Effective Quadriceps Training in Patellofemoral Pain
Top Contributors - Stacy Schiurring, Jess Bell and Kim Jackson
Introduction[edit | edit source]
Research into the cause of patellofemoral pain has been ongoing for decades. Looking back into the history of rehabilitation medicine, in the 1990s-2000s, it was believed that deficits of the vastus medialis oblique (VMO) of the quadriceps led to patellofemoral pain. However, early research often used fixed cadavers rather than live subjects. This meant that the data had limited applicability and external validity. More recently, research has utilised electromyography (EMG) of the VMO in isolation. While studying the VMO in isolation is not entirely without use, it limits the application of any research findings in clinical practice.
In more recent years, researchers have looked up and down the kinetic chain for a more holistic cause of patellofemoral pain.
While there is a large volume of research around the quadriceps, in particular the VMO, it does not prove that the quadriceps are the most likely problem or cause of patellofemoral pain. However, it does point to a way of predicting which rehabilitation patient will have VMO-related patellofemoral pain.[1]
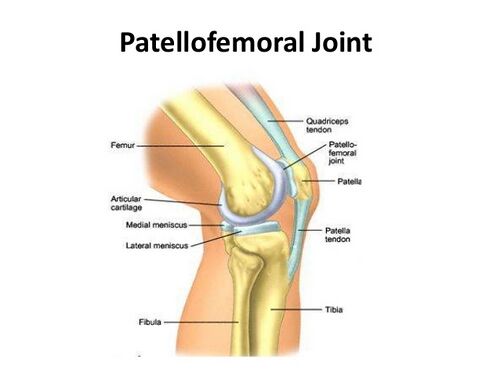
Patellofemoral Joint Biomechanics[edit | edit source]
Please review this article for an overview of the patellofemoral joint.
Joint Kinematics[edit | edit source]
The patella serves several mechanical functions:[2]
- It connects the muscles of knee extension to the tibia
- It contributes to knee extension by transferring the force of the quadriceps muscle to the tibia via the patellar tendon like a mechanical pulley[3][2]
- It alters the direction of the quadriceps' force throughout knee range of motion (ROM)[2]
Overview of patellofemoral kinematics[4]
- At full knee extension, the patella is located above the trochlear groove of the femur. Some of its articular surface is in contact at the distal lateral facets. The patella provides approximately 30% of the total knee extension torque at full knee extension.[2]
- During knee flexion, the patellar tendon pulls the patella into the trochlear groove which causes a slight medial translation.[3]
- At around 30° of knee flexion, the medial facets engage in the trochlear groove. Patella flexion increases with knee flexion. With increasing knee flexion, there is increasing patellar lateral translation and lateral tilt after an initial movement in the medial direction.[3]
- After 45° of knee flexion, the patella slowly moves into medial rotation.[3]
- In knee flexion greater than 90°, contact occurs on the proximal half of the medial and lateral facets.[3] The patella provides approximately 13% of total knee extension torque between 90° and 120° knee flexion.[2]
In open kinetic chain movements, the patella follows the path of the tibia due to the patellar tendon insertion at the tibial tubercle. The patella glides inferiorly during knee flexion and superiorly during knee extension. With a quadriceps set, the patella should move approximately 10 mm superiorly. With knee flexion, the overall pattern of patellar contact area increases and serves to distribute joint forces over a larger surface area. This decreases the likelihood of injury from repetitive high compressive forces.[2]
The patella also tracks lateral-medial-lateral during knee flexion. The patella moves approximately 3mm in each direction during medial and lateral displacement. As the knee flexes, the patella glides medially and becomes centered within the trochlear groove. During knee extension from 45° to 0°, the patella tilts medially. At around 30° of flexion, the patella glides back laterally and maintains this position for the remaining knee flexion. The motion has been described as a "C-curve pattern."[2]
In closed kinetic chain movements, the patella remains relatively in one place within the quadriceps tendon; this means the femur moves on the patella.
The optional 11-minute video in resources section provides a more detailed review of open versus closed kinetic chain exercises.
