Cervical Radiculopathy
Original Editor - Stéphanie Dartevelle
Top Contributors - Scott Buxton, Admin, Jasper Vermeersch, Stéphanie Dartevelle, Rachael Lowe, Garima Gedamkar, Kim Jackson, Scott Cornish, Simisola Ajeyalemi, Thomas Rodeghero, Jesse Demeester, Laura Ritchie, 127.0.0.1, WikiSysop, Evan Thomas, Stijn De Coninck, Venugopal Pawar, Fasuba Ayobami, Maxime Tuerlinckx, Candace Goh, Rucha Gadgil, Wendy Walker, Lucinda hampton, Jess Bell, Johnathan Fahrner, Khloud Shreif, Olajumoke Ogunleye and Jelle Van Hemelryck
Introduction[edit | edit source]
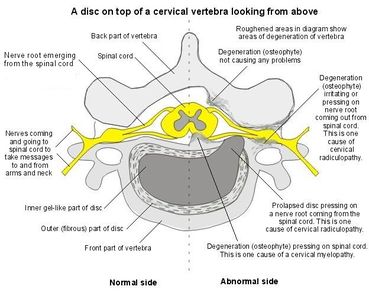
"Cervical radiculopathy is a disease process marked by nerve compression from herniated disk material or arthritic bone spurs. This impingement typically produces neck and radiating arm pain or numbness, sensory deficits, or motor dysfunction in the neck and upper extremities."[1]
Cervical radiculopathy occurs with pathologies that cause symptoms on the nerve roots. [2] Those can be compression, irritation, traction, and a lesion on the nerve root caused by either a herniated disc, foraminal narrowing, or degenerative spondylitic change (Osteoarthritic changed or degeneration) leading to stenosis of the intervertebral foramen[2] [3].
Most of the time cervical radiculopathy appears unilaterally, however it is possible for bilateral symptoms to be present if severe bony spurs are present at one level, impinging/irritating the nerve root on both sides. If peripheral radiation of pain, weakness, or pins and needle are present, the location of the pain will follow back to the concerned affected nerve root[2]
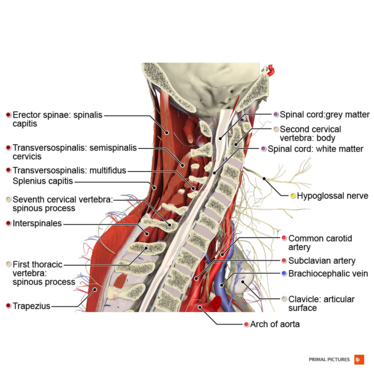
Clinically Relevant Anatomy[edit | edit source]
The human body has 8 cervical nerve roots, for 7 cervical vertebrae and this may seem confusing at first. However a nerve root comes out of the spinal column between C7 and T1, hence C8 as T1 already exists [2]. Tanaka N. et al[4] used a surgical microscope to do an anatomic study of the cervical intervertebral foramina, nerve roots, and intradural rootlets. The intervertebral foramina were shaped like a funnel with the entrance zone being the most narrow part. This was considered the place where the compression of the nerve roots in the intervertebral foramina occurs. Compression of the roots at the anterior side was ascribed to protruding discs and osteophytes of the uncovertebral region. Compression on the posterior side was caused by the superior articular process, the ligamentum flavum, and the periradicular fibrous tissues.
Nerve roots and the local vessels lack a perineurium and have a poorly developed epineurium, making them vulnerable to mechanical injury when compared to the periphery. The blood supply is also less secured and vulnerable to ischemic damage[5]. These anatomical differences to peripheral nerves may explain why low pressures on the nerve root elicit large changes and signs and symptoms. The nerve roots are vulnerable to pressure damage which is why small impingements can cause signs and symptoms.
