Running Mechanics for Clinicians
Original Editor - Mariam Hashem
Top Contributors - Mariam Hashem, Kim Jackson, Tarina van der Stockt, Jess Bell and Robin Tacchetti
Overview of Running Injuries[edit | edit source]
Lower extremity running-related injuries range from 19.4 to 79.3 percent[1]. Most runners in any one-year period will report an injury. [2]. The most common injuries are:[3][4]
- Patellofemoral pain
- Medial tibial stress syndrome (shin splints)
- Achilles tendinopathy
- Iliotibial band syndrome
- Plantar fasciitis
- Stress fractures of the metatarsals and tibia
*** The majority of running-related injuries are due to aggregate loading, are chronic in nature and located in the lower limbs.[5]
Hamstrings and calf problems were reported by male marathon runners, while hip pain problems were common among women[6]. Most of these injuries have a high recurrence rate.
A study from 2018 by Poppel and colleagues found that previous injuries, training volume and age are important risk factors for running related injuries.[7] Sanfilippo and colleagues also note that previous injury was the most relevant risk factor for running-related injuries.[8] A 2015 systematic review[9] of 15 studies identified different risk factors for women and men:
| Women | Men contributing factors to tissue stress | |
|---|---|---|
| Age | History of previous injury | |
| History of previous sports activity | Running experience for 2 years | |
| running on a concrete surface | History of previous injury | |
| Participating in a marathon | Average weekly running distance (20–29 miles) | |
| weekly running distance (30–39 miles) | ||
| wearing running shoes for 4 to 6 months |
Stress Frequency Model[edit | edit source]
Running injuries are caused by multiple, related factors. A simple injury causation model using the stress frequency curve can help us to develop an idea about the contributing factors and how to address them in the management plan.
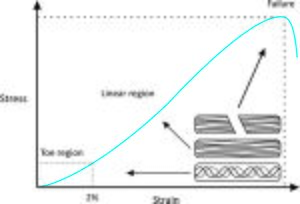
A tissue is influenced by the applied stress and the frequency of application. If the stress and its frequency are below the injury threshold, the tissue will function normally within its capacity. However, if either or both of these factors exceeded the injury threshold, the tissue is more likely to be injured. This explains why some runners may not experience injury for a long time and develop one as soon as they increase their frequency of training such as training for a marathon.
Considering stress and frequency is important to understand individual tissue's capacity.
Running mechanics influence the stress applied to the body, magnitude, type (bending, shear or tension) and the speed of application on each foot contact. Assessing running mechanics leads us to think about the stressed structure and explains the presented symptoms. For example; landing on toes -forefoot strike- results in greater stress on Achillies tendon and the calf muscle forces[10].
Assessing the frequency of running and training volume to understand the effect of the accumulated tissue stress. If falling below the tissue's threshold the likelihood of developing injury will be low and vice versa. A subjective examination can help us to understand the frequency, so ask your client about their weekly training and what is their standard training like? How much running they do? What was the frequency of applied stress before the injury occured?
The next thing is to identify the injury threshold which refers to the interaction between the tissue capacity to tolerate the stress the tissue capacity to tolerate the frequency of the applied stress. Tissue capacity refers to the functional capabilities of a specific tissue to cope with stress type and frequency. A muscle capable of producing high peak force may be able to tolerate high level of stress on individual foot contact. On the contrary, if the muscle's capability is low, applying stress with high frequency the muscle may not be able to cope well leading to injuries. To translate this into practical application, when assessing a runner we should think of adjusting the mechanical pattern or push up the tissue's endurance to tolerate the applied load. Lowering the applied stress by reducing the amount of running can be a method of off-loading the injured tissue while building up the tissue resilience to cope with the functional aspiration.
Clinical Running Assessment Set-Ups[edit | edit source]
Many of the common running-related biomechanical patterns can be identified by 2D analysis using inexpensive tools[11] such as a mobile phone or tablet camera. Standardizing the method of assessment is important for accuracy of identifying the patterns and to make sure your findings are not due to viewing angles.
Settings:
Tools/equipment: High speed camera or mobile phone/tablet camera and a tripod.
Distance: 1.5-2 meters from the treadmill
Height:0.8-1 meter-pelvic height
Views: side (saggital) and rear (frontal)
Timing: initial contact and mid-stance
Joints/regions: thorax, pelvis. hips, knees and ankles.
