Introduction to Clubfoot
Original Editor - Thomas Maeseele
Top Contributors - Naomi O'Reilly, Kudzanayi Ronald Muzenda, Kim Jackson, Rachael Lowe, Evan Thomas, Admin, 127.0.0.1, Thomas Maeseele, Esraa Mohamed Abdullzaher, WikiSysop, Simisola Ajeyalemi, Robin Tacchetti, Tony Lowe, Rucha Gadgil and Meaghan Rieke
Introduction[edit | edit source]
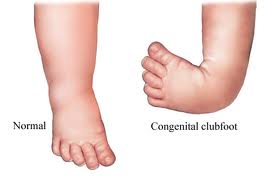
Clubfoot, also known as Congenital Talipes Equinovarus, is a complex, congenital deformity of the foot, that left untreated can limit a person’s mobility by making it difficult and painful to walk. [1] It is defined as a deformity characterized by complex, malalignment of the foot involving soft and bony structures in the hindfoot, midfoot and forefoot. [2] The deformity affects the structure and position of the foot, presenting as an adductus and cavus (an inward turning) of the midfoot and a varus hindfoot. At the subtalar joint, the foot is held in a fixed equinus, or downward pointing position[3]. The foot affected by clubfoot is shorter, and the calf circumference is less than a normal, unaffected foot[3]. On presentation, the clubfoot deformity is not passively correctable and presents with varying degrees of rigidity[4].
Clubfoot may be unilateral (30%-40%) one or bilateral (60%-70%). It is twice as common in males than females.[5] It is the most common congenital malformation of the foot affecting 1-2 newborns per 1000.[6] Most often it is an isolated abnormality, but occasionally it is associated with other congenital malformations or syndromes.
Talipes Equinovarus comes from the following: [7]
- “Tali” means Ankle,
- “Pes” means Foot
- “Equinus” means foot pointing down (like a horse’s foot)
- “Varus” means deviated towards midline
Global Burden of Clubfoot[edit | edit source]
If clubfoot is not treated or managed successfully, it can progress to a severe deformity causing lifelong impairment affecting participation in activities of daily living. As the child grows and puts weight on their feet they will bear weight through the sides, or even the tops of their feet. A large callus of thickened skin forms on the weight-bearing surface and the deformed position causes pain and leaves the feet open to injury and infection.
In an adult, this often means the individual is unable be able to wear normal footwear with most cases experiencing severe restriction in walking by the time they are in their 20's or 30's with visible deformity of the foot. This, in turn, often leads to discrimination and the inability to access education and employment, which further impacts the individual's capacity to contribute economically which may affect both the individual and their family members.
It is estimated that 80% of cases of clubfoot occur in Low and Middle Income Countries[8] . Lack of resources and medical services in these countries mean that there are high levels of disability from potentially treatable congenital anomalies such as clubfoot (Kushner et al, 2010; WHO, 2007). Many children born with clubfoot in Low and Middle Income Countries do not receive any treatment[8].
Untreated, the clubfoot deformity progresses to become a ‘Neglected Clubfoot’ as the child with clubfoot eventually begins to walk. Due to the position of the foot the child weight-bears through the lateral and dorsal side of the affected foot, where a large bursa and callous form. As the child continues to walk the soft and bony tissues are stretched further and the deformity worsens resulting in pain and reduced mobility[8]. The consequences of the clubfoot deformity can have a great impact on the life of an individual. In some countries girls with clubfoot may be less likely to marry[9], in others, the deformity is viewed by sectors of society as being the result of a curse[10]. Lack of mobility is extremely disabling in environments with poor transport infrastructure and where agriculture is the main source of income[8].
