Adult Spastic Cerebral Palsy: A Case Study with Anterior Knee Pain
Original Editor - Tessah MacDowall, Larry Burcher, Meagan Milton, Mackenzie Peters, Gillian Plummer and Erynne Rowe as part of Queen's University Neuromotor Function Project.
Top Contributors - Tessah MacDowall, Larry Burcher, Meagan Milton, Mackenzie Peters, Gillian Plummer, Erynne Rowe
Abstract[edit | edit source]
The purpose of this fictional case study is to outline the out-patient management of a 38-year-old female with cerebral palsy (CP) whose primary complaint is of bilateral anterior knee pain. Early on in her CP diagnosis, she was given a Level II rank on the Gross Motor Function Classification System (GMFCS) indicating that she can ambulate but has difficulties with uneven surfaces. Upon objective assessment, it was found that she has some indications of spasticity within the hamstrings and quadriceps according to the Modified Ashworth Scale. She also demonstrated a crouch gait pattern and reduced strength bilaterally in hip extensors, knee extensors, and ankle plantar flexors. Since quality of life has been shown to increase following improvements in walking, the focus of the program implemented in this case study is on gait training. Taken together, the information outlined in this fictional case can provide some evidence to guide decision-makers in the future and to highlight the importance of further research in adults that have CP.
Introduction[edit | edit source]
Cerebral palsy (CP) is an umbrella term used to describe a group of non-progressive motor impairment disorders.[1] [2] It is the result of neurodevelopmental disturbances, such as premature birth or stroke, that occurred at any time from conception to when the child was two years of age.[1][3] It is one of the most common causes of motor disability in children, with approximately 2 to 2.5 in 1000 Canadian children meeting the criteria for diagnosis.[1] [2][3] The disease’s severity is classified using the Gross Motor Function Classification System (GMFCS).[3]
Despite occurring in early childhood, approximately 75 percent of individuals currently living with CP are older than 18 years of age.[2] This number is expected to significantly increase by 2031.[1] As individuals with CP age, the clinical presentation of the condition changes. Adults with CP are roughly 7 to 10 times more likely than the general population to have a musculoskeletal morbidity.[4] [5] [2] Furthermore, nearly one-third of adults with CP report musculoskeletal pain that is associated with deteriorating physical function, such as inability to ambulate, and reduced participation in daily life. [6] [7] [8][9]
Musculoskeletal impairments and pain may be caused by altered gait patterns.[7] [10] [9] Specifically, the crouch (i.e., knee flexion) gait pattern commonly seen in individuals with CP has been significantly associated with knee pain.[7][9] Crouch gait is used to describe the two common knee patterns seen in CP gait: (1) increased knee flexion during the stance phase and (2) reduced knee flexion during the swing phase.[7] Increased knee flexion during stance may be caused by hamstring spasticity, quadriceps weakness, soleus weakness, and/or lever-arm dysfunction, whereas decreased knee flexion during swing may be due to rectus spasticity.[7] As a result of the crouch gait pattern, there is also an increase in patellofemoral forces in individuals with CP.[11][9] Furthermore, in a CP patient population, the patella is often located proximally to its typical anatomical location (i.e., patella alta) and is therefore more susceptible to dysfunction or subluxation that contributes to knee pain.[10] Improvements in independence, participation in activities of daily living, and overall quality of life can be seen following improvements in gait patterns.[6]
Client Characteristics[edit | edit source]
The patient is a 38-year-old female diagnosed with bilateral spastic CP. She was diagnosed at the age of 5 due to observable mild developmental delays, abnormal posture and high muscle tone. It was later discovered that she fell into the Level II category of the GMFCS. The patient reports that their forearm crutches are used during ambulation and provide increased stability and support. The patient presents with several health complications including type II diabetes, epilepsy, obesity (BMI of 32), chronic pain, and fatigue. The patient is seeking outpatient physiotherapy care for her bilateral anterior knee pain as a result of spasticity and altered gait.[12] The patient explains that the pain has progressively gotten worse over the last three months, rating it 7/10 on the numeric pain rating scale when walking and reports that it takes over an hour for her pain to come down to 3/10 when resting. The patient lives in a single-level community home where she has her own bedroom and bathroom. She reports being independent in most activities of daily living (ADLs) but relies on the support personnel for her meals and medication.
