Anaphylaxis
Original Editor - Wajeeha Hassan
Top Contributors - Wajeeha Hassan, Kim Jackson and Lucinda hampton
Introduction[edit | edit source]
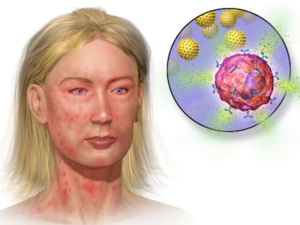
Anaphylaxis is a life threatening presentation of an acute systemic allergic reactions. It involves release of mediators which are derived from basophil cells and mast cells in the blood circulation and is an dangerous allergic condition that develops rapidly and can lead to death even.[1]
There is no specific clinical definition because of varied signs and symptoms. Some clinicians defined it as a condition that involves one or more than one systemic signs and symptoms but specific clinical features cannot be identified. This condition is usually triggered by the use of allergens.
French physiologist Charles Robert Richet in 1913 was awarded with Nobel prize in Medicine and Physiology for his research on anaphylaxis in collaboration with Paul Portier. [2]
Epidemiology[edit | edit source]
The world wide incidence of anaphylaxis roughly sit between 50 and 112 episodes per 100 000 person-years and prevalence over one’s life is roughly 0.3–5.1%.[1]
Causes[edit | edit source]
Common triggers which can induce an anaphylaxis includes
- Certain foods such as shell fish, peanuts, food additives or spices, tree nuts, beef, pork and almonds etc.
- Medication including Aspirin, Other NSAIDs, β -Lactams, Insulin, Protamine, Codeine, Meperidine, Dextromethorphan, Erythromycin, Methylprednisolone and Salmon calcitonin.
- Exercise induced
- Latex
- insect stings
- Idiopathic[3]
Effected Organs[edit | edit source]
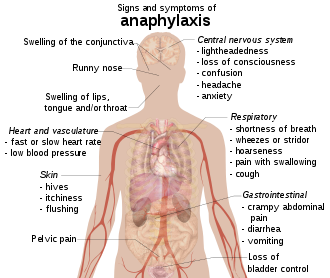
Organs which are most commonly effected in anaphylaxis include
- Skin
- Respiratory tract
- Gastrointestinal tract
- Cardiovascular system
- Central nervous system[4]
Classification[edit | edit source]
It has been classified into 3 categories on basis of severity of symptoms.
- Severe Reactions: It includes clinical features such as unconsciousness, confusion, incontinence, collapse and occur in combination with hypotension and hypoxia.
- Moderate Reactions: Diaphoresis, presyncope, dyspnea, vomiting, stridor, wheeze, chest tightness, nausea and abdominal pain has weak but significant association and is used to define moderate reactions.
- Mild Reactions: It includes reactions which are limited to involvement skin such as urticaria, erythema, and angioedema. [5]
Treatment[edit | edit source]
Epinephrine is most effective drug in initial treatment of anaphylaxis. This is because epinephrine works as alpha-1 adrenergic agonist and causes vasoconstriction which in turns helps in relieving laryngeal edema , hypotension and shock. [6] If timely injection of epinephrine is not given, it can lead an increased risk of hypoxic ischemic encephalopathy, biphasic anaphylaxis and fatality.[7] World Health Organization has designated the epinephrine as an essential medication for treatment of anaphylaxis and ampules of epinephrine are also available worldwide as compare to epinephrine auto-injectors.[8]
Personalised anaphylaxis management plans need to be incorporated in the longer-term care of patients post an anaphylachic event. This is very challenging in resources poor settings, affecting long term management adversley.[1]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Cardona V, Ansotegui IJ, Ebisawa M, El-Gamal Y, Fernandez Rivas M, Fineman S, Geller M, Gonzalez-Estrada A, Greenberger PA, Sanchez Borges M, Senna G, Sheikh A, Tanno LK, Thong BY, Turner PJ, Worm M. World allergy organization anaphylaxis guidance 2020. World Allergy Organ J. 2020 Oct 30;13(10):100472. Available from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7607509/
- ↑ Kemp SF, Lockey RF. Anaphylaxis: a review of causes and mechanisms. Journal of allergy and clinical immunology. 2002 Sep 1;110(3):341-8 https://www.sciencedirect.com/science/article/abs/pii/S0091674902001197
- ↑ Webb LM, Lieberman P. Anaphylaxis: a review of 601 cases. Annals of Allergy, Asthma & Immunology. 2006 Jul 1;97(1):39-43. https://www.sciencedirect.com/science/article/abs/pii/S1081120610613671
- ↑ Simons FE. Anaphylaxis pathogenesis and treatment. Allergy. 2011 Jul;66:31-4.https://onlinelibrary.wiley.com/doi/10.1111/j.1398-9995.2011.02629.x
- ↑ Brown SG. Clinical features and severity grading of anaphylaxis. Journal of Allergy and Clinical Immunology. 2004 Aug 1;114(2):371-6. https://www.sciencedirect.com/science/article/abs/pii/S0091674904013983
- ↑ Simons KJ, Simons FE. Epinephrine and its use in anaphylaxis: current issues. Current opinion in allergy and clinical immunology. 2010 Aug 1;10(4):354-61.https://pubmed.ncbi.nlm.nih.gov/20543673/
- ↑ Simons FE. 9. Anaphylaxis. Journal of Allergy and Clinical Immunology. 2008 Feb 1;121(2):S402-7. https://pubmed.ncbi.nlm.nih.gov/20176258/
- ↑ Simons FE, World Allergy Organization. World Allergy Organization survey on global availability of essentials for the assessment and management of anaphylaxis by allergy-immunology specialists in health care settings. Annals of Allergy, Asthma & Immunology. 2010 May 1;104(5):405-12.https://pubmed.ncbi.nlm.nih.gov/20486330/