Congenital Hand Deformities
Introduction[edit | edit source]
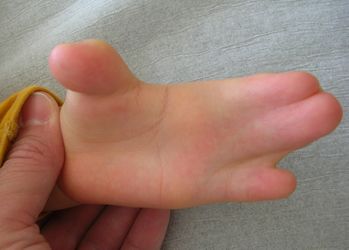
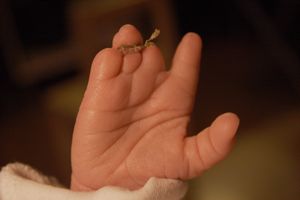
Congenital hand deformities are deformities of the hand that develop in a child before birth.[1] Congenital hand deformities are also known as- congenital hand differences[2], congenital hand anomalies[3], congenital hand conditions[4] and congenital hand problems[5].
Etiology[edit | edit source]
Congenital hand deformities usually occur between the fourth and eighth week after the embryo is formed. Failure of the transformation from arm bud cells to the upper limb can lead to an abnormal appearing/functioning upper extremity which is presented at birth. Some causes are linked to genetics while others are affected by the environment, and the rest have remained unknown.[6]
Epidemiology[edit | edit source]
Of the 1% to 2% of newborns that are born with congenital defects, 10% of these are born with upper extremity malformations.[7] Congenital hand deformities affect approximately 1 in 500 persons and present unique diagnostic and classification challenges[8]. In a study, congenital hand deformities were seen 1.5 times in male patients compared with female patients[9].
Classification[edit | edit source]
The Oberg, Manske, Tonkin (OMT) classification describes 3 groups of congenital hand deformities.[1][10]
1.Malformations: Malformations are abnormalities of formation and/or differentiation of the tissues[10]. Examples are- brachydactyly, symbrachydactyly, syndactyly, polydactyly, cleft hand/ectrodactyly, apert hand etc[1].
2.Deformations: Deformations are abnormalities that occur after the tissue is formed[10]. Examples include- constriction ring syndrome, trigger digits etc[1].
3.Dysplasias: Dysplasias are abnormalities that result from a lack of normal organization of cells into the tissue[10]. Examples- hemihypertrophy, macrodactyly, osteochondromatosis, fibrous dysplasia etc[1].
Treatment for congenital hand deformities[edit | edit source]
Specific treatment for congenital hand deformities will be determined based on:[edit | edit source]
- Age, overall health, and medical history
- Extent of the condition
- Cause of the condition
- Patient's tolerance for specific medications, procedures, or therapies
- Expectations for the course of the condition
- Parents' opinion or preference[12]
Treatment may include:[edit | edit source]
- Limb manipulation and stretching
- Splinting of the affected limbs
- Tendon transfers
- External appliances
- Physical therapy
- Correction of contractures
- Skin grafts
- Prosthetics[12]
Surgical Management of Some Common Congenital Hand Deformities[edit | edit source]
Polydactyly[edit | edit source]
An extra digit or polydactyly is one of the more common congenital hand conditions encountered in clinical practice. The commonest form of polydactyly is that of thumb duplication. In thumb polydactyly, reconstruction is usually offered. Besides the obvious cosmetic improvement, surgery also places the retained digit in a more functional position, and the reconstruction aims to enhance the stability of an often unstable metacarpophalangeal joint. While there is no real upper limit to surgery, most surgeons would prefer to do reconstruction sometime between six months and two years of age[13].
Syndactyly[edit | edit source]
Syndactyly refers to an abnormal linkage between adjacent digits. Surgery to separate the digits aims to produce a hand with as many stable and functionally independent fingers as possible. Separation is done earlier if the ring and little fingers or the index finger and thumb are involved, as the differential longitudinal growth rates between the digits will lead to bone and joint deformity if left untreated.[13]
Constriction Ring Syndrome[edit | edit source]
This condition is also known as the amniotic band syndrome or Streeter's disease. It is marked by constrictions or bands around digits or limbs. Release of the constrictions is not urgently required unless there is evidence of vascular compromise distally, such as an oedematous or ischaemic digit. Other techniques of reconstruction, such as toe transfers or lengthening procedures, may be required if the amputations are significant.[13]
Paediatric Trigger Thumb[edit | edit source]
This condition presents as a flexion deformity of the interphalangeal joint of the thumb. It is more commonly unilateral. Unlike adult trigger thumbs, it does not usually present as triggering per se, but with a flexion deformity. One important differential diagnosis is that of a clasped thumb. In more than 60% of cases, the condition will resolve spontaneously, but this requires about 48 months of waiting. As an alternative, surgical release is highly effective and has limited morbidity.[13]
Complications[edit | edit source]
Many of the congenital hand deformities are relatively minor and do not affect function. However, the appearances of the deformities have significant psychological impact on both the parents and child[13].
