Carpal Tunnel Syndrome
Original Editor - Kristin Sartore
Top Contributors - Jaroslaw Pospiech, Kristin Sartore, Laura Ritchie, Admin, Sien Bossant, Lucinda hampton, Kim Jackson, Rachael Lowe, Anas Mohamed, Mathieu Vanderroost, Camille Dewaele, Kai A. Sigel, Sai Kripa, Stuart Wildman, Wanda van Niekerk, Erica Alexander, Chelsea Mclene and Blessed Denzel Vhudzijena
Introduction[edit | edit source]
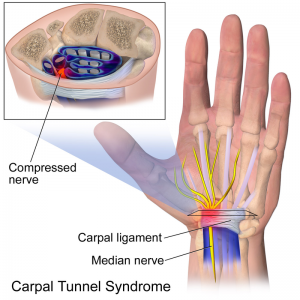
Carpal tunnel syndrome (CTS) is an entrapment neuropathy caused by compression of the median nerve as it travels through the wrist's carpal tunnel. Normal tissue pressure within the tunnel is approximately 3-7mm Hg. CTS can result in pressure with greater than 30mm Hg.
- It is the most common nerve entrapment neuropathy, accounting for 90% of all neuropathies.
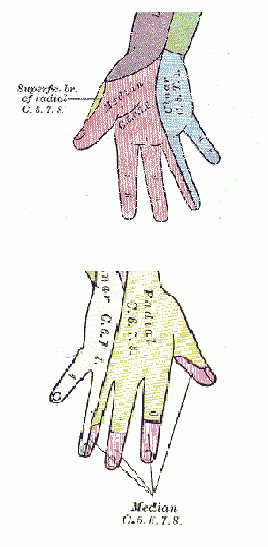
- Early symptoms of carpal tunnel syndrome include pain, numbness, and paresthesias. Sensory changes and paresthesia along with median nerve distribution in Hand.
- Symptoms typically present, with some variability, in the thumb, index finger, middle finger, and the radial half (thumb side) of the ring finger.
- Pain also can radiate up the affected arm. Radiate into upper extremity, shoulder and neck. With further progression, night pain, hand weakness, decreased fine motor coordination,decreased grip strength, clumsiness, reduced wrist mobility and thenar atrophy can occur. [1]
Patients can be diagnosed quickly and respond well to treatment but the best means of integrating clinical, functional, and anatomical information for selecting treatment choices have not yet been identified.[2][3]
Clinically Relevant Anatomy[edit | edit source]
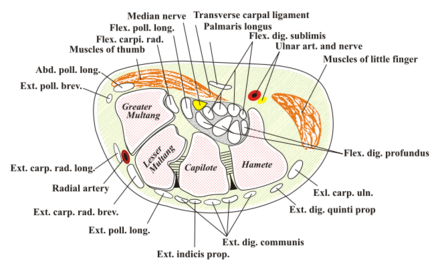
The carpal tunnel (CT) is formed by a non-extendable osteofibrous wall that forms a tunnel protecting the median nerve and flexor tendons.
The transverse carpal ligament (flexor retinaculum) makes up the superior boundary, and the carpal bones form the inferior border.
The carpal tunnel includes the median nerve and nine flexor tendons.
The flexor tendons include
- Four tendons from the flexor digitorum profundus
- Four tendons from the flexor digitorum superficialis
- One tendon from the flexor pollicis longus. [1]
Etiology[edit | edit source]
Carpal tunnel syndrome results from increased pressure in the carpal tunnel and subsequent compression of the median nerve. The most common causes of carpal tunnel syndrome include genetic predisposition, history of repetitive wrist movements such as repetitive use, typing, or machine work as well as obesity, diabetes, cumulative trauma disorders, tumor, hypothyroidism, wrist spine and fracture, autoimmune disorders such as rheumatoid arthritis, and pregnancy.[1]
Epidemiology[edit | edit source]
- The prevalence of carpal tunnel syndrome is estimated to be 2.7-5.8% of the general adult population, with a lifetime incidence of 10-15%, depending on occupational risk 4.
- Carpal tunnel syndrome usually occurs between ages 36 and 60 and is more common in women, with a female-to-male ratio of 2-5:1.[4]
Clinical Biomechanics of Carpal Tunnel Syndrome[edit | edit source]
Click here for information
Pathophysiology[edit | edit source]
There is a wide spectrum of causative pathologies, converging on two mechanisms of disease, both of which lead to entrapment:
- A decrease in the size of the carpal tunnel caused by such conditions as:
- Mechanical overuse (considered the most common association)
- osteoarthritis
- Trauma
- acromegaly
- Disease states leading to augmentation of carpal tunnel contents:
- Masses, For example, ganglion cysts, primary nerve sheath tumours
- Deposition of foreign material, e.g. amyloid
- Synovial hypertrophy in rheumatoid arthritis[4]
In general, the pathophysiology of CTS results from a combination of compression and traction mechanisms.
