Foundational Concepts in Sports Medicine
Original Editor - Wanda van Niekerk based on the course by James Laskin
Top Contributors - Wanda van Niekerk and Jess Bell
Foundation Blocks in Sports Medicine[edit | edit source]
Disablement Models[edit | edit source]
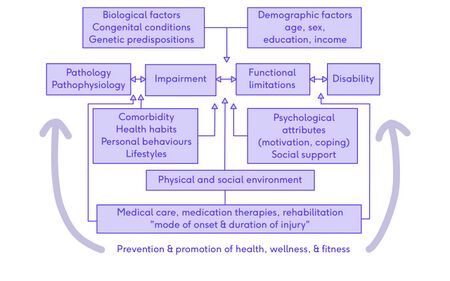
Disablement models are conceptual models which provide a framework for clinical practice and research.[1] These models are tools that are used to define impairment and more recently functioning and are utilised by governments and society to device strategies and policies for meeting the needs of people who have a loss in function as a result of health conditions, disease or injury. These models are used in healthcare as a way to organise clinical practice decisions. It creates a common language among healthcare professionals and facilitates patient-centred and whole-person healthcare.[1] Disablement models are an important piece of evidence-based practice. Evidence-based practice entails clinician expertise, research evidence and patient preferences and values. It is key to incorporate research evidence and the values of patients into their care model. A disablement model facilitates this incorporation.[1]
- The disablement model starting point may be pathology or pathophysiology (such as an injury)
- This may lead to an impairment (such as pain or loss of range of motion) and because of that there is a functional limitation (i.e. the inability to do some activity or having difficulty performing the activity).
- This leads to the determination of disability (i.e. the individual's perception of how specific functional limitations affect their activities of daily living (ADL), instrumental activities of daily living (IADL), work ability, participation in recreational activities or sport).
- Other components that play a role are:
- Biological factors
- Congenital factors
- Genetic predisposition
- Demographic factors such as age, sex, education, income
- Comorbidities
- Health habits
- Personal behaviours
- Lifestyle
- Psychological attributes (motivation, coping)
- Social support
- Physical and social environment
- Medical care, medication therapies, rehabilitation and mode of onset and duration of injury
From a sports perspective, prevention and promotion of health, wellness and fitness help mediate the development of pathology or the outcome.[2]
The International Classification of Functioning, Disability and Health (ICF) is a disablement model used worldwide. Read more about it here: Introduction to the International Classification of Functioning, Disability and Health (ICF)
Anatomy and Biomechanics[edit | edit source]
A good understanding of anatomy and biomechanics is critical in sports medicine. It adds value and understanding to mechanisms of injury, prevention of injury and also the treatment of the specific structure and any collateral damage elsewhere in the kinetic chain. A relevant definition of biomechanics for sports medicine clinicians is[3]:
"The application of mechanical principles in the study of living organisms."[3]
- To brush up on Biomechanics, see:
- For more on Biomechanics and Sport, see:
- For more on Anatomy, see:
- Musculoskeletal Anatomy available on Plus
Exercise Physiology[edit | edit source]
An understanding of the basic principles of the body's response to an exercise stimulus is vital for the performance and rehabilitation of athletes. This knowledge guides sports clinicians in terms of exercise prescription, rehabilitation and prevention of injury.
