Menstrual Cycle and Physical Activity
Introduction[edit | edit source]
Menstruation is a normal physiologic phase that begins during adolescence wherein the progestational endometrium is shredded leading to blood loss and numerous hormonal changes. In the normal menstrual cycle, there is a complex interplay between oestrogen and progesterone hormones. Under normal circumstances, it occurs every 28 to 35 days, the blood flow lasts for 3 to 5 days and the average blood loss is 30 to 80 ml. It is governed by the general health of the girl, and socioeconomic and nutritional status. The coordination is carried out by the hypothalamic-pituitary-ovarian axis.[1]
There are many menstrual disorders such as Dysmenorrhoea, Amenorrhea, Hypomenorrhea, Polymenorrhea, Oligomenorrhea, Menorrhagia, Metrorrhagia, and Premenstrual syndrome. All of these can be affected by many factors like age, family history, smoking, and physical activity.
It is very important to understand the association between physical activity and menstruation, reproductive hormones, and ovulation as it influences fertility outcomes. Studies have proved that physical activities and exercises have a great effect on the reduction of menstrual disorders.[1]
Menstrual disorders[edit | edit source]
Dysmenorrhoea: Painful cramps of the uterus during menses. Pain is felt in the lower abdomen and inner thighs. There are symptoms in many cases like low back pain, nausea, vomiting, diarrhoea, fatigue, and headache. It is quite common and almost 50% of the women suffer from it. 10% of women suffer severely. There are two categories in this: Primary and Secondary. Primary dysmenorrhoea occurs soon after menarche once ovulation is established.[2]Secondary dysmenorrhoea occurs due to any pelvic pathology such as ovarian cysts, uterine fibroids, adhesions, cervical stenosis, or adenomyosis. It even happens due to the usage of intrauterine contraceptive devices.
In electrotherapy, a high-intensity laser or TENS can be used to treat the symptoms of primary dysmenorrhoea..[3]
Premenstrual syndrome: Many women of reproductive age have some discomfort before a few weeks of menstruation. This includes mood swings, tension, breast tenderness, bloating, irritability, depression, and fearfulness.[4]One study has proved that exercise like swimming helps in reducing the physical and psychological symptoms of premenstrual syndrome.[5]
Amenorrhea: It has two types: Primary and Secondary, In the primary, there is failure to reach menarche due to chromosomal abnormalities like ovarian insufficiency or anatomic abnormalities. In secondary, there is the cessation of regular menses for three months or cessation of irregular menses for six months.[6]
Menorrhagia: Heavy menstrual bleeding (>80ml per menstrual cycle)is known as menorrhagia. This is common, affecting a quarter of females. It can lead to negative physical and emotional changes with a reduction in work capacity.[7]Studies have proven that heavy menstrual bleeding is seen in elite athletes which are associated with iron deficiency anaemia, it is even linked to reduced oxygen-carrying capacity and reduced haemoglobin. All this in turn reduces the performance. The athletes are at risk of gastrointestinal bleeding, sweating, and hemolysis especially the ones involved in contact sports. Hence excessive exercises lead to menstrual abnormalities.[8]
Effect of menstrual cycle phase on physical activities[edit | edit source]
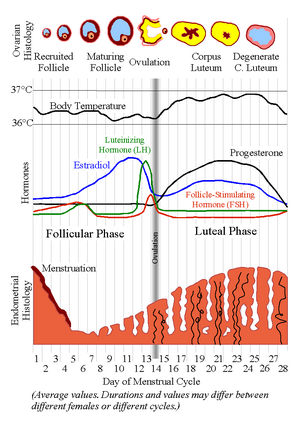
Female hormones keep on changing continuously during their ovulatory menstrual cycle. It affects various parameters of the body such as cardiovascular, respiratory, thermal, and metabolic which in turn have an influence on exercise physiology.[9] There are four main phases of a menstrual cycle: the early follicular phase, ovulation phase, and mid-luteal phase. The early follicular phase is characterised by low oestrogen and low progesterone phase. The ovulatory phase is characterised by high oestrogen and low progesterone phase. The mid-luteal phase has high oestrogen and high progesterone level. It is further classified into early follicular phase, late follicular phase, ovulation, early luteal, mid-luteal, and late-luteal phase.[10]
Studies have shown that the performance of exercises was reduced in the follicular phase due to low levels of oestrogen and progesterone. Oestrogen has anabolic effects and restores the glycogen stores. It even acts as an antioxidant and membrane stabiliser hence it helps against exercise-induced muscle damage and reduces inflammatory responses. It has neuroexcitatory effects where it activates voluntary activation and reduces inhibition. Therefore when the oestrogen rises in other menstrual phases the performance of exercises improves.[10] There is reduction of maximal endurance in the mid-luteal phase as per one study.[9]
Progesterone has anti-oestrogenic effects. Hence when the oestrogen effects are high in the ovulatory phase and late follicular phase, the performance is at its peak as there is no interference from progesterone.[10]
