Prescription Drug Abuse
Original Editors - Lauren Cotton & Erin Smith from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Erin Smith, Lauren Cotton, Lucinda hampton, Admin, Elaine Lonnemann, Kim Jackson, 127.0.0.1, WikiSysop, Wendy Walker and Lauren Lopez
Introduction[edit | edit source]
Prescription drug abuse occurs when someone uses a prescribed medication for purposes other than what it was intended for, use more than the dose prescribed by the physician, or continue prolonged use after the amount prescribed by the physician was taken[1]. Drug abuse may become ongoing and compulsive, despite the negative consequences.
An increasing problem, prescription drug abuse can affect all age groups, including teens. The prescription drugs most often abused include opioid painkillers, anti-anxiety medications, sedatives and stimulants. Early identification of prescription drug abuse and early intervention may prevent the problem from turning into an addiction.[2]
Epidemiolgy[edit | edit source]
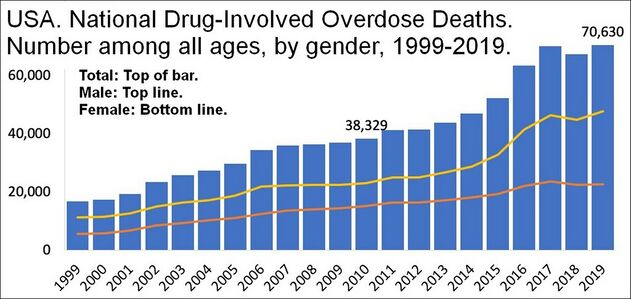
Abuse of prescription drugs has reached an epidemic level
- More than 16.7 million people age 12 and older in the United States abused prescription drugs in 2012, with approximately 2.1 million people meeting criteria for a diagnosis of a substance use disorder related to prescription drugs.[3]
- In Australia, in 2019, an estimated 900,000 people (4.2%) aged 14 and over used a pharmaceutical drug for non-medical purposes in the previous 12 months[4]
- Prescription drugs are the most commonly abused substances by teens after marijuana, synthetic marijuana (spice), and alcohol[5].
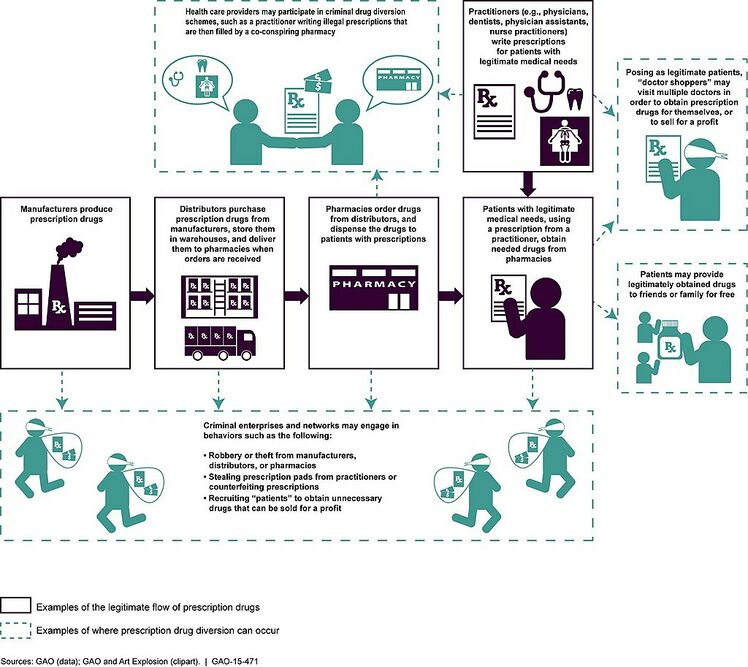
Obtaining[edit | edit source]
Some prescription drug addicts start with legitimate prescribed for them. eg A patient needing pain medication after surgery. When patients take their medications in ways that go beyond their doctors’ instructions, tolerance and eventual addiction can be the result.
Others become addicted to prescription drugs without ever legally obtaining a prescription. They either buy the drugs on the street, purchase them online, or steal them. Unfortunately, the black market for prescription medications is now growing at an alarming rate. People use them because they are cheap and easy to get.[6]
Characteristics/Clinical Presentation[edit | edit source]
Signs that go along with prescription drug addiction. These are:
- A tendency to visit doctors frequently
- A tendency to shop online for prescription drugs
- Regular complaints about medical conditions that would justify drug use
- A gradual drop-off in school or work performance
- And increasing disinterest in personal appearance
- A tendency toward defensiveness when talking about prescription medications[6].
Signs and symptoms of prescription drug abuse depend on the specific drug. Because of their mind-altering properties, the most commonly abused prescription drugs are:
| Opioids | Anti-anxiety medications and sedatives | Stimulants |
|---|---|---|
|
|
|
Dangers[edit | edit source]
The dangers that go along with prescription drug addiction are very similar to other addictions. Addictive prescription medications have adverse effects on the physical body that directly correlate with the kind of drug being used.
A hidden danger inherent to prescription drugs is the misplaced belief that they are completely safe because doctors prescribe them. What must be understood is that these drugs are classified as prescription only specifically because they are addictive and/or dangerous. The very fact that they are only obtainable through prescription should tell you something. Do not believe the myth that they are less harmful or less powerful.[5]
Physical Therapy Management[edit | edit source]
Physical therapists are not qualified to treat prescription drug abuse, but that does not mean that this is a problem PTs should ignore. An important part PTs can play is in recognising the signs and symptoms, screening a patient when a problem is suspected, and making sure to ask each patient about all drugs, prescription and over the counter, that they are currently taking.
If you suspect a client has an addiction to prescription drugs advice them to seek help, beginning with them talking with their doctor. They may feel embarrassed to talk about it, but remind them that medical professionals are trained to help, not judge. It's easier to tackle the problem early before it becomes an addiction and leads to more-serious problems[2].
References[edit | edit source]
see adding references tutorial.
- ↑ Mayo Clinic. Prescription Drug Abuse. http://www.mayoclinic.com/print/prescription-drug-abuse/DS01079/METHOD=print&DSECTION=all (accessed 15 March 2012).
- ↑ 2.0 2.1 2.2 Mayoclinic Prescription drug abuse Available:https://www.mayoclinic.org/diseases-conditions/prescription-drug-abuse/symptoms-causes/syc-20376813 (accessed 10.4.2022)
- ↑ McHugh RK, Nielsen S, Weiss RD. Prescription drug abuse: from epidemiology to public policy. Journal of substance abuse treatment. 2015 Jan 1;48(1):1-7.Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4250400/ (accessed 10.4.2022)
- ↑ AIHW Available: Illicit drug use https://www.aihw.gov.au/reports/australias-health/illicit-drug-use (accessed 10.4.2022)
- ↑ 5.0 5.1 Get smart about drugs Prescription Drug Abuse Available: https://www.getsmartaboutdrugs.gov/content/prescription-drug-abuse (accessed 10.4.2022)
- ↑ 6.0 6.1 UK Addiction treatment centre Prescription Drug Addiction and Abuse Available: https://www.ukat.co.uk/prescription-drug-addiction/ (accessed 10.4.2022)