Treatment of clubfoot in Low and Middle Income Countries is a challenge; large numbers of children and adults with neglected clubfoot observed by surgeons visiting Low and Middle Income Countries are indicative of the scale of the problem[8]. The current state of services for clubfoot in most Low and Middle Income Countries is not well documented. However, it has been reported that in some countries, the predominant treatment option being offered is the Kite Method, as in Brazil (Lourenco, 2007). In others, such as Malawi prior to 2007 there are almost no services for clubfoot and no unified, nationwide approach to clubfoot management[10]. Lack of services and belief that clubfoot is due to fate or is not treatable also mean that parents often do not seek treatment for their children[10].
Epidemiology[edit | edit source]
Clubfoot is more common in males with a 2.5 to 2.8:1 Male:Female ratio.[11] Various incidences have been noted between countries and regions ranging from 1-1.50 per 1000 live births, rising up to 3 per 1000 live births.[11][12][13] Similarly, ethnic differences in occurrence have been reported with the lowest incidence (0.6%) among the Chinese Population, while the highest incidence (6.8%) in the Polynesian Region. The accumulative incidence is approximately 1 per 1000 live births among Caucasians.[14] Worldwide 80% of children born with clubfoot are in low-and middle-income countries. [7]
Etiology[edit | edit source]
In approximately 80% of cases, clubfoot is idiopathic. The remaining 20% present in association with other disorders, most commonly Spina Bifida, Cerebral Palsy and Arthrogryposis[4]. Incidence of clubfoot varies globally from an estimated 0.39/1000 live births in the Chinese, 1-2/1000 in Caucasians and may be as high as 7-8/1000 in Polynesians[3][15]. Birth prevalence has been reported as varying between 0.51 and 2.03/1000 live births in LMICs.[16].
The causes of clubfoot are poorly understood[17]. There is almost certainly a genetic component[3] and environmental factors, seasonal variation and in utero positioning have all been suggested as possible causal factors but these have not been consistently demonstrated[17]. In some countries and cultures there are different beliefs about what causes a child to be born with clubfoot. These include include spiritual influences, spells, or curses often leading to mothers being blamed for the deformity. These ideas can cause the child with clubfoot to be excluded from society, so therefore it is important to explain to families that children with clubfoot are a valuable part of the community. [7]
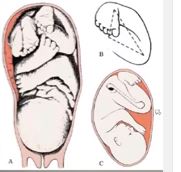
Several theories have been proposed to explain the origin of clubfoot, considering both intrinsic and extrinsic causes, including: intrauterine position of the foetus, mechanical compression or increased hydraulic pressure, interruption in foetal development, viral infections, vascular deficiencies, muscular alterations, neurological alterations, defect in the development of the bones structures and genetic defects.[2][18] Researchers believe there are both genetic and environmental influences.
The following theories have been reported[14][18] but are unproven and should not be considered as genuine causes:
- Neurogenic Theory - Reduced motor unit, which counts in the distribution of the common peroneal nerve, may be responsible for clinically demonstrable muscle weakness.[14]
- Myogenic Theory - Suggested by the presence of anomalous muscles, e.g. accessory soleus muscle and flexor digitorum accessorious longus muscles, which can produce equinovarus deformity.[14][18]
- Vascular Theory - Diminution of blood flow in the anterior tibial artery and its derivatives.[14][18]
- Embyonic Theory - Developmental defect occurring up to 12 weeks of intrauterine life.[18]
- Chromosonal Theory - Presence of some chromosonal defects in unfertilized germ cells.[14][18]
- Osteogenic Theory - Due to some unknown cause, temporary arrest of development occurs in the 7- to 8- week-old embryo, which can lead to clubfoot or other deformities.[14][18]
- Mechanical Block Theory - Due to some mechanical obstruction during the intrauterine development period, e.g. intrauterine fibrotic bands, less amniotic fluid, disproportionate uterine cavity, etc, talipes equinovarus can occur.[18]
Clinically Relevant Anatomy & Clinical Presentation[edit | edit source]
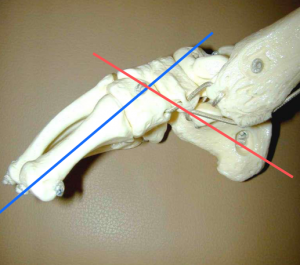
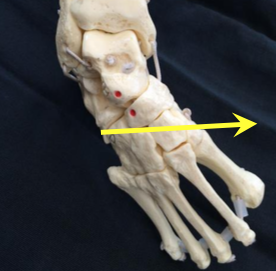