- The compressive element of the pathophysiology includes a detrimental cycle of increased pressure, obstruction of overall venous outflow, increasing local edema, and compromise to the median nerve's intraneural microcirculation. Nerve dysfunction becomes compromised, and the structural integrity of the nerve itself further propagates the dysfunctional environment-- the myelin sheath and axon develop lesions, and the surrounding connective tissues become inflamed and lose normal physiologic protective and supportive function.
- Repetitive traction and wrist motion exacerbates the negative environment, further injuring the nerve. In addition, any of the nine flexor tendons traveling through the carpal tunnel can become inflamed and compress the median nerve[1]
Idiopathic Carpal Tunnel Syndrome[edit | edit source]
- Idiopathic CTS occurs more frequently in females (65–80%), between the ages of 40 and 60 years; 50–60% of the cases are bilateral.[5]
- The bilateral characteristic increases in frequency with the duration of symptoms.[6]
- Idiopathic CTS is correlated with hypertrophy of the synovial membrane of the flexor tendons caused by degeneration of the connective tissue, with vascular sclerosis, edema and collagen fragmentation.[7]
- The histological changes were thought to be suggestive of dynamic factors as repetitive strain.
Clinical Presentation[edit | edit source]
CTS onset is generally gradual with tingling or numbness in the median nerve distribution of the affected hand. Fig.3. [9] [10] [11]
Patients may notice aggravation of symptoms with static gripping of objects such as a phone or steering wheel but also at night or early in the morning. [10] [11] Many patients will report an improvement of symptoms following shaking or flicking of their hand.
As the disorder progresses, the feeling of tingling or numbness may become constant and patients may complain of burning pain. [10]
The final symptoms are weakness and atrophy of muscles of the thenar eminence. These combined effects of sensory deprivation and weakness may result in a complaint of clumsiness and loss of grip and pinch strength or dropping things, [10]
Differential Diagnosis[edit | edit source]
The process of differential diagnosis should give consideration to all conditions which could potentially cause a dysfunction of the median nerve, or its contributories in brachial plexus, C 5 to 8 nerve roots and central nervous system.
Possible differential diagnoses of carpal tunnel syndrome include:
- other median nerve entrapment syndromes
- pronator teres syndrome
- anterior interosseous nerve syndrome
- an injury of nerve digitales in the palm.
- cervicobrachial syndrome.[4]
Diagnostic Procedures[edit | edit source]
Ultrasound and MRI are the two imaging modalities which best lend themselves to investigating entrapment syndromes. Next to directly visualizing direct causes and anatomical variants recognizing pathological muscle signal patterns on MRI can point to the affected nerve.[4]
Electromyography and nerve conduction studies are the basis for carpal tunnel syndrome diagnosis. Other clinical or special exams do not confirm carpal tunnel syndrome but do assist in ruling out other diagnoses. These findings can prompt electromyography and nerve conduction studies.[1]
X-ray is recommended to exclude other causes of wrist pain like arthritis or bony pathology. [3]
Outcome Measures[edit | edit source]
There are several questionnaires available to determine the outcome measures for CTS.
- Boston Carpal Tunnel Questionnaire (BCTQ)
- Disability of Hand and Shoulder (DASH) Questionnaire
- Brigham_and_Women's_Carpal_Tunnel_Questionnaire.
- Patient Evaluation Measures (PEM) The PEM is a self-, interview- or telephone-administered questionnaire to measure physical health. It consists of 3 components (patient’s opinion on delivery of care, hand health profile, overall assessment) and a total of 18 items scored on a 7-point scale. Low scores indicate positive outcomes.16 17 Hobby et al.20 found this instrument to be valid and reliable and to have good responsiveness. [12] [13]
Physical Examination[edit | edit source]
May include testing for sensory and motor deficits and evidence of thenar wasting. There are several special tests with varying degrees of sensitivities and specificities.
- The best of these include the carpal compression test. This is done by applying firm pressure directly over the carpal tunnel for 30 seconds. The test is positive when paresthesias, pain, or other symptoms are reproduced.
- The square sign test is an evaluation to determine the risk of developing carpal tunnel syndrome. The test is positive if the ratio of the thickness of the wrist divided by the width of the wrist is great than 0.7.
- Another test is a palpatory diagnosis. In this test, the health care provider examines soft tissue over the median nerve for mechanical restriction.
- The Phalen's test or ‘reverse prayer’ is performed by having the patient fully flex their wrists by placing dorsal surfaces of both hands for one minute. A positive test is when symptoms (numbness, tingling, pain) are reproduced.
