Cerebellar Ataxia - A Case Study
Abstract[edit | edit source]
The following is a fictional case study following Mr. Sam Brown. The purpose of this case study is to explore patient management for traumatic cerebellar ataxia and the findings and challenges that may arise. Sam is a 30-year-old retail worker who suffered cerebellar damage following a motor vehicle accident. Sam was diagnosed with truncal cerebellar ataxia after showing symptoms of impaired balance and gait. After spending five days in hospital, Sam was discharged to outpatient physiotherapy. His assessment revealed several ataxia symptoms (impaired balance, dysmetria, trouble with alternating movements). Sam’s supervised and home exercise programs focused on improving gait, balance, and coordination to improve his independence. Over eight weeks in physiotherapy Sam’s ability to ambulate and complete functional tasks have progressed to be ready to return to work on modified duties, and enjoy family activities.
Introduction[edit | edit source]
Cerebellar ataxia is a condition that can have a multitude of different causes and result in a wide variety of symptoms. Ashizara and Xia (2016) defined ataxia as “impaired coordination of voluntary muscle movement” - explaining that it is primarily the result of cerebellar damage. As a result of the cerebellum’s divisions and functional segregation, lesions in different areas can have different physical manifestations [1]. Common symptoms of cerebellar ataxia include delays in movement initiation, dysmetria, dyskinesia, dysdiadochokinesia, tremor, and disturbances in motor learning[2].
The following case study describes Sam Brown, a 30-year-old man who suffered cerebellar damage following a motor vehicle accident. In this case, damage was done primarily to the midline cerebellar structures. This region is needed for balance, posture, and gait, though cerebellar injuries are seldom isolated to only one region, and Sam also experienced some motor coordination deficits more typical of lateral cerebellar lesions[2]. A case study by Chester & Reznick (1987) discusses cerebellar ataxia symptoms following severe head trauma. In their research they note that the patient had both midline and lateral cerebellar symptoms. They also discuss an ambiguity behind the anatomical cause of the patient’s cerebellar ataxia – suggesting that it could be the result of diffuse axonal injury following his traumatic brain injury, and that it may have affected multiple brain regions, particularly the superior cerebellar peduncle[3].
The goal of this case study is to paint a picture of a patient suffering from cerebellar ataxia. Ataxia is widely regarded as a physical finding and not a disease[1] and research and case studies of patients suffering from cerebellar ataxia are not abundant. For this reason, it is important and interesting to explore a patient case for the specific condition.
Client Characteristics[edit | edit source]
The patient is Sam Brown, a 30-year-old male retail manager, working at Staples in Kingston, Ontario. At work he has a variety of tasks including manual labour, customer relations and paperwork. Sam lives with his wife and 6-year-old son in a 3rd floor apartment (20 stairs, has an elevator). Prior to his accident Sam was able to do all activities of daily living and ambulate completely independently. Sam’s hobbies include playing in a hockey league on Saturdays and hiking with his family. Overall, Sam is healthy and active, with no co-morbidities. He is a non-smoker and social drinker (1-2 drinks/week).
On his drive to work 18 days prior, he suffered a motor vehicle accident. In the crash he suffered from a severe concussion, whiplash and a fractured left radius. He was taken to hospital via ambulance and stayed for five days to be monitored and begin his rehabilitation process. While in hospital, Sam was assessed by Dr. Nancy, a neurologist who noticed Sam’s poor balance and postural control. Based on these observations, Dr. Nancy ordered an MRI scan to be completed which revealed a midline/left cerebellar hemisphere lesion as well as general cerebellar atrophy (see Figure 1)[4]. Though Dr. Nancy suspected cerebellar involvement based on Sam's symptoms, she needed to order labs (eg. thyroid function, serum B12) and run tests (initial SARA assessment - see Objective Assessment section for the physiotherapist completed SARA) to confirm her diagnosis and rule out other potential causes of Sam's symptoms[4]. This is an essential portion of Sam's early care because an accurate diagnosis is crucial to development of an effective treatment plan. Ultimately, Dr. Nancy diagnosed Sam with Truncal Cerebellar Ataxia and referred him to physiotherapy to help with his motor control symptoms.
