Huntington's Disease: A Case Study
This page is currently under revision by Queen's MScPT students in the course PT858 lab group 6. The scope of this article is to describe the characteristics and care related to the earliest clinical stage of Huntington's Disease.
Abstract[edit | edit source]
This is a fictional case study involving a 41-year-old male presenting with early-stage Huntington’s disease. Our case study encompasses the presentation of the patient, appropriate interventions, interdisciplinary care and functional outcomes one year after the initial visit. This patient presented with difficulty manipulating and gripping objects in his workplace as a teacher. Cognitive effects were also noted, including apathy and emotional outbursts. We concentrated on his patient-specific goals in tandem with the understanding that he has a progressive disease that will require ongoing and proactive treatment. Aerobic training was introduced as well as respiratory muscle training to combat the eventual symptoms of respiratory failure. Other interdisciplinary professionals were involved in his care and referrals were made at the follow-up visit to a speech-language pathologist and social worker. The patient’s outcomes for fine motor tasks were significantly reduced one year later; however, indirect measures of aerobic capacity experienced an initial increase after training and physiotherapy interventions.
Introduction and Background Information[edit | edit source]
Huntington’s Disease (HD) is an inherited disease that involves progressive degeneration of nerve cells in the brain, specifically within the basal ganglia[1]. Typical onset occurs at age 30 or 40 years of age; however, another variety of Huntington’s disease called juvenile Huntington’s disease can develop in children or young adults. The disease is inherited through autosomal dominant genes, meaning the affected person inherits the gene from a parent with the same affected gene[2]. In autosomal dominant disorders, the disease-causing gene is located on a non-sex or numbered chromosome. Through genetic testing, researchers can determine the number of repeats of the CAG (cytosine-adenine-guanine) trinucleotide on a specific gene called the Huntingtin (HTT) gene[3]. In the general population, the average number of CAG repeats is 17-20, whereas in people with Huntington’s disease the HTT gene has a CAG repeat count of 36 or more[3].
Normal Function of the Basal Ganglia[edit | edit source]
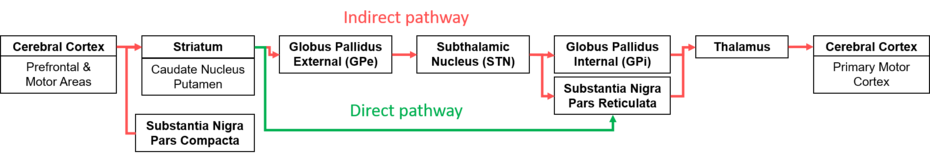
The basal ganglia (BG) are a collection of subcortical structures that are related to the subconscious regulation of voluntary body movement and mood[4]. Normally, movements that are desired by the prefrontal cortex activate the direct pathway to release tonic inhibition of the thalamus and permit movements through activating the primary motor cortex[4], see figure 1 the direct pathway in green. On the other hand, movements that are not desired by the prefrontal cortex are increasingly inhibited through the indirect pathway, preventing unwanted activation of movement from being generated in the primary motor cortex[4], see figure 1 the indirect pathway in red.
Figure 1. Linear schematic diagram of the direct and indirect pathways for the normal regulation of voluntary movements[5].
Neuropathology of HD and the Production of Chorea[edit | edit source]
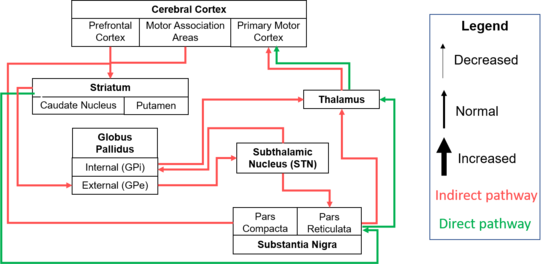
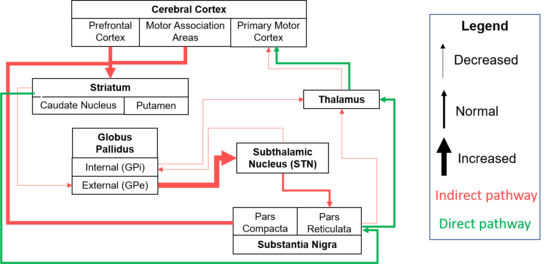
Populations with HD are highly heterogenous, and present with a vast array of motor and cognitive changes[4]. The pathological changes with HD in the basal ganglia are primarily characterized by atrophy to the caudate nucleus and putamen (together making the striatum)[4]. The degeneration of the striatum leads to a reduction of inhibition from the indirect pathway[4]. This leads to downstream changes (visually depicted in Figure 2.B.) of increased activity of the globus pallidus external (GPe), increased inhibition of the subthalamic nucleus (STN), decreased excitation of the globus pallidus internal (GPi), and lastly, increased excitation from the thalamus to the motor cortex[4]. The abnormal increase in excitation from the thalamus to the cortex results in the production of chorea[4].
