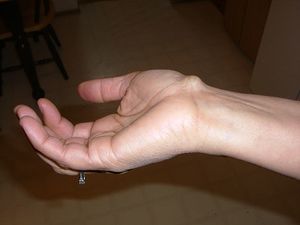
Ganglion Cyst
Original Editors - Lennert De Henau
Top Contributors - Evan Thomas, Kim Jackson, Lucinda hampton, Lennert De Henau, Vidya Acharya and Anas Mohamed
Definition/Description[edit | edit source]
A ganglion cyst or a Bible cyst is a benign swelling or bulge that often appears around or on joints and tendons in the hand or foot. A ganglion manifests as a subcutaneous limp or nodule. The size can change in time and it can also disappear completely.[1] See illustration:
In most cases (65%) the ganglion cysts are painful, especially in the beginning. But pain severity is not related with the size of ganglions. A ganglion in the musculoskeletal system is a spherical accumulation of fluid produce from an adjacent joint capsule or tendon sheath. A ganglion cyst is not a cyst because the collection of clear viscous fluid is contained in cavity, which is not lined by epithelium.[2]
Clinically Relevant Anatomy[edit | edit source]
A ganglion cyst is most frequently located around the dorsum of the wrist and the fingers. Along, the musculus extensor carpi radialis brevis is a common site of occurrence because it passes over the dorsum of the wrist joint [3]
88% of the cysts are located near the wrist joint and 11% near the foot and ankle[1]. In the wrist they are found especially at the scapho-lunate area.
Epidemiology /Etiology[edit | edit source]
Ganglion cysts are the most common soft tissue tumors of the hand and wrist[4] Ganglion is a mucin-filled hernia of synovial tissues from joint capsules or tendon sheaths due to one-way valve phenomenon. The cyst expands in size and the fluid cannot flow freely back into the synovial cavity. A ganglion cyst usually appears spontaneously without any particular cause. Anyone can be affected by ganglion cysts, but they occur 3 times as often in women as they do in men.
The occurrence of a ganglion cyst is related with osteoarthritis, and therefore most commonly seen in older patients. Ganglion cysts are predominantly seen in young adults and are rare in children[4]
The etiology of the ganglion cyst is unclear, although prior trauma, synovial herniation, internal derangement, and a degenerative process associated with mucin production are possible. Wrist ganglion cysts may connect to an adjacent joint in up to 70% of cases and are more common by women[5]
The degeneration of the connective tissue may be caused by an irritation or chronic damage causing the mesenchymal cells or fibroblasts to produce mucin[4].
Characteristics/Clinical Presentation[edit | edit source]
Ganglions are tumors that present adjacent to joints or tendons. The most common sites for ganglions are the dorsal aspect of the wrist near the scapholunate (SL) joint (60-70%), the volar wrist near the radioscaphoid joint or the pisotriquetral joint (18-20%), and the volar retinaculum between the A1 and A2 pulleys (10-12%)[6]. Ganglions are usually minimally symptomatic. However, depending on the location of the cyst, patients may present with a myriad of symptoms such as dull aching pain, change in size, spontaneous drainage, and sensory nerve dysfunction[7].
Associated Injuries/Differential Diagnosis[edit | edit source]
Tenosynovitis involves inflammation of the tendon and tendon sheath. Examples of tenosynovitis include de Quervain tenosynovitis of the wrist, volar flexor tenosynovitis (i.e.trigger finger), pyogenic flexor tenosynovitis, which can be from gonococcal infections and other infectious etiologies[8].
Lipomas are benign tumors composed of mature fat cells. They are the most common benign mesenchymal tumor. Lipomas are found in the subcutaneous tissues and, less commonly, in internal organs. Lipomas typically develop as discrete rubbery masses in the subcutaneous tissues of the trunk and proximal extremity. Lipomas usually are a few centimeters in size and can be removed by surgical excision or liposuction.
