Cyclist's palsy
Original Editor - Arno De Maeyer
Top Contributors - Lucinda hampton, Wanda van Niekerk, Evan Thomas, Kim Jackson, Kenneth de Becker, Vanessa Rhule, Scott Buxton, Anas Mohamed, Chrysolite Jyothi Kommu, Admin, Arno De Maeyer, Laura Ritchie, Wendy Walker, Naomi O'Reilly and Claire Knott
Description[edit | edit source]
Cycling is a fun, healthy exercise. However, it can take its toll on the body with inadequate or over-training, poor cycling posture or an incorrect bike fit.[1] Hand pain can become an issue, one study reporting that 31% of cyclists experienced some form of overuse hand pain[2].
(See also cyclist's back, cyclist's neck, cyclist's knee)
Pain and/or tingling and numbness can occur in various locations such as: the wrist; the ulnar side of the hand; the thumb side of the hand. This occurs as a result of:
- Too much pressure through the hands and nerves and compression of the blood vessels;
- The wrist being held in an extended position thus stretching soft tissue structures of the wrist;
- Insufficient core muscles causing excess weight on hands and or rocking of the pelvis;
- High saddle or low handlebars causing excess weight borne by upper limbs;
- Over-inflated tires, small wheels, skinny tires, all causing more vibrations in hands.
The video below gives a good summary of Cyclist's Hand
Specific Cyclists' Hand Injuries[edit | edit source]
Ulnar Nerve or Cyclist's Palsy[edit | edit source]
Typically the ulnar nerve becomes irritated and compressed in the wrist within or distal to Guyon's canal, due to the pressure exerted on the hands on the handlebars. This is even intensified when riding on rough terrain. Furthermore, when cycling, people often have a hyperextended position of the wrist resting on the handlebars or hoods, contributing to the neuropathy by compressing and stretching the nerve as it passes from the wrist to the hand.[4]
The symptoms include:
- Numbness
- Tingling
- Weakness
- Clumsiness
- Cramping
- Pain
- Possible motor limitation
The term palsy is used because the cyclist's hand often develops muscle paralysis. The affection can impact both sensory and motor functions of the hand, depending on the branch of the ulnar nerve that is affected.[4]
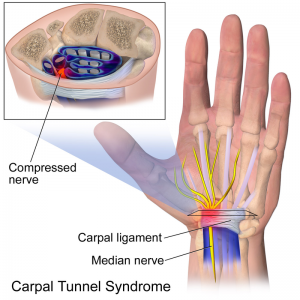
Median Nerve Compression / Carpal Tunnel Syndrome(CTS)[edit | edit source]
Compression of the median nerve – which causes tingling in the thumb, index, middle and ring finger – is called carpal tunnel syndrome. The carpel tunnel (a compact region at the wrist) is surrounded by the carpal bones on the dorsum of the wrist and tough connective tissue on the ventral aspect. Carpal tunnel syndrome (CTS), which is an overuse injury, occurs when the median nerve on the palm side of the wrist is compressed affecting the median nerve and flexor tendons of the fingers passing through the carpal tunnel. The area then becomes inflamed and narrowed, compressing the structures and it can cause pain, tingling or weakness in the thumb, fingers, and hand.
It is difficult to determine the exact incidence rate for these 2 types of non-traumatic overuse injury, as individuals often consider this injury not severe enough to seek medical care. This means that patient records are not always available. The prevalence of hand and wrist non-traumatic ulnar or median nerve compression described in the literature (manifesting itself in sensory or motor disturbance) ranges from 10% to 70%.
Clinically Relevant Anatomy[edit | edit source]
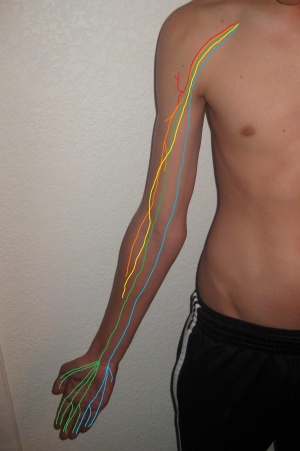
The ulnar nerve is a branch of the medial cord of the brachial plexus, which travels distally along the medial side of the arm. The nerve gives off two sensory branches which supplies sensation to the dorsomedial hand, the 5th digit, and half the 4th digit. At the wrist, the ulnar nerve enters the hand by passing through Guyon’s Canal. This tight tunnel is formed between the hamate, the pisiform, and the piso-hamate ligament which helps keep these carpal bones together. Either within or just beyond Guyon's Canal, the ulnar nerve divides again in two motor branches. In the cyclist, it is at or just before Guyon’s Canal where compressive injury to the ulnar nerve most commonly occurs.[5].
