Diuretics
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton
Introduction[edit | edit source]
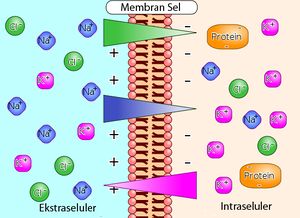
Diuretics are drugs that promote the removal from the body of excess water, salts, poisons, and accumulated metabolic products, such as urea[1]. In general, they inhibit electrolyte reabsorption from the lumen of the nephron, increasing osmolarity and enhancing water excretion.
Indications[edit | edit source]
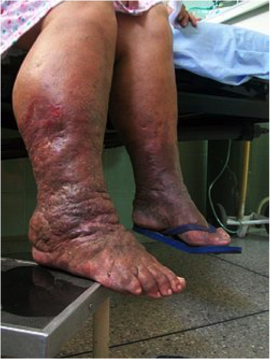
Diuresis is necessary for a variety of non-edematous and edematous conditions, which require clearing out excess water when the body abnormally sequesters fluid in third space in the form of edema ("Third spacing" is the abnormal accumulation of fluid into an extracellular and extravascular space).[2]
The quintessential of edematous conditions is heart failure (HF) where the inefficiency of the heart’s pumping ability results in:
- Decreased renal perfusion leading to activation of the renin-angiotensin-aldosterone-system (RAAS) and
- Long-standing venous stasis leading to extravasation of fluid into the interstitial space, both of which lead to intravascular volume expansion and result in signs of congestion such as weight gain, dyspnea, and generalized edema.
Diuretics are used in the treatment of a wide range of conditions. These include:
- Chronic Heart Failure (see also Aldosterone Receptor Antagonist Diuretics in the treatment of congestive heart failure)
- Hypertension (see also Diuretics in the Treatment of Hypertension)
- Glaucoma
- Liver disease
- Kidney disease
- Hyperaldosteronism
- Edema
- Hypokalemia[3]
Types[edit | edit source]
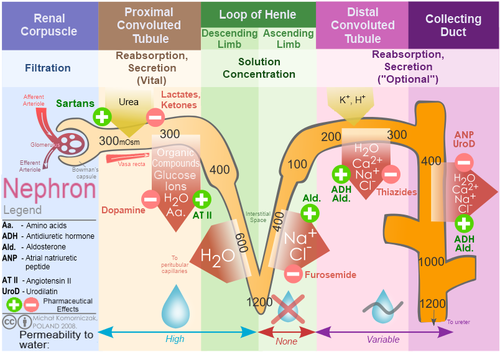
A major difference among the types of diuretics depends on the level of potency. This variation in potency is due to the differences in the sites of action of diuretics on the kidney structure. The different types include:
- Loop diuretics (eg, furosemide, bumetanide, torasemide), which are the most potent type, increase the elimination of sodium and chloride by primarily preventing reabsorption of sodium and chloride. Loop diuretics are often used to treat heart failure. The high efficacy of loop diuretics is because of to the unique site of action involving the loop of Henle (a portion of the renal tubule, in the kidneys). Loop Diuretics are very powerful, so if a less powerful diuretic can be used, it should be used. Indications:
- There is pulmonary edema and patient has a history of congestive heart failure (CHF)
- Edema around the liver, heart, or kidney and other diuretics haven't been useful
- Hypertension and other diuretics haven't been useful
2. Thiazides are the most commonly prescribed diuretics. They’re most often used to treat high blood pressure. These drugs not only decrease fluids, they also cause blood vessels to relax.[4] Thiazides work on the distal convoluted tubule. They are not as potent as Loop Diuretics. They also excrete sodium, chloride, potassium and water but they increase uric acid and glucose (these drugs only work if the patient has adequate kidney function, loop diuretics are used when kidney function is impaired). After they were synthesized in the late 1950s, thiadiazides replaced most other existing diuretics. They are more convenient than some other diuretics in that they can be taken orally in the form of pills[1]. Therapeutic Uses:
- Hypertension
- Edema (that's mild/moderate)
- Diabetes Insipidus (can decrease urine production by 30-50%)
3. Potassium-sparing diuretics reduce sodium reabsorption at the distal tubule, thus decreasing potassium secretion. In the distal tubule, potassium is excreted into the forming urine coupled with the reabsorption of sodium. Therapeutic uses: These drugs are most likely being used because a loop or thiazide diuretic is being used and don't want the patient to become hypokalemic.