You can read more here:
Continuum of Mechanical Stress[edit | edit source]
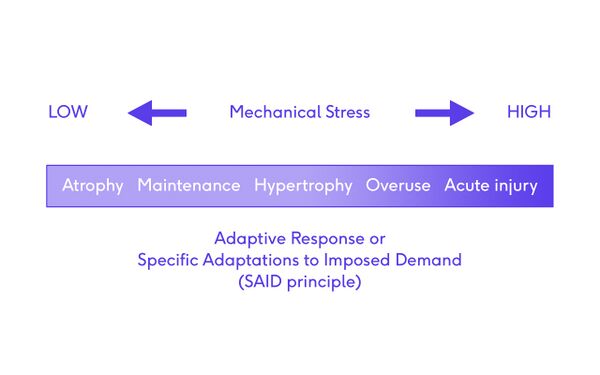
The different tissues in the body will respond differently under different levels of stress. Biological tissues show characteristic responses to physical stress and each response will occur within a defined range along the continuum of mechanical stress. The responses include:
| Response to Mechanical Stress | Explanation of Response |
|---|---|
| Atrophy | Physical or mechanical stress levels lower than the maintenance range leads to a decreased tolerance in tissue to subsequent stresses |
| Maintenance | Physical or mechanical stress levels in the maintenance range result in no apparent tissue change |
| Hypertrophy | Physical or mechanical stress levels that exceed the maintenance range (overload) lead to an increased tolerance in tissue to subsequent stresses |
| Overuse | High levels of physical stress may lead to the overuse of tissue structures |
| Acute Injury | Excessively high levels of physical stress may lead to tissue injury |
SAID Principle[edit | edit source]
SAID = Specific Adaptations to Imposed Demand
- The SAID principle is a framework on which strength and conditioning programmes can be designed[5]
- Biological tissue adapts to the demands, or the lack of demand, imposed on it
- Components of the SAID principle include[5]:
- Overload - tissue is challenged with increased intensity and/or duration
- Specificity - the tissue will adapt to the activity trained
- Read more: The Basic Principles in Exercise Physiology
General Physical Rehabilitation Pyramid[edit | edit source]
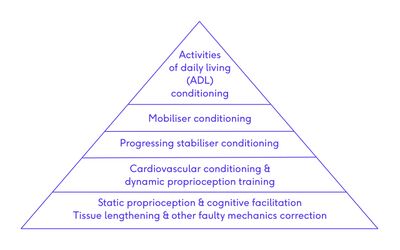
The general physical rehabilitation pyramid includes five tiers. The bottom tier can be considered the first and most important. Individuals should be evaluated for the components of each tier and the clinician needs to be satisfied that progression to the next tier will not hinder the healing and rehabilitation process.[7]
- General physical rehabilitation pyramid tiers (Tier 1 (bottom tier) to Tier 5 (top tier))
- Static proprioception and cognitive facilitation; correction of faulty mechanics and tissue lengthening
- Cardiovascular conditioning and dynamic proprioception training
- Progressing stabiliser conditioning
- Mobiliser conditioning
- ADL conditioning (or in sports medicine: sport-specific conditioning)
Sports Rehabilitation Pyramid[edit | edit source]
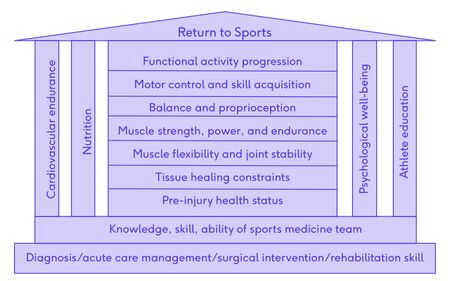
Return to sport or physical activity is the goal and important to athletes recovering from injury. This return to sport goal is supported by multiple components such as:
- Cardiovascular endurance
- Nutrition
- Psychological well-being
- Athlete education
- Building blocks of rehabilitation considerations such as:
- Pre-injury health status
- Tissue healing constraints
- Muscle flexibility and joint stability
- Muscle strength, power and endurance
- Balance and proprioception
- Motor control and skill acquisition
- Functional activity progression
All of the components and considerations mentioned above are supported by a sports medicine team consisting of professionals who have the relevant knowledge, skills and abilities.
Underpinning all of the above are:
- Skills to diagnose accurately
- Acute care management skills
- Relevance and influence of surgical intervention
- Excellent rehabilitative skills and competencies
Responsibilities of the Sports Physiotherapist[edit | edit source]
Prevention[edit | edit source]
- Educate and instruct
- Gledhill et al.[8] recommend three strategies for clinicians to empower athletes during their return to sport. These are:
- Educate
- Involve
- Collaborate
- Read more about these strategies here: Educate, involve and collaborate: three strategies for clinicians to empower athletes during return to sport[8]
- Monsonis et al.[9] investigated perspectives about sports injury prevention from various stakeholders (athletes, coaches, managers and healthcare professionals). It was evident that education, communication, knowledge, and empowerment were all fundamental role players in injury prevention.