Examination Findings[edit | edit source]
Subjective Assessment[edit | edit source]
The patient is seeking physiotherapy care due to progressive functional decline and worsening anterior knee pain as a result of spasticity and altered gait due to cerebral palsy.[12] At baseline, patient uses forearm crutches to ambulate at home and in the community. Over the last few weeks, the patient has been noticing a decline in walking endurance, stating that she was previously able to walk 800m to the pool down the street to attend open lane swims but is now only able to walk ~400m at a time before needing to stop and take a break. The patient has been experiencing worsening sharp bilateral anterior knee pain over the last 3 months that reaches a 7/10 during walking and can last for over an hour before returning to a 3/10 at rest. Knee pain is also a 4/10 when rising from a seated or lying position and she reports that her “knees are stiff” when getting out of bed in the mornings. The patient is currently taking 650mg of acetaminophen daily for pain management, however, is finding this dosage to be less effective as her pain progresses. The patient expresses her enjoyment of art, karaoke, and swimming at the pool down the street, however, her participation in these activities has significantly decreased due to the pain and restricted mobility. The patient has a supportive family who would often come to visit her, however the frequency has decreased since COVID-19.
Other Medications: Diazepam[13], Neurontin, and Metformin[14].
Objective Assessment[edit | edit source]
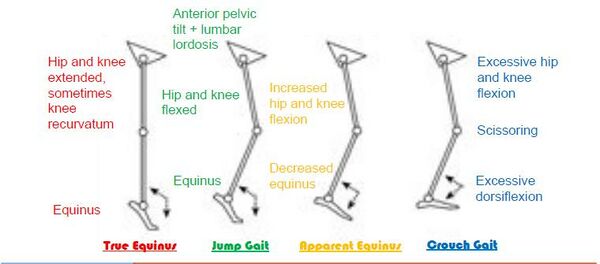
Objectively, the patient presents with increased anterior pelvic tilt, bilateral knee and hip flexion contractures and increased lumbar lordosis.[15] Upon palpation, the patient had increased tone in the hamstrings and quadriceps bilaterally throughout the available range as well as bilateral patella alta. The patient also had reduced strength bilaterally in the hip extensors (3+/5), knee extensors (3/5) and ankle plantar flexors (3/5).[16] Upper extremity strength was within normal limits. The patient also demonstrated spasticity in the hamstrings with a score of 1+ on the Modified Ashworth scale. The patient had intact sensation in the extremities, but deep tendon reflexes were brisk with clonus. This presentation of hyperreflexia is common in patients with spastic CP.[17] The Timed Up and Go (TUG) test and Six-Minute Walk Test (6MWT) were completed to assess locomotor function and walking endurance respectively. The patient completed both using her forearm crutches, the results are as follows TUG: 14.56s, 6MWT: 350m. During gait, the patient demonstrated increased knee flexion, hip flexion and ankle dorsiflexion during stance and reduced plantarflexion pre-swing.[15] She also walked with a slower gait speed, shortened stride length and required seated rest periods between trials. This gait pattern is similar to crouch gait, one of the most common gait patterns in CP.[18] For more information on how to classify crouch gait and other common CP gait patterns like the ones shown below click here.
Outcome Measures[edit | edit source]
Six-Minute Walk Test (6MWT)[edit | edit source]
The six-minute walk test is a submaximal VO2 test used to estimate an individual’s cardiorespiratory endurance. The six-minute walk test is commonly used with older adults and individuals with cardiorespiratory or neuromuscular conditions.
For more information on the 6MWT please click here Six-Minute Walk Test (6MWT).
Timed Up and Go (TUG) Test[edit | edit source]
The Timed Up and Go (TUG) test is used to determine the falls risk, balance, sit-stand, and walking ability of an individual. The TUG is commonly used with older adults and individuals with neuromuscular or musculoskeletal conditions.
For more information on the TUG please refer to Timed Up and Go Test (TUG).