The median nerve enters the hand through the carpal tunnel, deep to the flexor retinaculum along with the tendons of flexor digitorum superficialis, flexor digitorum profundus, and flexor pollicis longus. From there, it is divided into recurrent muscular branch and digital cutaneous branch, supplying the thumb, part of flexor pollicis brevis and skin of region shown thumb and digits 2,3 and half of 4.
Epidemiology/Etiology[edit | edit source]
Cyclist's palsy typically develops during long-distance or prolonged cycling and occurs with both mountain bike and road cyclists.[6] The position of the hands while holding the handlebar puts pressure on the nerves in the wrist. This pressure of holding the handlebar in combination with vibrations from the road or trails can be enough to damage the nerve due to compression. Especially when cycling downhill, a large part of the body weight is supported by the hands-on the corner of the handlebar. This leads to an even higher load on Guyon’s canal in the wrist or in the carpal tunnel. Cyclists also often place their hands in an hyperextended position on the handlebar, stretching sensitive structures in the wrist. All this can cause neuropraxia, a disorder of the peripheral nervous system in which there is a temporary loss of motor and/or sensory function due to blockage of nerve conduction.[4] Akuthota et al (2005)[6] concluded in a nerve conduction study of long-distance cyclists' hand nerves, that long-distance cycling may promote physiologic changes in the deep branch of the ulnar nerve and exacerbate symptoms of carpal tunnel syndrome.[6]
Other factors which can contribute to the occurrence of cyclist's palsy are:
- General fatigue, which leads to increased weight bearing on the hands[7]
- Not changing hand position on the handlebar frequently enough[7]
- Wearing ill-fitted or worn-out gloves[7]
- Improper bike fit[7]
- Using worn-out handlebar padding[7]
- Incorrect shape or size of the handlebar[7]
- Too high or downward tilted saddle causing improperly distributed body weight on the hands holding the handlebar[7]
Characteristics/Symptoms[edit | edit source]
The exact symptoms of cyclist's palsy may vary from one person to another, depending on the severity of the condition[1].
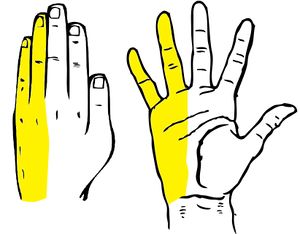
Compression of the sensory branch of the ulnar nerve will present itself in sensory disturbances, such as numbness and tingling in the ulnar innervated areas of the affected hand, namely the ring finger and the little finger. These symptoms are easily recognisable and often go away within a day or two.[8]
Compression of the motor branches of the nerves will present itself in motor deficits, such as weakness, clumsiness and possibly motor limitation due to loss of muscle function in the thumb or hand. The median nerve could cause thenar eminence wasting. These latter symptoms are often less distinguishable and if no sensory fibers are equally affected, a patient might continue cycling with an on-going compression of the motor branch, not realizing that there is an injury until a severe lesion develops. Correct and timely treatment of innervation injuries are important and the healing process can take anything from weeks to months. In case a patient does not receive treatment, the nerve entrapment can cause atrophy of the involved hand muscles or paresthesia of the hand muscles innervated by the nerve, which will be permanent.[9]
Differential Diagnosis[edit | edit source]
Apart from nerve compression resulting from pressure during cycling, there are a number of other injuries that can cause neuropathy in the wrist by compression.[10]
- Fracture of the hamate bone
- Hypermobile pisiform bone
- Occupational traumatic neuritis
- Tenosynovitis of the flexor tendons
- Crutch use
- osteoarthritis,
As always in an assessment ask about recent trauma and note any red flags.
Diagnostic Procedures[edit | edit source]
In suspected nerve damage additional imaging such as ultrasound, CT-scan, and MRI can be performed to help confirm the diagnosis and determine the location of compression. When we are able to localize the exact place on the hand where the patient has a numb feeling, we can differentiate between carpal tunnel syndrome or ulnar tunnel syndrome.
Electrodiagnostic studies can be used to localize the site of nerve compression and to determine the extent of the defect. More specifically, electromyography (EMG) measures the electrical activity of muscles at rest and during contraction, and may reveal degeneration in the nerves supplying a muscle when the patient is suffering from persistent weakness.
Medical Management[edit | edit source]
Cyclist's palsy is a type of nerve injury which is self-limiting and in most cases does not need medical intervention. Depending on the severity of the condition the following are options
- Oral or topical NSAID's medication to treat the inflammation
- In severe cases corticosteroid injections may be required to reduce swelling and ease the pressure on the nerve
- In Carpal Tunnel Syndrome, wrist splinting could help.