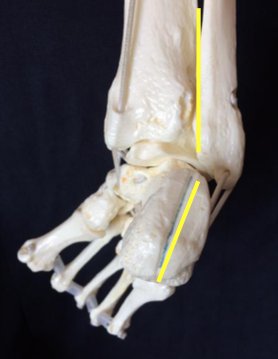
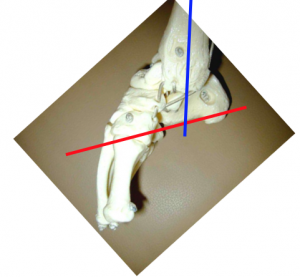
The foot consists of 26 bones. Most relevant for this congenital deformity are the Talus, Calcaneus and Navicular. The underlying deformity of clubfoot can be most easily understood if it is divided into four components, whose first letters make up the word CAVE. These components are: Cavus, Adductus, Varus, and Equinus. The Cavus and Adductus deformities occur in the midfoot, while the Varus and Equinus deformities occur in the hindfoot.[7]
- Cavus in the midfoot is the first part of the deformity of clubfoot. The arch of the foot is higher than normal.as a result of the first metatarsal being plantarflexed in relation to the calcaneum and hindfoot. [7]
- Adductus is movement towards the midline. Adductus is the second part of the clubfoot deformity. The forefoot is adducted towards the midline. This is the second part of the deformity of clubfoot. The navicular moves medially and starts to dislocate off the talus. The calcaneum also rotates medially under the talus as part of the adductus deformity.[7]
- Varus means movement towards the midline. Varus of the hindfoot is the third part of the deformity of clubfoot. The heel is in varus in relation to the tibia.[7]
- Equinus means an increase in the plantarflexion of the foot. The entire foot points downwards in relation to the tibia. Equinus of the hindfoot is therefore the fourth part of the clubfoot deformity.[7]
The deformity consists of equinus/plantarflexion at the ankle combined with adduction and inversion at the subtalar, midtarsal and anterior tarsal joints[19]. Clubfoot can be described as “congenital dislocation of the Talo-Calcaneal-Navicular (TCN) Joint” [20]. The navicular moves medially on the talus in clubfoot while the calcaneum rotates under the talus in clubfoot
The foot is held in adduction and inversion by ligaments and muscles. Muscles that are contracted are triceps surae, tibialis posterior, flexor digitorum longus and flexor hallucis longus. Further there is an imbalance between the inverter-plantarflexor muscles and the everter-dorsiflexor muscles. The calf and peroneal muscles are usually poorly developed.[19] Weak peroneal muscles allow the foot to be inverted. The ligaments of the posterior and medial aspect of the ankle are thick and taut.[21].
Classification[edit | edit source]
Not all Clubfeet are the same and it is important that all people treating clubfoot use the same terms to describe the different types. Each type of clubfoot has unique characteristics and may need specific treatment. Early recognition of the type of clubfoot one is dealing with can help guide appropriate treatment. Although there is no universal classification system for clubfoot, clubfoot can be classified according to the nature of the deformity: [22]
Positional Clubfoot[edit | edit source]
Positional clubfoot refers to a flexible foot that was held over time in an abnormal position in utero. When the child is born, due to the prolonged positioning, they may present with one or both feet in an atypical resting position. Children with positional clubfoot typically exhibit unrestricted passive range of motion of forefoot and ankle. The foot at the time of birth has some deformity but bony alignment is not impacted and foot position is likely corrected through conservative treatment involving a program of stretching, range of motion, and weight bearing. In a small number of cases post conservative treatment the foot needs 1 or 2 Casts to ensure they are maintained in a corrected position although in the majority of cases these feet usually correct well and do not lead to any long lasting, significant impairment.[7] [23]
Idiopathic Clubfoot[edit | edit source]
Most commonly, clubfoot is classified as “Idiopathic Clubfoot” meaning there is no known cause for the deformity. In idiopathic clubfoot, there can also be a definite hereditary influence, in that if a person has a relative, parent, or sibling has clubfoot, then they are more likely to have clubfoot or have a child with it (3-10% chance). Within the group of idiopathic clubfeet there is a wide spectrum of impairment depending on severity, as well as whether the clubfoot has been untreated, partially treated, poorly treated, or successfully treated[7]. These are outlined by the Arica Clubfoot Training[7] as follows:
- Untreated Clubfoot - all clubfeet from birth up to 2 years of age that have had very little or no treatment can be considered as untreated clubfeet.