Special Tests[edit | edit source]
Special tests are used frequently by physiotherapists to rule in or out potential differential diagnoses. There are a few special tests that are meant to assess anterior knee pain.
Manual Muscle Testing (MMTs)[edit | edit source]
Manual muscle testing is an assessment of muscle strength that can provide information about neurologic deficits. It is an important component to an objective assessment in patients with neurological conditions, gait abnormalities and balance problems.[3]
For more information on MMTs please refer to Muscle Strength Testing.
Modified Ashworth Scale[edit | edit source]
The Modified Ashworth scale was designed to assess spasticity in a variety of conditions including acquired brain injury (ABI), cerebral palsy (CP), multiple sclerosis (MS), spinal cord injury (SCI) and stroke.[19]
For more information on the Modified Ashworth scale please refer to Modified Ashworth Scale.
Numeric Pain Rating Scale (NPRS)[edit | edit source]
The Numeric Pain Rating Scale (NPRS) allows patients to rate their pain on a pre-defined scale. This is usually a scale from 0-10, where 0 is no pain and 10 is the worst pain imaginable. This scale is used in a variety of healthcare settings and allows clinicians to assess pain and track improvement in pain presentation.
Clinical Impression[edit | edit source]
Physiotherapy Diagnosis[edit | edit source]
38-year-old female patient presents with bilateral anterior knee pain which is limiting her ability to ambulate and participate in daily activities. The bilateral knee pain is resulting from an abnormal crouch gait pattern as well as spasticity and contracture in the muscles of the thighs.
Problem List[edit | edit source]
- Bilateral anterior knee pain impedes patient’s ability to ambulate.
- Presentation of bilateral patella alta resulting from hypertonicity of the quadriceps.
- Abnormal gait pattern due to hypertonicity and weakness.
- Bilateral weakness of the thigh muscles.
- Bilateral spasticity of the thigh muscles.
- Patient’s inability to participate in leisure activities due to increase in pain with ambulation.
- Poor VO2max as demonstrated by the 6MWT – negatively impacted by presentation of pain.
Goals[edit | edit source]
- Patient will be able to sit to stand without aggravating pain greater than 3/10 by the end of week 2.
- Patient will increase knee extensor strength to 4/5 by week 6.
- Patient will increase hip extensor strength to 4/5 by week 6
- Patient will be able to ambulate 800m to the pool with forearm crutches within 3 months.
Intervention[edit | edit source]
1. Interdisciplinary Collaboration[edit | edit source]
- Liaise with dietician regarding nutrition and diabetes management.
- Liaise with community occupational therapist for assessment of home set up and any equipment needs.
- Connect with community social worker for coping strategies due to decreased participation in social activities.
2. Pain Management[edit | edit source]
- Due to the patient’s history of epilepsy, the use of any electrical current modalities for pain management are contraindicated; therefore, the pain will be treated from a physiotherapy aspect by isometric exercise and cryotherapy.[20][21][22] [23] Cryotherapy will be in conjunction with cryo-stretch for intervention of spasticity management.
- Cryotherapy decreases the resistance to passive stretch from a few minutes up to 24 hours.[22][23]
3. Stretching[edit | edit source]
All stretches will be performed for 30 seconds, 2-3 times a day.[24]
| Joint | Muscle Group | Stretch |
| Knee | Hamstring
Quadriceps |
Sitting hamstring stretch
Side lying quad stretch |
| Ankle | Dorsiflexors | Kneeling stretch |
| Hip | Hip flexors | Lying prone |
Recent studies have found regular stretching does not produce clinically important changes in joint mobility, pain, spasticity or activity limitation in people with neurological conditions.[25] Due to this, stretching will be used in addition to cryotherapy while in the clinic.