- If other treatments fail, a doctor might try a corticosteroid injection of the Guyon's Canal or carpal tunnel or decompression surgery (i.e. to release the nerve and take away the pressure).[11][12]
Subjective Assessment[edit | edit source]
Questions to ask include:
- Past hand problems?
- Any accidents falling off bike?
- Check for any red flags i.e recent malignancy, unremitting pain, weight loss etc.
- Is it chronic, sub-acute or acute?
- Has a Bike Fit been done?
- Recent changes in bike handlebars or training regime/terrain?
- What type of work do they do, as this may predispose to wrist pain
- How long does it take for pain to come on?
- Is it only with certain movements or terrains?
Objective Assessment[edit | edit source]
- Bike position and posture
- Assess the client on the bike
- Cycling position - look out for:
- Extended wrist
- Forward tip or too high saddle
- Elbow joints locked out
- Hunched upper back
- Tight grip (All these can contribute to a potential cause of the problem).
- A clearing upper limb assessment should be undertaken noting any aberrations from the norm.
- Check movement in wrist and finger joints.
- Muscle lengths and strength should be assessed in the major muscles involved in hand and forearm movements. These include:
- Core muscles as involved in stabilising/supporting upper limb.
- Forearm muscles
- Wrist and hand muscles
- Neurodynamic tests: ULTT's
Outcome Measures[edit | edit source]
- Brigham and Women's Carpal Tunnel Questionnaire
- VAS
- Upper Extremity Functional Index
- DASH outcome measure
Physical Therapy Management[edit | edit source]
Prevention[edit | edit source]
In order to avoid cyclist's palsy or to reduce the prevalence of this type of non-traumatic hand and wrist injury during cycling, it is important to have a look at the prevention strategies. An effective measure is to cushion the pressure points, by using padded handlebars, handlebar grips ( see image) or padded cycling gloves. This provides an extra layer of fat tissue inside the palm of the hands so that there is better shock absorption and protection from pressure.[4] Also, the position of the hands-on the handlebar is important. The cyclist should try to avoid a hyperextended position of the wrist. Furthermore,during a long ride, it is advisable to change hand position regularly.[4][13]
Individual adaption of the type of handlebar and the consequential riding position is equally crucial in the prevention of this ailment. Using an upright horn handlebar instead of a drop model might be considered for certain individuals. This will bring the torso position more upright and will diminish the pressure on the hands. Another option is to equip the bike with both a conventional handlebar and an aerobar, which will allow the cyclist to lean forward and to rest the forearms on pads during certain parts of the track so that pressure can be taken away from the hands temporarily during a cycling trip.[4]
Enthusiastic long-distance cyclists should also adopt a comfortable and resilient riding posture. If the trunk gets tired or in case of general fatigue, the hands will invariably bear more weight to stabilize the rider on the bike. Developing a better posture on the bike requires strong trunk muscle endurance. Make sure to sit in a comfortable position on the bike. The torso should lean forward at about 45° to 50°. The shoulders should be relaxed. The arms should be at 90° to the torso. The elbows should be slightly bent, not straight or locked. Bent elbows will act as shock absorbers for any bumps in the road and will alleviate shocks from the hands. The hands should not be gripping excessively, but resting smoothly on the handlebar.[4]
Finally, the cyclist should make sure to ride on the right size of bicycle and to adapt the position of the saddle and handlebar to make sure that these allow to sit on the bike in a normal position.
Exercises[edit | edit source]
Exercises to focus on include:
Hand Strengthening Exercises[edit | edit source]
- Finger bending exercise: start from a stretched hand, bend your fingers of the affected hand in a right angle and hold for 10 seconds while keeping your fingers straight; repeat 5 times.
- Finger squeeze: place a small object (for example: pen, coin, sheet of paper) between 2 fingers of the affected hand and hold for 10 seconds; repeat 5 times for each pair of fingers and then move on to the next set of fingers.
- Grip strengthening: use a rubber ball and squeeze it with the affected hand; hold for 10 seconds and repeat 10 times. Build up gradually to 3 sets of 10.[13]
Stronger hand muscles will also help to prevent cyclist's palsy from recurring.
Range of Motion Exercises of the Neck and Wrist[edit | edit source]
- Cervical range of motion: rotation of the head, flexion and extension of the neck, and side bending of the neck; hold each position for 10 seconds and then return to neutral position.