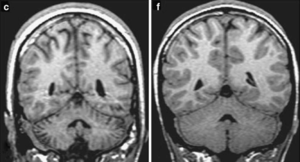
After five days in hospital, Sam was discharged and referred to outpatient physiotherapy. He is now arriving at physiotherapy day 18 post-accident (day 13 post discharge) to be assessed and have a treatment plan developed.
Examination Findings[edit | edit source]
Subjective Assessment
Patient chief Concerns:
- Patient reports having some balance issues post accident; such as feeling unstable when standing unsupported, feeling unsteady and swaying while seated (but able to stay upright in sitting).
- Patient has noticed he is walking much slower than usual and he is finding it very frustrating.
- Patient reported not having any falls but has had some close calls when getting out of bed.
- Patient is having trouble participating in typical family activities that he used to do prior to injury such as playing with his son and going on family hikes.
History of present Illness: Patient was admitted to the hospital presenting with concussion and whiplash injury due to an MVA. Upon examination by the neurologist and neuroimaging, patient was diagnosed with Truncal Cerebellar Ataxia and referred to physiotherapy. He is day 18 post-accident (day 13 post-hospital-discharge).
Past Medical History: Sam had a minor concussion 5 years ago from playing hockey. Other than that he has no history of any medical conditions. Patients reports no family history of ataxia or any cognitive conditions.
Current Functional History: Patient is more dependent on his wife for daily tasks such as cooking and cleaning. He is able to shower and dress independently but has some trouble with fine motor tasks such as buttoning up his shirt or zipping up his pants (these tasks are slow and take a while for Sam to complete). Sam is currently not working at his job due to the impacts of his condition. Currently he is using a quad cane at home and he reports that he is uncomfortable and unstable moving around without his cane.
Objective Assessment
Observation
- Posture: No visible deformities in standing and seated posture, some titubation (head and shoulders, anterior-to-posterior) visible when patient is seated.
- Gait Analysis: Patient has a wide base of support and presents with reduced gait speed and short stride length. Also, the patient has increased upper body/trunk movement during gait.
- Eye movement Exam:
- Saccadic eye movement test - patient presents with slow eye movements and with some compensatory head turning movement.
- Smooth pursuit test - the patient struggled to follow the examiners finger.
- Horizontal and vertical vestibulo-ocular reflex (VOR) tests - the patient struggled to keep his eyes on the examiner's finger.
- For all visual tests, the patient did not present with any headaches, dizziness, nausea or fogging of vision
Neurological Exam:
- Myotomes: Normal
- Dermatomes: Normal
- Deep Tendon Reflexes: Bicep, tricep, patella tendon and achilles tendons were assessed and all presented with normal reflexes
- Upper and Lower Motor neuron testing: Babinski and Clonus were both negative
Sensation testing
- Superficial: Sharp/dull mechanoreceptor test was performed and results were negative.
- Deep: Proprioception tests were done in the SARA outcome measure
- Cortical: 2 point discrimination was performed on patient's right and left forearm and palm, sensation was normal.