A hamartoma is a benign (noncancerous) tumorlike malformation made up of an abnormal mixture of cells and tissues found in areas of the body where growth occurs. It is considered a developmental error and can occur at a number of sites[9]
Dupuytren's contracture is a fixed flexion contracture of the hand where the fingers bend towards the palm and cannot be fully extended (straightened). It is an inherited proliferative connective tissue disorder which involves the palmar fascia of the hand .
Diagnostic Procedures[edit | edit source]
Ultrasound was used to confirm the diagnosis of a ganglion cyst and provide guidance for needle aspiration, fenestration, and subsequent steroid-anesthetic mixture injection. Scan was performed with a 12-5-Mhz linear transducer on an IU22 scanner[10]. Other methods that are being used are MRI scans. This depends where the ganglion cyst is located. Using magnetic resonance imaging is essential for the differential diagnosis, such as other masses like vascular lesions and lipomas. Another diagnostic tool in the evaluation of a ganglion cyst is the use of a radiopaque contrast dye. Gangliography is a method of evaluating the size and extent of a ganglion cyst, and is performed as an adjunct to aspiration. After the injection of a few. milliliters of contrast dye, a radiograph is obtained, and the extent of the lesion is more easily visualized[11].
Outcome Measures[edit | edit source]
The following outcome measures can be used:
- Grip and pinch strengths and wrist motion can be measured with standard assessment instrumentation.
- Visual Analogue Pain Scale
- Disabilities of the Arm, Shoulder, and Hand questionnaire.[12]
Examination[edit | edit source]
The diagnosis ganglion cyst can be made by the physician on the basis of a clinical trial or based on the history. If we think wear or trauma is the cause, we introduce some additional investigations: ultrasound, X- ray or an MRI. These studies are not painful. The sensitivity of a MRI is approximately 80% en has a specificity of about 50%. These results are given by a standard of intra-operative determination of the disease[13]. The MRI is performed when atypical features or neurologic symptoms are present and in specific preoperative settings. On MRI a cyst has a low signal intensity compared with muscle. Ultrasound is often sufficient for assessing typical cysts. It may be done to detect the presence of occult cysts. To exclude any more serious underlying pathology, radiographs in anteroposterior and lateral view are obtained. On ultrasound a simple cyst is well circumscribed and anechoic with posterior acoustic enhancement. The plastic surgeon will also conduct research into the physical of a existence of a possible trigger finger[14]. The physicians can often make a diagnosis on the basis of the phenomena. These phenomena are a subcutaneous lump, lump or nodule of that size can change. It is usually a soft bulge like the size of a pea. In the beginning, ganglion cysts are painful. Besides pain, a ganglion limiting movement causes loss of strength, mostly due to pressure from the swelling on adjacent tendons or nerves. In most cases, additional studies may be omitted[15].
Medical Management[edit | edit source]
Many ganglion cysts (38%-58%) can disappear without any treatment at all. Various treatments have been proposed over the years. Some include telling people with cysts without symptoms not to worry, using a needle to remove the cyst’s contents (aspiration) or surgery.[16][17]
Aspiration usually includes placing a needle into the cyst, drawing the liquid material out and injecting a steroid compound into the empty cavity (which acts as an anti-inflammatory agent).[16][17] Aspiration is beneficial and simple option for acute management but appears to have little long-term impact on resolution. Aspiration appears to be significantly more successful in ganglia of the flexor tendon sheath of the hand with success up to 60% or 70% of the time.[18]
Surgical excision remains the gold standard for the treatment of ganglion cysts. The surgical techniques include excision of the entire ganglion complex, including cyst, pedicle, and a cuff of the adjacent joint capsule. After the surgery, the wrist is sometimes getting a splint to keep it from moving[16][17]. It is to prevent the wrist motion from pumping synovial fluid through the one-way valve mechanism and refilling the cyst. This has proven no more effective than simple aspiration and in postoperative patients leads to prolonged joint stiffness and decreased range of motion.[18] Most studies, even with repeat aspirations, demonstrate a success rate of only 30-50%. If you compare aspiration/injection and surgical removal, in general, cysts return less often after surgery.[16][17] A higher recurrence rate is found by patients with a longer history, larger ganglia, and less experienced surgeons. The ganglion location, age and gender have no influence on the recurrence rate.[19]
Physical Therapy Management[edit | edit source]
A ganglion cyst can have consequences for the daily activities. Surgical excision is not always done, sometimes the cyst can disappear without any treatment at all or with therapy alone. The therapy is aimed in the normal use of the hand. If therapy is given after surgical excision than the accent is at exercise, splint therapy, edema relief and scar tissue reduction.
