Benign Paroxysmal Positional Vertigo: A Case Study
Abstract[edit | edit source]
This is a fictional story depicting a patient diagnosed with idiopathic benign paroxysmal positional vertigo (BPPV). The purpose of this fictional case study is to investigate the physiotherapy-related approaches for assessing, diagnosing and treating this condition. The patient decided to seek out physiotherapy treatment to reduce his symptoms. He currently is unable to perform activities he usually enjoys such as driving or walking his dog. He is also stressed out about his work performance.
The Epley’s maneuver treatment technique was used to target the semicircular canals in order to minimize patient symptoms. Patient education of risk factors for recurrence as well as vestibular exercises were employed to reduce the risk of recurrence. A variety of outcome measures (Dynamic Gait Index, Dizziness Handicap Inventory, Vertigo Handicap Questionnaire, Activities-specific Balance Confidence Scale) were used to monitor progression of treatment/symptoms. The patient surpassed the minimally detectable changes for each of the outcome measures.
After completing the physiotherapist's treatment plan, the patient stated that they only had mild dizziness during specific tasks. With adequate education on how to manage symptoms, the patient has been discharged.
Introduction[edit | edit source]
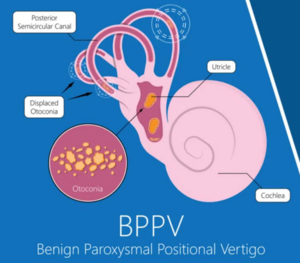
Benign Paroxysmal Positional Vertigo (BPPV) is a common disorder of the inner ear associated with the sensation of vertigo or dizziness. BPPV is the most common type of related vertigo condition and has an incidence of 107 cases out of 100,000 people per year[1]. It also has a 2.4% lifetime prevalence rate which increases with age [2]. The cause of this condition is usually insidious, but can also be brought on by a traumatic blow to the head. In this case study, the patient had a history of chronic headaches which is what may have caused his BPPV. Within the utricle of the inner ear, there are calcium-carbonate crystals (known as otoconia). These crystals may displace from their original location into the semicircular canals of the inner ear. Once the crystals are dislodged, the body’s ability to sense positional changes of the head, along with rotation and linear acceleration will be affected. Thus, creating symptoms of spinning or dizziness. This condition will cause a loss of balance, creating difficulties when attempting activities of daily living (ADLs).
BPPV can affect the posterior, lateral or anterior semicircular canals of the inner ear, but is most commonly found to affect the posterior canal[3]. Posterior canal BPPV typically presents with dizziness or vertigo with changes in head position, nystagmus, and balance deficits, with no cochlear symptoms or other neurological symptoms[4].
Physiotherapists may assist patients with this condition through education, manual therapy, and exercise prescription. By minimizing symptoms, the patient will have much more independence and an increased quality of life.
In the research, Burrows and Price (2017) highlight their experience with a 33-year-old male professional soccer player who had suffered from BPPV. They discuss the occupational risk of playing soccer with this condition due to the repetitive heading contact of the ball. As previously mentioned, the cause of this condition is most often insidious. Even if a patient has BPPV due to a non-traumatic cause, therapists must educate their patients on the risk of exacerbating their condition, even if their symptoms are resolved.[5]
The purpose of this fictional case study is to examine the role of physiotherapists in assessing, diagnosing, and treating posterior canal BPPV. Patient-centered goals will be identified to manage a typical problem list for this condition. The video below provides a brief description of BPPV.[6]
Client Characteristics[edit | edit source]
The patient is a 55 year old male who lives a relatively sedentary lifestyle and works as an accountant. He has high blood pressure which has been controlled by 40mg of Diovan daily. The patient also has high cholesterol in which he takes 5mg of Crestor daily to help control. The patient enjoys gardening, driving with his wife and walking his dog. He complains of nausea, dizziness and the feeling of the room spinning. He is planning on retiring and is nervous about not being able to do what he wants and enjoy his retirement because of his symptoms. He first noticed symptoms 2 weeks ago while turning his head quickly while driving. Following the onset, medications did not help symptoms and therefore he has since been getting treatment for BPPV. Sleeping has become increasingly difficult as any time he lays down he begins to feel dizzy.