Figure 2.Hierarchical schematic diagram of Cortico-basal pathways. A. Normal. B. Pathological changes with HD resulting in reduced inhibition of the indirect pathway causing hyperkinetic movements and chorea[5].
Symptoms[edit | edit source]
Huntington’s disease affects movement, cognition, and behaviour. Movement symptoms include non-suppressible, non-rhythmic, jerky, involuntary movements (chorea), and sustained involuntary contractions leading to abnormal postures (dystonia). Cognitive symptoms include lack of impulse control, which can result in outbursts, or a decline in reasoning abilities. Behavioural symptoms include psychiatric disorders such as depression or bipolar disorder, which could result in apathy[1]. As the disease progresses, these symptoms become more pronounced.
The following is a short video that effectively summarizes Huntington's Disease[6]:
Purpose[edit | edit source]
The chief purpose of this report is to demonstrate an example of physiotherapy management for a person with early stages of Huntington’s disease, approximately 6 months after clinical diagnosis. This fictional case study will present with typical symptoms of early Huntington's disease, such as chorea, impaired cognition, depression, and others. The case study provides information on the clinical presentation, subjective and objective findings, interventions, 1-year follow-up assessment, and interdisciplinary management of chorea. This may be useful to physiotherapy students as a general example of the presentation of early Huntington's disease, and the physiotherapy treatment that is typically involved.
Additional Note[edit | edit source]
An article by Roos[7] found that chorea can be the first presenting symptom of Huntington’s disease. However, other articles have conflicting results in terms of the symptoms presented during early stages. For example, Kirkwood[8] found that chorea can present in the middle stages of this disease. Therefore, we chose to focus on chorea as the initial motor problem to showcase one example of how Huntington’s disease can manifest during the early stage.
Client Characteristics[edit | edit source]
Patient is a 41-year-old, right hand dominant male schoolteacher who presents with a diagnosis of early-stage Huntington’s disease. Mr. McGee’s family doctor had suggested that physiotherapy could be an appropriate option for helping him to manage the various problems he has been experiencing at work, including writing with chalk and typing. Mr. McGee appeared to be highly agitated today as he spoke at an increased volume and speed. Mr. McGee has noticed an increase in symptoms lately due to high stress during exam season. He stated that he has been more irritable than usual over the last month.
The patient declared that he is “having difficulty controlling his hands and fingers” due to involuntary, uncontrolled movements, making it difficult to grade exams. Mr. Mcgee stated that he formerly relied on physical activity to alleviate stress, but now has difficulty keeping his fingers flexed on his bicycle handlebars and is concerned that he cannot ride his bicycle safely.
Mr. McGee ambulates with no gait aid and appears moderately fit; however, he collapses heavily into the chair when asked to sit down. He comments on increased fatigue but feels that his sleep quality and quantity is unchanged.
Examination Findings[edit | edit source]
Subjective[edit | edit source]
History of Present Illness (HPI)[edit | edit source]
Mr. McGee originally became aware of his condition when he began experiencing difficulties while teaching his grade 6 class. Teaching had become more challenging than usual for Mr. McGee, and he found it “frustrating to keep hold of a piece of chalk when writing on the blackboard”, usually resulting in him dropping the chalk and feeling “embarrassed” in front of his students. To remedy this frustrating reoccurrence, Mr. McGee purchased a chalk holder so that he could maintain a firmer grip on his chalk during his daily lectures. Mr. McGee admits that he “has always had a short temper”, though recently, his students presented their concerns about several of his recent angry outbursts in the classroom to the school principal, who later spoke with Mr. McGee about these incidences. Mr. McGee’s wife had also noticed a gradual change in his disposition, noting that he has become seemingly indifferent towards her and has no interest in seeing other people, even close family members and long-time friends. Mrs. McGee suggested that Mr. McGee book an appointment with his physician after becoming concerned with his varying moods and behaviour. Mr. McGee recognized that he was “not feeling like his usual self” and trusted his wife’s recommendation to consult his physician. Mr. McGee’s physician recognized that something was awry with his patient and referred him to a neurologist for further assessment and testing. After conducting genetic testing on Mr. McGee, the neurologist determined that Mr. McGee tested positive for Huntington’s Disease.