While some studies have reported a decrease in physical performance in the early follicular phase, other studies have found no significant changes in overall physical performance. For instance, a narrative review of athletes' perceived and objectively measured performance shows that: Female athletes believe their performance is slightly lower in the early follicular and late luteal phase. However, results based on objectively measured performance (with aerobic, anaerobic, and strength-related assessments) do not indicate that menstrual cycle phases have a significant impact on physical performance. As a result, the impact of the menstrual cycle on physical performance is still debated.[11]
Effect of menstrual cycle on joint laxity[edit | edit source]
It is proven that females have more laxity on day 5 of menses, days 3 to 5 of initial oestrogen rise, days 1 to 4 of the early luteal phase, and days 1,2,4, and 5 of the late luteal phase.[12]when the oestrogen level increases, laxity is increased as well. In 2012 Shultz found that "there was a direct relationship between the high oestrogen level and ACL injury, the knee laxity increased in direct relation to elevations in plasma estradiol levels. During oestrogen rise in the ovulatory phase, there is a concomitant rise in ACL ruptures"[13].
Menstrual Cycle-Related Performance Changes/Risk of Injuries[edit | edit source]
There may be different factors related to the menstrual cycle behind the risk of injury. The mechanisms that the menstrual cycle affects:
- Strength
- Balance
- Stiffness
- Thermoregulation
- Metabolism (Substrate availability)
- Body composition
It is considered that the incidence of injuries is greater in the late follicular phase as compared to other phases because of muscle stiffness because of the high level of oestrogen. This consideration is due to the inhibitory effect of oestrogen on collagen synthesis. However, the results are conflicting. There are some studies report that "any increase in oestrogen is not great enough to have a significant impact on collagen density".[11]
In professional soccer, the rate of women suffered from muscle strains was 54% lower than males along with the tendon injury but they were at a higher risk of ligament injury and this was more related to the level of oestrogen[14]. A recent study that measured the flexibility of hamstring and muscle strength during the menstrual cycle in healthy young females found that; there was a significant increase in the range of motion and passive torque during the ovulatory and luteal phase and the passive stiffness decreased significantly during the ovulatory phase. In addition, there was a significant increase in electromyographic activity and isometric muscle force during the luteal when compared to the ovulatory phase[15]
Exercise and Dysmenorrhoea[edit | edit source]
Dysmenorrhoea is not a threat to life but it affects the quality of life based on its severity. It is believed to be associated with increased prostaglandins and increased contraction of the uterine muscle.[2]Different medical and non-medical treatments are proven to reduce the symptoms such as taking NSAIDs, herbal diet therapies, yoga, meditation, and acupressure.
Mild to moderate exercises/physical activities help in controlling the symptoms of dysmenorrhoea. According to the intensity of exercise it was stated that "moderate –high-intensity exercise was believed to increase the anti-inflammatory cytokines, decrease the overall amount of prostaglandins released because of the decrease of over the all amount of menstrual flow and low-intensity exercise reduces the cortisol level and prostaglandin synthesis"[16].In overall exercises release endorphins which increase the pain threshold and improve the mood of exercising subjects. It reduces the consumption of drugs and the length of menstruation pain. It even promotes positive thoughts and distracts intrusive thoughts.[17]
There are different approaches to treating primary dysmenorrhoea. This includes NSAIDS or contraceptive medicines, but there are numerous side effects of these medications due to which nonpharmacological treatments like physiotherapy are preferred. Stretching techniques and isometric exercises help in this condition. Kegel exercises, jogging, and relaxation exercises are effective. Specific Yoga sanas like Suryanamaskar, Shavasana, Supta Vajrasna, Jannu Sirsana, and Pashimottasana can also be prescribed. [3]One should make sure that all the exercises are done under the supervision of a physiotherapist in order to avoid the mal performance.
Dosage of exercises for dysmenorrhoea:
- Moderate to high-intensity exercises three times a week, are recommended and it helps to decrease the symptoms during the menstruation[18]. A systematic review about the effect of exercises on dysmenorrhea found that doing exercises for 45 to 60 minutes each time, three times per week or more regardless of the intensity may be effective to decrease symptoms associated with menstrual pain intensity of around 25 mm on a 100 mm VAS[19].