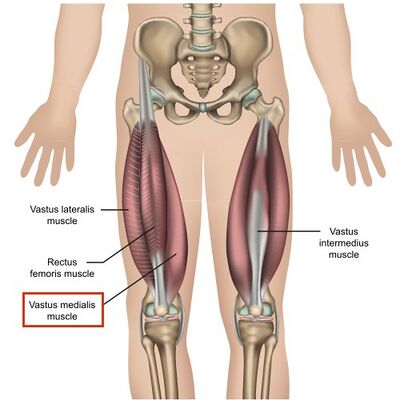
Quadriceps and Patellar Control[edit | edit source]
The following articles provide an overview of the quadriceps muscle: (1) Rectus femoris, (2) Vastus lateralis (VL), (3) Vastus medialis (VM), and (4) Vastus intermedius.
VMO Inhibition[edit | edit source]
The VMO has been the focus of much research in relation to patellofemoral pain. There are several scenarios where the VMO has no pull on the patella. This lack of pull causes joint dysfunction:[1]
- Swelling: In 1984, Stoke and Young elegantly demonstrated that 40 mL of fluid can inhibit the vastus lateralis, but only 10mL is needed to inhibit the VMO.[5] This is clinically relevant for patients who have a small effusion in the knee status post minor knee surgery. For example: a patient has undergone an arthroscopic meniscectomy then suddenly presents with post operative patellofemoral pain. Often in these situations, an effusion has shut down the VMO and this drives some patellofemoral pain in conjunction with other risk factors.[1]
- Post dislocation, or a heavy fall onto the knee: Approximately 50% of these patients, who do not have a patellar fracture, will have pain one year post injury, and often have an effusion as well. Situations such as surgery, dislocation, or trauma can set off an effusion which creates a dramatic change in the patient's dynamic stability.[1]
- Presence of pain: This is a similar group of patients to those who have had surgery, a dislocation, fall, or other trauma. Hodges et al.[6] demonstrated that alterations in knee muscle activity can be caused by pain, even when that pain is of non-muscle origin. The was done by injecting saline into the infrapatellar fat pad. EMG activity of the VMO was measured and found to be immediately slowed after the saline injection.[6]
It is important to remember that if a patient has a painful knee of any aetiology for long enough, it will drive secondary VMO sluggishness and poor performance. In addition, the atrophy will create VMO muscle architecture change.[1]
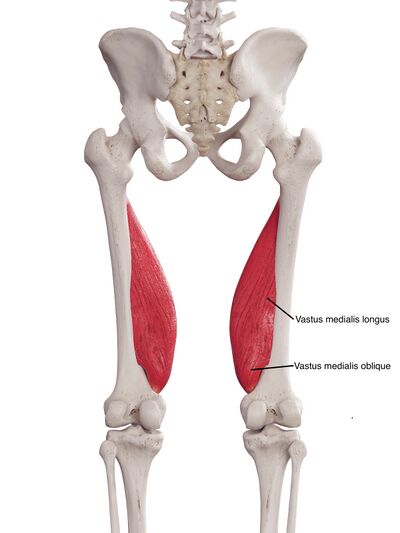
Vastus Medialis Muscle Architecture[edit | edit source]
Over the past few decades, rehabilitation science has been moving toward evidenced-based practice. This growing body of research provides validity to rehabilitation interventions and techniques. As recently as 2005, there was still uncertainty regarding the anatomical makeup and function of the quadriceps.