- The reverse Phalen's, or ‘prayer test,’ is done by having the patient extend both of their wrists by placing palmar surfaces of both hands together for 1 minute (as if praying). Again a positive test is with reproduction of symptoms.
- Although a low sensitivity and specificity, the Hoffmann-Tinel sign is another test commonly performed. In this test the healthcare professional taps immediately over the carpal tunnel to stimulate the median nerve. Like the above tests, a positive test is when symptoms are reproduced.[1]
- The 'Scratch Collapse Test' (SCT) has emerged as a new provocative test to assist in the localisation of peripheral nerve compression.
Clinical prediction rules (CPR), specifically for the Carpal Tunnel Syndrome, are a reliable examination method.
Medical Management[edit | edit source]
If carpal tunnel syndrome is identified early conservative treatment is recommended.
- Initially, the patient should be instructed in modifying symptom provoking wrist movement, For example, proper hand ergonomics such as placing the keyboard at a proper height and minimizing flexion, extension, abduction, and adduction of the hand when typing. It should be recommended to decrease repetitive activities if possible.[1]
- Non-surgical treatment comprises oral steroids [14] [15], corticosteroid injections [15], NSAID [14][15], diuretics [14][16], vitamin B6 [14] and splinting/hand brace [14][15][16]. If conservative treatments are not successful, an oral or local glucocorticoid could be offered.
- The definitive treatment for persistent carpal tunnel syndrome is surgical intervention with carpal tunnel release after nerve conduction studies showing significant axonal degeneration. Carpal tunnel release typically is performed by an orthopedic surgeon or hand surgeon. This procedure can be performed either open or endoscopically. Carpal tunnel release is considered a minor surgery in which the transverse carpal ligament or flexor retinaculum is cut, opening more space in the carpal tunnel and decreasing pressure on the median nerve. It does not typically require overnight hospitalization.[1]
Physical Therapy Management[edit | edit source]
Patients with mild to moderate symptoms can be effectively treated in a primary care environment [17] [18]
Physical therapists should give advice on modifications of activities and the workplace (ergonomic modifications) [17][18], task modification, For example, taking sufficient rest and variation of movements.
Often simple obvious alterations to the working practice can be beneficial in controlling milder symptoms of CTS.[18]
Manual therapy techniques include mobilisation of
- Soft tissue
- Carpal bone
- Median nerve[19]
Other modalities include: ultrasound [14][15][19] and electromagnetic field therapy [14][15] and splinting.[20]
Research findings (varies)
- Physiotherapy modalities (TENS and ultrasound) have little useful effects on hand sensory discomfort.[21]
- The evidence of the effectiveness of the exercise and mobilization interventions is limited and very low in quality.[19].
- Evidence about post-operative rehabilitation is also limited. None of them seems to have a prevailing benefit[22].
Clinical Bottom Line[edit | edit source]
Patients may benefit from physiotherapy based treatment with goals of CTS symptom reduction and functional gains, provided that:
- Their symptoms are intermittent and not rapidly worsening or if their CTS etiology is highly suggestive of the possibility of remission as an example of pregnancy-related CTS
- Patients are informed about the lack of high-quality evidence for the effectiveness and safety of therapeutic modalities used by physiotherapists,
Treatment should be discontinued when shown to be ineffective and appropriate, evidence-based discharge recommendations should be made.
CTS symptoms typically escalate over a longer-term despite conservative treatment. Surgical interventions for appropriate patients have been shown to be safe and more effective than any conservative intervention, Clinicians should be aware that constant tingling or numbness is associated with significant compression of the median nerve. Prolonged duration of such symptoms may lead to irreversible changes in its internal structure, affecting the effectiveness of surgery and leaving individuals with chronic symptoms and muscle atrophy of thenar eminence. Patients should be followed by their general practitioners to discuss surgical treatment options when necessary and desired.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Carpal Tunnel Syndrome Justin O. Sevy; Matthew Varacallo. Last Update: December 21, 2019. Available from:https://www.ncbi.nlm.nih.gov/books/NBK448179/ (last accessed 22.3.2020)
- ↑ Padua L, Coraci D, Erra C, Pazzaglia C, Paolasso I, Loreti C, Caliandro P, Hobson-Webb LD. Carpal tunnel syndrome: clinical features, diagnosis, and management. The Lancet Neurology. 2016 Nov 1;15(12):1273-84.
- ↑ 3.0 3.1 Chammas M, Boretto J, Burmann LM, Ramos RM, Neto FCS, Silva JB. Carpal tunnel syndrome – part 1 (anatomy, physiology, etiology and diagnosis). Revista brasileira de Ortopedia (English edition) 2014 September-October; 49 (5):429-436.
