Principles of Load Management in Sport and Exercise Rehabilitation
Original Editor - Wanda van Niekerk based on the course by Lee Herrington
Top Contributors - Wanda van Niekerk, Jess Bell, Kim Jackson, Lucinda hampton and Aminat Abolade
Model of Injury Causation[edit | edit source]
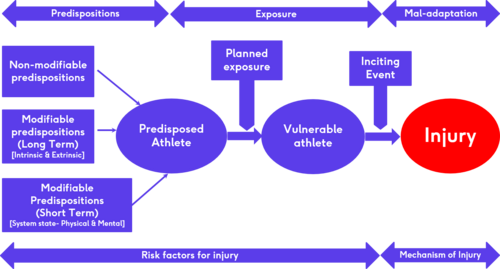
Several factors can predispose an athlete to injury. Some of these are non-modifiable predispositions (anatomy, genetics, previous injury, environmental factors) and some are modifiable predispositions. Modifiable predispositions can be long-term (training history, strength, movement, skill, flexibility) or short-term (state of the athlete, tired, mood, diet, etc.). No matter how predisposed an athlete is, they can only become injured when exposed to load. And there still needs to be an inciting event leading to the injury. This flow diagram by Dr Lee Herrington illustrates this point:
Read more here: Musculoskeletal Injury Risk Screening
Definition of Load[edit | edit source]
The International Olympic Committee defines load as follows[2]:
“The sport and non-sport burden (single or multiple physiological, psychological or mechanical stressors) as a stimulus that is applied to a human biological system (including subcellular elements, a single cell, tissues, one or multiple organ systems, or the individual). Load can be applied to the individual human biological system over varying time periods (seconds, minutes, hours to days, weeks, months and years) and with varying magnitude (ie, duration, frequency and intensity).”
Characteristics of Load[edit | edit source]
- Load is an external stimulus applied to an individual athlete that is measured independently of their internal characteristics[2]
- Exposure to load results in a physiological and psychological response
- Load can be applied to the whole system or whole body level or applied to the tissue level (system load vs tissue load)
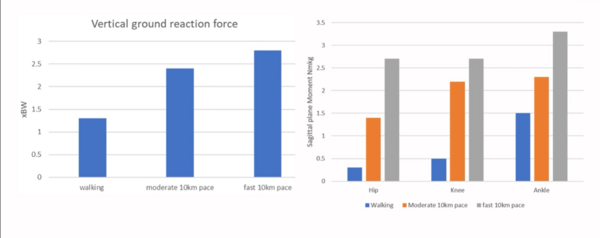
In sports injury rehabilitation, load application is often focused on applying load to the specific tissue that we wish to influence.[1] The following graphs explain the difference between system load and tissue load.[1]
The graph on the left depicts the amount of body weight (x BW) the body is exposed to in terms of vertical ground reaction force when walking, running at a moderate pace for 10km, and running at a fast pace for 10km. The load (vertical ground reaction force) going through the whole body (system load) increases steadily as the pace is increased.
When converting the load through specific areas of the body as in the graph on the right, it is clear that even though gravity is the same, the load expressed at different joints changes noticeably with pace.
- At the hip, as speed increases, a consistent increase in load or moment is seen.
- At the knee, as speed increases, there is a huge increase in load when changing from walking to moderate pace running. However, there is a relatively small increase in load when changing from moderate to fast pace running. Thus, the knee responds differently to the hip to a change in running pace.
- At the ankle, the level of load is higher, regardless of whether the task is walking or running. Like the hip, there is a more consistent relationship to changes in pace. However, the load through the ankle starts at a much higher baseline.
From this example, it is clear that even though gravity is the same (so the vertical load is the same), the way that load is expressed at different joints changes with pace. This shows that both system load and tissue load need to be considered when applying load in rehabilitation.