4. Strengthening [edit | edit source]
Isometric strengthening will be used for pain management as well as muscle group strengthening. Joint movements generated during walking have been found to be similar to the corresponding muscle groups under static conditions.[26]
| Muscle group | Position[26] | Exercise | Parameters |
| Hip extensors | Supine, hip and knee flexed to 90 degrees, foot resting on stool | “push button into ground” | 5 sets x 5 reps x 5 seconds, 30-120s rest between sets |
| Hip abductors | Supine, hip in neutral | “push leg outwards, keep toes pointing up” | 5 sets x 5 reps x 5 seconds, 30-120s rest between sets |
| Quadriceps | Sitting, knee flexed to 90 degrees | “kick leg out” | 5 sets x 5 reps x 5 seconds, 30-120s rest between sets |
| Plantar flexors | Supine, hip and knee at 90 degrees, ankle in neutral | “push up on toes and hold” | 5 sets x 5 reps x 5 seconds, 30-120s rest between sets |
Although ACSM guidelines recommend 5 reps of 5 seconds holds at 5 different joint angles, this may be increasingly difficult for someone diagnosed with CP due to motor control difficulties and spasticity therefore, it was a clinical decision to use 5 sets instead of 5 different joint angles.[24]
5. Gait Training [edit | edit source]
Since, this patient has access to robotic gait training, it will be used as the main gait training intervention. Robotic gait training (RGT) has been found to improve kinematics of the hip, knee and ankle ultimately improving balance, locomotor function and gait biomechanics in CP populations.[27]
Week 0-6[edit | edit source]
- 3 x 1 hour sessions per week
- 3 x 10 minute bouts on the Lokomat RGT
- On week 0 patient will begin at a speed of 1.7m/s, if tolerable; By week 6 the goal speed is 2.7m/s.
- At week 0 the weight will be 50% of the patient’s body weight; The amount of body weight support will decrease over the 6 weeks of treatment
Week 7-12[edit | edit source]
- Transition to ambulation on ground surface
- Verbal and visual cues via a mirror will be used as feedback to ensure the patient is aware of the correct gait pattern when transitioning from the Lokomat RGT to the ground surface.[29] [30]
- The patient will begin by ambulating 25m with close supervision. As comfort level and correct gait patterning is established, the distance will increase up to the goal distance of 800m. The amount of supervision will decrease as the patient progresses.
Outcome[edit | edit source]
Following the initial assessment with the 38-year-old female patient, a 12-week physiotherapy treatment program was created to address her functional impairments and goals. She was seen for three x 60 minute sessions per week for the 12-week duration at which point reassessment and discharge occurred.
Upon implementation of the treatment plan, the patient steadily improved her gait mechanics through the stretching and strengthening protocol that coincided with the corrective feedback given by the Lokomat RGT training (Robotic Rehabilitation for the Lower Extremity). Despite exhibiting a crouch gait-like pattern, the patient was able to benefit from the interventions as seen through improvements in the management of her pain, muscular weakness, and altered gait mechanics.
The following outcomes were achieved by the end of 12 weeks and informed the rational for discharge:
Strength measured by Muscle Strength Testing (MMT):
- Right hip extensors (4/5)
- Left hip extensors (4/5)
- Right knee extensors (4/5)
- Left knee extensors (4/5)
- Right ankle plantar flexors (4/5)
- Left ankle plantar flexors (4/5)
- Upper extremity strength remained within normal limits.
Pain:
- NPRS for knee pain while walking = 3/10; takes 10 minutes to decrease to 2/10 when resting
- NPRS for knee pain upon rising from sitting or lying = 2/10
Gait:
- TUG: 10.32s
- 6MWT: 545m
- Self-reported ability to ambulate uninterrupted without a resting break over 800m.
Discharge[edit | edit source]
Discharge was agreed upon as the patient had met her functional goals as marked by the outcome measures documented above. She expressed interest in continuing treatment to maintain her progress and continue to improve. The patient was put into contact with a collection of supportive healthcare personnel and professionals through referrals.
Moreover, referrals were made for the patient to see a dietician to help her continue her diabetes and chronic fatigue management. An exercise physiologist was to be seen for additional support and overall strength and conditioning. A referral to the family health team was also made in order to assist in the management of her diabetes, epilepsy, chronic pain and fatigue. The occupational therapist and social worker referral is for assistance in arranging homecare equipment and social support services.
