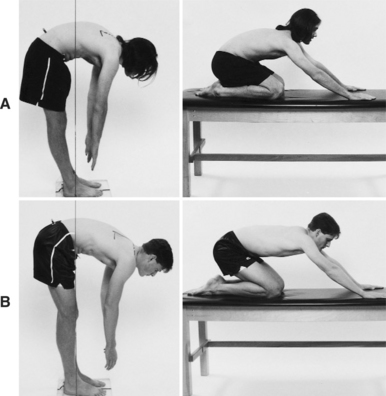
Shirley Sahrmann's Lumbar Flexion Syndrome
Introduction[edit | edit source]
There is rapidly growing acceptance among clinicians and researchers that the development of movement-based diagnostic frameworks is the way forwards in managing chronic and recurrent low back pain (LBP). The systems most supported by evidence are those that examine interrelationships between altered patterns of muscle recruitment and motor control strategies and establish a direction-based mechanism of provocation or relief of symptoms[1][2]. In the lumbar spine this approach is now well established. In the management of non-specific low back pain the subgrouping and classification of patients’ symptoms based on the assessment of movement and motor control has become more important than trying to identify a pathology based diagnosis[3][4].
A majority of spinal dysfunction is the result of cumulative microtrauma caused by impairments in alignment in stabilization and in movement patterns of the spine. In the properly functioning spine the balanced isometric support and control provided by the trunk muscles prevent these impairments[3]. Different postural positions have been shown to alter trunk muscle activation[5].In particular a lumbopelvic upright posture (with a maintained lumbar lordosis and some anterior pelvic tilt) recruits more of the internal oblique and superficial multifidus muscles than does an upright posture of thoracic extension, where there is less lumbar extension and anterior pelvic tilt, less superficial multifidus and internal oblique recruitment and more erector spinae activation. Similarly, sway standing postures and slump sitting postures decrease activity in the internal oblique and multifidus muscles and sway standing increases the activity in rectus abdominis. These changes in muscle recruitment patterns have been linked to the presence of lumbopelvic pain[3][6][5].Changes in the alignment of the lumbar spine have been noted in subjects with flexion-related lumbar pain[5].
One of those lumbar pain issues is lumbar flexion syndrome using S.Sharmann's classification. Lumbar flexion syndrome with and without radiating symptoms is more often found in men than women and in young individuals. Acutely herniated disk problems are most often associated with flexion[3].A patient can experience back pain of varying degrees of severity and acuity, as well as varying degrees of radiating symptoms. Pain problems include herniated disk disease, lumbosacral strain, lumbago, and degenerative disk disease[3].Major contributing factors that impose flexion on the lumbar spine include the following:
- Sitting with the lumbar spine flexed with the head and shoulders forward of the spine
- Having a structurally flat back
- Developing excessive flexion flexibility of the lumbar spine, which causes forward leaning motions to occur more readily in the spine than in the hips[3].
Alignment[edit | edit source]
The structural characteristics in alignment and body proportions that may be present in patients with the flexion syndrome include the following: tall in height and having a long trunk relative to the lower body, long tibias that cause the knees to be higher than the hips when sitting, and a flat back without posterior pelvic tilt and usually high iliac crests. The acquired impairments in alignment are swayback posture and a flat back with posterior pelvic tilt[3].
Muscle and Recruitment Pattern Impairments[edit | edit source]
The abdominal muscles may be recruited more readily than the hip flexors for leaning forward while in the sitting position. The hamstring and gluteus maximus muscles may be short and/or stiff. The back extensor muscles may be long and/or weak, whereas the abdominal muscles may be short and/or weak[3].
Relative stiffness (restrictions)
Hamstrings restriction of hip flexion – the hips lack 70° of normal range in standing forward bending. The lumbar spine frequently increases flexion to compensate for the lack of hip mobility. Hamstring extensibility can be tested passively and dynamically with manual muscle extensibility examination.
Thoracic restriction of flexion – mid and upper thoracic flexion restriction may also contribute to compensatory increases in lumbar flexion range. This is confirmed with manual segmental assessment (e.g. Maitland passive physiological intervertebral movements or passive accessory intervertebral movements)[7].