Past Medical History (PMHx)[edit | edit source]
Two years ago, during a routine physical, Mr. McGee informed his family doctor that he was feeling unusually depressed more days than not and was not experiencing much joy in his life anymore. After screening Mr. McGee for depression, his family doctor prescribed him an antidepressant medication.
Current Interventions[edit | edit source]
Mr. McGee uses a chalk holder while teaching to improve his grip and dexterity when he is writing on the chalkboard. As part of his depression management plan, Mr. McGee’s family doctor provided him with coping strategies and mindfulness techniques, as well as recommendations for physical activity.
Medications (Rx)[edit | edit source]
Mr. McGee is currently taking 100 mg of Sertraline (Zoloft), an antidepressant, orally once a day as prescribed by his family doctor.
Health Habits (HH)[edit | edit source]
Mr. McGee does not smoke cigarettes, drink alcohol, or use recreational drugs.
Social History (SHx)[edit | edit source]
Mr. McGee lives in a bungalow with his wife and 6-year-old daughter. His wife is currently pregnant with their second child and is a stay-at-home mom. They are planning on purchasing a larger home to accommodate their growing family. He has an older sister and parent in Toronto. His adoptive mother resides in a retirement home.
Prior Functional History[edit | edit source]
Mr. McGee used to ride his bicycle with his co-workers on Saturday afternoons for 45 minutes at a moderate intensity and go for leisurely walks with his wife and daughter every night for about 30 minutes.
Current Functional Status[edit | edit source]
He is reasonably active and engages in moderate-to-vigorous physical activity at least two days of the week for a total of ~80 minutes. He is “not as physically active now as [he] was in the past” due to his decreased motivation. Currently, Mr. McGee is not riding his bicycle due to increased choreatic movements of his hands and wrists, leading to a perceived lack of safety on his bicycle. He does not feel motivated to go for walks with his wife and daughter and has decreased from daily walks to 1-2x/week.
Family History (FHx)[edit | edit source]
At the age of two, Mr. McGee was adopted by his non-biological parents. Despite his efforts searching for his ancestry online, Mr. McGee has had no success determining his lineage. Mr. McGee’s adoptive father passed away one year ago from liver cancer. Mr. McGee’s adoptive mother had a TIA six months ago, at approximately the same time as Mr. McGee’s diagnosis of Huntington’s disease. Mr. McGee’s biological familial medical history is unknown.
Chief Concern[edit | edit source]
Mr. McGee would like to be able to write legibly and type on his computer in a timely manner with minimal error like he used to do. He gets very upset and frustrated when he makes mistakes in front of the class and these feelings have led to emotional outbursts that could jeopardize his career.
Objective[edit | edit source]
Observation[edit | edit source]
In seated position, the patient’s hands and fingers exhibit uninhibited, involuntary writhing and flexion/extension movements bilaterally. Mr. McGee also has slight twitching of his ankles bilaterally. Posture is upright and symmetrical with slight thoracic kyphosis.
Active Range of Motion (AROM)[edit | edit source]
| Joint | Range |
|---|---|
| Cervical spine flexion, extension, side flexion, rotation | WNL, bilaterally |
| Shoulder flexion, abduction, medial rotation, lateral rotation | WNL, bilaterally |
| Elbow flexion, extension | WNL, bilaterally |
| Wrist flexion, extension, radial deviation, ulnar deviation | WNL, bilaterally* |
* Difficult to assess with goniometer due to choreatic movements, movement was approximated as within normal limits (WNL)
Passive Range of Motion (PROM)[edit | edit source]
All body segments mentioned above WNL, normal end feels for each, bilaterally
Posture & Balance[edit | edit source]
Postural control will be assessed using the Berg Balance Scale[9] (see below in Outcome Measures)
Gait[edit | edit source]
Symmetrical limb movement bilaterally; cadence and speed were typical.
