Developmental Disabilities in Early and Middle Childhood
Top Contributors - Jess Bell, Kim Jackson, Wanda van Niekerk, Naomi O'Reilly, Tarina van der Stockt, Cindy John-Chu and Rucha Gadgil
Introduction[edit | edit source]
"Developmental disabilities are a diverse group of severe chronic conditions that are due to mental and/or physical impairments. People with developmental disabilities have problems with major life activities such as language, mobility, learning, self-help, and independent living."[1]
Developmental disabilities (DD) includes conditions such as:[2]
- Attention deficit hyperactivity disorder (ADHD)
- Autism
- Intellectual disability
- Learning difficulties (e.g. developmental coordination disorder (DCD) / dyspraxia, auditory processing disorder)
- Blindness
- Cerebral palsy
- Moderate to profound hearing loss
- Seizures
- Stuttering / stammering
- Other developmental delay
The prevalence of DDs is increasing. From 1997 to 2008, autism prevalence increased by 289.5 percent while ADHD prevalence increased by 33 percent.[3] The 2009-2017 National Health Interview Survey showed a 9.5 percent increase in the prevalence of DDs in children aged 3 to 17 years.[4]
Movement Difficulties - Hypermobility[edit | edit source]
1. Muscle Tone[edit | edit source]
Muscle tone is defined as: “the tension in the relaxed muscle”[5] - i.e. the amount of tension or resistance to stretch in a muscle.[2]
2. Hypotonia[edit | edit source]
Hypotonia is defined as: “poor muscle tone resulting in floppiness. It is abnormally decreased resistance encountered with passive movement of the joint.”[6]
There are different causes of hypotonia:[2]
- Lower motor neuron disease (neurological, metabolic and genetic causes)
- Infections (meningitis, polio)
- Genetic (Down’s syndrome, Prader-Willi, Tay-Sachs, spinal muscular atrophy, Charcot-Marie-Tooth syndrome, Marfan syndrome and Ehlers-Danlos syndrome)
- Metabolic (rickets)
- Congenital hypothyroidism
- Genetic acquired (muscular dystrophy)
- Benign congenital hypotonia (BCH)
- NB: BCH is a symptom, rather than a diagnosis. Diagnosis is made in the absence of other diagnoses (such as joint hypermobility, autism or developmental coordination disorder)
- Low connective tissue tone
- This is considered better terminology to describe hypermobility or increased laxity in connective tissue
- Joint hypermobility
- This term is used when only the connective tissue in joints is affected
- Benign joint hypermobility syndrome (BJHS)
3. Benign Joint Hypermobility Syndrome[edit | edit source]
BJHS is a hereditary condition[7] that causes musculoskeletal symptoms in hypermobile patients, without other rheumatological features being present. It appears to be caused by an abnormality in collagen or the ratio of collagen subtypes.[8]
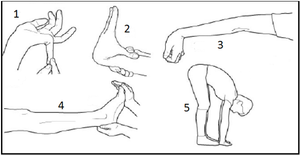
Diagnosis is made based on a medical examination and use of the Beighton score (see Figure 1).
Children with BJHS are susceptible to joint injury or dislocation, reduced stability, and a decreased ability to build muscle strength. They may tire easily, complain of pain or digestive issues, but symptoms are variable. They tend to be exacerbated during growth spurts, adolescence and hormone changes.[2] 32 percent of children with BJHS also present with movement and coordination disorders.[9]
For more information on the clinical assessment of generalised joint hypermobility, please see the Ehlers-Danlos Society website.