Examination Findings[edit | edit source]
Subjective[edit | edit source]
History of Present Illness
His symptoms first started on April 22nd, 2022, when he was shoulder checking to switch lanes while driving. He went to see his Family Physician on April 24th, 2022 who referred him to physiotherapy. Currently, his chief complaints are dizziness, a feeling of his surroundings "spinning", and occasional nausea.
Past Medical History
This patient was diagnosed with hypertension and hypercholesterolemia in December 2015. He has also been experiencing headaches for the past three months (about one headache per week, lasting longer than 30 minutes).
Medications
Currently, the patient takes 40mg of Diovan daily to control his high blood pressure and 5mg of Crestor daily to manage his high cholesterol[8]. He also takes 1 Gravol liquid gel capsule (50mg) every 4 hours when he begins feeling symptomatic.
Functional History
The patient has mentioned that he is unable to perform activities that he usually enjoys such as gardening, driving, and walking his dog. Although he can perform basic activities of daily living independently such as getting dressed, eating, walking short distances, using the washroom, and bathing, he has more difficulty with instrumental activities of daily living such as shopping, housework, and cooking. Aggravating activities include rolling out of bed and bending over. Pain is alleviated when lying on his back with his head elevated using multiple pillows.
Social History
This patient works full-time as an accountant. He lives in a bungalow in a small neighbourhood with his wife and golden retriever. All the rooms he needs (i.e. bedroom, kitchen, bathroom) are on the main floor, with the top floor mainly used for storage and guest bedrooms. His two adult children (aged 30 and 27) live within a 15 minute drive and visit often. In his free time, he enjoys gardening, walking his dog, and going on drives into the city with his wife. He has never been a smoker and does not use any recreational drugs, but will have the occasional beer or glass of wine on the weekend with his wife and kids. He reports feeling stressed about getting tasks done at work due to having to take frequent breaks.
Family History
When asked, the patient could not recall any family members having BPPV. However, he did report that his father also has hypertension and suffered a heart attack at the age of 65. His mother is also currently exhibiting signs of early dementia, although this has not been officially diagnosed yet. No other family history can be recalled by the patient.
Objective[edit | edit source]
Positive Findings
- Vestibulocochlear nerve exam - right side
- Dix-Hallpike test - right side
Negative Findings
- All other cranial nerve examinations
- Dix-Hallpike test - left side
- Supine roll test (for Horizontal semicircular canal) - bilateral
- Head Pitch Test
- Finger to nose test
Outcome Measures[edit | edit source]
The outcome measures chosen to assess this patient were the Dynamic Gait Index, Dizziness Handicap Inventory, Vertigo Handicap Questionnaire and Activities-specific Balance Confidence Scale. He obtained baseline scores of 18/24 on the Dynamic Gait Index, 37/100 on the Dizziness Handicap Inventory, 76% on the Vertigo Handicap Questionnaire and 44% on the Activities-specific Balance Confidence Scale.
Clinical Hypothesis[edit | edit source]
Physiotherapy Diagnosis[edit | edit source]
A 55 year old male patient presents with vertigo, nystagmus, dizziness and balance issues caused by different head positions onset 2 weeks ago. The present symptoms put the patient at a higher risk of falls and a decreased quality of life. Based on past level of functioning and timeline of onset the patient is expected to make a full recovery. Subjective and objective measures are consistent with right-sided posterior canal BPPV (canalithiasis) with unknown insidious cause.
Problem List[edit | edit source]
- Vertigo, nystagmus, dizziness and imbalance caused by sudden specific head position changes
- Unable to work caused by symptoms
- Unable to garden
- Unable to walk/play with dog
- Decreased productivity at work due to fear of onset of vertigo
- Unable to drive since onset of symptoms
Intervention[edit | edit source]
Goals:
Short-term Goals:
- The patient wants to go 48 hours without any provocation of symptoms by the second week of treatment (14 days post-treatment).
- The patient wants to improve his dynamic gait index score to 20 by the 10th-day post-treatment.
Long-term Goals:
- The patient wants to be able to drive to work without feeling dizzy checking his blind spots (30 min drive) in 6 weeks.
