Moebius Syndrome
Original Editor - Wendy Walker
- Top Contributors - Wendy Walker, Kim Jackson, WikiSysop, Rishika Babburu, Tony Lowe, Evan Thomas, Tarina van der Stockt and Daniele Barilla
Definition/Description[edit | edit source]
Moebius, or Möbius, syndrome is defined as congenital facial palsy combined with abnormal ocular abduction, caused by abnormal development of the 6th and 7th cranial nerves. It is a rare congenital condition that was first described by German neurologist Paul Julius Möbius in 1888[1], with a further report in 1892[2].
In 2007 a group of researchers and clinicians specialising in this syndrome proposed the following definition of Moebius Syndrome: "Congenital, uni- or bilateral, nonprogressive facial weakness and limited abduction of the eye(s)"[3]. The diagnosis is made based on clinical criteria.
These 2 clinical criteria are commonly used to make the diagnosis:
- Congenital (ie. present from birth) non-progressive congenital facial weakness
- Inability to abduct (move the eye away from the nose/centre of the face) one or both eyes
Both criteria must be fulfilled for a diagnosis of Moebius Syndrome to be made. These symptoms are due to impairment in the 7th and 6th cranial nerves.
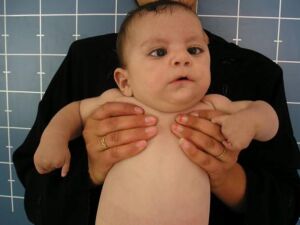
The most common description of the face of an individual with Moebius syndrome is "mask-like" as there is no activity of the muscles of facial expression, hence no smile or frown.
Moebius syndrome occurs due to the loss of function of motor cranial nerves. Most cases are diagnosed during infancy.
Clinically Relevant Anatomy[edit | edit source]
Please see the Facial Nerve and Facial Palsy pages for information on the anatomy of the seventh cranial nerve, AKA facial nerve.
Cranial nerve six, AKA the abducens nerve, innervates the ipsilateral lateral rectus muscle which abducts the ipsilateral eye.
The sixth nerve nucleus is located in the pons, just ventral to the floor of the fourth ventricle. Bilateral palsy of the abducens nerve (as seen in Moebius Syndrome) results in lack of eye movement in the horizontal plane, ie. inability to move the eyes laterally. This can be observed by testing lateral tracking of eye movement (keeping the head still) and also when the individual reads text, it is apparent that they have to move their head laterally.
Most individuals with Moebius Syndrome have bilateral signs, but occasionally it occurs on one side only, ie. unilateral.
Mechanism of Injury / Pathological Process[edit | edit source]
The etiology of Moebius Syndrome is not known, but it appears to be multifactorial. There has been evidence of a genetic component related to various loci on chromosomes 3, 10, and 13[4], but this is not the case for many individuals with Moebius Syndrome.
The close relationship embryologically between the motor nuclei of the sixth and seventh cranial nerves explains the pathology of this rare condition[5].
Equal risk between boys and girls. Thought to be increased risk if one of parents has Moebius Syndrome.
MRI investigations show absence of both the Facial Nerves and the Abducens Nerves in some individuals with this diagnosis[6][7], however this is not the case in the majority of cases.
Epidemiology[edit | edit source]
In 2007, the Moebius Syndrome Foundation estimated that there were at the time a total of approximately 2,000 cases of Moebius Syndrome worldwide[8].
A Dutch survey, in 2003, showed a prevalence for Moebius Syndrome of 0.002% of the population[9].
Clinical Presentation[edit | edit source]
Cranial Nerve VII Involvement[edit | edit source]
Bilateral facial immobility/paralysis is the most noticeable symptom, and is frequently noticed very soon after birth, with the parents reporting incomplete eyelid closure during sleep and difficulty sucking (due to lack of lip seal)[10].
However, occasionally the facial paralysis is not noticed for a few weeks or months, until the baby's inability to smile or the lack of facial movement with crying arouses the parents' concern. In extremely rare cases the facial paralysis is unilateral.
As the child grows, speech problems emerge due to inability to seal the lips for thee labial consonants. Speech problems are reported in 76-90% of patients with Möbius syndrome[11].
Cranial Nerve VI Involvement[edit | edit source]
Abducens nerve palsies are reported in approximately 75% of patients and are some of the most characteristic features of the syndrome.
Cranial Nerve XII Involvement[edit | edit source]
The hypoglossal nerve is the third most commonly affected cranial nerve (CN) and is involved in approximately 25% of reported cases[12]. Involvement of the hypoglossal nerves often leads to atrophy of the tongue. Patients may be unable to protrude their tongue beyond their lips because of this weakness. This involvement may result in paralysis and hypoplasia of the tongue, or fasciculations may be seen as a result of hypoglossal denervation. The ocular muscles are always involved when the tongue is affected.