At 5-10mmHg (0.1psi) capillary stasis and ischemia has been observed with partial blockage of axonal transport. At 50mmhg tissue permeability increases with an influx of oedema, higher than 75mmhg, there is nerve conduction failure if sustained for 2 hours. At 70+mmHg neural ischemia is complete and conduction is not possible[5]. It is rare to get pressures that high but 5-10mmhg is a large small amount of pressure and signs and symptoms occur[5]. These pressures can occur with a less severe clinical picture in unique circumstances, if the pressure is acute then symptoms are severe however if chronic the nervous tissue is given time to adapt and evolve to the surrounding structure and symptoms are less severe.
Epidemiology / Etiology[edit | edit source]
Cervical radiculopathy is a dysfunction of a nerve root in the cervical spine, is a broad disorder with several mechanisms of pathology and it can affect people of any age,[6] with peak prominence between the ages of 40-50 [2][7][8]. Reported prevalence is 83 people per 100,000 people [8]. Annual incidence has been reported to be 107,3 per 100.000 for men and 63,5 per 100.000 for women[9][10].
The two main mechanisms of the nerve root irritation or impingement are: [9]
- Spondylosis leading to stenosis or bony spurs - more common in older patients
- Disc herniation - more common in younger patients
Mechanical compression from spondylosis can affect the neuroforamen from all directions, which limits nerve root excursion. Cytokines released from damaged intervertebral discs can also cause this disorder. [9]
There is increasing evidence that inflammation itself and/or in association with root compression is the main cause of symptoms and signs. This is proved by the presence of interleukins and prostaglandin in herniated discs and the spontaneous recovery within weeks or months in the majority of patients. [11]
Level Of Compression
- Most common level of root compression is C7 (reported percentages 46.3–69%),
- Followed by C6 (19–17.6%)
- Compression of roots C8 (10– 6.2%)
- Compression of roots C5 (2–6.6%).
One possible explanation is that intervertebral foramina are largest in the upper cervical region and progressively decrease in size in the middle and lower cervical areas, with an exception of the C7-Th1 foramen (C8). [11][12]
Characteristics/Clinical Presentation[edit | edit source]
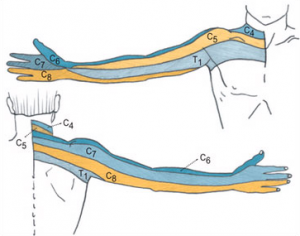
Typical symptoms of cervical radiculopathy are: irradiating arm pain corresponding to a dermatomal pattern, neck pain, parasthesia, muscle weakness in a myotomal pattern, reflex impairment/loss, headaches, scapular pain, sensory and motor dysfunction in upper extremities and neck[2][6][3][13][14].
Upper limb movements that are affected:
- C1/C2- Neck flexion/extension
- C3- Neck lateral flexion
- C4- Shoulder elevation
- C5- Shoulder abduction
- C6- Elbow flexion/wrist extension
- C7- Elbow extension/wrist flexion
- C8- Thumb extension
- T1- Finger abduction
The absence of radiating pain does not exclude nerve root compression. The same appears with sensory and motor dysfunction that might be present without significant pain [2].
Symptoms are generally amplified with movements that may be unidirectional or multidirectional reduce the space available for the nerve root to exit the foramen causing impingement [2]. This often causes the patient to present with a stiff neck and a decrease in cervical spine ROM, secondary musculoskeletal problems, decrease in muscle length of the cervical spine musculature (upper fibres of trapezius, scaleni, levator scapulae), weakness, joint stiffness, capsule tightness, and postural defects which can go on to affect movement mechanisms of the rest of the body.
Specifics
- The locality of sensory impairments associated with symptomatic C6 and C7 nerve root compression overlap to the extent that care should be exercised when diagnosing compression of either the C6 or C7 nerve roots based on locations of impaired sensation.
