors:
|
| Extension | Primary Elbow Extensors
Secondary Extensors |
| Pronation | |
| Supination | |
Differential Diagnosis[edit | edit source]
Take into consideration both form (structures) and function in the differential diagnosis of the elbow.[9]
Form[edit | edit source]
- Cervical radiculopathy (referred pain)[10]
- Systemic conditions (e.g. Rheumatoid Arthritis)[11]
- Anterior elbow:
- Biceps strain/tear/tendinopathy[12]
- Myositis ossificans in brachioradialis[13]
- Osteochondritis dissecans (trochlea)[14]
- Posterior elbow
- Radial side of elbow
- Synovial plica[18]
- Lateral epicondylalgia (involvement of extensor carpi radialis brevis)
- Osteochondritis dissecans (radio-capitellum)[14]
- Posterolateral rotatory instability (PLRI) - radiocarpal ligament combined with lateral ulnar collateral ligament[19][20]
- Nerve entrapment: posterior interosseus nerve (radial tunnel syndrome)[21]
- Ulnar side
- Medial epicondylalgia (Golfer’s Elbow)[22]
- Nerve entrapment of ulnar nerve[23]
- Dislocations can cause injury to the ulnar nerve
- Fractures
It is evident that there is a large number of conditions related to form that should be considered with the differential diagnosis of elbow pain. Thus, it can be helpful to distinguish between traumatic and non-traumatic mechanisms.[9]
| Diagnosis | Sport in which injury commonly occur |
|---|---|
| Biceps tendon rupture | Strength training; weightlifting[24] |
| Lateral elbow tendinopathy | Sports associated with repeated gripping and/or wrist extension activities such as tennis, squash, badminton[5] |
| Flexor/pronator tendinopathy (golfer's elbow) | Golf and in tennis players who uses a lot of topspin on their forehand |
| Medial collateral ligament sprain | Throwing sports such as baseball, javelin, water polo, handball, cricket[5] |
| Ulnar nerve entrapment | Throwing sports[5] |
| Olecranon bursitis | Athletes falling on the posterior aspect of the elbow on hard surfaces in sports such as football (goalkeepers) and basketball[5] |
| Posterior dislocation | Contact sports or when falling from a height such as pole vaulting[5] |
Function[edit | edit source]
Although the form/structures might be compromised in athletes with elbow injuries, often these individuals still show a high level of function in the injured area. As part of the differential diagnosis, it is key to not only identify the structures involved but also to have a clear picture of function (i.e. what the athlete can do; the pain pattern over time; traumatic vs non-traumatic injury; and urgency vs non-urgency in relation to surgical management).[9]
Factors relevant to function include:
- Kinetic chain
- Knowledge and understanding of the kinetic chain and how different components can be affected is important. For example, when a boxer throws a punch with his lead arm, the force is coming from the feet driving up into the hip. Approximately 50% of the force will come from the lower legs, 30% from the trunk and 20% from the upper limb.