Brachial Malformation[edit | edit source]
Brachial malformation is common and can involve the following:
Talipes Equinovarus AKA Clubfoot, frequently bilateral, occurs in almost one third of patients
Reports include hand malformations or congenital amputation of hand
In some cases of unilateral syndrome, the affected hand is smaller than the other hand (this is known as brachydactyly
Other abnormalities in the upper extremities include syndactyly (finger webbing) and an absence or hypoplasia of the radius, ulna, metacarpal, or digit
Motor Delay[edit | edit source]
Many children with this syndrome have some motor delay during infancy, although this is usually resolved after the first few years of life. One large Italian study[7] published in 2016, found that these children often "exhibit development characterized by global delay at 1 year of age, motor, emotional and speech difficulties at 2 years of age, a trend toward normalization at 3 years of age but with weakness in hand-eye coordination, and finally achieving average results at 5 years of age."
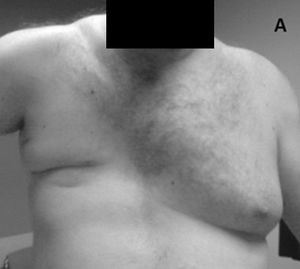
Poland Sequence[edit | edit source]
A congenital condition called the Poland sequence, characterized by ipsilateral hand malformations and by partial or complete absence of the pectoralis muscles and breast, occurs with Möbius syndrome in approximately 15% of patients[13].
Other problems[edit | edit source]
A number of individuals with Moebius Syndrome have been found to have missing (or incompletely developed) trunk muscles ; most often the trapezius and pectoral muscles, but other muscles which can be involved are serratus anterior, latissimus dorsi, abdominal & intercostal muscles.
Möbius syndrome has been associated with autistic behavior. Studies suggest that autistic symptoms are present in 30-40% of children and young adults with Möbius syndrome[14][15].
The patient’s intelligence is usually normal, but mild mental retardation is thought to occur in approximately 10-15% of patients[16].
Diagnostic Procedures[edit | edit source]
No diagnostic laboratory studies yield findings specific to Moebius syndrome.
The diagnosis is usually made using the most commonly accepted definition: the typical phenotypic appearance is an immobile facial appearance with various gaze palsies.
Electromyography can be used to help determine whether a patient’s symptoms stem from birth trama and are therefore NOT associated with Moebius syndrome.
CT scanning or MRI of the brain may demonstrate bilateral calcifications in the regions of the CN VI nuclei[17], but this is not true for all cases of Moebius syndrome.
Management / Interventions[edit | edit source]
No definitive treatment is available, with medical care being supportive and symptomatic.
In early infancy special bottles or even feeding tube may be required due to lack of lip seal.
Treatment for corneal ulcerations or abrasions may be required. These occur secondary to keratitis and conjunctivitis, which result from incomplete eyelid closure.
Surgery may be considered in order to try and provide the ability to smile; however, the results are limited and movement can be restored along only 1 vector.
Most frequently, the reconstructive surgery involves free-tissue transfers with bilateral gracilis muscles anastomosed to the masseter nerves on both sides in order to achieve a small smile[18][19].
Physiotherapy[edit | edit source]
The main areas requiring physiotherapy intervention are the bilateral facial palsy, and also techniques to address bilateral talipes equinas in children with this condition. Early in infancy, children with Moebius Syndrome may have mild motor delay, so paediatric physiotherapists may be able to provide advice on management.
- Motor Delay - general paediatric physiotherapy interventions can be utilised to educate the parents on how to help the child with motor delay. It is notable that in Moebius Syndrome motor delay, if present at all, is likely to be very mild, so often no specific intervention is indicated.
- Facial Palsy - physiotherapy techniques aimed at improving facial movements are indicated for the majority of individuals with Moebius Syndrome. More details are on the Facial Palsy page. Techniques include: neuromuscular reeducation, Trophic Electrical Stimulation, EMG biofeedback. Many of these children go on to have surgical interventions as the degree of facial palsy is frequently severe, and the response to conservative/physiotherapy interventions is often limited.
- Talipes Equinas, AKA Clubfoot - physiotherapy interventions are indicated for all children with this condition. In some cases, the response to conservative measures may be insufficient, so surgical intervention may be required. Please see the following pages for management of clubfoot: Assessing children with clubfoot, Management of clubfoot, Multidisciplinary team in managing clubfoot.