- Distal forearm impaired sensation is more common in C6 radiculopathies.[15]
Differential Diagnosis[edit | edit source]
Differentiating from cervical radiculopathy is derived from a combination of a patient's history, physical examination, and radiological findings. [16] Pathologies which mimic the signs and symptoms of radiculopathy.[17]
- Spinal Tumor
- Systemic diseases known to cause peripheral neuropathies
- Cervical myelopathy
- Ligamentous Instability
- Vertebrobasilar Insufficiency (VBI)
- Shoulder Pathology
- Peripheral nerve disorders
- Thoracic outlet syndrome
- Brachial plexus pathology
- Systemic disease
- Parsonage-Turner syndrome
- Superior pulmonary sulcus tumour
Diagnostic Procedures[edit | edit source]
The most common diagnostic methods used to assess the presence of possible compression are radiographs, MRI and electrophysiologic studies (EMG + Nerve Conduction Studies) to examine the nerve root and nerve conduction velocity [18][2][6].
Root compression seen on an MRI may confirm cervical radiculopathy, but to detect foraminal stenosis, which causes a bony compression on the nerve, spiral CT is described as the best way to detect this.[11]
There still is no consensus on whether conventional needle myography (EMG) has a strong diagnostic value for cervical radiculopathy. Several unblinded studies have reported sensitivities ranging from 30-95%.[11]
A subjective history and mechanism of Injury can be integral to an accurate diagnosis and the cause of radiating arm pain. More frequently acute radiating arm pain is caused by a disk herniation, while chronic bilateral axial neck and radiating arm pain is usually caused by cervical spondylosis [2].
Outcome Measures[edit | edit source]
Neck disability index NDIPatient Specific Functional Scale PSFS
Numerical Pain Rating Scale NPRS
Neck Pain and Disability Scale (NPAD)
Examination[edit | edit source]
Provocative tests are performed to provoke or worsen the symptoms in the affected arm and are indicative of cervical radiculopathy.[11]
Wainner et al[19] examined the accuracy of the clinical examination and developed a clinical prediction rule to aid in the diagnosis of cervical radiculopathy. Their research demonstrated that these 4 clinical tests, when combined, hold high diagnostic accuracy compared to EMG studies:
- Spurlings Test,
- Upper limb tension-1
- Distraction test
- involved side cervical rotation range of motion less than 60 degrees.
When all 4 of these clinical features are present, the post test probability of cervical radiculopathy is 90%, Where only 3 of the 4 tests are positive the probability decreases to 65%[19] [3][6][20]. A further combination of tests with good reliability are the combination of Spurlings Test, Neck Distraction, Valsalva and Upper Limb Tension Tests 1, 2a and 2b[21].
Tong HC et al [22]. performed the Spurling test before imaging was completed. The test had a sensitivity of 30% and a specificity of 93%. They concluded that the Spurling test is not sensitive, but it is very specific for cervical radiculopathy. It is therefore not useful as a screening test but it can well be used to confirm a cervical radiculopathy.
A study conducted by Gumina et al[23] found Arm Squeeze test useful to distinguish between cervical nerve root compression and shoulder disease. The test has 96% for both sensitivity and specificity, inter-observer value of 0.81 and intra-observer value of 0.87. However, the test utilizes subjective measures and needs to be validated.
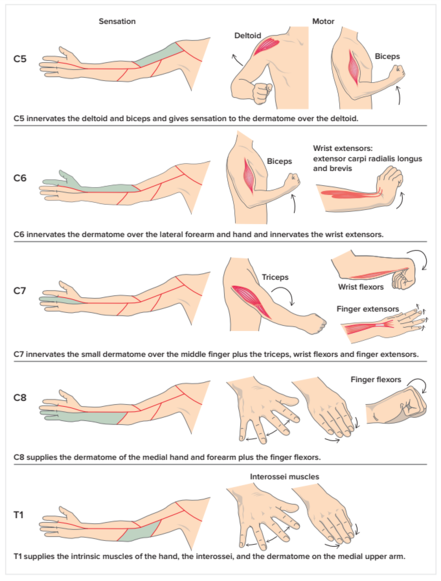
The neurologic examination has moderately strong intraobserver reliability with a kappa value between 0.4 and 0.64 The sensory examination can distinguish between a C8 radiculopathy and ulnar neuropathy, as there will be splitting of the hyperalgesia in either the third or fourth digit with ulnar neuropathy. With C8 radiculopathy, the entire digit will be affected. Motor examination may or may not show a grade of weakness in the myotome that corresponds to the pathologic nerve. No myotome corresponds to the upper four cervical nerve roots. C5 radiculopathy may show weakness in the deltoids (evaluated by testing for shoulder abduction); C6 will show weakness in the biceps and flexor carpi ulnaris (evaluated by testing for wrist extension); C7 weakness occurs in the triceps, as well as the brachioradialis (evaluated by testing for ellbow extension); C8 pathology causes weakness in the intrinsic muscles of the hand, as evaluated by finger abduction and grip. Muscle stretch reflexes also tend to be decreased in the setting of radiculopathy. Biceps hyporeflexia is indicative of C6 radiculopathy, while decrease in the triceps and brachioradialis reflexes corresponds to pathology at C7. according to Viikari-Juntura(1989). [24][25]