- The patient wants to be able to play fetch with his dog for 20 minutes without an onset of symptoms from picking up the ball in 8 weeks.
Following the assessment and informed consent for treatment, the Epley’s manoeuver[9] was performed 3 times on the right affected side to target the posterior semicircular canal which immediately reduced the patient’s BPPV symptoms[10]. The patient reported no symptoms within the 24 hours following this technique. The video below demonstrates how the manoeuver can be performed at home.
The Semont manoeuver is another effective approach for treating posterior canal BPPV, however it was not performed because Epley’s has better short-term effectiveness for treating this condition (although the two maneuver’s are equally as effective when it comes to long-term effectiveness for treating it)[12][13].
The patient was also educated on recurrence rates and risk factors before leaving the clinic. This included to keep their head vertical and to sleep in the semi-recumbent for the next 24 hours. In addition, they were also instructed to avoid provoking head positions such as sleeping on their right side, not flexing, extending, rotating, or side bending their head excessively in the next week[14]. If they were experiencing symptoms they were also instructed not to drive.
Upon the next treatment visit, vestibular rehabilitation was performed. Vestibular rehabilitation has been shown to be effective in both the short- and long-term for BPPV, and for older adults, leads to improvements in dynamic balance - a key area to improve in order for the patient to be able to play with his dog[15]. Furthermore, with technology becoming more omnipresent in society, it can play a key role in rehabilitation approaches. A device as simple as a smartphone, which is often carried and used daily, can easily be converted into a training device to assist with home balance training, providing real-time feedback on standing balance and posture [16]. This would enable the patient to receive real-time external feedback when performing vestibular rehabilitation exercises at home, and could improve the quality of training done outside of the physiotherapy clinic. Another piece of technology that could be leveraged for this patient is virtual reality (VR), as the patient does not experience vertigo and associated symptoms from looking at a screen, but rather from changing his head position. Research has shown that VR training can be as effective (or more effective) than traditional vestibular rehabilitation, while also being more enjoyable, less tiring, and less difficult to use[17][18]. These studies utilized patients with an average age of 50 years, indicating that it is not just beneficial for younger patients, and that it could be a rehabilitation method to explore for use with the patient.
In addition to the vestibular rehabilitation, the patient was taught Cawthrone-Cooksey exercises[19] with a focus of training the eyes to move independently of the head. This consisted of performing exercises by gradually building up from one exercise to the next. Having the patient rate the severity of symptoms during the exercise on a scale of 0-5 (where 0 = no symptoms and 5 = severe symptoms) to pace the progression of exercises. Exercises may include gaze training, balancing in day-to-day situations, improving coordination (catching and throwing a ball, walking on incline, stooping)[20].
[21] The patient was also taught Brandt-Daroff exercises[22] at the 1 week physiotherapy intervention mark to promote loosening of canals and to prevent the patient’s chance for BPPV recurrence[23]. They were instructed to perform 1-4 reps of 3 sets a day for 2 weeks. In addition, the patient was educated that if BPPV symptoms were to recur, this technique does show some effectiveness for self symptomatic relief[24].
Outcome[edit | edit source]
After six weeks of treatment, this patient experienced a great degree of improvement. First, his Dynamic Gait Index post-treatment score is now 22, compared to his baseline score of 18. This is considered a significant change as minimal detectable change is expected to be approximately 4 points[26]. This also means that this patient is no longer considered to be at fall risk as their score is now higher than 19/24[27].
Additionally, his Dizziness Handicap Inventory post-treatment score improved to 14, compared to his baseline score of 37 which surpasses the estimated minimal clinically important difference of 4 points and the minimal detectable change of 17 points[28]. This means that he is no longer considered to have a handicap associated with his dizziness[29].
Furthermore, his Activities-specific Balance Confidence Scale post-treatment score is now 86%, compared to his baseline score of 44%. This surpasses the estimated minimal detectable change of 15 points[30]. This also means that he is now considered to have a high level of functioning[31].
His Vertigo Handicap Questionnaire score has decreased from 76% down to 24%, indicating an improvement (less of a handicap), with key improvements with regards to the items on anxiety and fear surrounding his vertigo. Additionally, he no longer indicates that vertigo is causing him issues at work, and he is able to carry on with what he is doing when the vertigo becomes present[32][33].