Additionally, as the patient enjoys swimming at the pool, she was recommended to take part in an aquatic therapy program at her local pool. These programs have been shown to be beneficial in the relief of joint pain.[31]
Discussion[edit | edit source]
This fictional case followed a 38-year-old female, who presented to physiotherapy with bilateral anterior knee pain secondary to her diagnosis of spastic CP, through 12 weeks of treatment. Upon arrival, she mentioned that her knee pain was worsening and had limited her participation in many of her hobbies (ie., swimming). An objective assessment found indications of spasticity within the hamstrings and quadriceps and reduced strength bilaterally in hip extensors, knee extensors, and ankle plantar flexors contributing to a crouch gait pattern. As anterior knee pain can result from all of these findings, our treatment intervention focused on targeting these issues. Prior to discharge, after 12 weeks, the patient displayed marked improvements in gait, walking endurance, lower extremity strength and pain. At the time of discharge, she was starting to increase her participation in hobbies that she previously had issues with and met all her outpatient physiotherapy goals. She was encouraged to continue working on strengthening her hip extensors, knee extensors, and ankle plantar flexors.
In general, the interventions described throughout this fictional case would be applicable to other patients with similar conditions. First, the characteristics of this fictional case are similar to the typical presentation of CP. Specifically, 80 to 90 percent of individuals with CP have spastic CP and approximately 21 percent of individuals with CP experience anterior knee pain.[3][9] It is important to note that the chance of knee pain also increases significantly (73.2 percent) with the presence of patella alta.[32] It is therefore more likely that an individual with CP, who is coming to physiotherapy, will display one or multiple characteristics that are similar to this fictional case.
Secondly, despite representing 75 percent of all individuals living with CP, there is limited research surrounding its management in an adult population. This means that there are no validated outcome measures for this population making it difficult to objectively determine whether your patient is making progress or not. The current case study uses evidence-based literature to provide potential options, such as the TUG or 6MWT, to mitigate this issue. While the TUG and 6MWT are not specific to the CP population, they do provide meaningful information about the patient’s locomotor function and walking endurance. For example, previous research has found that it is possible to increase the speed that a child with crouch gait walks by 30 percent if you increase the amount of knee extension during the stance phase.[33] Since the interventions of this case study targeted increasing knee extension, measuring gait speed using the TUG or 6MWT, where a shorter time indicates a faster pace, will provide the physical therapist with an objective outcome measure.
In conclusion, research in management of CP in adults is limited. This fictional case used available literature to devise a treatment plan to resolve bilateral anterior knee pain, in an adult patient with CP, that would target the objective findings of spasticity and weakness of the lower extremities and an altered gait pattern.
Self Study Questions[edit | edit source]
1. Individuals with Cerebral Palsy often develop altered gait patterns, one gait pattern that is commonly observed in individuals with Cerebral Palsy and results in knee pain is:
a) Wide-based gait
b) Steppage gait
c) Flat foot gait
d) Crouch gait
2. The severity of CP is classified using which tool?
a) Gross Motor Function Classification System (GMFCS)
b) Modified Ashworth scale
c) Timed Up and Go (TUG) Test
d) Chedoke-McMaster Stroke Assessment
3. Robotic gait training has been found to have an impact on what factors in cerebral palsy populations?
a) Hip and ankle kinematics
b) Hip, knee and ankle kinematics
c) Static balance
d) Dynamic balance
Answer Key[edit | edit source]
- d)
- a)
- b)
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Amankwah N, Oskoui M, Garner R, et al. Original quantitative research-Cerebral palsy in Canada, 2011–2031: results of a microsimulation modelling study of epidemiological and cost impacts. Health promotion and chronic disease prevention in Canada: research, policy and practice. 2020. 40(2): 25.
- ↑ 2.0 2.1 2.2 2.3 van Gorp M, Hilberink SR, Noten S, Benner JL, Stam HJ, van der Slot WM, Roebroeck ME. Epidemiology of cerebral palsy in adulthood: a systematic review and meta-analysis of the most frequently studied outcomes. Archives of Physical Medicine and Rehabilitation. 2020 Jun 1;101(6):1041-52.
- ↑ 3.0 3.1 3.2 3.3 3.4 Physiopedia.Cerebral palsy introduction [Internet]. 2016 Sep [cited 2022 May 11]. Available from: Cerebral Palsy Introduction
- ↑ French ZP, Torres RV, Whitney DG. Elevated prevalence of osteoarthritis among adults with cerebral palsy. Journal of Rehabilitation Medicine. 2019 Sep 1;51(8):575-81.