Outcome Measures[edit | edit source]
Discussion on Unified Huntington's Disease Rating Scale (UHDRS)[edit | edit source]
The most common clinical tool for diagnosing and monitoring the progression of HD is the Unified Huntington’s Disease Rating Scale (UHDRS)[10]. The tool encompasses motor, cognitive, behavioural, and functional domains[11].
The most common motor diagnosis of HD involves a grade 4 of chorea[12], which is described as maximal chorea of the extremities, trunk, mouth, and face[11]. The motor domain’s total motor score (TMS) allows for measurement of the disease’s progression[10].
The Shoulson–Fahn functional capacity rating scale from 1979, also called the Total Functional Capacity (TFC) scale, was adopted into the UHDRS as the functional domain[13]. The functional domain measures the level of independence in occupation, finances, domestic chores, ADLs, and care level[11]. This domain is used by clinicians to assign a stage to the disease's progression ranging from I to V in an increasing degree of disability based on the scoring of the items[13].
The UHDRS is the gold standard assessment tool for monitoring the progression of motor symptoms of HD over time[10]. Unfortunately, the UHDRS is not a free tool and must be requested through the Huntington Study Group . Though not ideal, the following section includes outcome measures that are more accessible and free to use.
Other Relevant Outcome Measures[edit | edit source]
Patient Specific Functional Scale (PSFS)[14][edit | edit source]
- Holding and writing with chalk: 9
- Handwriting on paper: 8
- Typing on the keyboard: 9
- Average score: 8.67
Timed Up and Go (TUG)[15][edit | edit source]
Obtained score of 8.3 seconds without cognitive task and 13.2 seconds with cognitive task.
- On the TUG, an increased risk of recurrent falls with HD is at ≥14 seconds[15]
Berg Balance Scale (BBS)[15][edit | edit source]
Obtained score of 54 points
- Individuals with HD that are recurrent fallers (2≥ falls/year) are associated with BBS scores that are ≤40 points[15]
- In general populations, Berg notes that individuals who score <45 are at an increased risk of falls[16]
6 Minute Walk Test (6MWT)[17][edit | edit source]
Obtained score of 450.7 meters.
BORG-10 Rating of Perceived Exertion (RPE)[edit | edit source]
This tool will be used during aerobic exercise as an objective self-reported measurement, as well as to ensure safety.
Discussion of Other Relevant Outcome Measures[edit | edit source]
Patient Specific Functional Scale (PSFS)[edit | edit source]
The PSFS is a 10-point interval scale, where the scores of 10 = same levels as pre-injury, 0 = unable to perform activity. Individual score MCD: 3 points. Average score MCD: 2 points.
Timed Up and Go (TUG) and Berg Balance Scale (BBS)[edit | edit source]
A study was conducted on participants with HD who were in a hospital clinic and categorized as recurrent fallers (2≥ falls/year) and non-fallers (≤ 1 fall/year). The sample (n=24) had an average age of 56.6 (SD: ±11.7) years. The two groups were then assessed using the BBS and TUG to determine the threshold values of recurrent fall risk, where they found recurrent falls were associated with BBS scores ≤40 points and TUG times ≥14 seconds[15]
6 Minute Walk Test (6MWT)[edit | edit source]
Obtained 6MWT score is between average and +1SD of the expected for the stage of ‘manifested HD’ [17].
BORG-10 Rating of Perceived Exertion (RPE)[edit | edit source]
The MCID suggests a change of 2 units to have a large effect in perceived exertion during exercise interventions[18].
Clinical Impression[edit | edit source]
Physiotherapy diagnosis: Mr. McGee is a 41-year-old, right hand dominant male who is currently exhibiting bilateral chorea of the wrist and fingers in the upper extremity. He was previously diagnosed 6 months ago with early-stage Huntington’s disease. Mr. McGee presents with increased error during serial fine-motor tasks, specifically while writing on a chalkboard and typing on a keyboard.
Problem List[edit | edit source]
Body structure/function
- Progressive loss of aerobic fitness (i.e., aerobic deconditioning)
- Development of chorea in distal upper extremities
- Eventual loss of respiratory function due to disease progression[19]
Activity limitations
- Eventual loss of functional mobility including activities of daily living (ADLs) and instrumental activities of daily living (IADLs)
Participation Restrictions
- Inability to manipulate a piece of chalk while teaching
- Difficulty gripping handlebars while riding bicycle
Personal factors
- Lack of motivation/increased apathy
- Low mood, depression
- Increasingly sedentary lifestyle
Environmental factors
- Poor work-life balance (increased time working at home to grade papers)
- Stress with oncoming second child
- Financial factors like buying a new house and supporting his family
Intervention[edit | edit source]
Short-Term Goals[edit | edit source]
- Mr. McGee will take a 30-minute brisk walk with family at least 3 days per week for 2 weeks.