Timeline of quadriceps research:
- In 2005, Peeler et al.[7] performed a cadaver study to examine the anatomy and function on the VM. They observed that the VMO and the vastus medialis longus (VML) had different muscle fibre orientations depending on the angle of observation. However, they found no evidence of a fascial plane or separate innervation between the VMO and VML. They also stated that the VMO was not anatomically positioned to function as a primary active stabiliser of the patella.[7]
- In 2005, Ono et al.[8] also performed a cadaver study to examine the anatomical boundaries of the VML and the VMO. They observed that the line from the adductor hiatus to the medial rim of the patella appears to be the boundary between the VMO and VML. However, they concluded that a fascial plane was not required for a definitive separation between the VMO and VML. They confirmed different innervation of the VMO and the VML which suggested a difference in their functionality. This study also noted a difference in muscle fibre orientation between the VMO and VML.[8]
- In 2014, Engelina et al.[9] performed an ultrasound investigation of the VMO in vivo. They observed that the VMO was a separate entity from the VML. They also confirmed the presence of a fascial plane between the VMO and the VML, and noted a difference in origin on the adductor muscles, different fibre orientation, and different nerve distribution. In addition, this study found that the anatomy of the VM varied a great deal across the participant population.[9]
- In 2015, Benjafield et al.[10] looked at how an individual's level of activity can affect the structure of their VMO. The authors utilised ultrasound (US) to assess the VMO fibre angles of both active and sedentary participants, and measured their activity level using the Tegner scoring system. They found that people who were classified as sedentary had a smaller fibre angle and a smaller amount of insertion onto the patella, and people who were classified as athletic had a larger angle and a larger insertion. A larger insertion onto the patella provides a greater medial stabilising force. This, therefore, helps to validate the use of VMO strengthening exercises in the management of patellofemoral pain.[10]
- In 2016, Khoshkhoo et al.[11] tried to determine if changes could be made to VMO architecture using a physiotherapy driven strengthening programme. Upon assessment following a 6-week quadriceps strengthening programme, it was found that participants had undergone a significant increase in VMO fibre angle and insertion length. These results are important because they support the use of skilled physiotherapy strengthening to create significant changes in VMO architecture to make it a better medial stabiliser.[11]
- In 2017, Elniel et al.[12] compared the effects of closed-chain versus open-chain exercises on changes in VMO architecture. Their findings suggest that both types of exercise regimes have equal effects on the architecture of the VMO after six weeks of training.[12]
- In 2018, Arnantha et al.[13] dove deeper into the details of the exercise required to maintain changes in the VMO. They found that physiotherapy exercise programmes prescribed for patellofemoral pain have a positive effect on the VMO fibre angle and insertion level. However, exercises must be continued at least two times per week in order to maintain the gains achieved by the initial exercise programme. When exercises were discontinued after the initial exercise programme, participants experienced a slight reversal of the VMO architecture gains.[13]
- In 2018, Hilal et al.[14] studied the effect of neuromuscular electrical stimulation (NMES) on VMO architecture. They found that the benefits of exercise can be greatly enhanced by the addition of NMES when looking at changes in the architecture of the VMO.[14]
This research clarifies the following:[1]
- The VMO is a separate entity from the VML
- The VMO and the VML have different muscle fibre orientations
- The VMO and the VML have different nerve distributions
- The anatomy of the VM varies across the population
- Exercise can effect the muscle architecture of the VMO
How Does Muscle Architecture Change?[edit | edit source]
The changes in VMO muscle fibre architecture are the result of muscle hypertrophy. Exercise induced hypertrophy does not change the number of fibres present, but changes the diameter of the muscle fibres. As the muscle fibre diameter increases, their orientation within the muscle changes as the fibres push against the surrounding fibres. This changes the angle of pennation.[1][15]
"The pennation angle is the angle between the longitudinal axis of the entire muscle and its fibers. The longitudinal axis is the force generating axis of the muscle and pennate fibers lie at an oblique angle. As tension increases in the muscle fibers, the pennation angle also increases."[16]
The following optional video provides a simple overview of how muscular damage and repair result in muscular hypertrophy and growth.
