Conceptual Models of Disability and Functioning
Original Editors - Naomi O Reilly and ReLAB-HS
Top Contributors - Naomi O'Reilly, Admin, Tarina van der Stockt, Kim Jackson, Oyemi Sillo, Wanda van Niekerk, Lucinda hampton, Ashmita Patrao and Olajumoke Ogunleye
Introduction[edit | edit source]
Models of disability and functioning are tools that are used to define impairment and more recently functioning, which are utilised by governments and society to devise strategies and policies for meeting the needs of those who have a loss in function as a result of health conditions, disease or injury. While they provide a framework in which we can gain an understanding of impairment, disability and functioning, there is lots of contention, and discussion around the models. Overall these models reveal or reflect how society provides or limits access to work, goods, services, economic influence and political power for people with a disability or loss of function, and provide some insight into the attitudes, conceptions and prejudices in society. These models have changed as society has changed, and understanding the development and use of these models can provide us with a continuum on the changing societal attitudes towards disability and loss of functioning. [1]
Medical Model[edit | edit source]
Historically approaches towards health and disease has been very much focused on the medical or biological model where a person’s ill-health was exclusively thought to be related to pathology and treated purely by medical means. In more recent times thinking has moved towards a more functional model. The medical or biomedical model of disability is focused on pathology and impairment, which describes disability as a consequence of a health condition, disease or injury/trauma that can disrupt the functioning of a person in a physiological or cognitive way. It then focuses on the prevention or treatment of the condition, which is generally lead by the physician who directs the delivery of the service, with the physician being the decision-maker in the process. There has been a lot of discontent with this model, which some may feel assumes several unhelpful notions about the nature of the disability. This model was born around the First World War, when there was a strong philosophy of the doctor telling injured servicemen how to behave, how to get better, and how to get back as quickly as possible to active duty. Such a model may have been appropriate in that cultural context but not in wider society today.
Social Model[edit | edit source]
“The Social Model frames disability as something that is socially constructed. Disability is created by physical, organisational and attitudinal barriers and these can be changed and eliminated. This gives us a dynamic and positive model that tells us what the problem is and how to fix it. It takes us away from the position of "blaming" the individual for their shortcoming. It states that impairment is, and always will be, present in every known society, and therefore the only logical position to take, is to plan and organise society in a way that includes, rather than excludes, disabled people." Barbara Lisicki, 2013 [3]
The social models of disability frame disability not as an underlying medical condition or pathology but rather as secondary to the social, legislative, and attitudinal environment in which the person lives, best summarised by the definition of disability from Disabled Peoples’ International:
[3]
"the loss or limitation of opportunities to take part in the normal life of the community on an equal level with others, due to physical or social barriers.".
Although a person’s abilities may be different, the disability occurs secondary to a society that either actively discriminates against the person with an impairment or fails to account for their specific individual needs. For example, a person with hearing loss is not disabled by the hearing loss itself, but by the environment not providing the appropriate resources for that person. [1]
This considers a distinction between the terms impairment and disability, where the term "impairment" is used to refer to the actual attributes that affect a person, such as the inability to walk or breathe independently, while the term "disability" refers to the restrictions caused by society when it does not give equivalent attention and accommodation to the needs of individuals with impairments. Social models are effectively conceived in order to defend autonomy and personal freedoms despite the level of functioning.[1]
Thus if this model works there should be no disability within a fully developed society, as removal of attitudinal, physical and institutional barriers will improve the lives of people with a disability, and ensure the same opportunities on an equitable basis.
Human Development Model - Disability Creation Process (HDM-DCP)[edit | edit source]
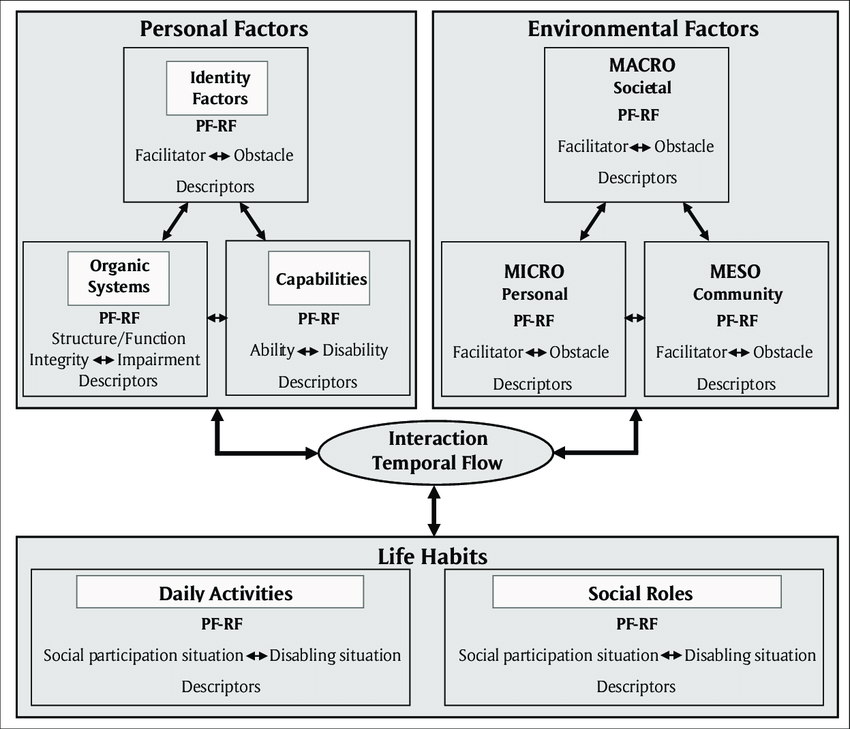
Designed to focus on the adaptation, rehabilitation, social participation and exercise of human rights of people with a disability and their families, the Human Development-Disability Creation Process, is a conceptual model that aims to document and explain the causes and consequences of disease, trauma, and other effects on the development of the person. Research, directed by Patrick Fougeyrollas in 1988, led to the development of the initial model in 1998,[6] which differed from other human development models at the time in that it incorporated the concepts of “risk factors”, “organic systems” and “capabilities” and was the first introduction to the environmental factors dimension highlighting the interaction between impairments, disabilities and environmental obstacles, and defined disabling situations as the result of this interaction. [6]
This model recognises the role that rehabilitation has in allowing an individual to reinforce their abilities, while compensating for the loss in function and consider that “environmental factors” found in a person’s or population’s environment may be either facilitators or obstacles e.g. a prejudice, the lack of assistance or resources, the lack of accessibility at home and at school, a problem in obtaining adapted printed information or moving around with the help of accessible signage. It allows us to view the impact of the environment, and provides us with an indicator of the quality of social participation, which is measured over a continuum or scale ranging from an optimal situation of social participation to a complete disabling situation.[6]
Biopsychosocial Model[edit | edit source]
The Biopsychosocial Model of disability is an attempt to account for both the social and biomedical models of disability. First conceptualised by George Engel in 1977, it suggests that to understand a person's medical condition it is not simply the biological factors that need to be considered, but also the psychological and social factors [7].