Range of motion and Manual Muscle Testing
| Joint Movement | ROM | MMT Grade |
|---|---|---|
| Shoulder Flexion | WNL B/L | 4 B/L |
| Shoulder Extension | WNL B/L | 4 B/L |
| Shoulder Abduction | WNL B/L | 4- B/L |
| Elbow Flexion | WNL B/L | 5 B/L |
| Elbow Extension | WNL B/L | 4+ B/L |
| Wrist ROM | Not tested due to radial fracture | Not tested due to radial fracture |
| Hip flexion | WNL B/L | R:4+ L:4- |
| Hip extension | WNL B/L | R:4+ L:4- |
| Hip abduction | WNL B/L | R:4 L:4 |
| Hip Adduction | WNL B/L | R:4+ L:4- |
| Knee Flexion | WNL B/L | R:4+ L:3+ |
| Knee Extension | WNL B/L | R:4 L:3+ |
| Ankle Dorsiflexion | WNL B/L | R:4+ L:4- |
| Ankle Plantar flexion | WNL B/L | R:4 L:3+ |
WNL = within normal limits
Outcome measures
- Scale for the Assessment and Rating of Ataxia (SARA)
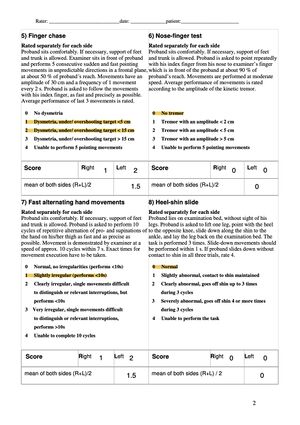
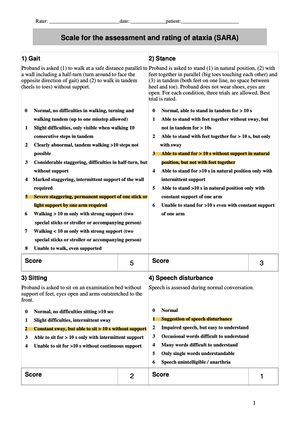
- SARA was completed on May 10th and Patient scored 14/40 (see Figure 2 and 2.1)
- During the test patient mainly presented with truncal symptoms such difficulties with gait(5/8), stance (3/6) and posture (2/4)
- Patient also had some issues with the finger chase (task 5) specifically on the left side
- Berg Balance Scale (BBS)
- Patient achieved a score of 18/56 which puts him at high risk for falls.
- Patient struggled with standing unsupported with feet together (0/4), standing with eyes closed (0/4), Tandem standing (0/4) and standing on one foot (0/4)
- Time Up and Go (TUG) test
- Patient performed the TUG with his cane and achieved a time of 18.7 sec, which is associated with an increase risk of fall.
- 36- Item Short From Survey (SF-36)
- Patient scored scored 12/36
- Patient reported increased limitations of daily activities and increased physical health problems post accident. He also reported having some emotional health problems since since he has lost some independence and cannot do his regular activities. He feels like he is accomplishing less than he would like to.
Clinical Impression[edit | edit source]
Physiotherapy Diagnosis
Mr. Brown was referred to physical therapy post-MVA with a diagnosis of Truncal Cerebellar Ataxia. He is presenting with impaired balance, gait and posture as well as some motor coordination symptoms on his left side, affecting his ability to ambulate and complete activities of daily living independently. The patient is also worried about falls and reports having some close calls at home. Patient reports relying on his wife more for activities around the house and he is currently unable to return to work. Sam is a good candidate for physical therapy. Sam's major goals are to improve his balance, coordination, lower limb strength and gait to allow for safe independent ambulation, facilitating his return to work and participation in regular activities with his family.
Problem List
The problem list was completed based on the International Classification of Functioning, Disability and Health[6]
| Body Structure & Function | Activity | Participation |
|---|---|---|
| Left leg weakness | Inability to complete ADLs independently | Currently unable to return to work |
| Ataxia | Reduced quality of life (SF-36 score of 12/36) | Unable to play sports and participate in regular family activities such as playing with his son and going on family hikes |
| Impaired balance (particularly in standing with reduced base of support & eyes closed) | ||
| Reduced postural control (titubation and postural sway) | ||
| Slow gait speed and reduced stride length | ||
| Dysdiadochokinesia | ||
| Dysmetria | ||
| Impaired visual reflexes and rapid eye movement |
Intervention[edit | edit source]
Short Term Goals
- Patient will improve his BBS score from 18/56 to 30/56 in 3 weeks by completing the balance exercises in the clinic with supervision and home exercise program.
- Patient will improve left leg strength to 4/5 in all joint movements in 3 weeks by completing strength exercises and walking.
Long Term Goals
- Patient will be able to ambulate safely and independently indoors in 2 months.
- Patient will be able to safely walk to the park which is 150m away from his apartment to play with his son in 6 weeks using a single point cane.
- Patient will be able to return to work with modified duties (ie. no lifting, shorter hours) in 2 months.
- Patient will improve his BBS score to 42/56 in 2 months.