Quadriceps Exercise Theory[edit | edit source]
VMO exercise considerations:[1]
- Focus on quadriceps exercises rather than attempting to isolate the VMO individually
- Ideally, do not exercise in the presence of swelling
- Do not exercise into pain beyond a 3 out of 10
- Consider icing before exercise, especially for post-surgical patients, to improve muscle fibre recruitment[18]
- Consider time of day when scheduling treatment sessions to manage soreness and or timing with pain medication
- Push to muscle fatigue on alternating days to create hypertrophy
- Consider blood flow restriction training if the patient cannot effectively exercise to fatigue[19]
- Work synergistically with the gluteal muscles to encourage quality limb control
- Incorporate movements and activities that are meaningful to the patient and help them work towards their long-term goals
Closed-chain Exercises[edit | edit source]
In 1993, Steinkamp et al.[20] studied the knee moment, patellofemoral joint reaction force, and patellofemoral joint stress of 20 healthy adult subjects during leg press and leg extension exercises at 0°, 30°, 60°, and 90° of knee flexion. They found that all parameters were significantly greater in the leg extension exercise at 0°and 30° of knee flexion; and that all parameters were significantly greater in the leg press exercise at 60°and 90° of knee flexion.[21] Patellofemoral joint stresses for exercises intersected at approximately 50° knee flexion. This study demonstrates that patients with patellofemoral joint arthritis may tolerate leg press exercises better than leg extension exercises within functional range of motion (ROM) because of the lower patellofemoral joint stresses.[20][22]
Progression of closed-chain exercises such as squats, lunges, or the leg press does not necessarily mean moving into deeper flexion, which is more likely to cause irritation. Progression can be modifying the activity by changing the load, the support surface, length of isometric hold, etc. Once the patient has improved their strength and endurance, it is appropriate to increase the depth of movement. Building their exercise tolerance slowly will decrease the likelihood of exercise induced muscle soreness.[1]
Early exercise progression example:[1]
- Limit ROM from 0° to 50°, but increase the weight load
- Start with a double leg wall squat to 45°
- Stand with the majority of weight on one leg, off-load the other foot on a step or ball, and perform isometric holds
- Increase the length of the isometric hold
- Come away from the wall, perform a double leg squat but add in some weight on a barbell or dumbbells
- Progress to double leg squat on an unstable surface such as foam or a BOSU
Further progression of exercise can include closed-chain exercises between 0° and 45° and open-chain between 90° and 45°, to encourage work throughout the entire knee ROM. Vary the exercises and modify as appropriate to ensure the patient is achieving muscle fatigue. You also want to ensure that the patient has time to recover. This is important because if the muscle does not work to fatigue, and the patient does not get recovery, they will not achieve the desired muscle hypertrophy.[1]
Example of exercise prescription:[1]
- 4 sets of 8 repetitions to fatigue, alternate days
- Once the patient has achieved VMO architecture change, aim for 3 or 4 sets of 20, with increased repetitions to fatigue
Open-chain Exercises[edit | edit source]
- Perform in the earlier stages of rehabilitation
- Limit ROM to between 90° and 45°
- Seated exercises, with or without a therapy band
- Open-chain leg extension machine[1]
Resources[edit | edit source]
Optional Additional Reading:
- Barber-Westin S, Noyes FR. Blood flow–restricted training for lower extremity muscle weakness due to knee pathology: a systematic review. Sports Health. 2019 Jan;11(1):69-83.
- Loro WA, Thelen MD, Rosenthal MD, Stoneman PD, Ross MD. The effects of cryotherapy on quadriceps electromyographic activity and isometric strength in patient in the early phases following knee surgery. Journal of Orthopaedic Surgery. 2019 Feb 25;27(1):2309499019831454.
- Wheatley MG, Rainbow MJ, Clouthier AL. Patellofemoral mechanics: a review of pathomechanics and research approaches. Current Reviews in Musculoskeletal Medicine. 2020 Jun;13(3):326-37.
Optional Video:
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 Robertson, C. Patellofemoral Joint Programme. Effective Quadriceps Training in Patellofemoral Pain. Plus. 2022.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Loudon JK. Biomechanics and pathomechanics of the patellofemoral joint. International journal of sports physical therapy. 2016 Dec;11(6):820.
- ↑ 3.0 3.1 3.2 3.3 3.4 Wheatley MG, Rainbow MJ, Clouthier AL. Patellofemoral mechanics: a review of pathomechanics and research approaches. Current Reviews in Musculoskeletal Medicine. 2020 Jun;13(3):326-37.
- ↑ Huang W, Zeng X, Man GC, Yang L, Zhang Y. Simultaneous Measurement of Patellofemoral Joint Kinematics and Contact Mechanics in Intact Knees: A Cadaveric Study. Orthopaedic Surgery. 2022 Sep;14(9):2317-29.
- ↑ Stokes M, Young A. Investigations of quadriceps inhibition: implications for clinical practice. Physiotherapy. 1984 Nov;70(11):425-8.
- ↑ 6.0 6.1 Hodges PW, Mellor R, Crossley K, Bennell K. Pain induced by injection of hypertonic saline into the infrapatellar fat pad and effect on coordination of the quadriceps muscles. Arthritis Care & Research. 2009 Jan 15;61(1):70-7.
- ↑ 7.0 7.1 Peeler J, Cooper J, Porter MM, Thliveris JA, Anderson JE. Structural parameters of the vastus medialis muscle. Clinical Anatomy: The Official Journal of the American Association of Clinical Anatomists and the British Association of Clinical Anatomists. 2005 May;18(4):281-9.