Identifying Load[edit | edit source]
- External load = features of training load describing magnitude and amount of physical work[3]
- Examples of external loads which could be captured:
- Training parameters such as time, distance, repetitions, nature of the load (absolute speeds, acceleration, deceleration, biomechanical moments)
- In sport itself – impact, nature of the skill, competition and the weight lifted
- Examples of external loads which could be captured:
- Internal load = features describing resultant physiological and biomechanical response to load[3]
- Examples of internal loads which could be captured:
- Things the athlete feels or expresses such as:
- Session Rate of Perceived Exertion (RPE)
- Wellness parameters:
- Mood, tiredness, sleep, readiness to train, soreness
- Physiological parameters
- Heart rate (recovery, variability, resting)
- Blood tests and results
- Things the athlete feels or expresses such as:
- Examples of internal loads which could be captured:
- Relationship between exposure (load) and consequence
- There is not necessarily a clear relationship between load, the load exposure and the consequence of that load. The consequences of load exposure vary considerably depending on the individual athlete and their previous experience with load.[1]
Is Load a Bad Thing?[edit | edit source]
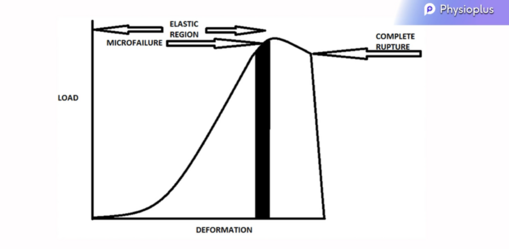
Load deformation curve
- Shows tissue deformation when a load is applied
- Initially, when a biological structure is loaded, the tissue deforms slowly and then more rapidly until it reaches the point of micro failure
- If the load is removed before this point of micro failure (elastic region), the tissue will return to its previous form
- If the tissue is loaded beyond the elastic region, there is a permanent change in the tissue
Implications of the load-deformation curve in injury or exercise rehabilitation
- If the aim is to create tissue adaptation and load tolerance (i.e. stronger and able to resist load), training or rehabilitation need to happen within the left half of the micro failure zone. This will cause enough damage to stimulate physiological processes which will allow for tissue adaptation.[5]
- If training and rehabilitation happen on the right half of the micro failure zone, too much damage occurs, which may lead to irreparable damage and breakdown.[1]
Load is a good thing, but can also be a bad thing
- Correct loading is necessary for the rehabilitation and strengthening of an athlete, but if too much is applied, it can have negative consequences.
- The "sweet spot" for loading needs to be determined
- Too little load = failure to provide appropriate stimulus to the tissue to adapt and strengthen and can lead to atrophy
- Too much load = irreparable tissue breakdown
What About Repetitive Load?[edit | edit source]
- High load might be protective[6]
- Sudden increases or changes in load might be the problem[6]
- When increases in load are ≥ 15% above the previous week’s load, injury risk escalates to between 21% - 49%
- To minimise injury risk, weekly training load increases should be limited to < 10%
- Read more: The training—injury prevention paradox: should athletes be training smarter and harder?[6]
- Acute:chronic workload ratio (ACWR)
- Acute:chronic workload ratio is the amount of training the athlete has completed during the period of rehabilitation compared with what is needed for a full training session.[8]
- Acute load is the training done in 1 week. Chronic load is the average acute load / training done in the last 4 weeks. The ratio between acute and chronic shows if the acute workload is greater or less than the total workload of the weeks before it.[8]
- Recently the ACWR has received criticism[9] [10][11] [12][13]
- Read more about the reasons why, here: The acute:chronic workload ratio. Science or religion?
- Biological systems versus local tissue
- One of the reasons why the ACWR has struggled to replicate itself across varied circumstances is that the measures quite often used to measure load, measure whole system load rather than tissue load and injury at a tissue level.[1]
- Load applied at the tissue level can be quite different than the load applied across the whole system.