- Mr. McGee will score at least 56 points on the BBS after 3 weeks of physiotherapy.
- Mr. McGee will be able to write legibly and in a timely manner on a chalkboard during class lectures. This will involve writing the sentence “the quick brown fox jumps over the lazy dog,” which contains every letter in the alphabet. The physiotherapist records the amount of time required to complete the sentence at a self-selected pace when writing on a whiteboard in clinic. This time will be compared at future time points for amount of legibility. This will be assessed within the next session of physiotherapy.
Long-Term Goals[edit | edit source]
- Mr. McGee will be able to maintain his ability to type on a full-size keyboard with minimal errors and in a timely manner for at least 2 hours a day in 4 weeks' time.
- Mr. McGee will be able to ambulate 400 m without a gait aid from his vehicle to the classroom with a minimum RPE of 4 on the Borg-10 scale to focus on safety and efficiency. This will be completed within 4 weeks.
Treatment[edit | edit source]
| Intervention | Frequency | Intensity | Time/Volume | Type |
Education on energy conservation regarding physical activity and fatigue
*See below for a more detailed explanation on this topic[20] |
Initially and ongoing as required | N/A | N/A | N/A |
| Aerobic exercise training[21] | 3-5 days x week | Moderate to vigorous | ≥ 150 minutes x week | Recumbent bicycle / NuStep trainer, brisk walking[20] |
| Motor control training with gross, discrete, functional tasks of reaching, grasping, and manipulating with the upper extremity[22] | 3-5 days x week | Low to moderate | Random practice of ≥30-40 repetitions per task | Transferring a variety of objects (pan handle, keys, phone, paper clips, pens) from one area into a bin/container. |
| Motor control training with fine, serial/continuous, pen and chalk writing, and typing tasks[22] | 3-5 days x week | Low to moderate | Random practice of ≥30-40 repetitions per task | Chalk holder, keyboarding, handwriting with pen |
| Neuromotor exercise to maintain balance, coordination, and proprioception | 3-5 days x week | Low to moderate | ≥ 20-30 minutes x session | Yoga, Tai Chi[20] |
| Postural muscle strengthening[9] | 2-3 days x week, with at least 1-2 days rest between sessions | Moderate to vigorous | 2-4 sets of 8-12 repetitions | Exercises:
Bird dog Side plank McGill Curl up |
| Respiratory muscle training | Daily, or at least 3-5 days x week | 40% to 85% MSV | ≥ 15 minutes (initiate as tolerated) | Inspiratory Muscle Training with TheraBand resisted (HEP) |
Interdisciplinary Care Team Management[edit | edit source]
These are various specialists that are within a typical care team for Huntington’s disease. Currently, Mr. Magee is attending physiotherapy and is also receiving care from an occupational therapist, psychologist, and his family physician. Referrals are in place for Mr. Magee to receive care from a social worker and a speech language pathologist.
Social worker[23][edit | edit source]
- Management of familial “burden”, stress, fear of gene inheritance in children
- Mental health support, psychoeducation, counselling
- Advocacy in accessing programs to reduce health expenditures
Occupational therapist[22][edit | edit source]
- Handwriting strategy implementation and training
- Re: STG3 Mr. McGee would like train his ability write legibly and in a timely manner for as long as possible. Suggesting use of an outcome measure for writing legibility, such as the Handwriting Legibility Scale.
- Cognitive strategy implementation and training for stress management, mindfulness, self-efficacy, motivation, etc.
- Home environment modification - reducing clutter or slippery surfaces to prevent falls
- Assistive devices and/or modified tools to improve function regarding eating, manipulation of objects
Psychologist[24][edit | edit source]
- Observation of patient and family in home environment
- Assess disease burden on family and caregivers
- Determine functional effects of Huntington’s disease, including cognitive and mood assessment
Speech and language therapist[24][edit | edit source]
- Investigation on swallowing impairment
- Speech and language processing assessment
- Advice and therapy regarding speech, language and swallowing
Family Physician[24][edit | edit source]
- Assessment of disease and consequences for functional capacity
- Neurological testing and screening
- Medication prescription
Outcome[edit | edit source]
We followed up with Mr. McGee one year later and have summarized the results of his assessment below:
- Initial 6MWT distance of 450.7 meters increased by 34.2 meters to 484.9 meters.
