Current Management of Lisfranc Injuries
Top Contributors - Ewa Jaraczewska and Jess Bell
Introduction[edit | edit source]
Lisfranc injuries are rare, but severe midfoot injuries. They are often missed on initial assessment. About 20% of these injuries. are not diagnosed in time or at the point of the injury.[1] A subtle, but unstable injury may receive conservative treatment when surgery should be considered. [2] When undetected, Lisfranc complex injuries have long-term consequences. [3] This article reviews conservative and surgical treatment principles in Lisfranc injuries.
Definition and Epidemiology[edit | edit source]
The Lisfranc joint is where the tarsal bones connect to the metatarsal bones - i.e. the tarsometatarsal (TMT) joint. A 'Lisfranc injury' was first described in 1815 by the French surgeon and gynaecologist Jacques Lisfranc de St. Martin (1787- 1847). It is a condition where one or more metatarsal bones are displaced.[4]
According to Ponkilainen et al.[5], the epidemiology of mid-foot injuries, including Lisfranc, is unknown. A five-year study found that out of all mid-foot traumas, Lisfranc injury occurred in 18.2% of cases. A survey by Desmond and Chou[6] confirmed this type of injury in less than 2% of all fractures. However, statistics suggest that diagnosis is not always adequate. Late or missed diagnosis occurs in 20% of cases.[7] It has been found that:
- Lisfranc injuries are more common in men; the reported ratio is 4.25:1.[8]
- The most common cause of traumatic injury is low-energy trauma[9] (e.g. falling over a plantar flexed foot).[1]
- The most frequent high-energy trauma is a car accident, followed by a motorcycle accident.[8]
- The most common fractures include the second and fifth metatarsal bones[10], followed by the cuboid bone.[8]
- Multiple metatarsal fractures are not uncommon. In these cases, fractures of the third metatarsal are associated with a fracture of either the second or fourth metatarsal.[10]
- Lisfranc injuries occur more frequently in athletes.[11]
Risk Factors[edit | edit source]
The following can increase the risk of an unstable injury:[9]
- Intraarticular fractures in the two lateral tarsometatarsal joints
- Female gender
- A shorter height of the second tarsometatarsal joint
Clinically Relevant Anatomy[edit | edit source]
Lisfranc injuries involve trauma to the tarsometatarsal (TMT) joint. The descriptions of this injury vary significantly, as does the documentation of the anatomy of the Lisfranc joint.[12]
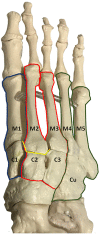
The Lisfranc joint complex includes the first to fifth metatarsal bones, three cuneiform bones, the cuboid, the interconnecting ligaments, capsules, and reinforcing tendons. The primary role of this joint is to provide mid-foot stability.[3] The metatarsal bases create an arch structure, with the second metatarsal bone as its midpoint (i.e. keystone).[3] It articulates with the second cuneiform bone and sits between the first and third cuneiforms. The following tarsometatarsal joint ligaments add to the strength of the joint:[3]
- Dorsal ligaments (longitudinal direction)
- Interosseous ligaments (transverse direction)
- Plantar ligaments (oblique direction)
Three tarsometatarsal synovial joint systems relate to the three columns of the foot:[3]
- Medial column formed by the base of the first metatarsal and medial cuneiform
- Middle column formed by the second and third metatarsals and respective cuneiforms
- Lateral column formed by the fourth and fifth metatarsals and cuboid
You can read about the foot bones and ligaments here.
Mechanism of Injury / Pathological Process[edit | edit source]
Lisfranc injuries can be caused by:
- Direct, high energy level: crush injury to the joint region, industrial accident (heavyweight lands on foot when dropped from a height), fall from a height, motor vehicle accident.[11]
- Indirect, low level of energy: sports injury that "usually involves a longitudinal force while the foot is plantar flexed with a medial or lateral rotational force",[11] stepping off a curb with the foot forcefully plantar flexed,[13] ground-level fall.
Classification of Lisfranc injuries includes the following: [14]
- Traditional dislocation (first and second tarsometatarsal ligament tear)
- Medial column dislocation (second tarsometatarsal and medial-middle cuneiform ligament tear)
- Proximal extension dislocation (first, second, and medial-middle cuneiform ligament tear)
Weak dorsal transverse ligaments and no ligaments connecting the first and second metatarsals are factors that increase the risk of joint dislocation in a dorsal and lateral direction. [15]
Low-energy injuries include partial injuries (sprains). In this type of injury, the plantar tarsometatarsal ligaments remain intact, and the injury is stable.[16]
Diagnosis[edit | edit source]
Assessment[edit | edit source]
Each assessment should include the following components:[16]
- An interview/medical history
- Listen and understand the mechanism of the injury
- Find out the exact injury mechanism, including the position of the foot, the direction of force, and the extent of energy involved.