Supervised Exercise Program
The goal of the gait training is to transition Sam from unbalanced ambulation with a quad cane to independent and safe ambulation. The physiotherapist will review the step-through gait pattern and general mobility aid education. As Sam’s balance improves when walking, the physiotherapist will transition to a single point cane and progress to walking without a mobility aid. Treadmill walking is incorporated to practice walking, and maintaining balance as he becomes fatigued[7]. The balance component's purpose is to improve stability in static and dynamic environments, and decrease his fear of falling[7]. Gaze stabilization exercises were implemented to help improve balance and stability[8]. Frenkel Exercises are designed to improve coordination for patients with ataxia[9]. These exercises require concentration/attention, precision and repetition. Throughout the 8 weeks of physiotherapy, education on cerebellar ataxia is a priority as it is a new diagnosis for Sam.
| Exercise | Parameters | Safety/Setup |
|---|---|---|
Balance
|
Reach with each hand forward, to the side, and across body just before it feels too unstable
10 reps each direction x 3 sets |
If wife is available she can spot him, or have another chair in front that he can grab onto |
| Walking | 10 min walking | Use single point cane until physiotherapist determines safe |
Trunk/Lower Extremity Strengthening
|
10 reps x 2 sets of each exercise | |
| Frenkel Exercises | Refer to in clinic exercise program | Only complete on days not in the clinic |
Lower Extremity
- Heel of one limb to opposite knee, sliding down crest of tibia to ankle in supine
- Sitting hip abduction and adduction both unilaterally and bilaterally
- Walk along a winding strip
Upper Extremity (in standing once mastered in sitting)
- Flex/ext one elbow at a time (shoulder flexed to 90 degrees)
- Flex/ext opposite elbows at the same time
- Reach and touch specific targets on the wall at arms reach
(5min upper, 5 min lower extremity)
- Walking in clinic
- Walking with head turning
- Walking with cognitive task
- Visual fixation with stationary and moving (slow and fast speed
- Active eye and head movement between two targets (slow and fast)
- Eyes open fixated on a moving target with head movement
Quiet standing on foam
- Progress to weight shifting
External perturbations
- In anterior posterior and lateral directions
Internal perturbations
- Reaching to move different coloured cones in all planes around the body
External perturbations 5 reps in each direction
Internal perturbations 10 reps of moving different directions
Examples of a variety of Frenkel Exercises
Outcome[edit | edit source]
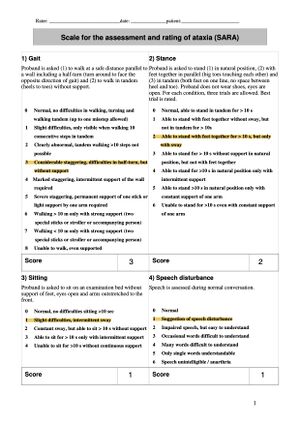
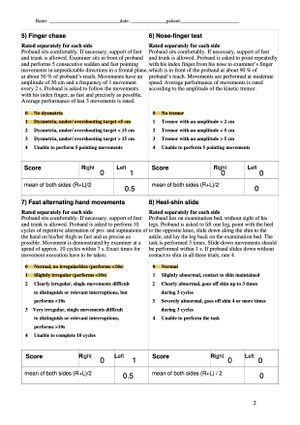
Sam has made great improvements over the last 8 weeks in physiotherapy, and has been able to achieve most of his goals. Sam improved his SARA score by 6 points, with a recorded score of 8/14 (see Figure 3 and 3.1). As the primary outcome measure for cerebellar ataxia this is a positive result. Sam made significant improvements in the gait and stance sections of the measure which were previously his biggest impairments. His gait now has increased stability, speed, cadence and step length. Sam's TUG score improved from 18.7s to 10.1s using a single point cane. Sam’s balance has also improved significantly as his BBS score increased by 23 points and scored 41/56 at follow up. His improved confidence and balance has allowed him to increase his participation and confidence in IADL’s, chores, and playing with his son without the fear of falling. Left lower extremity strength has improved, and now has 4+ strength bilaterally in hip, knee and ankle manual muscle tests. Sam can ambulate with confidence in the community with a single point cane, and without a gait aid in his apartment. It is noted Sam’s attitude has drastically changed over the last two months. Seeing increased independence, progress, and ability to play with his son while in physiotherapy has given him more optimism for the future. He reports not feeling like a burden at home. This is reflected in an increased SF-36 score of 24. Sam is ready to begin the process of returning to work on modified duties with the consultation of an occupational therapist. Sam and the physiotherapy team both agree Sam is ready to be discharged based on his progress, but would benefit with monthly appointments to progress his home exercise program.