- Using different metrics when loading at tissue level compared to the metrics used to measure loading at a system level is therefore recommended.[1]
- A recent systematic review investigating the relationship between ACWR and injury risk in sports reported high variability in studies. However, studies were generally of good quality, completed in multiple countries and included various sports. It did appear that using ACWR for external and internal loads may be related to injury risk. However, there are still issues with the ACWR method and this should be addressed through further research.[14]
Managing Rehabilitation Loads[edit | edit source]
- Collect data to base decisions on[1]
- Understand external load and the extent of external loads[1]
- Level of external load can be measured through:
- Body weight or multiples of body weight
- Weight lifted
- Global (system) level load can be calculated, but ideally, tissue level load should be understood
- Level of external load can be measured through:
- Research to improve our understanding on how typical tasks load tissue is growing
- Repetitions (and sets) or distance covered
- Consider the number of times the load is applied to the athlete
- Also consider the non-rehabilitation or non-sports load in athletes
- Work, activities of daily living (ADLs)
- Understanding these other loads is crucial to understanding the totality of an individual’s load
- Monitor the consequences of loading
- How does the tissue respond to load?
- Ways to measure this: read more here
- What is the global response to load?
Rehabilitation Process[edit | edit source]
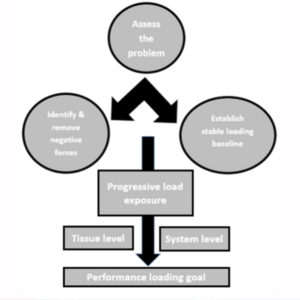
- Assess the extent of the problem
- Understand the current status
- Remove any negative forces
- Progressively expose system and tissue to load
- Reach performance goals
- Clinicians need to understand[1]:
- The extent of the loads an athlete is exposed to
- How does the athlete / tissue react to that load?
- Development of pain
- Development of stiffness
- Development of soreness
- Fatigue
- Less able to repeat effort the next day
- This will indicate if an athlete is adapting appropriately to rehabilitation or training loads
- Using data to understand knowledge and then act upon it[1]
Progression of Rehabilitation Loads[edit | edit source]
Example of Progressing Load for a Runner with Achilles Tendinopathy[edit | edit source]
The following example is from Lee Herrington's video on Principles of Load Management in Sport and Exercise Rehabilitation.[1]
Available Data on Achilles Loading[edit | edit source]
- Peak loads during running of x5-6 BW (Body Weight)[16][17]
- Trowell et al.[18] peak loads
- Ankle bounces < running
- Bounding = running
- A-skips > running
- Trowell et al.[18] compared plantarflexor musculotendon unit (MTU) output between plyometric exercises and running. The results included:
- "Ankle bounce produced low gastrocnemius and soleus MTU output compared to running."[18]
- "One A-skip generated greater total positive and negative work for both plantarflexors compared to one running stride and each A-skip cycle involved twice the number of ground contacts and toe-off phases as one running stride, thus increasing total work for the plantarflexors."[18]
- The researchers concluded the following[18]:
- Ankle bounce and A-skip produced low MTU output for gastrocnemius and soleus compared to running. This may suggest that these two exercises can be used as alternatives to running if low plantarflexor loads are needed.[18]
- Bounding produced greater peak strain compared to running and may be used in runners who need to train or rehabilitate with high eccentric loads[18]
- Hurdle jumps may be used in runners who need soleus overload, with low lateral gastrocnemius loads.[18]
- Baxter et al.[16] peak loads
- Seated heel raise x 0.5 BW
- Single leg squat x 1 BW
- Standing heel raise x 2 BW
- Forward hop x 5 BW
- Single leg drop jump x 5.5 BW