- Ask for location of the pain to define potential structures involved.
- Palpation of the midfoot
- It helps to localise an area suspicious for injury.
- Assessment is limited by the soft-tissue swelling, which produces a diffuse type of pain.
- When pain is present at the N spot (the apex of the navicular bone), a navicular stress fracture must be ruled out.[17]
- Soft tissue inspection
- Checking for plantar ecchymosis (bruising) at the midfoot
- Provocative manoeuvres to evaluate for instability: squeezing of the midfoot, pronation, supination, abduction, adduction, single limb weight-bearing
- squeezing the mid-foot: The examiner squeezes the medial and lateral parts of the foot with one hand while the tender area is palpated with the other hand.[18]
- testing abduction/adduction: The examiner stabilises the calcaneus and talus with one hand while the other hand moves the foot medially to test for adduction and laterally to test for abduction.[19]
- single-limb weight-bearing assess patient's ability to tolerate weightbearing on the injured foot
- Tinel’s test
- Passive range of motion in the sagittal and coronal planes of all three columns of the foot
Clinical Presentation[edit | edit source]
- Diffuse pain in the mid-foot, usually lasting for a few days. Pain refers to the third toe when pressure is applied at the mid-foot [1]
- Tenderness to palpation of the mid-foot[16]
- Reproduction of pain with passive motion of the forefoot[16]
- Inability to weight bear[16] / difficulties weight bearing
- Development of compensatory strategies for pain and mobility restrictions, including wearing stiff leather shoes or boots[1]
- Pitting oedema[1]
- Flattening of the transverse arch[1]
- Plantar ecchymosis at the midfoot due to ligament rupture[16]
Diagnostic Procedures[edit | edit source]
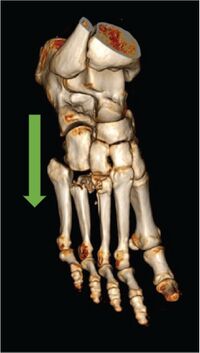
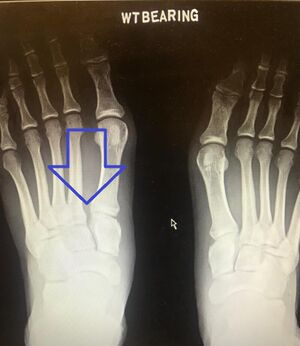
- Radiography to evaluate diastasis at the TMT joints includes:[3]
- Standard, three-view films of the foot—anteroposterior, 30-degree internal oblique, and lateral views.
- The patient should be standing for all films, with weight-bearing.
- An x-ray of both feet should be completed for comparison.
- Radiographic images completed in non-weight-bearing positions tend to miss Lisfranc injuries 20-50% of the time.
According to Yan et al.[3], the diagnostic accuracy of radiographs is low. If clinical symptoms continue, but the X-ray is negative, the patient should be referred for computed tomography (CT) or magnetic resonance imaging (MRI).[3]
- CT to detect non-displaced fractures and minimal osseous subluxation.[20]
- MRI to evaluate ligament abnormalities.[20]
Differential Diagnosis[edit | edit source]
Differential diagnosis to Lisfranc injury includes: midfoot sprain, metatarsal fracture, cuboid fracture, posterior tibialis tendon dysfunction, and compression injuries to the navicular.[21]
Recommendations for Intervention[edit | edit source]
- Conservative management:[3]
- Lisfranc injuries without evidence of instability (<2 mm diastasis)
- Extra-articular fractures with stability confirmed by weight-bearing[16]
- Operative management:
- All types of injury not listed above as suitable for surgical management
- There is a lack of one optimal surgical treatment
- There is also a lack of concrete evidence supporting any particular treatment modality
- All types of injury not listed above as suitable for surgical management
Management / Intervention[edit | edit source]
Conservative Management[edit | edit source]
The following conservative management is recommended:[1]
- Pain management
- Medial arch support. The type of support depends on the degree of injury and can include wearing a boot, supportive shoes or a customised orthotic
- Immobilisation: immobilise in a cast or boot for 6-10 weeks to offload the foot
- Limit weight-bearing activities: do not push for full weight-bearing
- Arch support: consider arch support in the boot and the cast
- Strengthening programme for:
- Intrinsics of the foot to improve dynamic foot support
- Toe flexors to help with toe push-off
- Strengthening exercises for tibialis posterior
- Isometric strengthening for peroneus longus
- Taping the metatarsal arch to improve stability. This video demonstrates using rigid tape in foot arch supporting taping. Using an elastic tape is another taping option for arch support. Be aware of precautions when using rigid or elastic taping techniques, including skin condition, skin and other allergies, and patient's medical condition. Using taping technique requires specialty training.