- Heart Failure
- Primary Hyperaldosteronism
- Premenstrual Syndrome
- Polycystic Ovary Syndrome
4. Carbonic anhydrase inhibitors work by increasing the excretion of sodium, potassium, bicarbonate and water from the renal tubules. Carbonic anhydrase inhibitors (acetazolamide) are used for the prophylaxis of mountain sickness (unlicensed indication) and glaucoma.[5]
5. Osmotic diuretics (mannitol) are used in a hospital setting for the treatment of cerebral oedema[5]. They work on the lumen of the nephron by creating osmotic force. It has no significant effect on the excretion of electrolytes. Therapeutic Uses:
- Mainstay of medical therapy for raised intracranial pressure (ICP) after traumatic brain injury and cerebral edema.
- Mannitol also promotes diuresis in acute renal failure and to excrete toxic metabolites and substances.
- Though hypertonic saline similarly is used to treat high ICP and sometimes has demonstrated greater efficiency than mannitol is not considered a diuretic[6][3][7][2]
Natural Diuretics[edit | edit source]
Heart failure, hypertension, cirrhosis and nephritic syndrome are among conditions that alter volume and composition of body fluids and are modulated by diuretics. Natural products are important source of diuretics and have been considered remarkable alternative with greater effectiveness and fewer side effects. However, many of these plants used in traditional medicine must be scientifically assessed about their efficacy and toxicity. Despite the large number of published articles claiming that plants or plant-derived components may act as diuretic agents, few studies have addressed the mechanism of action of medicinal plants.[8]
Examples of natural diuretics include:
- Nigella sativa, black cumin, black seed, or black caraway, is a natural diuretic that may be as effective as a popular prescription diuretic. Nigella sativa increases urine output and in turn reduces sodium and potassium levels.
- Hibiscus: The Hibiscus sabdariffa plant works as a natural diuretic and also prevents the body from getting rid of potassium. Hibiscus sabdariffa is also known as roselle or red sorrel. It is often used as a medicinal supplement or made into a tea. Hibiscus tea is made by steeping the dried petals of the hibiscus flower in hot water.
- Alcohol is a well-known diuretic that works by increasing urine output. However, alcohol has many adverse health effects and should always be consumed in moderation.
- Nasturtium leaves: its main compound isoquercitrin (ISQ), exhibit pronounced diuretic effects, supporting the ethnopharmacological use of this plant[9]
- Dandelion: A common wildflower found in many parts of the Northern hemisphere.
- Ginger: Both dandelion and ginger are popularly used in drinks and teas claiming to be detoxifying because of their diuretic qualities. No sound human studies have proven their effects, however.
- Parsley: A study found that parsley seed extract given to rats increased their urine volume significantly. Parsley has been used as a home remedy diuretic for many years. The mechanism of action of parsley seems to be mediated through an inhibition of the Na+-K+ pump that would lead to a reduction in Na+ and K+ reabsorption leading thus to an osmotic water flow into the lumen, and diuresis.[10]
- Caffeine may have a mild, short-term diuretic effect. Caffeine is found in coffee, tea, soda, and energy drinks. People who regularly have drinks with caffeine can develop a tolerance to caffeine and will not see any difference[11].
General Adverse Effects[edit | edit source]
The most common adverse effect for any diuretic is mild hypovolemia, which can lead to transient dehydration and increased thirst.
- When there is an over-treatment with a diuretic, this could lead to severe hypovolemia, causing hypotension, dizziness, and syncope.
- More generalized side-effects of diuretic agents include headache, urinary frequency, restlessness, weakness, fatigue, and lethargy. GI disturbances like nausea, vomiting, constipation, diarrhea, anorexia, and abdominal pain can occur with loop diuretics and PSDs than any other diuretic group.
- Electrolyte abnormalities are commonly associated with all the diuretic agents. Acid-base disorders usually accompany the electrolyte derangement due to their close association with their reabsorption in the renal tubules. Metabolic disturbances can lead to derangement of glucose, uric acid, or lipid levels with certain diuretics and are individually discussed.
- In general, adverse effects are dose-dependent and are higher with loop diuretics as they have the most significant diuretic effect. With controlled low-dose formulations, adverse effects have reduced substantially, especially with thiazide diuretics.[2]
- Diuretic-induced hypokalaemia is a common and potentially life-threatening adverse drug reaction in clinical practice. Previous studies revealed a prevalence of 7%–56% of hypokalaemia in patients taking thiazide diuretics. Reducing diuretic dose and potassium supplementation are the most direct and effective therapies for hypokalaemia. Combining with a potassium-sparing diuretic or blocker of the renin–angiotensin system also reduces the risk of hypokalaemia. Lowering salt intake and increasing intake of vegetables and fruits help to reduce blood pressure as well as prevent hypokalaemia.[12]
Diuretic Abuse[edit | edit source]
Diuretics are not highly controlled drugs and hence have a high probability for misuse, particularly with athletes who might abuse them for rapid weight loss or to conceal the presence of other banned drugs.