Follow a structured process of assessment by looking at one joint/region at a time. To end up with a structured problem list, slow down the speed of the camera to allow you to go backward and forward and take still pictures to draw lines and identify areas of stress.
Common Mechanical Patterns[edit | edit source]
Bramah et al found that similar mechanical patterns were associated with multiple injuries[13].
Looking from the saggital plan, we can identify the following patterns:
- Foot Inclination Angle at Initial Contact: by drawing lines to compare the angle between the sole of the shoes and the treadmill. A great angle indicates greater foot inclination. It can potentially be caused by rear foot strike if the runner's toes are too high compared to the heel or a forefoot strike when the inclincation is mainly due to a high angle at the heel. Neither strikes are considered to be superior to the other. Landing with high inclination will limit the ability to engage in dorsiflexion which serves as shock absorption. A high inclined foot will take longer time to get the foot flat on the floor to start the shock absorption mechanics resulting in high impact vertical loading[11]. Fig 3 in the study by Souza RB shows how to identify foot inclination. Conversely, landing with forefoot strike (on tip-toes) allows less time to engage in dorsiflexion utilizing the calf complex and possibly stressing the achilles tendon. Refer to this link to see the difference between different foot strike patterns. In the management plan, a relatively low inclination angle where foot is low to the ground regardless of the type of strike (heel or toe) minimizes the stress on achillies for forefoot runners or engage dorsiflexion for heelstrike runners.
- Knee flexion angle at mid stance: compare a straight line drawn through femur to the floor to a line from the lateral condyle of femur to lateral malleolus (Figure). A greater angle indicates more knee flexion. Injured runners tend to land with more knee extension at initial contact[13] This influences tissue stress and the ability to absorb shocks. During running, the knee and ankle function as suspensions. Landing with the knee in flexion and foot flat engages the suspension spring from the moment the foot touches the ground[11][14]. On the other hand, runners with extended knee and high inclined foot at initial contact are less likely to engage the shock absorption mechanism within knee and ankle resulting in higher shocks. This places greater eccentric demands on the quadriceps and is linked to the development of PFPS[15]. The body can respond by compensating on different levels leading to further complications. From a management perspective, this can e addressed by gait re-education to alter the mechanical pattern and/or eccentric training of quadriceps to meet the shock absorption demands.
Frontal plane:
- Trunk side flexion : the angle between a vertical line drawn through the central line (starting mid-way between Posterior superior iliac spines PSISs upwards through the trunk) and a vertical line starting between PSIS to C7. A greater angle indicates greater side flexion. There is no evidence suggesting an associated pathology with increased trunk side flexion, however, it may indicates compensation from a dysfunction in a distal joint. As the trunk shifts greatly side to side it shifts the body's centre of mass COM. This could result in excessive pelvis drop opposite to the weight bearing leg. To address this pattern we need to think of possible causes for trunk shifting as compensation to off-load hip muscles by shifting COM away.
- Contralateral pelvic drop away from weigh-bearing leg (hip dip): an angle between a horizontal line between PSISs and another horizontal line across the body. Refer to (Figure3) in this study. Healthy runners show some degree of pelvic drop, ranging from 3-4 degrees but it's usually controlled. Injured runners demonstrate contralateral pelvic drop compared to healthy runners which refer to a link between this pattern and multiple injuries. Different compensations can be expected to keep the body's balance as the COM is shifting away from such as increased hip adduction resulting in different presentations such as ITB, patellar maltracking and/or PFPS[13].
- Hip adduction angle: the angle between a horizontal line across the PSISs and another starting at the PSIS on the weight-bearing leg down the central point of the tibiofemoral joint. A greater angle indicates great hip adduction. Losing the gap between the knees indicates greater hip adduction. As a response, the femur will rotate medially underneath the patella which, in response, will rotate laterally elevating the stress in patellofrmoral compartment. A runner may develop ITB syndrome as a result of increased hip adduction[16]. Other possible compensations are; rearfoot eversion stressing the medial compartment of Achillies tendon, increased tibial adduction influencing the bending forces on tibia[17].
Key Points[edit | edit source]
- A stressing mechanical pattern associated with increased training volume (frequency) contribute to the possibility of injury
- When assessing running mechanics, follow a structured method to identify abnormalities
- Always look for obvious patterns. If a mechanical abnormality is not obvious then it's unlikely to contribute to the presented pathology
- Adjust training frequency initially to off-load the stressed tissue while addressing mechanics or building up tissue resilience.