- Treated Clubfoot - untreated clubfeet that have been corrected with Ponseti treatment are termed “treated clubfeet”. Treated clubfeet are usually braced full-time for 3 months and at night up to age 4 or 5 years.
- Recurrent Clubfoot - this is a clubfoot which has achieved a good result with Ponseti treatment, but the deformity has recurred. The commonest reason is due to abandoning the braces early.
- Neglected Clubfoot - the neglected clubfoot is a clubfoot in a child older than 2 years, where little or no treatment has been performed. The neglected clubfoot may respond to Ponseti treatment, but also may have bony deformity that requires surgical correction.
- Complex Clubfoot - any foot with deformity that has received any type of treatment other than the Ponseti method may have added complexity because of additional pathology or scarring from surgery.
- Resistant Clubfoot - this is a clubfoot where Ponseti treatment has been correctly performed but there has been no significant improvement. It is often found that this type of clubfoot is not in fact idiopathic after all and is secondary or syndromic.
- “Atypical” Clubfoot - this is a type of clubfoot dealt with in the advanced section of this course (chapter 15). It involves a foot that is often swollen, has a plantarflexed first metatarsal and an extended big toe. It can occur spontaneously but most often occurs after slippage of a cast.
Secondary Clubfoot[edit | edit source]
Secondary clubfoot, on the other hand, occurs when there is another disease or condition that is causing or linked to the development of clubfoot. Such conditions are usually Neurological such as Spina Bifida associated with concurrent sensory and or motor impairments or Syndromic Disorders such as Arthrogryposis associated with more global findings and involvement of other musculoskeletal issues.[24]
Diagnosis[edit | edit source]
Clubfoot is usually detected antenatally, by ultrasound scan, or at birth. The examination after birth consists of taking the foot and manipulating it gently to see if it can be brought into normal position. If not, there is a positive diagnosis of clubfoot.[25]
Prognosis[edit | edit source]
Prognosis can be dependant on when treatment begins. When treatment is started before the child begins weight bearing, the chances of successful treatment and relatively ‘normal’ foot function are high. Persistence in wearing the Foot Abduction Brace also contributes to a good prognosis, by preventing relapse.[19] In older children, some may achieve partial, or even full correction with the Ponseti treatment. In others, a period of casting following the Ponseti principles may need to be supplemented with surgery to gain full correction of the foot position.
Outcome Measures[edit | edit source]
The most common used outcome measure is the scoring system of Pirani. This scoring system assesses the severity of clubfoot deformity and response to treatment[26]. It has a predictive value concerning the number of casts needed to correct the foot. A high score, 4 or more, predicts the use of at least 4 casts. A score less than 4 predicts the need of 3 or fewer casts. Each component is scored as 0 (normal), 0.5 (mildly abnormal) or 1 (severely abnormal) [21] For other outcome measures see Roye Score and the Bangla Clubfoot Tool.