- Cardiovascular fitness
- Core strengthening with progression from supine, adding movement of arms and legs, trough dynamic positions, to whole-body movements, agility and balance. Examples include:
- Supine: breathing exercises to activate pelvic floor, alternate arm reaches, alternate knee lifts, combine opposite arm and leg, knee extension as a progression from alternate knees in supine, alternate straight leg raise.
- Standing: alternate arm raises, add exercises with Theraband.
- Agility and balance: lunges, stepping, stepping to the side, side squats, high stepping, hand to opposite heel while moving.
Surgical Management[edit | edit source]
The timing of surgery remains controversial[2] , however when the injury is unstable, surgical management for the ligaments, bone or a combination of both is indicated:[16]
- Reduction and immobilisation of any dislocation-producing skin and soft tissue tension.[16]
- In high-energy injury, a temporary external fixation may be recommended, especially when foot alignment cannot be maintained in a splint.[16]
- Tissue swelling must be resolved before definitive surgery is scheduled .[16] The general rule for the timing of the surgery is "the sooner, the better, as long as the swelling is manageable"[3], which may take up to 10-14 days after injury.
- Open reduction and internal fixation (ORIF) with transarticular screw fixation.[16]
- Controversy around the optimal implant size and implant type
- Inconsistent recommendation regarding removal of definitive implants, and the optimal timing of implant removal
- ORIF with primary arthrodesis when a pure ligamentous pattern is present.[16]
- The long-term effect is unknown. A systematic review compared primary partial arthrodesis to ORIF and it shows that the American Orthopaedic Foot and Ankle Society (AOFAS) score of ORIF patients was 72.5/100. The AOFAS-score of patients with primary partial arthrodesis was 88% within one year of follow-up. This study compared six articles to 193 patients. Conclusion: Both therapies have equivalent results but the primary partial arthrodesis has a small advantage in terms of clinical outcomes.[26]
- Lower hardware removal rates as compared to ORIF alone
- High percent of patients returned to pre-operative level of activity
- Significant reduction in planned and unplanned secondary surgeries
Good anatomical reduction in the surgery significantly improves the outcome.[1] Helene Simpson
Resources[edit | edit source]
- Paek S, Mo M, Hogue G. Treatment of paediatric Lisfranc injuries: A systematic review and introduction of a novel treatment algorithm. Journal of Children's Orthopaedics. 2022 May 10:18632521221092957.
- van den Boom NA, Stollenwerck GA, Lodewijks L, Bransen J, Evers SM, Poeze M. Lisfranc injuries: fix or fuse? a systematic review and meta-analysis of current literature presenting outcomes after surgical treatment for Lisfranc injuries. Bone & Joint Open. 2021 Oct 8;2(10):842-9.
- Lakey E, Hunt KJ. Patient-Reported Outcomes in Foot and Ankle Orthopedics. Foot Ankle Orthop. 2019 Jul 19;4(3):2473011419852930.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Simpson H. Lisfranc Injuries Course. Plus, 2022.
- ↑ 2.0 2.1 Singh A, Lokikere N, Saraogi A. Unnikrishnan PN, James Davenport J. Missed Lisfranc injuries—surgical vs conservative treatment. Ir J Med Sci 2021;190:653–656.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 3.9 Yan A, Chen SR, Ma X, Shi Z, Hogan M. Updates on Lisfranc Complex Injuries. Foot Ankle Orthop. 2021 Jan 25;6(1):2473011420982275.
- ↑ Moracia-Ochagavía I, Rodríguez-Merchán EC. Lisfranc fracture-dislocations: current management. EFORT Open Rev. 2019 Jul 2;4(7):430-444.
- ↑ Ponkilainen VT, Laine HJ, Mäenpää HM, Mattila VM, Haapasalo HH. Incidence and characteristics of midfoot injuries. Foot & Ankle International. 2019 Jan;40(1):105-12.
- ↑ Desmond EA, Chou LB. Current concepts review: Lisfranc injuries. Foot Ankle Int. 2006 Aug;27(8):653-60.
- ↑ Myerson MS, Cerrato R. Current management of athletes' tarsometatarsal injuries. Instr Course Lect. 2009;58:583-94.