- The use of diuretics is prohibited in athletes. (Athletes require a prior exemption for therapeutic use in athletes) and is routinely screened for by the world anti-doping agency.
- Such abuse, if it persists chronically, can lead to detrimental effects on CV and thermoregulatory functions, which could lead to death when combined with excessive physical activity as encountered in athletes[2].
Diuretics are not helpful for losing weight. Anyone who wishes to lose weight should follow a healthy, balanced diet and exercise regularly. Any weight lost will return as the body rehydrates.[11]
Patient Education[edit | edit source]
Patient education plays a crucial role and adequate knowledge of the adverse effects, dietary, and lifestyle modifications that are necessary while on diuretics. Patients (especially in an outpatient setting) must understand to report any type of changes in their compliance pattern or any adverse effect thereof. Adherence to strict treatment protocols and timely intake of the drug and avoidance of any overdosing when the patients miss their dosing will significantly improve the clinical course and the effectiveness of the diuretic agent[2].
Examples of education include:
- Diet - Specifically, with loop diuretics, you have to make sure that the patient has a diet that is high in potassium. Loop diuretics are potassium-wasting diuretics, which mean that they deplete potassium from the body and into the potty. For this reason, it is critical that you instruct your patient to consume foods that are high in potassium and some examples are: Bananas; Oranges; Spinach; Green, leafy vegetables. A low salt diet should be promoted.
- Evening Doses are a No-No: Never give diuretics in the evening. You don’t want your patients to fall on the ground or trip themselves when going to the toilet.
- Take AM: To prevent the risk of falling, diuretics are given only in the morning[13].
References[edit | edit source]
- ↑ 1.0 1.1 Britnnica Diuretics Available from: https://www.britannica.com/science/diuretic(accessed 15.4.2021)
- ↑ 2.0 2.1 2.2 2.3 2.4 Arumugham V, Shahin M. Therapeutic Uses Of Diuretic Agents. StatPearls. 2021 Mar 28.Available:https://www.statpearls.com/articlelibrary/viewarticle/20623/ (accessed 16.4.2021)
- ↑ 3.0 3.1 NAPLEX study guide Diuretics Available from: https://naplexstudyguide.com/diuretics-pharmacology/(accessed 15.4.2021)
- ↑ Healthline Diuretics Available from:https://www.healthline.com/health/diuretics#types(accessed 16.4.2021)
- ↑ 5.0 5.1 Patient Diuretcis Available from: https://patient.info/doctor/diuretics (accessed 16.4,2021)
- ↑ Hello nurse Diuretics Available from:http://www.hellooonurse.com/2015/01/know-your-drugs-pharmacology-of.html (accessed 15.4.2021)
- ↑ Natural therapy Diuretics Available from:https://www.naturaltherapypages.com.au/article/diuretics (accessed 15.4.2021)
- ↑ Aparecida Livero F, Vergutz Menetrier J, Luiz Botelho Lourenco E, Gasparotto Junior A. Cellular and molecular mechanisms of diuretic plants: an overview. Current pharmaceutical design. 2017 Mar 1;23(8):1247-52.Available from: https://pubmed.ncbi.nlm.nih.gov/27758702/(accessed 15.4.2021)
- ↑ Junior, A.G., Prando, T.B.L., Leme, T.D.S.V., Gasparotto, F.M., Lourenço, E.L.B., Rattmann, Y.D., Da Silva-Santos, J.E., Kassuya, C.A.L. and Marques, M.C.A., 2012. Mechanisms underlying the diuretic effects of Tropaeolum majus L. extracts and its main component isoquercitrin. Journal of Ethnopharmacology, 141(1), pp.501-509.Available: https://pubmed.ncbi.nlm.nih.gov/22465728/(accessed 15.4.2021)
- ↑ Kreydiyyeh SI, Usta J. Diuretic effect and mechanism of action of parsley. Journal of ethnopharmacology. 2002 Mar 1;79(3):353-7.Available: https://pubmed.ncbi.nlm.nih.gov/11849841/ (accessed 15.4.2021)
- ↑ 11.0 11.1 Med news today Diuretics Available from: https://www.medicalnewstoday.com/articles/313001#natural_diuretics(accessed 1.4.2021)
- ↑ Lin Z, Wong LY, Cheung BM. Diuretic-induced hypokalaemia: an updated review. Postgraduate Medical Journal. 2021 Mar 8.Available:https://pmj.bmj.com/content/early/2021/03/08/postgradmedj-2020-139701 (accessed 16.4.2021)
- ↑ Simple nursing Diuretics Available :https://simplenursing.com/precautions-administering-diuretics/ (accessed 16.4.2021)