- Keep in mind that these percentages may be different in different athletes (i.e. wheelchair-based athletes and swimmers)
- The key consideration is to acknowledge and understand the whole body contribution in an injury, pathology or dysfunction.[9]
- Strength Testing
- Isometric testing
- An examiner applying resistance with their hand in different ranges will provide information on quality
- Isometric testing with a handheld dynamometer will provide quantitative information in different ranges
- Isokinetic testing
- Testing strength through range of motion
- Strength testing in tennis elbow
- Dorf et al.[25] investigated the effect of elbow position on grip strength in the evaluation of lateral epicondylitis. They found that there was no difference in grip strength in elbow flexion and extension for the healthy extremity. Grip strength was 29% stronger in elbow flexion than extension for the affected extremity. When comparing the healthy extremity with the affected extremity, the affected extremity was 50% weaker in elbow extension compared to the healthy extremity. In elbow flexion, the affected extremity was 31% weaker than the healthy extremity. This is significant especially with regards to elbow extension providing a mechanical advantage in grip strength of the hand. Using strength testing in people with tennis elbow will provide better objectivity.[25]
- Isometric testing
- Range of motion
- Movements at the elbow to consider and measure:
- Flexion and extension
- Pronation and supination
- Smartphone apps are available to help clinicians measure elbow range of motion.[26]
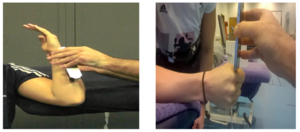
- Measuring flexion and extension with an inclinometer app on smartphone
- Patient rests arm flat on table, so that the humerus is parallel to the horizontal plane. The forearm is in neutral. Inclinometer is set to zero on table. The patient flexes elbow maximally. Smartphone placed parallel to forearm and value can be read.[26]
- For elbow extension the smartphone is aligned to the forearm in maximal extension.[26]
- Movements at the elbow to consider and measure:
- End-feel
Special Investigations[edit | edit source]
- Ultrasound
- Can assist in the management of stubborn cases of lateral epicondylalgia by characterising the extent of the tendon tearing and identifying the presence of concomitant RCL injury.[27]
- MRI
- Injection (Lignocaine or Marcaine)[28]
Clinical Tests[edit | edit source]
- Lateral epicondylalgia
- Middle finger strength test/Maudsley’s test
- Mill’s test
- Cozen’s test
- Chairlift test
- Polk’s test lateral
- Grip strength test
- Medial collateral ligament complex/ulnar collateral ligament insufficiency
- Moving valgus stress test
- Valgus stress test
- Milking manoeuvre
Valgus Stress Test video provided by Clinically Relevant
Milking Maneuver Test video provided by Clinically Relevant
- Posterolateral rotatory instability
- Table-top relocation test
- Stand-up test/chair push up test
- Push-up test
- Lateral pivot shift test
Table Top Relocation Test video provided by Clinically Relevant
Lateral Pivot Shift Test video provided by Clinically Relevant
Chair Sign Test video provided by Clinically Relevant
- Total distal biceps rupture
- Hook test
- Passive forearm pronation (PFP) test
- Supination-pronation test
- Biceps squeeze test
- Biceps crease interval (BCI)
- Bicipital aponeurosis (BA) flex test
- Total distal triceps rupture
- Triceps squeeze test
- Posteromedial impingement syndrome
- Arm bar test
- Valgus overload test/posteromedial impingement test
- Medial epicondylalgia
- Epicondylitis medialis test/ Golfer’s elbow test
- Polk’s test medial
Whatever clinical test is being performed, always consider the amount of stress being applied to the structure and the element of safety.[9]
Proximal Radioulnar Joint and Humeroradial Joints in Lateral Epicondylalgia[edit | edit source]
It is important to consider the proximal radioulnar joint (PRUJ) and the humeroradial joints (HR) in relation to lateral epicondylalgia. Specifically taking into consideration the following:
- Extensor carpi radialis brevis arises from the lateral epicondyle and the annular ligament
- Radial collateral ligament also originates from lateral epicondyle and inserts into the ligament
- The close relationship between ECRB and RCL is seen in:
- Concomitant injuries
- Potential instability around this region may provoke lateral epicondylalgia (tennis elbow)
Therefore, having a good understanding of the close relationship between ECRB and RCL, as well as the mobility of the radiohumeral joint will have an impact on lateral epicondylalgia (tennis elbow) management. Furthermore, consider the open- and close-packed positions of the elbow joints to avoid confusion when palpating or mobilising these joints.
| Joints | Open Packed | Close Packed |
|---|---|---|
| PRUJ | Elbow flexion (70°)
Supination (5°) |
Elbow extension
Full supination |
| HR | Elbow extension
Full supination |
Elbow flexion (70°)
Supination (5°) |
Medial Epicondylalgia and Pronator Teres[edit | edit source]
- Hypertrophy of pronator teres may lead to symptoms around the medial epicondyle of the elbow.