| Tier | Exercise | Loading Peak (BW) |
|---|---|---|
| Tier 1 | Seated heel raise (2-leg) | 0.5 ± 0.2 |
| Seated heel raise (1-leg) | 0.7 ± 0.2 | |
| Squat | 1.1 ± 0.3 | |
| Low step up (leading leg) | 1.6 ± 0.4 | |
| High step up (leading leg) | 1.8 ± 0.3 | |
| Standing heel raise | 1.6 ± 0.2 | |
| Tier 2 | Rebounding heel raise (2-leg) | 2.5 ± 0.7 |
| Lunge (leading leg) | 2.1 ± 0.6 | |
| Low step down (leading leg) | 2.2 ± 0.5 | |
| Low step up (trailing leg) | 2.9 ± 0.4 | |
| High step down (trailing leg) | 2.6 ± 0.3 | |
| Walk (stance) | 3.3 ± 0.3 | |
| Low step down (trailing leg) | 2.9 ± 0.3 | |
| Forward jump (2-leg) | 3.2 ± 1.0 | |
| High step down (leading leg) | 3.2 ±0.6 | |
| High step up (trailing leg) | 3.7 ± 0.6 | |
| Lunge (trailing leg) | 2.4 ± 0.5 | |
| Counter movement jump (2-leg) | 3.4 ±0.3 | |
| Rebounding heel raise | 4.2 ± 0.9 | |
| Standing heel raise (1-leg) | 3.0 ± 0.3 | |
| Tier 3 | Drop jump (2-leg) | 3.6 ± 0.6 |
| Hopping (2-leg) | 4.8 ± 1.8 | |
| Run (stance) | 5.2 ± 0.9 | |
| Forward hopping (2-leg) | 5.2 ± 2.6 | |
| Counter movement jump (1-leg) | 4.9 ± 0.6 | |
| Forward jump (1-leg) | 5.4 ± 1.1 | |
| Tier 4 | Hopping (1-leg) | 6.7 ± 1.8 |
| Drop jump (1 -leg) | 5.5 ± 0.8 | |
| Lateral hopping (1-leg) | 7.3 ± 2.4 | |
| Forward hopping (1-leg) | 7.3 ± 1.9 |
Requirements of the Patient for Running[edit | edit source]
- Typically runs 25 – 30 km per week (6 – 10 km each run), runs 3 -4x week
- Best 10 km time 48 minutes, trains at 5min/km pace
- Typical running cadence 170 steps/min
- Aerobic exercise target heart rate 120 beats/min
- Main reason for running:
- Health (mental and physical)
- Weight management
Baseline Data[edit | edit source]
- Pain after running greater than 2km post-run and the next morning
- Pain limits standing heel raise to 18 repetitions, but is able to do 28 on the other leg
- Able to bilateral ankle bounce 10 times with no pain
Managing and Progressing Tissue Load[edit | edit source]
Peak Load Exposure[edit | edit source]
- For Achilles tendon during running, data indicates 5-6BW
- Peak load exposure – progression
- Continue with 2 km running
- Build ability to tolerate load
- Ankle bounces
- Bounding
- A-skips
Volume of Exposure[edit | edit source]
- Incrementally increase running volume / distance from 2 km
- Monitor the effect of this increase
- Morning stiffness and soreness
- Knee to wall test
- Calf raises
Managing and Progressing System Load[edit | edit source]
Aerobic Fitness[edit | edit source]
- Provide an alternate stimulus if running is not enough, such as an exercise bike, or combine with the current run load tolerance of the athlete
- Training at heart rate (HR) of 120 beats/minute - aim to do bike workout at same intensity
- Still providing the athlete with weight management and mental health stimulus through different forms of exercise
Key Take Home Messages[edit | edit source]
- Understand the performance requirements
- Identify what load the tissue (and individual) can currently tolerate
- Identify the gap between current status and performance requirements
- Progressively apply the maximum loads the tissue (and individual) can tolerate towards overall performance requirements
- Assess the impact of loading on the tissue and the individual
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 Herrington, L. Principles of Load Management in Sport and Exercise Rehabilitation. Plus , Course. 2022
- ↑ 2.0 2.1 Soligard T, Schwellnus M, Alonso JM, Bahr R, Clarsen B, Dijkstra HP, Gabbett T, Gleeson M, Hägglund M, Hutchinson MR, Van Rensburg CJ. How much is too much?(Part 1) International Olympic Committee consensus statement on load in sport and risk of injury. British journal of sports medicine. 2016 Sep 1;50(17):1030-41.
- ↑ 3.0 3.1 Impellizzeri FM, Marcora SM, Coutts AJ. Internal and external training load: 15 years on. International journal of sports physiology and performance. 2019 Feb 1;14(2):270-3.