- Addressing mechanical patterns by gait re-training will help lower the applied stress and can possibly allow runners to recover from injuries and progress beyond their pre-injury potentials
- If addressing mechanical problems wasn't enough to address the pathology, consider building up tissue tolerance to increase its ability to cope with the mechanics.
References[edit | edit source]
- ↑ Van Gent RN, Siem D, van Middelkoop M, Van Os AG, Bierma-Zeinstra SM, Koes BW. Incidence and determinants of lower extremity running injuries in long distance runners: a systematic review. British journal of sports medicine. 2007 Aug 1;41(8):469-80.
- ↑ Schreiber C, Becker J. Performance on the single-legged step down and running mechanics. Journal of Athletic Training. 2020 Dec 1;55(12):1277-84.
- ↑ Callahan LR, Sheon RP. Overview of running injuries of the lower extremity. UpToDate, Grayzel J.(Accessed on July 06, 2017). 2002.
- ↑ Francis P, Whatman C, Sheerin K, Hume P, Johnson MI. The Proportion of Lower Limb Running Injuries by Gender, Anatomical Location and Specific Pathology: A Systematic Review. J Sports Sci Med. 2019;18(1):21-31.
- ↑ Sheerin KR, Reid D, Besier TF. The measurement of tibial acceleration in runners—A review of the factors that can affect tibial acceleration during running and evidence-based guidelines for its use. Gait & Posture. 2019 Jan 1;67:12-24.
- ↑ Fredericson M, Misra AK. Epidemiology and aetiology of marathon running injuries. Sports Medicine. 2007 Apr 1;37(4-5):437-9.
- ↑ van Poppel D, Scholten-Peeters GGM, van Middelkoop M, Koes BW, Verhagen AP. Risk models for lower extremity injuries among short- and long distance runners: A prospective cohort study. Musculoskelet Sci Pract. 2018;36:48-53.
- ↑ Sanfilippo D, Beaudart C, Bruyère O, Kaux JF. What are the main risk factors for lower-extremity running-related injuries? A retrospective survey-based on 3669 respondents. British Journal of Sports Medicine. 2020;54(Suppl1):A138.
- ↑ Van der Worp MP, Ten Haaf DS, van Cingel R, de Wijer A, Nijhuis-van der Sanden MW, Staal JB. Injuries in runners; a systematic review on risk factors and sex differences. PLoS One. 2015 Feb 23;10(2):e0114937.
- ↑ Human Kinetics Europe. (2019). Training variables for running can lead to overuse injuries. [online] Available at: https://uk.humankinetics.com/blogs/excerpts/training-variables-for-running-can-lead-to-overuse-injuries [Accessed 7 Oct. 2019].
- ↑ 11.0 11.1 11.2 Souza RB. An evidence-based videotaped running biomechanics analysis. Physical medicine and rehabilitation clinics. 2016 Feb 1;27(1):217-36.
- ↑ How to get your running gait analysed. Available from: https://www.youtube.com/watch?v=gmBz3QC5JAg. [last access:06/10/2019]
- ↑ 13.0 13.1 13.2 Bramah C, Preece SJ, Gill N, Herrington L. Is there a pathological gait associated with common soft tissue running injuries?. The American journal of sports medicine. 2018 Oct;46(12):3023-31.
- ↑ van Oeveren BT, de Ruiter CJ, Beek PJ, van Dieën JH. The biomechanics of running and running styles: a synthesis. Sports biomechanics. 2021 Mar 6:1-39.
- ↑ Dierks TA, Manal KT, Hamill J, Davis I. Lower extremity kinematics in runners with patellofemoral pain during a prolonged run. Medicine and science in sports and exercise. 2011 Apr;43(4):693-700.
- ↑ Noehren B, Davis I, Hamill J. ASB Clinical Biomechanics Award Winner 2006: Prospective study of the biomechanical factors associated with iliotibial band syndrome. Clinical biomechanics. 2007 Nov 1;22(9):951-6.
- ↑ Milner CE, Hamill J, Davis IS. Distinct hip and rearfoot kinematics in female runners with a history of tibial stress fracture. journal of orthopaedic & sports physical therapy. 2010 Feb;40(2):59-66.
- ↑ How to get your running gait analysed. Available from: https://www.youtube.com/watch?v=AMi70SnTxa0 [last accessed:06/10/2019]