4. The Good News About Hypermobility[edit | edit source]
- Strengthening is beneficial[10]
- Swimming, pilates, climbing, horse riding can help (i.e. non-impact activities):[2]
- If children engage in high impact sports, they may require rest days (particularly if they are complaining of night pain after activity)
- Specific movement programmes such as PhysiFun are beneficial[2]
NB: If children with BJHS participate in ballet, gymnastics or dancing, it is important that they avoid “locking out” their joints. Instead, teach them to have “soft knees”. Also, watch for lordotic postures and tight hamstrings.[2]
Social, Behaviour and Movement Difficulties[edit | edit source]
Social Communication Disorder and Autism Spectrum Disorder[edit | edit source]
Social (pragmatic) communication disorder (SCD) is a relatively new diagnosis, described in the DSM-5. It is characterised by problems with verbal and non-verbal social communication,[11] but individuals with this condition do not display any restricted and repetitive interests or behaviours.[12] People with SCD may, for example, have difficulty taking turns to speak, adapting their voice, making small talk, and making eye contact.[2]
Autism spectrum disorder (ASD) is a neurodevelopmental disorder that affects how individuals communicate and interact with others. Conditions that were previously seen as separate disorders (i.e. autism, Asperger’s) are now included under the umbrella term ASD.[13] There is a very broad spectrum of affect in ASD – from mild to very severe.[2] Individuals with ASD also display restricted, repetitive patterns of behaviour, interests or activities.[14]
Other signs of ASD are:[2]
- One-sided conversations
- Robotic monotone speech
- Awkward movements and/or mannerisms
While motor impairment is not currently part of the diagnostic criteria or evaluation of autism, individuals with ASD can also present with motor difficulties.[15] These motor difficulties may be due to:[2]
- A lack of body awareness
- Avoidance of exercise due to its social nature
- Limited strength
- Difficulty following commands and communicating
The Good News[edit | edit source]
Learning and Behavioural Difficulties - Attention Deficit Hyperactivity Disorder[edit | edit source]
Attention deficit hyperactivity disorder (ADHD) is a neurodevelopmental disorder that affects the functioning of the brain. It seems to be due to abnormalities in the dopamine system and a change in frontal lobe development.[2] While its cause is unknown, it is considered a genetic disorder, with environmental factors (e.g. diet, physical and social environments) playing a small role in its aetiology.[2][18]
The following factors can increase the risk of ADHD:[2]
- Very low birth weight
- Premature birth
- Exceptional early adversity
ADHD is diagnosed based on reported behaviours or psychiatric assessment. The primary symptoms associated with ADHD are inattentiveness, hyperactivity and impulsiveness.[2] However, fine and gross motor skills are affected in around 30 to 50 percent of children with ADHD,[2][19][20] particularly in the predominantly inattentive and combined ADHD group.[21]
These motor problems are often ignored due to behaviour difficulties, but children typically struggle with:[2]
- Dressing
- Handwriting
- Learning to ride a bicycle
- Tying shoelaces
The Good News[edit | edit source]
- Exercise can be beneficial[2][22][23][24]
- Realistic goals, attention practice, intrinsic motivation can help, as can grit and determination, locus of control and having a champion[2]
Sensory Difficulties[edit | edit source]
1. Sensory Processing Disorder[edit | edit source]
Sensory processing disorder (SPD) is characterised by “chronic and significant impairments with the modulation and integration of sensory stimuli.”[28]
It is important to note that opinion is divided on whether or not SPD is a specific diagnosis on its own,[29][30] but presenting features of SPD are listed in Table 1.
| Sensory System | Symptoms |
|---|---|
| Auditory | Negative response to unexpected/loud noises
Holds hands over ears Unable to walk with background noise Appears oblivious in active environments |
| Visual | Prefers darkness
Hesitates going up and down steps Avoids bright lights Stares intently at people or objects Avoids eye contact |
| Taste and smell | Avoids specific tastes/smells that would typically be part of a child's diet
Routinely smells non-food objects Seeks out certain tastes or smells Does not seem to smell strong odours |
| Body position | Always seeking movement activities
Hangs on people, furniture, objects, even in familiar situations Seems to have weak muscles, gets tired easily and has reduced endurance Walks on toes |
| Movement | Becomes anxious or distressed when feet leave the ground
Avoids climbing or jumping Avoids playground equipment Seeks all kinds of movement, which interferes with daily life Takes excessive risks while playing and has no safety awareness |
| Touch | Avoids getting messy in glue, sand, finger paint or tape
Is sensitive to certain fabrics (clothing, bedding) Touches people and objects at an irritating level Avoids going barefoot, especially in grass or sand Has decreased awareness of pain or temperature |
2. Intervention - Sensory Integration Therapy[edit | edit source]
Sensory integration therapy (SIT) was initially proposed as a treatment for SPD in 1972 by Jean Ayres. It is primarily used by occupational therapists (OTs). Children are provided with various sensory experiences. Each experience is matched with a “just right” challenge - i.e. an activity that requires an adaptive response from the child.[30]
However, the evidence for SIT is considered weak at best.[30] OTs also use other interventions based on SIT, but with some key differences. While they tend to use a sensory integration framework to understand/explain the child’s behaviour, the focus is not on fixing an underlying impairment. Rather, they work with the child, parents and teachers to help change the environment to enable greater participation. Modifications might include:[30]
- Clothing
- Room configurations
- Noise or light levels
- Experimenting with food textures
- Adapting tools and materials
- Changing programme requirements
For a review of the evidence for sensory integration, please read this article: Sensory integration: A review of the current state of the evidence.