Mr. Reid is the occupational therapist who will be working with Sam to return him to work. Mr. Reid assessed Sam two weeks ago and got into contact with his employer. It was determined Sam was able to continue most of his manager duties, but will not be able to do lifting above 10lbs as it is a safety concern. Mr. Reid has assessed Sam’s workplace and helped make modifications to the work environment. Sam wants to go back to work but has concerns about managing his new diagnosis, rehab, family and work. Mr. Reid and Sam will work together to develop a stress reduction plan and implement prevention strategies and various tools[13].
Discussion[edit | edit source]
Sam Brown, a healthy 30 year old male, was diagnosed with cerebellar ataxia after being involved in a motor vehicle accident. Following the accident Sam was taken to the hospital in stable condition where he underwent an assessment by a neurologist. Symptoms of cerebellar ataxia were identified and MRI imaging was ordered, confirming a midline/left cerebellar hemisphere lesion. Following the accident Sam spent five days in the hospital during which he was monitored for changes to his condition, received treatment for his other injuries and began rehabilitation. By the fifth day Sam’s healthcare team felt confident that his condition was stable and he could safely return home with his wife and son. Prior to discharge Sam worked with an occupational therapist to prepare him for his transition back home and he was referred to outpatient physiotherapy to continue his rehabilitation.
Two weeks following the accident Sam had his first appointment with the outpatient physiotherapy team. During the assessment, the SARA and SF-36 were administered, both of which have been found to be valid and reliable tools for use with ataxic patients[14][15]. The SARA is particularly helpful in quantifying the degree of impairment from cerebellar ataxia, guiding the development of a treatment plan that accurately reflects the patient's current level of impairment[7]. In the assessment, Sam presented with impaired balance, gait and posture, as well as some motor coordination symptoms of his left side. These impairments resulted in Sam having difficulty ambulating, an inability to complete ADL independently, and an overall decreased quality of life. Together with Sam, the physiotherapy team worked to develop treatment goals, all of which had a focus of returning to functional independence, increasing confidence, and allowing Sam to return to full engagement in social and work activities.
Treatment for cerebellar ataxia is focused on preventing further decline, stabilizing current symptoms, and improving functional ability[16]. Due to the wide range of impacts cerebellar ataxia can have, treatment is best delivered from a multidisciplinary team, which could include, but is not limited to, a neurologist, speech language pathologist, occupational therapist, and/or physiotherapist[17]. As treatment should be focused on maximizing safety and achieving patient goals[18], Sam’s physical therapy incorporated activities that support achievement of independent functioning such as balance training, trunk strengthening and gait training[7][18][11]. Frenkel exercises were also incorporated as they have been found to be beneficial for improving balance and gait in patients by focusing on coordination and utilizing visual feedback[19]. In addition to exercises performed in the clinic, Sam was provided a home exercise plan (HEP) to be completed independently outside of his physiotherapy appointments. HEPs, specifically balance training exercises, have been found to be beneficial in patients experiencing ataxia from cerebellar injuries[10]. In designing HEP for patients with cerebellar ataxia, the degree of challenge to balance is a important factor to consider as it, over duration or exercise frequency, has been found to be the most important factor for positive outcomes[10]. This finding highlights the importance of individualizing and continuously updating Sam’s HEP to reflect his progress.