- Gledhill et al.[8] recommend three strategies for clinicians to empower athletes during their return to sport. These are:
- Bracing and taping
- Read more on:
- Monitor the safety of participation
- Ensure a safe sports participation environment (check for any possible risk areas on the field)
- Emergency safety plan in case of serious or catastrophic injuries
- Being on the sideline can provide sports medicine professionals the chance to witness and evaluate an athlete's pathology at the time of injury
- It is vital to develop and practise an Emergency Action Plan (EAP) to efficiently administer medical care at sports events[10]
- Read more:
- Facilitate safe conditioning
- Ensure proper instruction on how to perform the exercise
- Check that equipment is safe to use
- Sanitation
- Continuing physical activity or exercise may prolong or aggravate infectious diseases[12]
- Infection control measures should be followed. These include hand washing, cleaning of facilities, preventing shared use of personal items (i.e. water bottles)[12]
- Early diagnosis can reduce transmission risk, reduce time loss from play and prevent larger breakouts[12]
- Promotion of nutritional concerns
Recognition, Evaluation and Assessment[edit | edit source]
- History
- Observation
- Palpation
- Special tests
- Assessment
- Educate
- Inform
- Plan
Immediate Care[edit | edit source]
- Initiate emergency medical care procedures[11]
- Stabilise musculoskeletal injuries
- Facilitate referral when appropriate
- Educate members of the health care team on immediate care procedures[11]
- Read more:
- Creating a model of best practice: the match day emergency action protocol[15]
- Invited clinical suggestion: "On the sidelines" - Emergency care basics for the sports physical therapist[16]
- Perceived management of acute sports injuries and medical conditions by athletic trainers and physical therapists[17]
Treatment, Rehabilitation and Reconditioning[edit | edit source]
- Therapeutic modalities
- Therapeutic exercises
- Reassess and treat
- Educate
- Provide guidance
Organisation and Administration[edit | edit source]
- Plan of action
- Write policies and procedures concerning:
- Safe participation
- Facilities
- Timely care
- Safety
- Legal compliance
- Sanitation
- Read more: Sport safety policy changes: Saving lives and protecting athletes[18]
- Manage resources
- Maintain records
Professional Development and Responsibilities[edit | edit source]
- Demonstrate professional conduct
- Continuing education
- Adhere to professional ethics
- Follow legal responsibilities
Work and Volunteer Settings[edit | edit source]
- High schools
- Colleges and universities
- Professional sports
- Sports medicine clinics
- Clinical health care programmes
- Industrial health care programmes
- Health and fitness clubs
- Local sports club
Interesting read on: Growing sports physiotherapy experts takes a village - technical, creative and contextual learning doesn't happen in a vacuum[19]
Resources[edit | edit source]
Professional Sports Medicine Organisations[edit | edit source]
- International Federation of Sports Medicine (FIMS)
- International Federation of Sports Physical Therapy (IFSPT)
- National Athletic Trainers' Association (NATA)
- American College of Sports Medicine (ACSM)
- American Orthopaedic Society for Sports Medicine (AOSSM)
- American Academy of Orthopaedic Surgeons (AAOS)
- National Strength and Conditioning Association (NSCA)
- American Academy of Paediatrics, Sports Committee (AAP)
- American Academy of Sports Physical Therapy
- National Collegiate Athletic Association (NCAA) Committee on Competitive Safeguards and Medical Aspects of Sports
- British Association of Sport and Exercise Medicine (BASEM)
- Swiss Sports Physiotherapy Association (SSPA Sportfisio)
- Physios in Sport
- Sports Medicine Australia
- Sports and Exercise Physiotherapy New Zealand
- South African Sports Medicine Association (SASMA)
Sports Medicine Journals[edit | edit source]
- American Journal of Physical Medicine and Rehabilitation
- British Journal of Sports Medicine
- Clinical Journal of Sports Medicine
- Clinical Orthopaedics and Related Research
- Current Opinion in Orthopaedics
- Current Opinion in Rheumatology
- Exercise and Sports Science Reviews
- Bone and Joint Journal
- Journal of Bone and Joint Surgery
- Journal of Orthopaedic Trauma
- Journal of Pediatric Orthopaedics
- Medicine and Science in Sports and Exercise
- Sports Medicine and Arthroscopy Review
- Sports Medicine
- Techniques in Foot and Ankle Surgery
- Scandinavian Journal of Medicine and Science in Sports
- Physical Therapy in Sport
Guidelines for Sports Medicine[edit | edit source]
- NCAA Sports Medicine Handbook
- Sports Medicine Guidelines
- Sports Medicine Australia: Policies and Guidelines
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Snyder AR, Parsons JT, Valovich McLeod TC, Curtis Bay R, Michener LA, Sauers EL. Using disablement models and clinical outcomes assessment to enable evidence-based athletic training practice, part I: disablement models. Journal of athletic training. 2008 Jul;43(4):428-36.