The Good News[edit | edit source]
Developmental Coordination Disorder[edit | edit source]
Developmental coordination disorder (DCD) / dyspraxia is a common neuromotor condition, which affects around 5 to 6 percent of school-aged children, but it often goes unrecognised by health professionals.[32] In the DSM-5, DCD is specifically characterised as a neurodevelopmental motor disorder. Other neurodevelopmental motor disorders include stereotypic movement disorder and tic disorders.[2] Individuals with DCD have problems acquiring and executing coordinated motor skills. As defined in the DSM-5:
“the child with developmental coordination disorder has motor coordination below expectations for his or her chronologic age, may have been described as “clumsy” and may have had delays in early motor milestones, such as walking and crawling. Difficulties with coordination of either gross or fine motor movements, or both, interfere with academic achievement or activities of daily living. Coordination difficulties do not relate to a medical condition or disease (e.g., cerebral palsy, muscular dystrophy, visual impairment or intellectual disability)”.[32]
The most obvious difficulties are physical:[2]
- Poor balance
- Poor combining of different movements to achieve a goal
- Handwriting difficulties
- Speech production issues
The full diagnostic criteria is available here.
Interventions[edit | edit source]
Previously, deficit oriented approaches were used to address these issues. This approach aimed to address underlying deficits in one system (e.g. the nervous system) with interventions that were targeted at specific structures (e.g. the cerebellum or sensory processes, such as vision or proprioception)[33] in order to improve the performance of the entire system (reading, writing, movement etc).[2]
However, contemporary theories suggest that motor performance results from a dynamic relationship between the environment, body and task. In this approach, motor deficits are seen in terms of motor learning and motor control.[2] Performance or task-oriented approaches are, therefore, used to encourage motor learning.
In task-orientated interventions, there is a focus on teaching functional skills that are necessary to complete/participate in a certain activity.[34] Children are given the opportunity to try to solve a movement problem. During this process, they may work out a number of ways to complete a task. They are also encouraged to experience the impact of their different solutions on their bodies or the environment.[34] The interaction between the task, environment and child is, therefore, the key to the treatment.[2]
- Cognitive Orientation to daily Occupational Performance (CO-OP)
- Based on the theory that DCD is a motor learning problem, rather than a neurodevelopmental difficulty
- It is task and process-orientated and it aims to teach functional skills that children need/want to perform in order to address activity and participation goals
- Cognitive motor neuro-scientific approach (i.e. brain behaviour)
- Ecological intervention (i.e. increasing a child’s participation through changing the environment)[35]
However, evidence suggests that gains made by children with DCD using these motor-based interventions are small or non-existent.[2]
The Good News[edit | edit source]
- Exercise can be beneficial
- Practice makes perfect
- Resources:
References[edit | edit source]
- ↑ Xcitesteps. What are developmental disabilities? Available from: http://www.xcitesteps.com/faqs/developmental-disabilities/ (accessed 9 August 2021).
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 2.21 2.22 2.23 2.24 2.25 2.26 2.27 2.28 Prowse T. The Social, Cognitive and Emotional Development of Children - Developmental Disabilities Course. Plus , 2021.
- ↑ Boyle CA, Boulet S, Schieve LA, Cohen RA, Blumberg SJ, Yeargin-Allsopp M et al. Trends in the prevalence of developmental disabilities in US children, 1997-2008. Pediatrics. 2011;127(6):1034-42.
- ↑ Zablotsky B, Black LI, Maenner MJ, Schieve LA, Danielson ML, Bitsko RH. Prevalence and trends of developmental disabilities among children in the United States: 2009-2017. Pediatrics. 2019;144(4):e20190811.
- ↑ Ganguly J, Kulshreshtha D, Almotiri M, Jog M. Muscle tone physiology and abnormalities. Toxins (Basel). 2021;13(4):282.
- ↑ Madhok SS, Shabbir N. Hypotonia. [Updated 2020 Sep 19]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK562209/
- ↑ Neki NS, Chhabra A. Benign joint hypermobility syndrome. Journal of Mahatma Gandhi Institute of Medical Sciences. 2016; 21(1):12-8.
- ↑ Simpson MMR. Benign Joint Hypermobility Syndrome: Evaluation, Diagnosis, and Management. J Am Osteopath Assoc. 2006;106(9): 531–536.
- ↑ Easton V, Bale P, Bacon H, Jerman E, Armon K, Macgregor AJ. A89: the relationship between benign joint hypermobility syndrome and developmental coordination disorders in children. Arthritis & Rheumatology. 2014;66(S3):S124.
- ↑ Palmer S, Bailey S, Barker L, Barney L, Elliott A. The effectiveness of therapeutic exercise for joint hypermobility syndrome: a systematic review. Physiotherapy. 2014; 100(3): 220-7.
- ↑ Mandy W, Wang A, Lee I, Skuse D. Evaluating social (pragmatic) communication disorder. J Child Psychol Psychiatr. 2017;58:1166-75.
- ↑ Norbury CF. Practitioner review: Social (pragmatic) communication disorder conceptualization, evidence and clinical implications. J Child Psychol Psychiatry. 2014;55(3):204-16.