- Upon observation, chorea has become more proximal in upper extremities only, affecting the elbow joint bilaterally in addition to previous symptoms at the wrist and fingers.
- BBS score has decreased from 54 to 44 (increased risk of falls in typical population)
- Mr. McGee’s progressive decline in speech function has necessitated referral to Speech Language Pathologist.
- Mr. McGee’s condition has put tremendous strain on his family’s mental health and well-being. His ongoing interdisciplinary care services are very costly, and these financial stresses have been negatively contributing to his family’s functioning. These factors suggest that Mr. McGee is a strong candidate for referral to a Social Worker.
- PSFS scores for:
- Holding and writing with chalk: 7 (initial: 9)
- Handwriting on paper: 5 (initial: 8)
- Typing on the keyboard: 6 (initial:9)
- Overall average: 6 (initial: 8.67)
Referrals[edit | edit source]
- Speech language therapist for assessment of speech impairment and assistive strategies.
- Social worker for familial support, counselling, and advocacy in accessing financial support.
- In-home community physiotherapy care from advanced practice neuroscience specialist physiotherapist for continuation of physiotherapy services.
Discharge[edit | edit source]
Discharge is not yet indicated for this patient, as Huntington’s disease is progressive and will worsen with time. Mr. McGee is currently managing his symptoms well and can continue physiotherapy treatment as needed.
Discussion[edit | edit source]
Rex McGee is a 41-year-old male diagnosed with early-stage Huntington’s disease. During the initial assessment, Mr. McGee presented with chorea in distal upper extremities and reported behavioural symptoms such as apathy. He showed limitations in activity measured by the outcome measures PSFS, TUG, BBS, 6MWT, and Borg-10. Treatment interventions were aimed at improving patient-stated functional tasks such as typing on a keyboard or writing on a chalkboard (e.g., handwriting task). Interventions also included treatments that would be beneficial for Mr. McGee in the future, as Huntington’s disease is a progressive degenerative disease (e.g., aerobic exercise, respiratory muscle training[19]).
The following treatments were implemented at the patient’s initial visit: respiratory training, aerobic training, postural and balance training, education on conservation of energy during movement, and training on functional reach and grasp activities. Respiratory muscle training was advised due to the inevitable effects of Huntington’s disease on respiratory muscles and the resultant atrophy[19]. Aerobic and functional reach and grasp activities were related to the patient’s individual goals of walking with his family and being able to manipulate objects at work. Since the patient reported having difficulty with fatigue, he was educated on energy conservation during movement to enable more efficient movement. Balance and postural muscle training were initiated for the same purpose, to achieve more functional movement and limit the risks of fatigue, in preparation for eventual atrophy of respiratory muscles. Busse[25] suggests that physiotherapy intervention soon after diagnosis of early to middle stages of Huntington's disease can have a positive impact on motor and functional performance and may even slow the decline. Therefore, implementing these treatments early in the disease will inevitably be beneficial for Mr. McGee.
Evidence-based clinical recommendations for patient management of Huntington’s disease continue to evolve as further research is developed. Physiotherapy interventions for Huntington's disease focus on maintenance of physical activity, physical functioning, and reduction of impairments secondary to mobility limitations[21]. Physiotherapy interventions that emphasize physical activity and exercise translate to patient perceptions of improved gait and balance, improved self-confidence and self-efficacy, and improved mindfulness and communication, especially when interventions emphasize personal enjoyment, meaningfulness, and relevance as much as possible[21]. The progressive nature of Huntington’s disease necessitates interdisciplinary care and continual engagement within the circle of care so that the patient and their family are optimally supported.
Self-study Questions[edit | edit source]
1. Which of the following measurement scales is considered the gold standard for assessing the progression of Huntington's disease motor symptoms?
- MDS-UPDRS
- MDS-UHDRS
- 6MWT
- TUG
2. Huntington’s disease is characterized by progressive degenerative changes in which of the following systems?
- Cognitive
- Behavioural
- Movement
- A and C
- All of the above
3. Based on what you know of the genetic nature of Huntington's disease, which is the correct statement below? Huntington’s disease is...