- ↑ Laskin, J. Foundational Concepts in Sports Medicine Course. Plus. 2022
- ↑ 3.0 3.1 Hall SJ. Basic Biomechanics, 8e. McGraw-Hill; 2019.
- ↑ Mueller MJ, Maluf KS. Tissue adaptation to physical stress: a proposed “Physical Stress Theory” to guide physical therapist practice, education, and research. Physical therapy. 2002 Apr 1;82(4):383-403.
- ↑ 5.0 5.1 Johnson AM, Sandage MJ. Exercise science and the vocalist. Journal of Voice. 2021 Jul 1;35(4):668-77.
- ↑ Training for 600. Exercise Science Foundations 2 - S.A.I.D. Principle. Available from: https://www.youtube.com/watch?v=iGbjL0qfbh4 [last accessed 27/10/2022]
- ↑ Stark TW. Introduction of a pyramid guiding process for general musculoskeletal physical rehabilitation. Chiropractic & Osteopathy. 2006 Dec;14(1):1-6.
- ↑ 8.0 8.1 Gledhill A, Forsdyke D, Goom T, Podlog LW. Educate, involve and collaborate: three strategies for clinicians to empower athletes during return to sport. British Journal of Sports Medicine. 2022 Mar 1;56(5):241-2.
- ↑ 9.0 9.1 Monsonís OB, Verhagen E, Kaux JF, Bolling C. ‘I always considered I needed injury prevention to become an elite athlete’: the road to the Olympics from the athlete and staff perspective. BMJ open sport & exercise medicine. 2021 Dec 1;7(4):e001217.
- ↑ McDermott ER, Tennent DJ, Patzkowski JC. On-field Emergencies and Emergency Action Plans. Sports Medicine and Arthroscopy Review. 2021 Dec 3;29(4):e51-6.
- ↑ 11.0 11.1 11.2 Patterson M, Gordon J, Boyce SH, Lindsay S, Seow D, Serner A, Thomson K, Jones G, Massey A. Set-piece approach for medical teams managing emergencies in sport: introducing the FIFA Poster for Emergency Action Planning (PEAP). British Journal of Sports Medicine. 2022 Feb 13.
- ↑ 12.0 12.1 12.2 Herrero H. Sports and Infections. InInjury and Health Risk Management in Sports 2020 (pp. 281-286). Springer, Berlin, Heidelberg.
- ↑ Grozenski A, Kiel J. Basic Nutrition for Sports Participation, Part 1: Diet Composition, Macronutrients, and Hydration. Current Sports Medicine Reports. 2020 Oct 1;19(10):389-91.
- ↑ 14.0 14.1 Tscholl PM. Let us spend time pitchside for our athletes’ benefit: a call to broaden collaboration by Sport and Exercise Medicine Switzerland (SEMS).
- ↑ Shah R, Chatterjee AD, Wilson J. Creating a model of best practice: the match day emergency action protocol. British Journal of Sports Medicine. 2018 Dec 1;52(23):1535-6.
- ↑ Smith DD. Invited clinical suggestion:“on the sidelines”-emergency care basics for the sports physical therapist. International Journal of Sports Physical Therapy. 2011 Mar;6(1):59.
- ↑ Wallace A, Briggs MS, Onate J, DeWitt J, Rinehart-Thompson L. Perceived management of acute sports injuries and medical conditions by athletic trainers and physical therapists. International journal of sports physical therapy. 2021;16(6):1548.
- ↑ Adams WM, Casa DJ, Drezner JA. Sport safety policy changes: saving lives and protecting athletes. Journal of athletic training. 2016 Apr;51(4):358-60.
- ↑ Phillips N, Paterson C. Growing sports physiotherapy experts takes a village—technical, creative and contextual learning doesn’t happen in a vacuum. British Journal of Sports Medicine. 2020 May 1;54(9):499-501.