In addition to outcome measures, the patient now only reports mild dizziness during specific tasks, but does not feel like the room is spinning around them and no longer feels nauseous. He is also now able to do all the tasks he was able to do prior to the onset of symptoms such as gardening and driving. He is very motivated and continues to work on his balance training at home.
Due to the patient's current functional status as well as their high motivation levels, it is highly likely that they are ready for discharge. In order to prepare them for discharge, a meeting with the patient along with any family members they want to include in this process (ex. spouse) to make a plan together. The patient will also be encouraged to continue their at-home balance management programme and will be provided with resources to educate him on his condition as well as positions and movements that might alleviate or aggravate symptoms. However, it must be explained to him that although his scores have improved tremendously since beginning treatment, there is always room for improvement. A follow-up appointment will therefore be made for three months from the discharge date with a goal of near-perfect scores on the Dynamic Gait Index, Dizziness Handicap Inventory, Vertigo Handicap Questionnaire, and Activities-specific Balance Confidence Scale.
At this time, referral to other health care providers is not deemed necessary as this patient is highly functional with minimal symptoms. However, the patient will be told that if symptoms become worse or if they experience any other symptoms, they should seek help from their Family Physician, a neurologist, or an otolaryngologist as soon as possible[34].
Multidisciplinary Team[edit | edit source]
While the physiotherapist will be the main health care professional responsible in this case, otolaryngologists may also be used if imaging or surgery is required. If the conservative approaches to treating BPPV do not work, the otolaryngologist may perform a semicircular canal occlusion. This procedure is typically only used when the posterior canal is affected because there is a risk of hearing loss with the other canals. During this minimally invasive procedure, the surgeon will open up the posterior semicircular canal and destroy the lumen. This will provide immediate relief to the BPPV symptoms while preserving the inner ear[34].
Vestibular suppressant medications such as dimenhydrinate may also be helpful to reduce residual symptoms such as lightheadedness once a Canalith repositioning procedure has been performed[32]. The patient’s family doctor should also monitor their medication or if any new or ongoing symptoms are representing[35].
Discussion[edit | edit source]
The patient's reason for physiotherapy visit and chief complaints included dizziness, feeling of the room spinning, and nausea. After a full examination, the patient showed signs of a posterior canal BPPV, which may be causing his chronic headaches. After 6 weeks of treatment, his outcome measures dramatically improved, indicating a return to a high level of function.
Techniques outlined in the management programme included the Epley manoeuver, Cawthrone-Cooksey exercises and Brandt-Daroff exercises, alongside vestibular rehabilitation, representing a number of appropriate treatment techniques for BPPV. Similar interventions outlined may also be implemented to treat dizzy spells caused by medication side effects or other vestibular conditions. Additionally, balance training is beneficial for the general population and can help reduce the risk of falls and improve stability.
References[edit | edit source]
- ↑ Froehling DA, Silverstein MD, Mohr DN, Beatty CW, Offord KP, Ballard DJ. Benign positional vertigo: incidence and prognosis in a population-based study in Olmsted County, Minnesota. Mayo Clin Proc. 1991 Jun; 66(6):596-601. doi: 10.1016/s0025-6196(12)60518-7.
- ↑ von Brevern M, Radtke A, Lezius F, Feldmann M, Ziese T, Lempert T, et al. Epidemiology of benign paroxysmal positional vertigo: a population based study. J Neurol Neurosurg Psychiatry . 2007; 78(7):710-5. doi: 10.1136/jnnp.2006.100420.
- ↑ Califano L, Salafia F, Mazzone S, Melillo MG, Califano M. Anterior canal BPPV and apogeotropic posterior canal BPPV: two rare forms of vertical canalolithiasis. Acta Otorhinolaryngol Ital. 2014; 34(3):189-97. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4035840/
- ↑ Imai T, Takeda N, Ikezono T, Shigeno K, Asai M, Watanabe Y, et al. Committee for Standards in Diagnosis of Japan Society for Equilibrium Research. Classification, diagnostic criteria and management of benign paroxysmal positional vertigo. Auris Nasus Larynx. 2017; 44(1):1-6. doi: 10.1016/j.anl.2016.03.013
- ↑ Burrows L, Price R. Benign paroxysmal positional vertigo (BPPV) diagnosis and treatment in an elite professional football (soccer) player. BMJ Case Reports. 2017; 1-4. doi:10.1136/bcr-2017-220000.