- Wrist range of motion: bend the wrist forward and back to neutral position, then bend the wrist backward and back to neutral position; hold each position for 5 seconds; repeat 10 times.[13]
If a transient "palsy" has occurred with temporary motor paralysis with minimal sensory and autonomic function loss it is a reversible process, if the mechanical compression seizes the nerve will regenerate on its own and function of the muscles will be restored. In more severe handlebar palsy cases it can take weeks to several months to heal, depending on the severity of the condition. While the nerve and muscles are regenerating, the patient needs to interrupt his sport activities for a while.[13]
[See Neuropathies for physiotherapy management]
Other Modalities[edit | edit source]
Other modalities to use include:
- Ice(cryotherapy)/heat
- Electrical Stimulation
- Low level laser
- Ultrasound
- Active release techniques
Conclusion[edit | edit source]
Patterson et al (2008)[8] reported in a prospective study of cyclists that Cyclist's palsy occurs at high rates in both experienced and inexperienced cyclists. Steps may be taken to decrease the incidence of cyclist's palsy; these include wearing cycling gloves, ensuring proper bicycle fit, and frequently changing hand position.[8] Hopefully then the cyclist can go on to have fun, hand issue free, rides.
References[edit | edit source]
- ↑ 1.0 1.1 Gloria,C. Cohen, MD, CCFP. Cycling Injuries. Canadian Family Physician, VOL 39, March 1993
- ↑ Schwellnus, Martin & Derman, Wayne. (2014). Common injuries in cycling: Prevention, diagnosis and management. South African Family Practice. 47. 14-19. 10.1080/20786204.2005.10873255. Available from: https://www.researchgate.net/publication/275065012_Common_injuries_in_cycling_Prevention_diagnosis_and_management (last accessed 8.9.2019)
- ↑ Global Cycling Network How To Prevent Numbness Or Pain In Your Hands Whilst Cycling Available from: https://www.youtube.com/watch?v=FbyVuuGXmDY&t=158s (last accessed 10.9.2019)
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Cohen GC. Cycling injuries. Canadian Family Physician. 1993 Mar;39:628. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2379777/ (last accessed 12.9.2019)
- ↑ Praktijkgids Pols-en handletsels. Meeusen, R. p. 74-77
- ↑ 6.0 6.1 6.2 Akuthota V, Plastaras C, Lindberg K, Tobey J, Press J, Garvan C. The effect of long-distance bicycling on ulnar and median nerves: an electrophysiologic evaluation of cyclist palsy. The American journal of sports medicine. 2005 Aug;33(8):1224-30. Available from: https://www.ncbi.nlm.nih.gov/pubmed/16000656 (last accessed 9.9.2019)
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 Dettori NJ, Norvell DC. Non-traumatic bicycle injuries. Sports medicine. 2006 Jan 1;36(1):7-18. Available from: https://www.ncbi.nlm.nih.gov/pubmed/16445308 (last accessed 12.9.2019)
- ↑ 8.0 8.1 8.2 Patterson JM, Jaggars MM, Boyer MI. Ulnar and median nerve palsy in long-distance cyclists: a prospective study. The American journal of sports medicine. 2003 Jul;31(4):585-9. Available from: https://journals.sagepub.com/doi/abs/10.1177/03635465030310041801 (last accessed 9.9.2019)
- ↑ Capitani D, Beer S. Handlebar palsy–a compression syndrome of the deep terminal (motor) branch of the ulnar nerve in biking. Journal of neurology. 2002 Oct 1;249(10):1441-5. Available from: https://www.ncbi.nlm.nih.gov/pubmed/12382163 (last accessed 12.9.2019)
- ↑ Bickerton, T. Handlebar Palsy. Where to Ride. [ONLINE] accessed on 24 September 2010. Available at http://www.wheretoridelondon.co.uk/London-262.html
- ↑ Hankey GJ, Gubbay SS. Compressive mononeuropathy of the deep palmar branch of the ulnar nerve in cyclists. Journal of Neurology, Neurosurgery & Psychiatry. 1988 Dec 1;51(12):1588-90. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1032781/ (last accessed 12.9.2019)
- ↑ Lund AT, Amadio PC. Treatment of cubital tunnel syndrome: perspectives for the therapist. Journal of Hand Therapy. 2006 Apr 1;19(2):170-9. Available from: https://www.ncbi.nlm.nih.gov/pubmed/16713864 (last accessed 12.9.2019)
- ↑ 13.0 13.1 13.2 13.3 Ulnar Neuropathy. Primary Sports Care Medicine. December 2016 Available from: https://www.primarycaresportsmedicine.com/wp-content/uploads/2016/12/ELBOW-ULNAR-NEUROPATHY.pdf (last accessed 12.9.2019)