- ↑ 8.0 8.1 8.2 Sobrado MF, Saito GH, Sakaki MH, Pontin PA, Santos AL, Fernandes TD. Epidemiological study on Lisfranc injuries. Acta Ortopédica Brasileira. 2017 Jan;25:44-7.
- ↑ 9.0 9.1 Stødle AH, Hvaal KH, Enger M, Brøgger H, Madsen JE, Husebye EE. Lisfranc injuries: incidence, mechanisms of injury and predictors of instability. Foot and Ankle Surgery. 2020 Jul 1;26(5):535-40.
- ↑ 10.0 10.1 Petrisor BA, Ekrol I, Court-Brown C. The epidemiology of metatarsal fractures. Foot & ankle international. 2006 Mar;27(3):172-4.
- ↑ 11.0 11.1 11.2 Buchanan BK, Donnally III CJ. Lisfranc dislocation. InStatPearls [Internet] 2021 Jul 25. StatPearls Publishing.Last Update: February 2, 2022.
- ↑ DeLuca MK, Boucher LC. Morphology of the Lisfranc Joint Complex. The Journal of Foot and Ankle Surgery. 2022 Jul 25.
- ↑ Kalia V, Fishman EK, Carrino JA, Fayad LM. Epidemiology, imaging, and treatment of Lisfranc fracture-dislocations revisited. Skeletal Radiol. 2012 Feb;41(2):129-36.
- ↑ Porter DA, Barnes AF, Rund A, Walrod MT. Injury pattern in ligamentous Lisfranc injuries in competitive athletes. Foot & Ankle International. 2019 Feb;40(2):185-94.
- ↑ Shah NN, MD, DeMeo J. Keys To Diagnosing And Treating Lisfranc Injuries. Podiatry Today 2016. Available from https://www.hmpgloballearningnetwork.com/site/podiatry/keys-diagnosing-and-treating-lisfranc-injuries [last access 22.10.2023]
- ↑ 16.00 16.01 16.02 16.03 16.04 16.05 16.06 16.07 16.08 16.09 16.10 16.11 16.12 Clare MP. Lisfranc injuries. Curr Rev Musculoskelet Med. 2017 Mar;10(1):81-85.
- ↑ Young CC, Mark W. Niedfeldt MW, Morris GA, Kevin J. Eerkes KJ.Clinical Examination of the Foot and Ankle. Prim Care Clin Office Pract 2005;32:105–132
- ↑ Hattam P, Smeatham A. Special Tests in Musculoskeletal Examination. Edinburgh: Churchill Livingstone, 2010.
- ↑ Alazzawi S, Sukeik M, King D, Vemulapalli K. Foot and ankle history and clinical examination: A guide to everyday practice. World J Orthop. 2017 Jan 18;8(1):21-29.
- ↑ 20.0 20.1 Sripanich Y, Weinberg MW, Krähenbühl N, Rungprai C, Mills MK, Saltzman CL, Barg A. Imaging in Lisfranc injury: a systematic literature review. Skeletal Radiology. 2020 Jan;49(1):31-53.
- ↑ Reischl SF, Noceti-DeWit LM. Current concepts of orthopaedic physical therapy. 2nd edition. Alexandria: Orthopaedic Section, APTA, 2006
- ↑ Sandringham Sports Physio. Foot Arch Supportive Taping.2019. Available from: https://www.youtube.com/watch?v=7QM41olCNS4 [last accessed 29/09/2022]
- ↑ Richard Blake. Taping for Arch Support with Kinesio Tape. Available from: https://www.youtube.com/watch?v=NLfzvAJgyJ4 [last accessed 22/10/2023]
- ↑ LaCroix AZ, Bellettiere J, Rillamas-Sun E, Di C, Evenson KR, Lewis CE, Buchner DM, Stefanick ML, Lee IM, Rosenberg DE, LaMonte MJ; Women’s Health Initiative (WHI). Association of Light Physical Activity Measured by Accelerometry and Incidence of Coronary Heart Disease and Cardiovascular Disease in Older Women. JAMA Netw Open. 2019 Mar 1;2(3):e190419.
- ↑ Bradley SM, Michos ED, Miedema MD. Physical Activity, Fitness, and Cardiovascular Health: Insights From Publications in JAMA Network Open. JAMA Netw Open. 2019;2(8):e198343.
- ↑ Sheibani-Rad S, Coetzee JC, Giveans MR, DiGiovanni C. Arthrodesis versus ORIF for Lisfranc fractures. Orthopedics. 2012 Jun;35(6):e868-73.