Treatment[edit | edit source]
Many different treatment methodologies for clubfoot have been used but since the 1970’s the Ponseti Method of treatment has grown in popularity and has completely replaced the previous methods of treating clubfoot in many countries, which included a mix of surgical and conservative techniques. Ponseti Method consists of 2 equally important phases: the Corrective Phase and the Maintenance Phase.
| Ponseti Method Phases of Treatment | |
| Corrective Phase | During the corrective phase the position of the foot is gradually corrected using a series of manipulations and plaster of Paris casts, then finally a small outpatient procedure is performed to cut the Achilles tendon (tenotomy). The corrective phase usually takes 4–8 weeks and the baby is seen weekly for the treatment. |
| Maintenance Phase | Once the corrective phase has achieved a good position for the foot, the treatment is not over as the foot will tend to return to its deformed position, so the aim of the maintenance phase involves keeping the corrected position for the next 4–5 years. This is achieved by putting the child’s feet into a brace for:
|
The Ponseti Method is a simple, cost-effective treatment that has become widely used around the world. Numerous research studies in countries across the globe in the last 20 years have shown that in more than 90% of cases of newborn children with idiopathic clubfoot it can be treated effectively with the Ponseti technique. The Ponseti Method’s efficacy is backed up by a large and growing body of evidence, and has now become the treatment of choice for clubfoot. [11][12][13][21][26][27]
The goals of treatment are:
- To have functional, pain-free feet
- To wear normal shoes
- To avoid permanent disability
The entire course of treatment can cost as little as US$150, which compared to many treatments for similar conditions is extremely economical. This is why many Ministries of Health, NGOs, and others see the value of providing Ponseti treatment as an early intervention in order to avoid preventable disability.[7]
Throughout the Ponsetti Management of Clubfoot there are Ten Key Messages to keep in mind:[7]
- Assess, Plan, and Treat
- Talk to Parents from the Start (Especially about Braces!)
- Correct First then Maintain
- Correct Cavus First
- Never Touch the Heel
- TWO People to Cast
- Toe to Groin Casts
- In most cases Tenotomy is required
- Cover the Talus before Tenotomy
- Keep Talking to Parents - they are key to maintaining correction through good adherence to Bracing!
References[edit | edit source]
- ↑ Amanda Marie De Hoedt, Clubfoot Image Classification, University of Iowa, Iowa Research Online, 2013 [Available from Iowa Research Online /ir.uiowa.edu/etd/4836 http://ir.uiowa.edu/etd/4836]
- ↑ 2.0 2.1 Daniel Augusto Carvalho Maranho, Jose Batista Volpon, Congenital Clubfoot , 2011;19(3):163-9.
- ↑ 3.0 3.1 3.2 3.3 Dietz F. The genetics of idiopathic clubfoot. Clinical orthopaedics and related research. 2002 Aug 1;401:39-48.
- ↑ 4.0 4.1 Bridgens J, Kiely N. Current management of clubfoot (congenital talipes equinovarus). BmJ. 2010 Feb 2;340(6):c355.
- ↑ McKinney J, Rac MW, Gandhi M. Congenital talipes equinovarus (clubfoot). American Journal of Obstetrics & Gynecology. 2019 Dec 1;221(6):B10-2.
- ↑ Dibello D, Di Carlo V, Colin G, Barbi E, Galimberti A. What a paediatrician should know about congenital clubfoot. Italian Journal of Pediatrics. 2020 Dec;46(1):1-6.
- ↑ 7.00 7.01 7.02 7.03 7.04 7.05 7.06 7.07 7.08 7.09 7.10 7.11 7.12 Africa Clubfoot Training Project. Chapter 2 Africa Clubfoot Training Basic & Advanced Clubfoot Treatment Provider Courses - Participant Manual. University of Oxford: Africa Clubfoot Training Project, 2017.
- ↑ 8.0 8.1 8.2 8.3 8.4 Penny JN. The neglected clubfoot. Techniques in orthopaedics. 2005 Jun 1;20(2):153-66.
- ↑ Staheli L. Clubfoot: ponseti management: Global HELP Organization; 2009.
