Klippel-Feil syndrome
Original Editor - Emy Van Rode
Top Contributors - Emy Van Rode, Lucinda hampton, Rachael Lowe, Kim Jackson, Priyanka Chugh, Oyemi Sillo, WikiSysop, 127.0.0.1, Admin, Evan Thomas and Rucha Gadgil
Introduction[edit | edit source]
Klippel-Feil syndrome (KFS) is a complex condition presenting due to abnormal fusion of cervical vertebrae at C2 and C3, caused by a failure in the division or normal segmentation of the cervical spine vertebrae in the early fetal development. This condition leads to a characteristic appearance of a short neck, low hairline, facial asymmetry, and limited neck mobility. The anomalies can lead to chronic headaches, a limited range of neck motion, and neck muscle pain. Importantly, it can also result in spinal stenosis, neurologic deficit, cervical spinal deformity and instability. Patients can be polysyndromic in their presentation, as well.[1]
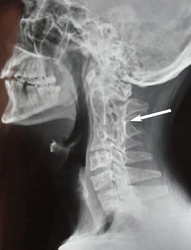
Image 1: X-ray showing fused cervical vertebrae as seen in Klippel–Feil syndrome
Etiology[edit | edit source]
The etiology of Klippel-Feil syndrome is not well known.
- Several studies have hypothesized that vascular disruption, global fetal insult, primary neural tube complications, or related genetic factors may carry implications in the development of KFS.
- It can co-present with fetal alcohol syndrome, Goldenhar syndrome, as well as Sprengel deformity[1].
Epidemiology[edit | edit source]
- Klippel-Feil syndrome occurs in approximately 1 in 40,000 to 42,000 newborns worldwide with a slight preference for females.
- It is important to recognize that asymptomatic pediatric patients, who do not undergo cervical imaging and do not present with an obvious physical deformity, are likely to graduate into adulthood unaware of their condition.[1]
Clinical Presentation[edit | edit source]
The following list includes the most common signs and symptoms in people with Klippel-Feil syndrome (KFS). These features may be different from person to person. Some people may have more symptoms than others and symptoms can range from mild to severe. This list also does not include every symptom or feature that has been described in this condition.[2]
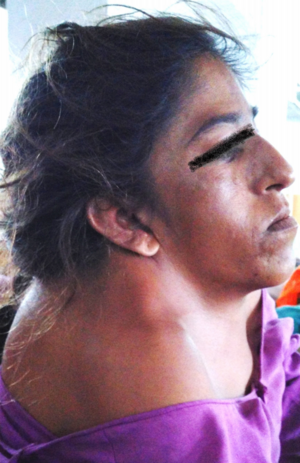
Image 2: Woman with Klippel–Feil syndrome
- Fusion of two or more spinal bones in the neck
- Short neck and low hairline
- Torticollis
- Congenital scoliosis
- Spina Bifida
- Kidney, rib and heart malformations
- Respiratory problems
- Neurological deficits
- Syndactyly (webbed fingers) and hypoplastic thumb (abnormality of the thumb)
- A condition called synkinesia — or mirror movement — where movement in one hand involuntarily mimics the deliberate movement of the other hand
- Sprengel's deformity, where the scapula are underdeveloped and sit high on the back causing weakness of the shoulders
- Cleft palate
- Hearing issues[3]
The classic complete clinical triad of the low hairline, short neck, and restricted neck motion is only present in 50% of patients with Klippel-Feil syndrome.[1]
Differential Diagnosis[edit | edit source]
- Healing osteomyelitis or discitis
- Previous fusion without instrumentation
- Juvenile idiopathic arthritis
- Juvenile rheumatoid arthritis can present with similar cervical spine anomalies, but a thorough workup and antibody testing would facilitate differentiating from KFS easily
- Ankylosing spondylitis
Diagnostic Procedures [edit | edit source]
KFS is typically diagnosed based on a clinical examination, symptoms and imaging studies (X-rays, MRI or CT scan). Additional studies may be necessary to look at other parts of the skeleton and other body systems.
- Some people with KFS have few or no symptoms, and are diagnosed by chance after having imaging studies for some other reason.[2]
- This syndrome is usually diagnosed when the presentation of complaints occur[4].
Treatment[edit | edit source]
No definitive treatment exists.
- Lifestyle modifications and preventive activities include avoidance of contact sports eg rugby.
- Neck braces and traction may provide symptomatic relief[5].
- Patients with persistent neurological pain, myelopathy, new-onset muscle group weakness, and documented spinal instability are operative candidates. Spinal deformities and instability drive surgical decision making. The surgeon can perform cervical fusion from either anterior or posterior approaches secondary to evaluation[1].
Physical Therapy Management[edit | edit source]
Klippel-Feil Syndrome can benefit from physiotherapy however these vary depending upon the person, their pain, severity and preferences
- For axial symptoms and radiculopathy, physiotherapists can use soft tissue massage and soft tissue mobilisation techniques. Avoid spinal manipulation.
- Aerobic (eg walking) and aquatic exercise (eg swimming) are preferred.
- Low intensity exercises are preferred as compared to strenuous exercises which might aggravate the problem .
- Avoid contact sports, exercises with falls, tumbling, jumping, and exercises stressing the cervical spine. Non-contact sports are recommended.
- Postural exercises and strengthening of neck, shoulder, and periscapular musculature is recommended in most patients.
- Range of motion should be increased in cases of torticollis and Sprengel's deformity.
- Scoliosis strengthening/stretching techniques (see here) and breathing exercises.
- A home exercise program.[6]
KFS cannot be resolved with physical therapy.
- Physical therapy in combination with non-steroidal medications could be useful to prevent degenerative changes.
- When a patient has several fused vertebrae the risk of osteoarthritic changes is increased because of the immobile joint. It is likely that the superior joint undergoes degenerative changes with formation of osteophytes. This can lead to Radiculopathy and/or myelopathy.[7][8]
Outlook[edit | edit source]
The prognosis for most children with KFS is good if the condition is diagnosed early in life. Continued monitoring for complications and treatment are important to successful long-term outcomes for individuals with KFS[3].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Menger RP, Rayi A, Notarianni C. Klippel Feil syndrome. Available: https://www.statpearls.com/articlelibrary/viewarticle/23908/ accessed11.10.2021)
- ↑ 2.0 2.1 NIH KFS Available: https://rarediseases.info.nih.gov/diseases/10280/klippel-feil-syndrome (accessed 11.10.2021)
- ↑ 3.0 3.1 Childrens Hospital Philadelphia KFS Available: https://www.chop.edu/conditions-diseases/klippel-feil-syndrome(accessed 11.10.2021)
- ↑ Tracy MR, Dormans JP, Kusumi K. Klippel-Feil Syndrome: Clinical Features and Current Understanding of Etiology. Clinical orthopaedics and related research. 2004; Nr. 424, pp. 183–190. Level of evidence: 2C
- ↑ Radiopedia KFS Available: https://radiopaedia.org/articles/klippel-feil-syndrome-3(accessed 11.10.2021)
- ↑ Disease maps Is there any natural treatment for Klippel-Feil Syndrome? Available:https://www.diseasemaps.org/klippel-feil-syndrome/top-questions/natural-treatment/ (accessed 11.10.2021)
- ↑ An HS, Simpson MJ. Surgery of the cervical spine. London: Baltimore: Williams & Wilkins, 1994. Print.
- ↑ Tollison DC, Satterhtwaite JR. Practical Pain Management. Philadelphia: Lippincott Williams & Wilkins, 2002. Print.