The progress and recovery of cerebellar ataxia resulting from a traumatic brain injury (TBI) can be variable and have unique impairments that may affect the course of treatment[20]. It has been found that patients with TBI resulting in cerebellar ataxia achieve the greatest improvement six months post-injury, however improvements can continue to be achieved for years after[20]. In the case of Sam, following 8 weeks of physiotherapy treatment, he improved in all measures and had achieved a number of his rehabilitation goals. These progressions allowed him to complete an increased number of independent functional activities as well as participate in activities with his son. Although Sam still requires the use of a single point cane for ambulation in the community, he was able to progress to safe, independent walking within his home. Findings from Katz et al.[21] indicate that the achievement of independent ambulation is more favourable in patients who are younger, have lower initial TBI injury severity, and lower initial gait impairment. Based on these findings and Sam’s characteristics, with continued rehabilitation it is likely that he will be able to achieve recovery of independent ambulation within 5 months[21]. With consideration of Sam's current progress and consultation with him, the physiotherapy team assessed that he was fit for discharge, however would benefit from continued completion of his HEP. It was also agreed that Sam would have monthly appointments to update his HEP, ensuring that it continued to provide an adequate level of challenge based on his improvement.
Cerebellar ataxia resulting from a traumatic event, such as a motor vehicle accident, can be quite variable in its presentation[20] and impact many aspects of a patient's health[17]. To achieve an optimal prognosis and outcome it is therefore vital that a multidisciplinary team be utilized in order to address all areas of concern from physical to mental health[17]. For Sam’s care, the role of an occupational therapist, neurologist and physiotherapist were highlighted, however there would be many other healthcare professionals involved in his care such as a social worker or speech language pathologist. Overall the prognosis for traumatic cerebellar ataxia is very dependent on patient variables as well as the severity and location of the lesion[1]. Due to the large impact that cerebellar ataxia has on physical functioning, physiotherapy can contribute largely to more positive outcomes by both teaching compensatory strategies and restoring previous abilities[22]. Sam's personal characteristics, as well as his initial injury severity indicate that with continued engagement in rehabilitation he can expect continued improvement, facilitating his return to previous activities and level of functioning.
Self-Study Questions[edit | edit source]
Question 1 - Which of the following outcomes measures would not be appropriate for use with patients with acute cerebellar ataxia?
- Community Balance and Mobility Scale (CBMS)
- Scale for the Assessment and Rating of Ataxia (SARA)
- Function in Sitting (FIS)
- Manual Muscle Testing (MMT)
Question 2 - Which of the following are not common presentations of truncal ataxia?
- Dysmetria
- Titubation
- Reduced gait speed
- Impaired balance
Question 3 - In physical rehabilitation of cerebellar ataxia, which of the following is not typically a major focus?
- Gait retraining
- Postural control
- Motor coordination training
- Power and strength training
Answers - 1) 1; 2) 1; 3) 4.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Ashizawa T, Xia G. Ataxia. Continuum: Lifelong Learning in Neurology. 2016;22(4 Movement Disorders):1208–26. doi:10.1212/CON.0000000000000362
- ↑ 2.0 2.1 Diener HC, Dichgans J. Pathophysiology of cerebellar ataxia. Movement Disorders: Official Journal of the Movement Disorder Society. 1992;7(2):95-109. doi:10.1002/mds.870070202
- ↑ Susan Chester C, Reznick BR. Ataxia after severe head injury: The pathological substrate. Annals of Neurology. 1987;22(1):77–9. doi:10.1002/ana.410220117
- ↑ 4.0 4.1 de Silva RN, Vallortigara J, Greenfield J, Hunt B, Giunti P, Hadjivassiliou M. Diagnosis and management of progressive ataxia in adults. Practical Neurology. 2019;19(3):196–207. doi:10.1136/practneurol-2018-002096