Like pointed out above the main goal of physical therapy is to restore the normal use of the hand. Therefore we need to regain full mobility of all the joints of the hand. In most protocols following exercises are used to achieve full mobility[20]:
- PROM (passive ROM) exercises: there are 3 finger joints (MCP, PIP and DIP-joints) and 2 wrist joints (radiocarpal en mediocarpal joint). It’s important that all the possible movements are trained.
- PNF (proprioceptive neuromuscular facilitation) exercises: the finger is kept in flexion by the therapist. The patient needs to keep this position for a while (active), afterwards the patient relaxes the finger. Repeat for al fingers.
- Tendon gliding exercises: from wrist flexion with finger extension to wrist extension with finger flexion.
- Blocking exercises: lay your hand palm side up on a table. With your opposite hand grasp and hold the affected finger at the middle section just below the end joint. Bend and straighten the finger at the end joint only while holding the rest of the finger straight. Repeat for all joints and fingers.
It’s also important to reduce scar tissue to restore functional mobility, to improve range of motion and to decrease pain. Scar tissue remodeling occurs as you start to stretch and pull on it. Stretching of, in this case, the hand helps to align the collagen fibers to allow them to return to normal. This realignment of the collagen fibers makes the tissue better able to tolerate the forces that are placed on it during the day. Another way to help remodel scar tissue in the skin is massage. This can also help loosen any adhesions between the scar and the underlying tissue and fascia. Stretching, scar massage along with flexibility and strengthing exercises can help loosen the scar tissue and ensure that proper remodeling takes place.[21][22]
With specialized therapy there is a lower recurrence rate and a faster recovery. Patients with a ganglion cyst are able to use their hand back, 2 weeks after the surgical excision.
References[edit | edit source]
- ↑ 1.0 1.1 @inproceeding Camasta 2012 EXCISIONOT, EXCISION OF THE GANGLION CYST, Craig A. Camasta 2012 Available from: https://www.semanticscholar.org/paper/EXCISION-OF-THE-GANGLION-CYST-Camasta/67d2f2944bbe3a87f570fcf41ff1d4e92cc92467 (last accessed 11.10.2019)
- ↑ Syed M. et al. Comparative study of two methods for treatment of dorsal wrist ganglion, the journal of Pakistan orthopaedic association, February 2010 vol. 22 No.1 53-57
- ↑ McNabb JW. A practical guide to joint & soft tissue injection & aspiration: an illustrated text for primary care providers. Lippincott Williams & Wilkins; 2009 Nov 1. Available from: https://shop.lww.com/Practical-Guide-to-Joint---Soft-Tissue-Injections/p/9781451186574 (last accessed 11.10.2019)
- ↑ 4.0 4.1 4.2 Thornburg LE. Ganglions of the hand and wrist. JAAOS-Journal of the American Academy of Orthopaedic Surgeons. 1999 Jul 1;7(4):231-8. Available from: https://www.ncbi.nlm.nih.gov/pubmed/10434077 (last accessed 11.10.2019)