References[edit | edit source]
- ↑ 1.0 1.1 Kulshrestha S, Durrani AM. Prevalence of menstrual disorders and their association with physical activity in adolescent girls of aligarh city. Int J Health Sci Res. 2019;9(8):384-93.
- ↑ 2.0 2.1 Mahvash N, Eidy A, Mehdi K, Zahra MT, Mani M, Shahla H. The effect of physical activity on primary dysmenorrhea of female university students. World Applied Sciences Journal. 2012;17(10):1246-52.
- ↑ 3.0 3.1 López-Liria R, Torres-Álamo L, Vega-Ramírez FA, García-Luengo AV, Aguilar-Parra JM, Trigueros-Ramos R, Rocamora-Pérez P. Efficacy of physiotherapy treatment in primary dysmenorrhea: a systematic review and meta-analysis. International Journal of Environmental Research and Public Health. 2021 Jan;18(15):7832.
- ↑ Yonkers KA, O'Brien PS, Eriksson E. Premenstrual syndrome. The Lancet. 2008 Apr 5;371(9619):1200-10.
- ↑ Maged AM, Abbassy AH, Sakr HR, Elsawah H, Wagih H, Ogila AI, Kotb A. Effect of swimming exercise on premenstrual syndrome. Archives of gynecology and obstetrics. 2018 Apr;297(4):951-9.
- ↑ Klein DA, Poth MA. Amenorrhea: an approach to diagnosis and management. American family physician. 2013 Jun 1;87(11):781-8.
- ↑ Bruinvels G, Burden R, Brown N, Richards T, Pedlar C. The prevalence and impact of heavy menstrual bleeding (menorrhagia) in elite and non-elite athletes. PLoS One. 2016 Feb 22;11(2):e0149881.
- ↑ Huhmann K. Menses requires energy: a review of how disordered eating, excessive exercise, and high stress lead to menstrual irregularities. Clinical Therapeutics. 2020 Mar 1;42(3):401-7.
- ↑ 9.0 9.1 Julian R, Hecksteden A, Fullagar HH, Meyer T. The effects of menstrual cycle phase on physical performance in female soccer players. PloS one. 2017 Mar 13;12(3):e0173951.
- ↑ 10.0 10.1 10.2 McNulty KL, Elliott-Sale KJ, Dolan E, Swinton PA, Ansdell P, Goodall S, Thomas K, Hicks KM. The effects of menstrual cycle phase on exercise performance in eumenorrheic women: a systematic review and meta-analysis. Sports Medicine. 2020 Oct;50(10):1813-27.
- ↑ 11.0 11.1 Carmichael MA, Thomson RL, Moran LJ, Wycherley TP. The impact of menstrual cycle phase on athletes’ performance: A narrative review. Int J Environ Res Public Health. 202;18(4):1667.
- ↑ Shultz SJ, Sander TC, Kirk SE, Perrin DH. Sex differences in knee joint laxity change across the female menstrual cycle. The Journal of sports medicine and physical fitness. 2005 Dec;45(4):594.
- ↑ Shultz SJ, Wideman L, Montgomery MM, Beasley KN, Nindl BC. Changes in serum collagen markers, IGF‐I, and Knee joint laxity across the menstrual cycle. Journal of Orthopaedic Research. 2012 Sep;30(9):1405-12.
- ↑ Hägglund M, Waldén M, Ekstrand J. Injuries among male and female elite football players. Scandinavian journal of medicine & science in sports. 2009 Dec;19(6):819-27.
- ↑ Miyazaki M, Maeda S. Changes in hamstring flexibility and muscle strength during the menstrual cycle in healthy young females. Journal of Physical Therapy Science. 2022;34(2):92-8.
- ↑ Warren MP, Perlroth NE. Hormones and sport-the effects of intense exercise on the female reproductive system. Journal of endocrinology. 2001;170(1):3-12.
- ↑ Koushkie Jahromi M, Gaeini A, Rahimi Z. Influence of a physical fitness course on menstrual cycle characteristics. Gynecological endocrinology. 2008 Jan 1;24(11):659-62.
- ↑ Lefebvre G, Pinsonneault O, Antao V, Black A, Burnett M, Feldman K, Lea R, Robert M. Primary dysmenorrhea consensus guideline. J Obstet Gynaecol Can. 2005 Dec 1;27(12):1117-46.
- ↑ Armour M, Ee CC, Naidoo D, Ayati Z, Chalmers KJ, Steel KA, de Manincor MJ, Delshad E. Exercise for dysmenorrhoea. Cochrane Database of Systematic Reviews. 2019(9).