- Pronator teres syndrome – i.e. the median nerve is trapped between the two heads of pronator – will mainly produce symptoms distally rather than locally.
Conclusion[edit | edit source]
General guidelines to consider:[9]
- Diagnosis
- Consider traumatic vs non-traumatic injuries
- Structures (form) involved
- Prognosis = function
- What can or can’t the athlete do?
- Strength
- Range of motion
- End feel
- With non-traumatic injuries consider contributions from the shoulder and forearm, as well as the hand and wrist.
- For lateral epicondylalgia and medial epicondylalgia, consider the surrounding structures that could also be involved
- The elbow can be tricky – if unsure get a second opinion!
References[edit | edit source]
- ↑ Zwerus EL, Somford MP, Maissan F, Heisen J, Eygendaal D, Van Den Bekerom MP. Physical examination of the elbow, what is the evidence? A systematic literature review. British journal of sports medicine. 2018 Oct 1;52(19):1253-60.
- ↑ 2.0 2.1 Acosta Batlle J, Cerezal L, Lopez Parra MD, Alba B, Resano S, Blazquez Sanchez J. The elbow: review of anatomy and common collateral ligament complex pathology using MRI. Insights into imaging. 2019 Dec;10(1):1-25.
- ↑ Bryce CD, Armstrong AD. Anatomy and biomechanics of the elbow. Orthopedic Clinics of North America. 2008 Apr 1;39(2):141-54.
- ↑ Cavallo M, Rotini R, Cutti AG, Parel I. Functional Anatomy and Biomechanic Models of the Elbow. In The Elbow 2018 (pp. 29-40). Springer, Cham.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 Vicenzino w, Scott A, Bell S, Popovic N. Elbow and arm pain. In: Brukner P, Clarsen B, Cook J, Cools A, Crossley K, Hutchinson M, McCrory P, Bahr R, Khan K. eds. Brukner & Khan’s Clinical Sports Medicine: Injuries, Volume 1, 5e.Sydney: McGraw Hill, 2017.
- ↑ Ward K. The elbow region: anatomy, assessment and injuries. InRoutledge Handbook of Sports Therapy, Injury Assessment and Rehabilitation 2015 Sep 16 (pp. 458-498). Routledge.
- ↑ Smith JR, Amirfeyz R. Clinical Anatomy of the Elbow. InSports Injuries of the Elbow 2021 (pp. 1-13). Springer, Cham.
- ↑ Chin K, Hussain S, Mazis G, Arya A. Clinical anatomy and biomechanics of the elbow. Journal of Clinical Orthopaedics and Trauma. 2021 Jun 24:101485.
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 9.6 Gatt, I. Sporting Elbow - Clinical Reasoning and Differential Diagnosis Course. Plus. 2021.
- ↑ Kang KC, Lee HS, Lee JH. Cervical radiculopathy focus on characteristics and differential diagnosis. Asian Spine Journal. 2020 Dec;14(6):921.
- ↑ Javed M, Mustafa S, Boyle S, Scott F. Elbow pain: a guide to assessment and management in primary care. British Journal of General Practice. 2015 Nov 1;65(640):610-2.
- ↑ Bauer TM, Wong JC, Lazarus MD. Is nonoperative management of partial distal biceps tears really successful?. Journal of shoulder and elbow surgery. 2018 Apr 1;27(4):720-5.
- ↑ Devilbiss Z, Hess M, Ho GW. Myositis ossificans in sport: a review. Current sports medicine reports. 2018 Sep 1;17(9):290-5.
- ↑ 14.0 14.1 14.2 Churchill RW, Munoz J, Ahmad CS. Osteochondritis dissecans of the elbow. Current reviews in musculoskeletal medicine. 2016 Jun;9(2):232-9.
- ↑ Shuttlewood K, Beazley J, Smith CD. Distal triceps injuries (including snapping triceps): a systematic review of the literature. World journal of orthopedics. 2017 Jun 18;8(6):507.