Physiotherapy[edit | edit source]
- A considerable amount of therapy is needed, the keystones being stretching and splinting. It is essential to have parental understanding and input.
- Community therapy services are very valuable but close communication with the hospital services is needed to ensure shared objectives and continuity of care. In some conditions therapy needs to start in the neonatal period, for instance radial clubhand, flexed proximal interphalangeal joints lacking extension and the “wind blown” conditions where the thumb or fingers lack extension.[15]
- Treatment plans geared specifically for children, achieving increased independence with activities of daily living,[16]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Oberg KC. Classification of congenital upper limb anomalies: towards improved communication, diagnosis, and discovery. Journal of Hand Surgery (European Volume). 2019 Jan;44(1):4-14.
- ↑ Sullivan MA, Adkinson JM. Congenital hand differences. Plastic Surgical Nursing. 2016 Apr 1;36(2):84-9.
- ↑ Gishen K, Askari M. Congenital hand anomalies: etiology, classification, and treatment. Journal of Craniofacial Surgery. 2014 Jan 1;25(1):284-94.
- ↑ Oda T, Pushman AG, Chung KC. Treatment of common congenital hand conditions. Plastic and reconstructive surgery. 2010 Sep;126(3):121e.
- ↑ Netscher DT. Congenital hand problems. Terminology, etiology, and management. Clinics in plastic surgery. 1998 Oct 1;25(4):537-52.
- ↑ Peng H, Wang X, Duan Y, Frey SH, Gu X. Brain morphometry on congenital hand deformities based on Teichmüller space theory. Computer-Aided Design. 2015 Jan 1;58:84-91.
- ↑ Linder JM, Pincus DJ, Panthaki Z, Thaller SR. Congenital anomalies of the hand: an overview. Journal of Craniofacial Surgery. 2009 Jul 1;20(4):999-1004.
- ↑ Sammer DM, Chung KC. Congenital hand differences: embryology and classification. Hand clinics. 2009 May 1;25(2):151-6.
- ↑ Yesilada AK, Sevim KZ, Sucu DO, Kilinc L. Congenital hand deformities-a clinical report of 191 patients. Acta chirurgiae plasticae. 2013 Jan 1;55(1):10-5.
- ↑ 10.0 10.1 10.2 10.3 Tonkin MA. Classification of congenital anomalies of the hand and upper limb. Journal of Hand Surgery (European Volume). 2017 Jun;42(5):448-56.
- ↑ OHSU. Congenital Anomalies, A Review with Cartoons, Amy L. Ladd, M.D. Available from: https://www.youtube.com/watch?v=g8JuFy5TZd4&t [Last accessed November 8, 2020]
- ↑ 12.0 12.1 John Hopkins Medicine. Congenital Hand Deformities. Available from: https://www.hopkinsmedicine.org/health/conditions-and-diseases/hand-conditions/congenital-hand-deformities (accessed 14 October 2020)
- ↑ 13.0 13.1 13.2 13.3 13.4 Ak C. Common congenital hand conditions. Singapore Med J. 2010;51(12):965.
- ↑ AboutKidsHealth. Hand/difference. Available from: https://www.youtube.com/watch?v=i690lLdBI-M [Last accessed November 8, 2020]
- ↑ Watson S. The principles of management of congenital anomalies of the upper limb. Archives of disease in childhood. 2000 Jul 1;83(1):10-7.
- ↑ Lake A. Hand therapy for children with congenital hand differences. Techniques in Hand & Upper Extremity Surgery. 2010 Jun 1;14(2):78-84.