- ↑ MUSC Health. MUSC: Benign Paroxysmal Positional Vertigo (BPPV) [1]. 2016. Available from: https://www.youtube.com/watch?v=mXmlFPJyvZA (accessed 2022 May 11).
- ↑ MUSC: Benign Paroxysmal Positional Vertigo (BPPV). Available from: https://www.youtube.com/watch?v=mXmlFPJyvZA
- ↑ Cunha JP. Crestor [internet]. RxList [Updated 2021 Oct 13, cited 2022 May 6]. Available from: https://www.rxlist.com/crestor-drug.htm
- ↑ AquacarePT. How to perform the epley maneuver at home for BPPV [2] . 2016. Available from: https://www.youtube.com/watch?v=VtJB5Vx7Xqo&t=2s (accessed May 11 2022)
- ↑ Epley JM. The canalith repositioning procedure: for treatment of benign paroxysmal positional vertigo. Otolaryngol Head Neck Surg. 1992;107(3):399-404. doi: 10.1177/019459989210700310
- ↑ AquacarePT-How to perform the epley maneuver at home for BPPV. Available from: https://www.youtube.com/watch?v=VtJB5Vx7Xqo
- ↑ Lee JD, Shim DB, Park HJ, Song CI, Kim MB, Kim CH, et al. A multicenter randomized double-blind study: comparison of the Epley, Semont, and sham maneuvers for the treatment of posterior canal benign paroxysmal positional vertigo. Audiol Neurootol. 2014;19(5):336-41. doi: 10.1159/000365438
- ↑ Bhattacharyya N, Gubbels SP, Schwartz SR, Edlow JA, El-Kashlan H, Fife T, et al. Clinical Practice Guideline: Benign Paroxysmal Positional Vertigo (Update). Otolaryngol Head Neck Surg. 2017;156(3_suppl):S1-S47. doi: 10.1177/0194599816689667
- ↑ Otolaryngology Associates, P.C. Vertigo (BPPV) Post Treatment Instructions. 2013. Available from:http://www.otolaryngology-assoc.com/for_patients/vertigo_bppv_post_treatment_instructions.aspx (accessed May 6 2022).
- ↑ Dunlap P, Holmberg J, Whitney S. Vestibular rehabilitation: advances in peripheral and central vestibular disorders. Current Opinion in Neurology. 2019; 32 (1): 137-144. doi: 10.1097/WCO.0000000000000632
- ↑ Lee BC, Kim J, Chen S, Sienko KH. Cell phone based balance trainer. J Neuroeng Rehabil. 2012; 9:10. doi: 10.1186/1743-0003-9-10
- ↑ Micarelli A, Viziano A, Augimeri I, Micarelli D, Alessandrini M. Three-dimensional head-mounted gaming task procedure maximizes effects of vestibular rehabilitation in unilateral vestibular hypofunction: a randomized controlled pilot trial. Int J Rehabil Res. 2017; 40(4):325-332. doi: 10.1097/MRR.0000000000000244.
- ↑ Meldrum D, Herdman S, Vance R, Murray D, Malone K, Duffy D, et al. Effectiveness of conventional versus virtual reality-based balance exercises in vestibular rehabilitation for unilateral peripheral vestibular loss: results of a randomized controlled trial. Arch Phys Med Rehabil. 2015; 96(7):1319-1328.e1. doi: 10.1016/j.apmr.2015.02.032.
- ↑ BonitalocalogTV. Cooksey-Cawthorne Exercise || Vestibular Rehabilitation || Therapeutic Exercise || Physical Therapy [3] 2020 [cited 2022 May 11] Available from https://www.youtube.com/watch?v=VjGVIXgMCLo
- ↑ Brain & Spine Foundation. Vestibular rehabilitation exercises: Fact sheet. Available from: https://www.brainandspine.org.uk/our-publications/our-fact-sheets/vestibular-rehabilitation-exercises/# (accessed May 5 2022).