- ↑ Whitney DG, Hurvitz EA, Devlin MJ, Caird MS, French ZP, Ellenberg EC, Peterson MD. Age trajectories of musculoskeletal morbidities in adults with cerebral palsy. Bone. 2018 Sep 1;114:285-91.
- ↑ 6.0 6.1 Booth AT, Buizer AI, Meyns P, Oude Lansink IL, Steenbrink F, van der Krogt MM. The efficacy of functional gait training in children and young adults with cerebral palsy: a systematic review and meta‐analysis. Developmental Medicine & Child Neurology. 2018 Sep;60(9):866-83.
- ↑ 7.0 7.1 7.2 7.3 7.4 Ganjwala D, Shah H. Management of the knee problems in spastic cerebral palsy. Indian Journal of Orthopaedics. 2019 Feb;53(1):53-62.
- ↑ O'Connell NE, Smith KJ, Peterson MD, Ryan N, Liverani S, Anokye N, Victor C, Ryan JM. Incidence of osteoarthritis, osteoporosis and inflammatory musculoskeletal diseases in adults with cerebral palsy: a population-based cohort study. Bone. 2019 Aug 1;125:30-5.
- ↑ 9.0 9.1 9.2 9.3 9.4 Rethlefsen SA, Nguyen DT, Wren TA, Milewski MD, Kay RM. Knee pain and patellofemoral symptoms in patients with cerebral palsy. Journal of Pediatric Orthopaedics. 2015 Jul 1;35(5):519-22.
- ↑ 10.0 10.1 Miller F. Anterior Knee Pain and Patellar Subluxation in Cerebral Palsy. Cerebral Palsy. 2020:2127-35.
- ↑ Pelrine E, Novacheck T, Boyer E. Association of knee pain and crouch gait in individuals with cerebral palsy. Journal of Pediatric Orthopaedics. 2020 Jul 6;40(6):e504-9.
- ↑ 12.0 12.1 Yi YG, Jung SH, Bang MS. Emerging issues in cerebral palsy associated with aging: a physiatrist perspective. Annals of rehabilitation medicine. 2019 Jun;43(3):241.
- ↑ Goyal V, Laisram N, Wadhwa RK, Kothari SY. Prospective Randomized Study of Oral Diazepam and Baclofen on Spasticity in Cerebral Palsy. Journal of Clinical and Diagnostic Research. 2016;.
- ↑ Metformin [Internet]. Bethesda, MD: National Library of Medicine [2022, cited 2022 May 11]. Available from: https://medlineplus.gov/druginfo/meds/a696005.html
- ↑ 15.0 15.1 Gage JR, Schwartz MH, Koop SE. The identification and treatment of gait problems in Cerebral Palsy. 2014 [cited 2022 May 11]. p.194, 561 Available from: https://books.google.ca/books?hl=en&lr=&id=PiiDMzb551sC&oi=fnd&pg=PR9&dq=The%20treatment%20of%20gait%20problems%20in%20cerebral%20palsy&ots=77tEohFI8b&sig=NEdOjMtStwSLA6FDgUbaDxP4x1w&redir_esc=y&fbclid=IwAR01PRH28pXX4brwgQ9PtooErAbhh0K-RMwk_YderzyarJDzZ8TjfiXkREM#v=snippet&q=flexion%20contracture&f=false
- ↑ Arnold AS, Anderson FC, Pandy MG, Delp SL. Muscular contributions to hip and knee extension during the single limb stance phase of normal gait: a framework for investigating the causes of crouch gait. Journal of biomechanics. 2005 Nov 1;38(11):2181-9.
- ↑ Odding E, Roebroeck ME, Stam HJ. The epidemiology of cerebral palsy: incidence, impairments and risk factors. Disability and rehabilitation. 2006 Jan 1;28(4):183-91.
- ↑ Wren TA, Rethlefsen S, Kay RM. Prevalence of specific gait abnormalities in children with cerebral palsy: influence of cerebral palsy subtype, age, and previous surgery. Journal of Pediatric Orthopaedics. 2005 Jan 1;25(1):79-83.