Relative flexibility (potential UCM)
Lumbar flexion – the lumbar spine may initiate the movement into flexion and contribute more to producing forward bending while the hips and thoracic contributions start later and contribute less. At the limit of forward bending, excessive or hypermobile range of lumbar flexion may be observed. During the return to neutral the lumbar flexion and posterior pelvic tilt persists and unrolls late[8].
Physical Examination and Movement Impairments[edit | edit source]
Standing position the following tests are performed with the patient in a standing position: position effects and forward bending.
- Position effects. In the standing position the patient has less symptoms than when he or she is sitting.
- Forward bending. The lumbar spine is often flat, it flexes more readily than the hips and this movement increases the symptoms. To confirm a positive test for lumbar flexion the patient performs forward bending with hip flexion only when the hands are on a raised table to support the body. The therapist notes the effect of this movement on the symptoms. If the patient has radicular symptoms there may be an increase of symptoms even with the corrected forward bending.
Supine position the following tests are performed with the patient in a supine position: position effects hip and knee flexion and bilateral hip and knee flexion.
- Position effects. In the supine position the patient is often able to keep his hips and knees extended without increasing his symptoms. If compression contributes to his symptoms he may need to flex his hips and knees.
- Hip and knee flexion. At the end of this movement passively pulling his knee to his chest may increase his symptoms because of the associated lumbar spine flexion.
- Bilateral hip and knee flexion. At the end of this movement passively pulling his knees to his chest may increase his symptoms because of the associated lumbar spine flexion.
Prone position the following tests are performed with the patient in a prone position:position effects and knee flexion.
- Position effects. The prone position may decrease symptoms.
- Knee flexion. At the initiation of this movement there may be posterior pelvic tilt, but this finding is not common.
Quadruped position The following tests are performed with the patient in a quadruped position: position effects and rocking backward.
- Position effects. In the quadruped position the lumbar spine is often flexed and the hips are in less than 90 degrees of flexion. When the patient allows his lumbar spine to flatten or assume a neutral alignment often symptoms will decrease.
- Rocking backward. When performing this movement the lumbar spine flexes and the symptoms may increase. To confirm a positive test for lumbar flexion the patient maintains a flat lumbar spine and rocks backward by flexing only at the hips. The therapist notes the effect of this motion on the symptoms.
Sitting position The following tests are performed with the patient in a sitting position: position effects spine in flexion, spine in extension and knee extension.
- Spine in flexion. With the lumbar spine in flexion there is an increase in the symptoms.
- Spine in extension. With the lumbar spine in extension there is a decrease in the symptoms.
- Knee extension. This movement causes posterior pelvic tilt and lumbar flexion and may increase the symptoms. To confirm a positive test for lumbar flexion the spine and pelvis is supported to prevent the flexion movement. The therapist notes the effect of preventing this motion on the symptoms[3].
Confirming Tests[edit | edit source]
When the patient avoids the flexed alignment of his spine and learns to lean forward by moving the hips and not the lumbar spine, the symptoms will decrease[3].
Physical Treatment[edit | edit source]
PRIMARY OBJECTIVES. The primary objective of the exercise program is to teach the patient to sit correctly and to move in the hips, not in the lumbar spine.The keys to preventing and alleviating spinal dysfunction are to have]] the trunk muscles hold the vertebral column and pelvis in their optimal alignments and to prevent unnecessary movement. To achieve these goals the muscles must be the correct length and strength and be able to produce the correct pattern of activity. During movement of the extremities optimal isometric contraction of the trunk muscles is needed to appropriately stabilize the proximal attachments of the limb muscles[3]. Also treatment includes patient education, analysis and correction of daily activities and prescription of specific exercises[11]
[12]
Corrective Exercise Program[edit | edit source]
Supine. The patient performs hip and knee flexion by passively pulling the knee to the chest with the hands, making certain not to flex the lumbar spine. If the rectus abdominis muscles have become short or stiff, the patient performs shoulder flexion to the maximum range and then lifts the chest to improve the length of the muscle.
Side lying. There are no specific exercises for this syndrome in the side-lying position.