- Autosomal recessive
- Allosomal recessive
- Autosomal dominant
- Allosomal dominant
Answers: (1) 2; (2) 5; (3) 3
Explanation for (1): Answer 2 is correct. The Movement Disorder Society (MDS) has produced both Unified Parkinson's Disease Rating Scale and the Unified Huntington's Disease Rating Scale. The UHDRS measures the appearance of HD symptoms in the motor domain, and the patient's functional ability in the function domain.
Explanation for (2): Answer 5 is correct. HD is known to effect many dimensions of how people function. HD is not just a movement disorder due to the degree of interconnectivity of the subcortical structures, namely the basal ganglia and how it interfaces with the cortex and limbic system.
Explanation for (3): Answer 3 is correct. The gene for HD is found on chromosome #4 therefore it is autosomal. Allosomal (‘sex chromosomes’) are only for the chromosome pair #23. The HTT gene is dominant, meaning that only one of the two chromosomes in a pair possessing the HD gene will express the disease.
References[edit | edit source]
- ↑ 1.0 1.1 Mayo Clinic. Huntington’s disease [Internet]. Mayo Foundation for Medical Education and Research; 2014 [updated 2014 Apr 14; cited 2021 May 9]. Available from: https://www.mayoclinic.org/diseases-conditions/huntingtons-disease/symptoms-causes/syc-20356117
- ↑ Medline Plus. Huntington disease [Internet]. U.S National Library of Medicine; 2020 [updated 2020 Aug 18; cited 2021 May 9]. Available from: https://medlineplus.gov/genetics/condition/huntington-disease/
- ↑ 3.0 3.1 Warby SC, Montpetit A, Hayden AR, Carroll JB, Butland SL, Visscher H, et al. CAG Expansion in the Huntington Disease Gene Is Associated with a Specific and Targetable Predisposing Haplogroup. Am J Hum Genet. 2009 Mar 13;84(3):351–66. DOI: 10.1016/j.ajhg.2009.02.003
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 Waldvogel HJ, Kim EH, Tippett LJ, Vonsattel JP, Faull RL. The Neuropathology of Huntington's Disease. Curr Top Behav Neurosci. 2015;22:33-80. Doi: 10.1007/7854_2014_354
- ↑ 5.0 5.1 Neuroanatomy and Neuroscience at a Glance. Neuropathways of Huntington’s disease. [Image on Internet]. 2018 [cited 2021 May 8]. Available from: https://higheredbcs.wiley.com/legacy/college/barker/1119168414/ppt_slides/ch41.pptx
- ↑ Huntington’s Disease Society of America. What is Huntington’s Disease? [video on the Internet]. 2020 Apr 22. Available from: https://www.youtube.com/watch?v=ej7-OhSb4H0
- ↑ Roos RA. Huntington's disease: a clinical review. Orphanet J Rare Dis. 2010 Dec 20;5:40. doi: 10.1186/1750-1172-5-40
- ↑ Kirkwood SC, Su JL, Conneally PM, Foroud T. Progression of Symptoms in the Early and Middle Stages of Huntington Disease. Archives of neurology (Chicago). 2001;58(2):273–8. :doi
- ↑ 9.0 9.1 Paillard T, Noé F. Techniques and Methods for Testing the Postural Function in Healthy and Pathological Subjects. BioMed Research International. 2015 Nov 12;2015. doi:https://www.hindawi.com/journals/bmri/2015/891390/
- ↑ 10.0 10.1 10.2 Beglinger LJ, O'Rourke JJ, Wang C, Langbehn DR, Duff K, Paulsen JS, Huntington Study Group Investigators. Earliest functional declines in Huntington disease. Psychiatry research. 2010 July 30;178(2):414–418. doi: https://doi.org/10.1016/j.psychres.2010.04.030
- ↑ 11.0 11.1 11.2 Huntington’s Study Group [HSG]. Unified Huntington's disease rating scale: Reliability and consistency. Movement Disorder Society. 1996;11(2):136-142. doi:10.1002/mds.870110204
- ↑ Loy CT, McCusker EA. Is a Motor Criterion Essential for the Diagnosis of Clinical Huntington Disease? PLOS Currents Huntington Disease. 2013 Apr 11;1. doi: 10.1371/currents.hd.f4c66bd51e8db11f55e1701af937a419