- ↑ 4.0 4.1 4.2 4.3 Radiopedia CTS Available from:https://radiopaedia.org/articles/carpal-tunnel-syndrome-1 (last accessed 23.3.2020)
- ↑ Michelsen H, Posner MA. Medical history of carpal tunnel syndrome. Hand clinics. 2002 May 1;18(2):257-68.
- ↑ Bagatur A.E., Zorer G. The carpal tunnel syndrome is a bilateral disorder. J Bone Joint Surg Br. 2001;83(5):655–658.
- ↑ Schuind F., Ventura M., Pasteels J.L. Idiopathic carpal tunnel syndrome: histologic study of flexor tendon synovium. J Hand Surg Am. 1990;15(3):497–503.
- ↑ Gray, Henry. Anatomy of the Human Body. Philadelphia: Lea & Febiger, 1918; Bartleby.com, 2000. www.bartleby.com/107/. [Date of Printout].
- ↑ Jesus Filho AG, do Nascimento BF. Comparative study between physical examination, electroneuromyography and ultrasonography in diagnosing carpal tunnel syndrome. Revista Brasileira de Ortopedia (English Edition). 2014 September–October; 49(5): 446–451.
- ↑ 10.0 10.1 10.2 10.3 Ashworth NL, MBChB. Carpal Tunnel Syndrome Clinical Presentation [Internet]. 1994 [Updated 2014 Aug 25; cited 2015 March 20].fckLRAvailable from:fckLRhttp://emedicine.medscape.com/article/327330-clinical.
- ↑ 11.0 11.1 Krom de M.C.T.F.M., MD, KnipschildP.G. Prof. Efficacy of provocative tests for diagnosis of carpal tunnel syndrome. The Lancet. 1990 Feb 17; Vol.335 Issue 8686: 393-395.
- ↑ Hadi M, Gibbons E, Fitzpatrick R. A structured review of patient-reported outcome measures for procedures for carpal tunnel syndrome. Oxford: Departmet of Public Health (University of Oxford); 2011. 33p.
- ↑ Sambandam SN, Priyanka P, Gul A, Ilango B. Critical analysis of outcome measures used in the assessment of carpal tunnel sundrome. Int Orthop. 2008 Aug; 32(4):497-504.
- ↑ 14.0 14.1 14.2 14.3 14.4 14.5 14.6 O’Connor D, Marshall SC, Massy-Westropp N, Pitt V. Non-surgical treatment (other than steroid injection) for carpal tunnel syndrome (Review). The Cochrane database of systematic reviews. 2012; volume (7):1-106.
- ↑ 15.0 15.1 15.2 15.3 15.4 15.5 Huisstede BM, Hoogvliet P, Randsdorp MS, Glerum S, van Middelknoop M, Koes BW. Carpal Tunnel Syndrome. Part I: Effectiveness of Nonsurgical Treatments–A Systematic Review. Archives of physical medicine and rehabilitation. 2010 Jul; 91(7):981-1004.
- ↑ 16.0 16.1 Piazzini DB, Aprile I, Ferrara PE, Bertolini C, Tonali P, Maggi L, Rabini A, Piantelli S, Padua L. A systematic review of conservative treatment of carpal tunnel syndrome. Clinical rehabilitation. 2007 Apr; 21(4):299-314.
- ↑ 17.0 17.1 Oskouei AE, Talebi GA, Shakouri SK, Ghabili K. Effects of Neuromobilization Maneuver on Clinical and Electrophysiological Measures of Patients with Carpal Tunnel Syndrome. Journal of physical therapy science. 2014 Jul; 26(7):1017-22.
- ↑ 18.0 18.1 18.2 Burke FD, Ellis J, McKenna H, Bradley MJ. Primary care management of carpal tunnel syndrome. Postgraduate medical journal. 2003 Aug; 79 (934):433-7.
- ↑ 19.0 19.1 19.2 Page MJ, O’Connor D, Pitt V, Massy-Westropp N. Exercise and mobilisation interventions for carpal tunnel syndrome. Cochrane Database Syst Rev. 2012;6:CD009899.
- ↑ Page MJ, Massy-Westropp N, O'Connor D, Pitt V. Splinting for carpal tunnel syndrome.
- ↑ Talebi GA, Saadat P, Javadian Y, Taghipour M. Manual therapy in the treatment of carpal tunnel syndrome in diabetic patients: A randomized clinical trial. Caspian journal of internal medicine. 2018;9(3):283.Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6121348/ (last accessed 23.3.2020)
- ↑ Peters S, Page MJ, Coppieters MW, Ross M, Johnston V. Rehabilitation following carpal tunnel release (Review). The Cochrane database of systematic reviews. 2013 Jun; 5(6): 1-147.