- ↑ 8.0 8.1 Ono T, Riegger-Krugh C, Bookstein NA, Shimizu ME, Kanai S, Otsuka A. The boundary of the vastus medialis oblique and the vastus medialis longus. Journal of Physical Therapy Science. 2005;17(1):1-4.
- ↑ 9.0 9.1 Engelina S, Antonios T, Robertson CJ, Killingback A, Adds PJ. Ultrasound investigation of vastus medialis oblique muscle architecture: an in vivo study. Clinical Anatomy. 2014 Oct;27(7):1076-84.
- ↑ 10.0 10.1 Benjafield AJ, Killingback A, Robertson CJ, Adds PJ. An investigation into the architecture of the vastus medialis oblique muscle in athletic and sedentary individuals: an in vivo ultrasound study. Clinical Anatomy. 2015 Mar;28(2):262-8.
- ↑ 11.0 11.1 Khoshkhoo M, Killingback A, Robertson CJ, Adds PJ. The effect of exercise on vastus medialis oblique muscle architecture: an ultrasound investigation. Clinical anatomy. 2016 Sep;29(6):752-8.
- ↑ 12.0 12.1 Elniel AR, Robertson C, Killingback A, Adds PJ. Open-chain and closed-chain exercise regimes: an ultrasound investigation into the effects of exercise on the architecture of the vastus medialis oblique. Phys Ther Rehabil. 2017;4:3.
- ↑ 13.0 13.1 Arnantha, Harry, C. Robertson, A. Killingback and Philip J. Adds. “Maintenance of exercise-induced changes in the architecture of the VMO: how much is enough? An in-vivo ultrasound study.” (2018)
- ↑ 14.0 14.1 Hilal Z, Robertson CJ, Killingback A, Adds PJ. The Effect of Exercise and Electrical Muscle Stimulation on the Architecture of the Vastus Medialis Oblique - The ‘Empi’ Electrotherapy J Ortho & Sport Med. 2018. (1)1-5.
- ↑ Torrente QM, Killingback A, Robertson C, Adds PJ. The effect of self-myofascial release on the pennation angle of the vastus medialis oblique and the vastus lateralis in athletic male individuals: an ultrasound investigation. International Journal of Sports Physical Therapy. 2022;17(4):636.
- ↑ Wikipedia. Muscle architecture. Available from: https://en.wikipedia.org/wiki/Muscle_architecture (accessed 24/08/2022).
- ↑ YouTube. What makes muscles grow? - Jeffrey Siegel| TED Ed. Available from: https://www.youtube.com/watch?v=2tM1LFFxeKg [last accessed 16/08/2022]
- ↑ Loro WA, Thelen MD, Rosenthal MD, Stoneman PD, Ross MD. The effects of cryotherapy on quadriceps electromyographic activity and isometric strength in patient in the early phases following knee surgery. Journal of Orthopaedic Surgery. 2019 Feb 25;27(1):2309499019831454.
- ↑ Barber-Westin S, Noyes FR. Blood flow–restricted training for lower extremity muscle weakness due to knee pathology: a systematic review. Sports Health. 2019 Jan;11(1):69-83.
- ↑ 20.0 20.1 Steinkamp LA, Dillingham MF, Markel MD, Hill JA, Kaufman KR. Biomechanical considerations in patellofemoral joint rehabilitation. The American journal of sports medicine. 1993 May;21(3):438-44.
- ↑ Pereira PM, Baptista JS, Conceição F, Duarte J, Ferraz J, Costa JT. Patellofemoral Pain Syndrome Risk Associated with Squats: A Systematic Review. International Journal of Environmental Research and Public Health. 2022 Jul 28;19(15):9241.
- ↑ Martín-Fuentes I, Oliva-Lozano JM, Muyor JM. Influence of feet position and execution velocity on muscle activation and kinematic parameters during the inclined leg press exercise. Sports Health. 2022 May;14(3):317-27.
- ↑ YouTube. CLOSED VS OPEN KINETIC CHAIN MOVEMENTS. WHAT'S THE DIFFERENCE ? CKC Vs OKC !!! Available from: https://www.youtube.com/watch?v=3wwEyV5CdBM [last accessed 16/08/2022]