Prone. The patient places the shoulders in flexion in the overhead position and flexes one shoulder at a time to improve the performance of the back extensor muscles. The patient places a pillow under the abdomen to bring the hips into slight flexion, and he or she performs unilateral hip extension to improve the performance of the back extensor muscles.
Quadruped. The patient allows the lumbar spine to become flat or slightly extended. The patient rocks backward making certain the motion is hip flexion not lumbar flexion.
Sitting. The patient sits and performs knee extension. Using the back of the chair as support, the patient performs isometric back extension. If the hamstring muscles are particularly short, the patient sits with his or her foot on a footstool, stretching the hamstring muscles for 15 to 20 seconds at a time. The patient leans forward using hip flexion and not lumbar flexion, and performs the sit-to-stand motion without lumbar flexion.
Standing. The patient bends forward with motion occurring in the hips, not in the lumbar spine. The patient may need to flex the knees during this motion. He or she practices the squatting motion while avoiding lumbar flexion. If the rectus abdominis muscle is short or stiff, the patient stands with the back to the wall, shoulders flexed overhead, and chest lifted. Care is taken to avoid flattening the lumbar spine.
Correcting postural habits and movement patterns. The sitting posture and the movement pattern during leaning forward are two of the most important habits to correct. The patient may also perform bentknee sit-up exercises, which should be eliminated[3].
References[edit | edit source]
- ↑ Luomajoki H, Kool J, de Bruin E.D, Airaksinen O. Improvement in low back movement control, decreased pain and disability, resulting from specific exercise intervention. Sports Medicine, Arthroscopy, Rehabilitation, Therapy and Technology 2010;23(2):11.
- ↑ Van Dillen L.R, Maluf K.S, Sahrmann S.A. Further examination of modifying patient-preferred movement and alignment strategies in patients with low back pain during symptomatic tests. Manual Therapy 2009;14 (1), 52–60.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 Sahrmann S. Diagnosis and Treatment of Movement Impairment Syndromes. Mosby, 2002.
- ↑ Fritz J.M, Cleland J.A, Childs J.D. Subgrouping patients with low back pain: evolution of a classification approach to physical therapy. Journal of Orthopaedic and Sports Physical Therapy 2007; 37 (6), 290–302.
- ↑ 5.0 5.1 5.2 O’Sullivan P.B, Mitchell T, Bulich P, Waller R, Holte J. The relationship between posture and back muscle endurance in industrial workers with flexion-related low back pain. Manual Therapy 2006; 11 (4), 264–271.
- ↑ Dankaerts W, O’Sullivan P.B, Burnett A.F, Straker L.M. The use of a mechanism-based classification system to evaluate and direct management of a patient with non-specific chronic low back pain and motor control impairment – a case report. Manual Therapy 2007; 12 (2),181–191.
- ↑ Maitland G, Hengeveld E, Banks K, English K. Maitland’s vertebral manipulation. Oxford: Butterworth Heinemann, 2005.
- ↑ Comerford M, Mottram S. Kinetic Control The Management of Uncontrolled Movement. Elsevier Australia: Churchill Livingstone, 2012.
- ↑ Physiotutors. Luomajoki Lumbar Movement Control Dysfunction Screening. Available from: https://www.youtube.com/watch v=A4gU0YD6HS4&list=PLO_peL93VBmlQuSYrCQutFiqqTDgUByxK&index=4 [last accessed 18/02/2020]
- ↑ hysiotutors. Lumbar Spine Local Stabilizers Assessment | Pressure Biofeedback Unit Available from: https://www.youtube.com/watch?v=O0bMUrzZxAA&list=PLO_peL93VBmlQuSYrCQutFiqqTDgUByxK&index=7[last accessed 18/02/2020]
- ↑ Sahrmann S. Movement System Impairment Syndromes of the Extremities, Cervical and Thoracic Spines.Elsevier: Health Sciences, 2010.
- ↑ Physiotutors. Lumbar Movement Control Exercises | Motor Control Impairment . Available from: https://www.youtube.com/watch?v=x6mRy22eYkA&list=PLO_peL93VBmlQuSYrCQutFiqqTDgUByxK&index=5 [last accessed 18/02/2020]