- ↑ Mayo Clinic. Autism spectrum disorder. Available from: https://www.mayoclinic.org/diseases-conditions/autism-spectrum-disorder/symptoms-causes/syc-20352928 (accessed 9 August 2021).
- ↑ Crasta JE, Salzinger E, Lin MH, Gavin WJ, Davies PL. Sensory processing and attention profiles among children with sensory processing disorders and autism spectrum disorders. Front Integr Neurosci. 2020;14:22.
- ↑ Licari MK, Alvares GA, Varcin K, Evans KL, Cleary D, Reid SL et al. Prevalence of motor difficulties in autism spectrum disorder: analysis of a population-based cohort. Autism Res. 2020;13(2):298-306.
- ↑ Medscape. Autism Spectrum Disorder | Clinical Presentation. Available from: https://www.youtube.com/watch?v=FCejya1WWC8 [last accessed 9/8/2021]
- ↑ Bremer E, Crozier M, Lloyd M. A systematic review of the behavioural outcomes following exercise interventions for children and youth with autism spectrum disorder. Autism. 2016;20(8):899-915.
- ↑ Azeredo A, Moreira D, Barbosa F. ADHD, CD, and ODD: Systematic review of genetic and environmental risk factors. Res Dev Disabil. 2018;82:10-19.
- ↑ Fliers E, Rommelse N, Vermeulen SH, Altink M, Buschgens CJ, Faraone SV et al. Motor coordination problems in children and adolescents with ADHD rated by parents and teachers: effects of age and gender. J Neural Transm (Vienna). 2008;115(2):211-20.
- ↑ Kaiser ML, Schoemaker MM, Albaret JM, Geuze RH. What is the evidence of impaired motor skills and motor control among children with attention deficit hyperactivity disorder (ADHD)? Systematic review of the literature. Res Dev Disabil. 2015;36C:338-57.
- ↑ Mokobane M, Pillay BJ, Meyer A. Fine motor deficits and attention deficit hyperactivity disorder in primary school children. S Afr J Psychiatr. 2019;25:1232.
- ↑ Rassovsky Y, Alfassi T. Attention improves during physical exercise in individuals with ADHD. Front Psychol. 2019;9:2747.
- ↑ Piepmeier AT, Shih CH, Whedon M, Williams LM, Davis ME, Henning DA et al. The effect of acute exercise on cognitive performance in children with and without ADHD. Journal of Sport and Health Science. 2015;4(1):97-104.
- ↑ Vysniauske R, Verburgh L, Oosterlaan J, Molendijk ML. The Effects of Physical Exercise on Functional Outcomes in the Treatment of ADHD: A Meta-Analysis. J Atten Disord. 2020;24(5):644-54.
- ↑ TED. Every kid needs a champion | Rita Pierson. Available from: https://www.youtube.com/watch?v=SFnMTHhKdkw [last accessed 9/8/2021]
- ↑ TED. Grit: the power of passion and perseverance | Angela Lee Duckworth. Available from: https://www.youtube.com/watch?v=H14bBuluwB8 [last accessed 9/8/2021]
- ↑ TED. Dr. Dean Ornish: Your genes are not your fate. Available from: https://www.youtube.com/watch?v=z_VdcDJAlWQ [last accessed 9/8/2021]
- ↑ McMahon K, Anand D, Morris-Jones M, Rosenthal MZ. A path from childhood sensory processing disorder to anxiety disorders: the mediating role of emotion dysregulation and adult sensory processing disorder symptoms. Front Integr Neurosci. 2019;13:22.
- ↑ Kumpel SH. Measuring awareness of sensory processing disorder among college students and professionals in early childhood development [dissertation]. Bakersfield: California State University, 2013.
- ↑ 30.0 30.1 30.2 30.3 Pollock N. Sensory integration: A review of the current state of the evidence. Occupational Therapy Now. 2009;11(5):6-10.
- ↑ Wheadon A, Fedoruk R. Intense exercise as a change agent for improving functional outcomes in children with sensory processing challenges. 2020.
- ↑ 32.0 32.1 Harris SR, Mickelson ECR, Zwicker JG. Diagnosis and management of developmental coordination disorder. CMAJ. 2015;187(9):659-65.
- ↑ Sugden D. Current approaches to interventions in children with developmental coordination disorder. Developmental Medicine and Child Neurology. 2007;49:467-71.
- ↑ 34.0 34.1 CanChild. Management - is intervention important for children with DCD? Available from: https://www.canchild.ca/en/diagnoses/developmental-coordination-disorder/management (accessed 9 August 2021).
- ↑ Sugden D. Intervention for children with Developmental Coordination Disorder: working with professionals and parents. Available from: https://www.pearsonclinical.co.uk/Sitedownloads/ot-learn/2015-presentations/david-sugden-slides.pdf (accessed 9 August 2021).