- ↑ Cooksey-Cawthorne Exercise || Vestibular Rehabilitation || Therapeutic Exercise || Physical Therapy. Availabale from :https://www.youtube.com/watch?v=VjGVIXgMCLo&t=10s
- ↑ Dallas Ear Institute / Hearing Center/ Brandt-Daroff Exercise [4]. 2020 [cited 2022 May 11]. Available from: https://www.youtube.com/watch?v=Lz9wHq3DcWA
- ↑ Radtke A, Neuhauser H, von Brevern M, Lempert T. A modified Epley's procedure for self-treatment of benign paroxysmal positional vertigo. Neurology [internet]. 1999 Oct 12 [cited 2022 May 6]; 53(6):1358-60. doi: 10.1212/wnl.53.6.1358
- ↑ Bhattacharyya N, Baugh RF, Orvidas L, Barrs D, Bronston LJ, Cass S, et al. Clinical practice guideline: benign paroxysmal positional vertigo. Otolaryngol Head Neck Surg. 2008; 139(5 Suppl 4):S47-81. doi: 10.1016/j.otohns.2008.08.022.
- ↑ Brandt-Daroff Exercise. Available from : https://www.youtube.com/watch?v=Lz9wHq3DcWA
- ↑ Marchetti GF, Lin CC, Alghadir A, Whitney SL. Responsiveness and minimal detectable change of the dynamic gait index and functional gait index in persons with balance and vestibular disorders. J Neurol Phys Ther. 2014; 38(2):119-24. doi: 10.1097/NPT.0000000000000015
- ↑ Advocate at home. Dynamic Gait Index [internet]. 2019. Available from: https://www.cptrehab.com/wp-content/uploads/sites/60/2016/09/Dynamic-Gait-Index.pdf (accessed May 6 2022)
- ↑ Noble GJ, Hwang E, Wu A, Cushing S, Lin VY. Vestibular function following unilateral cochlear implantation for profound sensorineural hearing loss. Head and Neck Surg. 2016; 45(1):1-6. DOI 10.1186/s40463-016-0150-6
- ↑ Physician Outreach. Scoring for Dizziness Handicap Inventory [internet]. 2012. Available from: https://www.audiologist.org/_resources/documents/physician-outreach/Dizziness-Handicap-Inventory-Scoring.pdf (accessed May 6 2022)
- ↑ Wang YC, Sindhu B, Lehman L, Li X, Yen SC, Kapellusch J. Rasch Analysis of the Activities-Specific Balance Confidence Scale in Older Adults Seeking Outpatient Rehabilitation Services. J Orthop Sports Phys Ther. 2018; 48(7):574-583. doi: 10.2519/jospt.2018.8023.
- ↑ Wildschut A, Rochette A, Filiatrault J. Activities-specific Balance Confidence Scale (ABC). Heart & Stroke Foundation; 2020. Available from: https://strokengine.ca/en/assessments/activities-specific-balance-confidence-scale-abc-scale/#:~:text=The%20ABC-S%20Scale%20has%20demonstrated%20high%20internal,consistency%20%28reliability%20index%200.86%29%20and%20good%20convergent%20validity (accessed May 6 2022)
- ↑ 32.0 32.1 Min-beom K, Hyun L, Jae B. Vestibular suppressants after canalith repositioning in benign paroxysmal positional vertigo. Larynscope. 2014; 124(10):2400-2403. Available from https://doi.org/10.1002/lary.24741
- ↑ Shirley Ryan bilitylab. Vertigo Handicap Questionnaire [internet]. AbilityLab. 2022. Available from: https://www.sralab.org/rehabilitation-measures/vertigo-handicap-questionnair (accessed May 11 2022).
- ↑ 34.0 34.1 MercyHealth. Benign Paroxysmal Positional Vertigo (BPPV) [internet]. 2019. Available from: https://www.mercy.com/health-care-services/ear-nose-throat-ent/conditions/benign-paroxysmal-positional-vertigo (accessed May 112022).
- ↑ Michigan Ear Institute. BPPV surgery. Michigan Ear Institute [internet]. 2020. Available from: https://michiganear.com/posts/bppv-surgery/ (accessed May 11 2022).