- ↑ Andrew Wiseman. Internal and External Training Load: 15 Years On. Available from: https://www.youtube.com/watch?v=suukV0POxqog [last accessed 01/08/2022]
- ↑ 5.0 5.1 Herrington, L, Spencer, S. Principles of Exercise Rehabilitation. In Petty NJ, Barnard K, editors. Principles of musculoskeletal treatment and management e-book: a handbook for therapists. Elsevier Health Sciences; 2017 Jun 28.
- ↑ 6.0 6.1 6.2 Gabbett TJ. The training—injury prevention paradox: should athletes be training smarter and harder?. British journal of sports medicine. 2016 Mar 1;50(5):273-80.
- ↑ Tim Gabbett. RESEARCH VLOG #6: Train Smarter and Harder. Available from: https://www.youtube.com/watch?v=I_FVqXZ9DBk [last accessed 1/08/2022]
- ↑ 8.0 8.1 8.2 8.3 Blanch P, Gabbett TJ. Has the athlete trained enough to return to play safely? The acute: chronic workload ratio permits clinicians to quantify a player's risk of subsequent injury. British journal of sports medicine. 2016 Apr 1;50(8):471-5.
- ↑ Buchheit M. Applying the acute: chronic workload ratio in elite football: worth the effort?. British Journal of Sports Medicine. 2017 Sep 1;51(18):1325-7.
- ↑ Williams S, West S, Cross MJ, Stokes KA. Better way to determine the acute: chronic workload ratio?. British Journal of Sports Medicine. 2017 Feb 1;51(3):209-10.
- ↑ Lolli L, Batterham AM, Hawkins R, Kelly DM, Strudwick AJ, Thorpe R, Gregson W, Atkinson G. Mathematical coupling causes spurious correlation within the conventional acute-to-chronic workload ratio calculations. British journal of sports medicine. 2019 Aug 1;53(15):921-2.
- ↑ Wang C, Vargas JT, Stokes T, Steele R, Shrier I. Analyzing activity and injury: lessons learned from the acute: chronic workload ratio. Sports Medicine. 2020 Jul;50(7):1243-54.
- ↑ Impellizzeri FM, Tenan MS, Kempton T, Novak A, Coutts AJ. Acute: chronic workload ratio: conceptual issues and fundamental pitfalls. International journal of sports physiology and performance. 2020 Jun 5;15(6):907-13.
- ↑ Maupin D, Schram B, Canetti E, Orr R. The relationship between acute: chronic workload ratios and injury risk in sports: a systematic review. Open access journal of sports medicine. 2020;11:51.
- ↑ Van Rossom S, Smith CR, Thelen DG, Vanwanseele B, Van Assche D, Jonkers I. Knee joint loading in healthy adults during functional exercises: implications for rehabilitation guidelines. journal of orthopaedic & sports physical therapy. 2018 Mar;48(3):162-73.
- ↑ 16.0 16.1 16.2 16.3 Baxter JR, Corrigan P, Hullfish TJ, O'Rourke PA, Silbernagel KG. Exercise Progression to Incrementally Load the Achilles Tendon. Medicine and Science in Sports and Exercise. 2021 Jan 1;53(1):124-30.
- ↑ Starbuck C, Bramah C, Herrington L, Jones R. The effect of speed on Achilles tendon forces and patellofemoral joint stresses in high‐performing endurance runners. Scandinavian Journal of Medicine & Science in Sports. 2021 Aug;31(8):1657-65.
- ↑ 18.0 18.1 18.2 18.3 18.4 18.5 18.6 18.7 Trowell D, Fox A, Saunders N, Vicenzino B, Bonacci J. A comparison of plantarflexor musculotendon unit output between plyometric exercises and running. Journal of Science and Medicine in Sport. 2022 Apr 1;25(4):334-9.
- ↑ Health and High Performance. Runners: Choosing plyometric exercises to target the calf muscles. Available from: https://www.youtube.com/shorts/m4cZ--UwUsE [last accessed 1/08/2022]