- ↑ Potts MB, Adwanikar H, Noble-Haeusslein LJ. Models of traumatic cerebellar injury. Cerebellum. 2009;8(3):211–21. doi:10.1007/s12311-009-0114-8
- ↑ Stucki G, Cieza A, Ewert T, Kostanjsek N, Chatterji S, ÜstÜn TB. Application of the International Classification of Functioning, Disability and Health (ICF) in clinical practice. Disability and Rehabilitation. 2002;24(5):281–2. doi:10.1080/09638280110105222
- ↑ 7.0 7.1 7.2 7.3 Marquer A, Barbieri G, Pérennou D. The assessment and treatment of postural disorders in cerebellar ataxia: A systematic review. Annals of Physical and Rehabilitation Medicine. 2014;57(2):67–78. doi:10.1016/j.rehab.2014.01.002
- ↑ Gill-Body KM, Popat RA, Parker SW, Krebs DE. Rehabilitation of balance in two patients with cerebellar dysfunction. Physical Therapy. 1997;77(5):534–52. doi:10.1093/ptj/77.5.534
- ↑ Armutlu K, Karabudak R, Nurlu G. Physiotherapy approaches in the treatment of ataxic multiple sclerosis: A Pilot Study. Neurorehabilitation and Neural Repair. 2001;15(3):203–11. doi:10.1177/154596830101500308
- ↑ 10.0 10.1 10.2 Keller JL, Bastian AJ. A home balance exercise program improves walking in people with cerebellar ataxia. Neurorehabilitation and Neural Repair. 2014;28(8):770–8. doi:10.1177/1545968314522350
- ↑ 11.0 11.1 Freund JE, Stetts DM. Use of trunk stabilization and locomotor training in an adult with cerebellar ataxia: A single system design. Physiotherapy Theory and Practice. 2010;26(7):447–58. doi:10.3109/09593980903532234
- ↑ Physiopedia Mentor. Frenkle Exercises for Ataxia Patients | Physiotherapy | physiomentor [video file]. October 4, 2020 [May 13, 2021]. Available from: https://www.youtube.com/watch?v=BN2mfZed9xsreference
- ↑ Phillips J, Drummond A, Radford K, Tyerman A. Return to work after traumatic brain injury: recording, measuring and describing occupational therapy intervention. The British Journal of Occupational Therapy. 2010;73(9):422–30. doi:10.4276/030802210X12839367526138
- ↑ Schmitz-Hubsch T, Montcel ST du, Baliko L, Berciano J, Boesch S, Depondt C, et al. Scale for the assessment and rating of ataxia: development of a new clinical scale. Neurology. 2006;66(11):1717–20. doi:10.1212/01.wnl.0000219042.60538.92
- ↑ Sanchez-Lopez CR, Perestelo-Perez L, Escobar A, Lopez-Bastida J, Serrano-Aguilar P. Health-related quality of life in patients with spinocerebellar ataxia. Neurología (Barcelona, Spain). 2017;32(3):143–51. doi:10.1016/j.nrl.2015.09.002
- ↑ Pilotto F, Saxena S. Epidemiology of inherited cerebellar ataxias and challenges in clinical research. Clinical and Translational Neuroscience. 2018;2(2):2514183. doi:10.1177/2514183X18785258
- ↑ 17.0 17.1 17.2 Fonteyn EM, Keus SH, Verstappen CC, Schols L, Groot IJM de, Warrenburg BPC van de. The effectiveness of allied health care in patients with ataxia: a systematic review. Journal of Neurology. 2014;261(2):251–8. doi:10.1007/s00415-013-6910-6
- ↑ 18.0 18.1 Sartor-Glittenberg C, Brickner L. A multidimensional physical therapy program for individuals with cerebellar ataxia secondary to traumatic brain injury: a case series. Physiotherapy Theory and Practice. 2014;30(2):138–48. doi:10.3109/09593985.2013.819952
- ↑ Afrasiabifar A, Karami F, Najafi Doulatabad S. Comparing the effect of Cawthorne–Cooksey and Frenkel exercises on balance in patients with multiple sclerosis: a randomized controlled trial. Clinical Rehabilitation. 2018;32(1):57–65. doi:10.1177/0269215517714592
- ↑ 20.0 20.1 20.2 Freund JE, Stetts DM. Continued recovery in an adult with cerebellar ataxia. Physiotherapy Theory and Practice. 2013;29(2):150–8. doi:10.3109/09593985.2012.699605
- ↑ 21.0 21.1 Katz DI, White DK, Alexander MP, Klein RB. Recovery of ambulation after traumatic brain injury. Archives of Physical Medicine and Rehabilitation. 2004;85(6):865–9. doi:10.1016/j.apmr.2003.11.020
- ↑ Peri E, Panzeri D, Beretta E, Reni G, Strazzer S, Biffi E. Motor improvement in adolescents affected by ataxia secondary to acquired brain injury: A pilot study. BioMed Research International. 2019;2019:8967138–8. doi:10.1155/2019/8967138