- ↑ Ashworth Scale / Modified Ashworth Scale [Internet]. Chicago, IL: Shirley Ryan AbilityLab. [updated 2016 May 26, cited 2021May11]. Available from: https://www.sralab.org/rehabilitation-measures/ashworth-scale-modified-ashworth-scale
- ↑ Rio E, Kidgell D, Purdam C, Gaida J, Moseley GL, Pearce AJ, Cook J. Isometric exercise induces analgesia and reduces inhibition in patellar tendinopathy. British journal of sports medicine. 2015 Oct 1;49(19):1277-83.
- ↑ Van Ark M, Cook JL, Docking SI, Zwerver J, Gaida JE, Van Den Akker-Scheek I, Rio E. Do isometric and isotonic exercise programs reduce pain in athletes with patellar tendinopathy in-season? A randomised clinical trial. Journal of science and medicine in sport. 2016 Sep 1;19(9):702-6.
- ↑ 22.0 22.1 Akinbo SR, Tella BA, Onunla AB, Temiye EO. Comparison of the effect of neuromuscular electrical stimulation and cryotherapy on spasticity and hand function in patients with spastic cerebral palsy. Nigerian medical practitioner. 2007 Sep 18;51(6):128-32.
- ↑ 23.0 23.1 Mead S, Knott M. Topical Cryotherapy—Use for Relief of Pain and Spasticity. California Medicine. 1966 Sep;105(3):179.
- ↑ 24.0 24.1 American College of Sports Medicine. ACSM's guidelines for exercise testing and prescription. Lippincott Williams & Wilkins. 2018;
- ↑ Katalinic OM, Harvey LA, Herbert RD. Effectiveness of stretch for the treatment and prevention of contractures in people with neurological conditions: a systematic review. Physical therapy. 2011 Jan 1;91(1):11-24.
- ↑ 26.0 26.1 Dallmeijer AJ, Baker R, Dodd KJ, Taylor NF. Association between isometric muscle strength and gait joint kinetics in adolescents and young adults with cerebral palsy. Gait & posture. 2011 Mar 1;33(3):326-32.
- ↑ Carvalho I, Pinto SM, das Virgens Chagas D, Dos Santos JL, de Sousa Oliveira T, Batista LA. Robotic gait training for individuals with cerebral palsy: a systematic review and meta-analysis. Archives of physical medicine and rehabilitation. 2017 Nov 1;98(11):2332-44.
- ↑ Hocoma. Gait Training with LokomatPro - Product Demo. Available from: https://www.youtube.com/watch?v=7RGZ6JxVeAU&list=PLeIQpgcm-K09RBkCBOOiOFqZDwMSkY6-x&index=20
- ↑ Hamed NS, Abd-elwahab MS. Pedometer-based gait training in children with spastic hemiparetic cerebral palsy: a randomized controlled study. Clinical rehabilitation. 2011 Feb;25(2):157-65.
- ↑ Hussein ZA, Salem IA, Ali MS. Effect of simultaneous proprioceptive-visual feedback on gait of children with spastic diplegic cerebral palsy. Journal of Musculoskeletal & Neuronal Interactions. 2019;19(4):500.
- ↑ Kamioka H, Tsutani K, Okuizumi H, Mutoh Y, Ohta M, Handa S, Okada S, Kitayuguchi J, Kamada M, Shiozawa N, Honda T. Effectiveness of aquatic exercise and balneotherapy: a summary of systematic reviews based on randomized controlled trials of water immersion therapies. Journal of epidemiology. 2010 Jan 5:0910270113-.
- ↑ Pelrine E, Novacheck T, Boyer E. Association of knee pain and crouch gait in individuals with cerebral palsy. Journal of Pediatric Orthopaedics. 2020 Jul 6;40(6):e504-9.
- ↑ Cherni Y, Pouliot Laforte A, Parent A, Marois P, Begon M, Ballaz L. Lower limb extension is improved in fast walking condition in children who walk in crouch gait. Disability and Rehabilitation. 2019 Dec 18;41(26):3210-5.