- Bio (physiological pathology)
- Psycho (thoughts, emotions and behaviours such as psychological distress, fear/avoidance beliefs, current coping methods and attribution)
- Social (socio-economical, socio-environmental, and cultural factors such as; work issues, family circumstances and benefits/economics)
Traditionally within a medical model the primary skills of a doctor are most often in the area of pathology and impairment, whereas those of the health and social care professionals are more based on activity and participation, while within this biopsychosocial model the Rehabilitation Team should to be able to take an informed overview considering the whole person, and ensure a holistic approach to rehabilitation that is person centred.
The World Health Organisation International Classification of Functioning, Disability and Health is underpinned by the Biopsychosocial Model. There has been some controversy around incorporating aspects of health within a model of disability from those that use the social model of disability, as they would define disability as being solely due to a lack of response of society to change the environment to accommodate the needs of the individual. The full ICF is a detailed and lengthy document, which recognises the importance of not only of describing the functioning of an individual but also placing such functioning into its social context. [8]
Summary[edit | edit source]
These conceptual models should not be utilised purely to define disability but should consider functioning, and more importantly to provide an understanding of the impact of impairment and context-specific factors on function. The models have applications for quantitative and qualitative assessment of disability and functioning, to inform needs and resources, monitor costs, direct social policy, and maximize awareness and acceptance globally[9].
Rehabilitation medicine should focus on function, which is considered an umbrella term for body functions, body structures, activities and participation. It denotes the positive aspects of the interaction between an individual (with a health condition) and that individual’s contextual factors (environmental and personal factors) and focuses on activity and participation, attempting to optimise these according to what is felt to be most important by the individual involved, determined through goal setting. While elements of pathology and impairment may need to be addressed, the overall aim or goal should be based at the level of activity or participation in order to "optimise function".[8][9]
Therefore rehabilitation medicine does not minimize the importance of diagnosis and impairment but sees addressing these as part of a whole spectrum of management to achieve a person’s goals and optimise function.
References [edit | edit source]
- ↑ 1.0 1.1 1.2 Whiteneck G. Conceptual models of disability: past, present, and future. InWorkshop on disability in America: A new look 2006 Feb 27 (pp. 50-66). Washington: National Academies Press.
- ↑ Social and Behavioral Sciences at Bethel Univ. Models of Disability. Available from: https://youtu.be/r3ezHVM3XOE[last accessed 30/06/21]
- ↑ 3.0 3.1 Inclusion London. The Social Model of Disability Fact Sheet. Available from: https://www.inclusionlondon.org.uk/disability-in-london/social-model/the-social-model-of-disability-+and-the-cultural-model-of-deafness/ [Accessed on 20 June 2021]
- ↑ Shonaquip. Social Models of Disability Animation. Available from: https://youtu.be/MftKzY15_Vg[last accessed 30/06/21]
- ↑ Geoff Adams-Spink. Social Model Animation. Available from: https://youtu.be/9s3NZaLhcc4[last accessed 30/06/21]
- ↑ 6.0 6.1 6.2 International Network on the Disability Creation Process. The HDM-DCP Model - History of the Model. Available from: https://ripph.qc.ca/en/hdm-dcp-model/history-of-the-model/ (accessed on 26/06/2021)
- ↑ Gatchel, Robert J., Peng, Yuan Bo, Peters, Madelon, L.; Fuchs, Perry, N.; Turk, Dennis C. 2007 The biopsychosocial approach to chronic pain: Scientific advances and future directionsfckLR Psychological Bulletin, Vol 133(4), 581-624
- ↑ 8.0 8.1 The ICF: An Overview. Available at: https://www.wcpt.org/sites/wcpt.org/files/files/GH-ICF_overview_FINAL_for_WHO.pdf
- ↑ 9.0 9.1 Berghs M, Atkin K, Graham H, Hatton C, Thomas C. Scoping models and theories of disability. InImplications for public health research of models and theories of disability: a scoping study and evidence synthesis 2016 Jul. NIHR Journals Library.