- ↑ Wang G, Jacobson JA, Feng FY, Girish G, Caoili EM, Brandon C. Sonography of wrist ganglion cysts: variable and noncystic appearances. Journal of ultrasound in medicine. 2007 Oct;26(10):1323-8. Available from: https://www.ncbi.nlm.nih.gov/pubmed/17901135 (last accessed 11.10.2019)
- ↑ Hotchkiss RN, Pederson WC, Kozin SH, Cohen MS, Wolfe SW. Green's Operative Hand Surgery, 2-Volume-Set. Elsevier; 2017.Available from: https://www.elsevier.com/books/greens-operative-hand-surgery-2-volume-set/wolfe/978-1-4557-7427-2 (last accessed 13.10.2019)
- ↑ Peters F, Vranceanu AM, Elbon M, Ring D. Ganglions of the hand and wrist: determinants of treatment choice. Journal of Hand Surgery (European Volume). 2013 Feb;38(2):151-7. Available from: https://www.ncbi.nlm.nih.gov/pubmed/22508801 (last accessed 13.10.2019)
- ↑ Marx J, Walls R, Hockberger R. Rosen's Emergency Medicine-Concepts and Clinical Practice E-Book. Elsevier Health Sciences; 2013 Aug 1. Available from: https://www.worldcat.org/title/rosens-emergency-medicine-concepts-and-clinical-practice-vol-3/oclc/278499349 (last accessed 13.10.2019)
- ↑ Hanssen AM, Fryns JP. Cowden syndrome. Journal of medical genetics. 1995 Feb 1;32(2):117-9. Available from: https://www.ncbi.nlm.nih.gov/pubmed/20580873 (last accessed 13.10.2019)
- ↑ Saboeiro GR, Sofka CM. Ultrasound-guided ganglion cyst aspiration. HSS journal. 2008 Sep 1;4(2):161-3. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2553163/ (last accessed 13.10.2019)
- ↑ Suen M, Fung B, Lung CP. Treatment of ganglion cysts. ISRN orthopedics. 2013 May 28;2013. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4045351/ (last accessed 13.10.2019)
- ↑ Scott G. Edwards, Prospective Outcomes and Associations of Wrist Ganglion Cysts Resected Arthroscopically, American Society for surgery of the Hand, 2009;34A:395-400
- ↑ Goldsmith, S et all. Magnetic resonance imaging in the diagnosis of occult dorsal wrist ganglions. Journal of hand surgery-european volume. October 2008, vol: 33E issue 5, p595-599
- ↑ Freire V, et All, Imaging of hand and wrist cysts: A clinical approach. American journal of roentgenology. November 2012, volume 199 number 5
- ↑ http://www.handclinic.nl/content.asp?id=299
- ↑ 16.0 16.1 16.2 16.3 Elisa E. Aumont, MD, Ganglion Cyst, emedicinehealth
- ↑ 17.0 17.1 17.2 17.3 Harvey V. Thommasen et al. Management of the occasional wrist ganglion, society of Rural Physicians of Canada, 2006
- ↑ 18.0 18.1 Warren Gude, Morelli Vincent, Ganglion cysts of the wridt: pathophysiology, clinical picture and management, Curr Rev Musculoskelet Med. 2008 December; 1 (3-4): 205-211
- ↑ Schicke, S. H. et All. Ganglia of the hand and wrist: a retrospective study on the origination of recurrences. Handchirurgie mikrochirurgie plastische chirurgie. Oct 2011 Volume: 43 Issue: 5, pages: 298-301
- ↑ Evelyn J. Mackin, Anne D. Callahan, Terri M. Skirven, Lawrence H. Schneider, and A. Lee Osterman, editors; and James M. Hunter, editor emeritus. St. Louis: Mosby; 2002. 2109 pages.
- ↑ Kisner, C., & Colby, L. A. (1996). Therapeutic exercise: Foundations and techniques. (3 ed.). Philadelphia: FA Davis.
- ↑ Hertling, D. (2006). Management of common musculoskeletal disorders. (4th ed.). Philadelphia: Lippincott Williams & Wilkins