- ↑ 10.0 10.1 10.2 Lavy CB, Mannion SJ, Mkandawire NC, Tindall A, Steinlechner C, Chimangeni S, Chipofya E. Club foot treatment in Malawi–a public health approach. Disability and rehabilitation. 2007 Jan 1;29(11-12):857-62.
- ↑ 11.0 11.1 11.2 Boden, R.A., Nuttall, G.H., & Paton, R.W. (2011). A 14-year longitudinal comparison study of two treatment methods in clubfoot: Ponseti versus traditional. Acta Orhopaedica Belgica, 77(4), pp. 522-528.
- ↑ 12.0 12.1 Harnett, P., Freeman, R., Harrison, W.J., Brown, L.C., ; Beckles, V. (2011). An accelerated Ponseti versus the standard Ponseti method. The Journal of Bone ; Joint Surgery, 93, pp. 404-408.
- ↑ 13.0 13.1 Jowett, C.R., Morcuende, J.A., ; Ramachandran, M. (2011). Management of congenital talipes equinovarus using the Ponseti method. The Journal of Bone & Joint Surgery, 93, pp. 1160-1164.
- ↑ 14.0 14.1 14.2 14.3 14.4 14.5 14.6 Henrik M. Wallander, Congenital Clubfoot (Aspects on Epidemiology, Residual Deformity and Patient Reported Outcome), ACTA University, 2009.
- ↑ Dobbs MB, Gurnett CA. Update on clubfoot: etiology and treatment. Clinical orthopaedics and related research. 2009 May 1;467(5):1146.
- ↑ Smythe T, Kuper H, Macleod D, Foster A, Lavy C. Birth prevalence of Congenital Talipes Equinovarus in Low and Middle Income Countries: A Systematic Review and Meta‐analysis. Tropical medicine & international health. 2016 Dec 1.
- ↑ 17.0 17.1 Siapkara A, Duncan R. Congenital talipes equinovarus. Bone & Joint Journal. 2007 Aug 1;89(8):995-1000.
- ↑ 18.0 18.1 18.2 18.3 18.4 18.5 18.6 18.7 Pandey, S., & Pandey, A.K. (2003). The classification of clubfoot a practical approach. The Foot, 13, pp. 61-65.
- ↑ 19.0 19.1 19.2 Adams, J.C., & Hablen, D.L. (2001). Outline of Orthopaedics. London: Churchill Livingstone.
- ↑ Anand, A., & Sala, D.A. (2008). Clubfoot: Etiology and treatment. Indian Journal of Orthopaedics, 42(1), pp. 22-28.
- ↑ 21.0 21.1 21.2 Staheli, L. (2009). Clubfoot: Ponseti Management Third Editon. Seattle: Global Help.
- ↑ Clubfoot,http://emedicine.medscape.com/article/1237077-overview#a4 (accessed 28 June 2017)
- ↑ Africa Clubfoot Training Project. Chapter 1 Africa Clubfoot Training Basic & Advanced Clubfoot Treatment Provider Courses - Participant Manual. University of Oxford: Africa Clubfoot Training Project, 2017.
- ↑ Africa Clubfoot Training Project. Chapter 15 Africa Clubfoot Training Basic & Advanced Clubfoot Treatment Provider Courses - Participant Manual. University of Oxford: Africa Clubfoot Training Project, 2017.
- ↑ Goldie, B.S. (1992). Orthopaedic Diagnosis and Management. A guide to the care of orthopaedic patients. Oxford: Blackwell Scientific Publications.
- ↑ 26.0 26.1 Docker, C.E.J., Lewthwaite, S., & Kiely, N.T. (2007). Ponseti treatment in the management of clubfoot deformity – a continuing role for paediatric orthopaedic services in secondary care centres. The Royal College of Surgeons of England, 89, pp. 510-512.
- ↑ Suzann, K.C., Vander Linden, D.W., & Plisano, R.J. (2005). Physical Therapy for Children. Missouri: Elsevier.