- ↑ 13.0 13.1 Liou S. The HD Measuring Stick: Assessment Standards for Huntington’s Disease [Internet]. Stanford University; 2010 Jul 6 [cited 2021 May 10]. Available from: https://hopes.stanford.edu/assessment-standards-for-huntingtons-disease-severity/#fahn-rating-scale-physical-and-mental
- ↑ Stratford P, Gill C, Westaway M, Binkley J. Assessing Disability and Change on Individual Patients: A Report of a Patient Specific Measure. University of Toronto Press Journals. 1995;47(4):258-263. Doi: https://doi.org/10.3138/ptc.47.4.258
- ↑ 15.0 15.1 15.2 15.3 15.4 Busse ME, Wiles CM, Rosser AE. Mobility and falls in people with Huntington's disease. Journal of Neurology, Neurosurgery & Psychiatry. 2009;80:88-90. https://jnnp.bmj.com/content/80/1/88
- ↑ Berg K, Wood-Dauphinee S, Williams JI, Maki B. Measuring balance in the elderly: validation of an instrument. Can J Pub Health. 1992 Jul-Aug;83 Suppl 2:S7-11. doi: https://pubmed.ncbi.nlm.nih.gov/1468055/
- ↑ 17.0 17.1 Quinn L, Khalil H, Dawes H, Fritz NE, Kegelmeyer D, Kloos AD, Gillard JW, Busse M. Reliability and Minimal Detectable Change of Physical Performance Measures in Individuals With Pre-manifest and Manifest Huntington Disease. Physical Therapy. 2012 Jul 1;93(7):942–956. Doi: https://doi.org/10.2522/ptj.20130032
- ↑ Ries AL. Minimally Clinically Important Difference for the UCSD Shortness of Breath Questionnaire Borg Scale, and Visual Analog Scale. 2009 Aug 24;105-110. Doi: https://doi-org.proxy.bib.uottawa.ca/10.1081/COPD-200050655
- ↑ 19.0 19.1 19.2 Jones U, Busse M, Enright S, Rosser AE. Respiratory decline is integral to disease progression in Huntington's disease. European Respiratory Journal. 2016;48:585-588; DOI: 10.1183/13993003.02215-2015
- ↑ 20.0 20.1 20.2 20.3 Grover, P. Energy Expenditure During Basic Mobility and Approaches to Energy Conservation [Internet]. Rosemont, IL: PM&R KnowledgeNow; 2016 Aug 22 [updated 2020 Dec 15; cited 2021 May 10]. Available from: https://now.aapmr.org/energy-expenditure-during-basic-mobility-and-approaches-to-energy-conservation/#:~:text=Energy%20Conservation%20is%20one%20goal%20of%20human%20locomotion&text=This%20principle%20suggests%20that%20efficient,designed%20to%20minimize%20energy%20expenditure.&text=As%20a%20motor%20skill%2C%20walking,automatic%2C%20and%20goal-directed
- ↑ 21.0 21.1 21.2 Quinn L, Kegelmeyer D, Kloos A, Rao AK, Busse M, Fritz NE. Clinical recommendations to guide physical therapy practice for Huntington disease. American Academy of Neurology. 2020 Feb 4;94(5): 217-228. DOI: 10.1212/WNL.0000000000008887
- ↑ 22.0 22.1 22.2 American Occupational Therapy Association. Handwriting [Internet]. American Occupational Therapy Association Inc; 2021 [cited 2021 May 10]. Available from: https://www.aota.org/About-Occupational-Therapy/Patients-Clients/ChildrenAndYouth/Schools/Handwriting.aspx
- ↑ Vota S, Byrne M, Adcock C. Social work implementation into an outpatient neurology clinic: utilization and patient outcomes (P3.037). American Academy of Neurology. 2017 Apr 18;88(16 supplement). doi: https://n.neurology.org/content/88/16_supplement/p3.037
- ↑ 24.0 24.1 24.2 Veenhuizen RB, Kootstra B, Vink W, Posthumus J, van Bekkum P, Zijlstra M, Dokter J. Coordinated multidisciplinary care for ambulatory Huntington's disease patients. Evaluation of 18 months of implementation. Orphanet J Rare Dis. 2011 Nov 18;6(77). Doi: https://doi.org/10.1186/1750-1172-6-77
- ↑ Busse ME, Khalil H, Quinn L, Rosser AE. Physical Therapy Intervention for People With Huntington Disease. Physical Therapy. 2008 Jul 1;88(7):820–831. Doi: https://doi.org/10.2522/ptj.20070346