- ↑ Nchinda NN, Wolf JM. Clinical Management of Olecranon Bursitis: A Review. The Journal of Hand Surgery. 2021 Apr 9.
- ↑ Robinson PM, Watts AC. Boxer’s Elbow: Internal Impingement of the Coronoid and Olecranon Process. InSurgical Techniques for Trauma and Sports Related Injuries of the Elbow 2020 (pp. 189-193). Springer, Berlin, Heidelberg.
- ↑ Lubiatowski P, Wałecka J, Dzianach M, Stefaniak J, Romanowski L. Synovial plica of the elbow and its clinical relevance. EFORT Open Reviews. 2020 Sep;5(9):549-57.
- ↑ Conti Mica M, Caekebeke P, van Riet R. Lateral collateral ligament injuries of the elbow–chronic posterolateral rotatory instability (PLRI). EFORT open reviews. 2016 Dec;1(12):461-8.
- ↑ Fedorka CJ, Oh LS. Posterolateral rotatory instability of the elbow. Current reviews in musculoskeletal medicine. 2016 Jun;9(2):240-6.
- ↑ Moraes MA, Goncalves RG, Santos JB, Belloti JC, Faloppa F, Moraes VY. Diagnosis and treatment of posterior interosseous nerve entrapment: systematic review. Acta ortopedica brasileira. 2017 Jan;25:52-4.
- ↑ Barco R, Antuña SA. Medial elbow pain. EFORT open reviews. 2017 Aug;2(8):362-71. Instability UCL ligament Rossy WH, Oh LS. Pitcher’s elbow: medial elbow pain in the overhead-throwing athlete. Current reviews in musculoskeletal medicine. 2016 Jun;9(2):207-14.
- ↑ McCarty LP. Approach to medial elbow pain in the throwing athlete. Current reviews in musculoskeletal medicine. 2019 Mar;12(1):30-40.
- ↑ Pitsilos C, Gigis I, Chitas K, Papadopoulos P, Ditsios K. Systematic review of distal biceps tendon rupture in athletes: Treatment and Rehabilitation. Journal of Shoulder and Elbow Surgery. 2022 Mar 31.
- ↑ 25.0 25.1 Dorf ER, Chhabra AB, Golish SR, McGinty JL, Pannunzio ME. Effect of elbow position on grip strength in the evaluation of lateral epicondylitis. The Journal of hand surgery. 2007 Jul 1;32(6):882-6.
- ↑ 26.0 26.1 26.2 Vauclair F, Aljurayyan A, Abduljabbar FH, Barimani B, Goetti P, Houghton F, Harvey EJ, Rouleau DM. The smartphone inclinometer: A new tool to determine elbow range of motion?. European Journal of Orthopaedic Surgery & Traumatology. 2018 Apr;28(3):415-21.
- ↑ Smith J, Finnoff JT. Diagnostic and interventional musculoskeletal ultrasound: part 2. Clinical applications. PM&R. 2009 Feb 1;1(2):162-77.
- ↑ Hsieh LF, Kuo YC, Lee CC, Liu YF, Liu YC, Huang V. Comparison between corticosteroid and lidocaine injection in the treatment of tennis elbow: a randomized, double-blinded, controlled trial. American journal of physical medicine & rehabilitation. 2018 Feb 1;97(2):83-9.
- ↑ Clinical Physio. Maudsley's Test. Available from: watch?v=tV8mymHe8Nw[last accessed 1 December 2021]
- ↑ The Student Physical Therapist. Mill's Test. Available from: https://www.youtube.com/watch?v=-qbwX4SCHNY [last accessed 1 December 2021]
- ↑ Clinical Physio. Cozen Test for Lateral Epicondylitis (Tennis Elbow) Available from: watch?v=faCi3v5Heo0&t=24s [last accessed 1 December 2021]