Differential Diagnosis[edit | edit source]
Abducens (CN VI) nerve palsy
Congenital facial (CNVII) nerve palsy
Brainstem syndromes
Metabolic neuropathy
Myotonic diseases
Neuromuscular diseases
Congenital neuropathies
Congenital muscular dystrophy
Duane syndrome
Kallmann syndrome
Poland anomaly
Klippel-Feil anomaly
Resources[edit | edit source]
http://www.moebiussyndrome.com/ USA organisation
http://www.moebiusresearchtrust.org/projects-1/ Scottish organisation
http://www.facialpalsy.org.uk/about-facial-palsy/causes-diagnoses/developmental/moebius-syndrome/275 A useful, concise summary of Moebius syndrome on a general UK facial palsy website
References[edit | edit source]
- ↑ Mobius PJ. Uber angeboren doppelseitige abducens-facialis-lahmung. Munchen Medizinische Wochenschrift. 1888;35:91-4.
- ↑ Mobius PJ. Uber infantilen kernschwund. Munchen Medizinische Wochenschrift. 1892. 39:17-21, 41-3, 55-8
- ↑ Miller, G. Neurological disorders. The mystery of the missing smile. Science. 2007 May 11;316(5826):826-7.
- ↑ Uzumcu A, Karaman B, Toksoy G, Uyguner ZO, Candan S, Eris H. Molecular genetic screening of MBS1 locus on chromosome 13 for microdeletions and exclusion of FGF9, GSH1 and CDX2 as causative genes in patients with Moebius syndrome. Eur J Med Genet. Sep-Oct 2009;52(5):315-20
- ↑ May M, Schaitkin BM. Facial Nerve Disorders in Newborns and Children. In: The Facial Nerve. 2nd ed. New York, NY: Thieme New York; 2000:339-65
- ↑ Kim N, Kim JH, Kim JS, Hwang JM. Möbius syndrome: clinico-radiologic correlation. Send to Graefes Arch Clin Exp Ophthalmol. 2018 Aug 1. doi: 10.1007/s00417-018-4089-3. [Epub ahead of print]
- ↑ 7.0 7.1 Picciolini, O., Porro, M., Cattaneo, E. et al. Moebius syndrome: clinical features, diagnosis, management and early intervention. Ital J Pediatr 42, 56 (2016). https://doi.org/10.1186/s13052-016-0256-5
- ↑ Broussard AB, Borazjani JG. The faces of Moebius syndrome. Am J Matern Child Nurs. Sept/Oct, 2008. 33(5):272-278.
- ↑ Verzijl HT, van der Zwaag B, Cruysberg JR, Padberg GW. Möbius syndrome redefined: a syndrome of rhombencephalic maldevelopment. Neurology. 2003 Aug 12. 61(3):327-33
- ↑ Kumar D. Moebius syndrome. J Med Genet. Feb 1990;27(2):122-6
- ↑ Briegel W. Neuropsychiatric findings of Mobius sequence -- a review. Clin Genet. Aug 2006;70(2):91-7
- ↑ Kumar D. Moebius syndrome. J Med Genet. Feb 1990;27(2):122-6
- ↑ Sugarman GI, Stark HH. Mobius syndrome with Poland's anomaly. J Med Genet. 1973;10(2):192-6
- ↑ Gillberg C, Steffenburg S. Autistic behaviour in Moebius syndrome. Acta Paediatr Scand. Mar 1989;78(2):314-6.
- ↑ Johansson M, Wentz E, Fernell E, Strömland K, Miller MT, Gillberg C. Autistic spectrum disorders in Möbius sequence: a comprehensive study of 25 individuals. Dev Med Child Neurol. May 2001;43(5):338-45
- ↑ Verzijl HT, van Es N, Berger HJ, Padberg GW, van Spaendonck KP. Cognitive evaluation in adult patients with Möbius syndrome. J Neurol. Feb 2005;252(2):202-7
- ↑ Dooley JM, Stewart WA, Hayden JD, Therrien A. Brainstem calcification in Möbius syndrome. Pediatr Neurol. Jan 2004;30(1):39-41
- ↑ Marre D, Hontanilla B. Brain plasticity in Möbius syndrome after unilateral muscle transfer. Ann Plast Surg. 2011
- ↑ Vila PM, Kallogjeri D, Yaeger LH, Chi JJ. Powering the Gracilis for Facial Reanimation: A Systematic Review and Meta-analysis of Outcomes Based on Donor Nerve. JAMA Otolaryngol Head Neck Surg. 2020;146(5):429–436. doi:10.1001/jamaoto.2020.0065