Medical Management[edit | edit source]
There are several intervention strategies for managing cervical radiculopathy, with physical therapy and surgical interventions being the most common. The long term benefits of surgical interventions are questionable however with 25% of patients continuing to experience pain and disability at 12 month follow-ups [26]. There is a significant amount of evidence to support the use of physical therapy interventions [27], and the benefit of physical therapy and manual techniques in general for patients with neck pain with or without radicular symptoms.
Surgery[edit | edit source]
Indications for a single level surgery; [28]:
- Sensory symptoms (radicular pain and/or paresthesias) in a dermatomal distribution that correlates with involved cervical level
- Motor deficit, reflex changes or positive EMG correlated to involved cervical level
- A positive response to a selective nerve root block (SNRB).
- Positive MRI or myelogram with computed tomography (CT) scan.
- At least 6 weeks of conservative care such as physical therapy, epidural injections, NSAID’s, pain killers.
- In case of clear motor deficit, 6 weeks of conservative care are not required.
Criteria for a 2nd level surgery:
- All of the criteria previously described for a single level surgery, not including SNRB, are present at the primary level.
- The adjacent level has radicular pain correlating with at least moderate foraminal stenosis or lateral recess herniation or EMG changes, motor deficits or reflex changes correlated to adjacent level.
Operative techniques that are frequently used as treatment for cervical radiculopathy are:
- Anterior Cervical Dissectomy (decompression) (ACD),
- Anterior Cervical Dissectomy and Fusion (ACDF),
- Total Disc Arthroplasty (TDA),
- Laminotomy,
- Foraminotomy,
- Corpectomy. [29][28]
Engquist M et al. found that surgery with physiotherapy resulted in a more rapid improvement during the first postoperative year, with significantly greater improvement in neck pain and the patient's global assessment than physiotherapy alone. The differences between the groups decreased after 2 years. They suggested that structured physiotherapy should be tried before surgery is chosen.[30]
Persson et al. concluded that there were no long term (1 year) differences between surgery and physical therapy in strength, pain and sensation.[31] Several other studies demonstrated that physical and social functioning and pain significantly improved after surgery, although these improvements remained relatively short termed (max 1 year) and diminished after a longer period (1 to 4 years).[29]
ACDF is associated with diminished ROM and strength compared to conservative treated subjects. This can, occasionally, be associated with prolonged pain. [29]
Peolsson A et al. concluded that ACDF did not result in additional improvements in neck active range of motion, neck muscle endurance, or hand-related function compared with a structured physiotherapy program alone in patients with cervical radiculopathy. The article suggests that a structured physiotherapy program should precede a decision for ACDF intervention in patients with cervical radiculopathy, to reduce the need for surgery. [32]
Short duration of pain, low health quality, high levels of anxiety due to neck/arm pain, low self-efficacy, and a high level of distress before treatment were associated with poor outcomes from surgery.[30]
Injections[edit | edit source]
Epidural steroid injections can also be used as treatment for cervical radiculopathy. The injections are given under the guidance of fluoroscopy or CT. There is limited evidence that transforaminal epidural steroid injections provide relief for 60% of the patients and about 25% of the patients with clear surgical indications. Steroid injections are not a causal treatment and are not a solution, although they can be considered when developing a medical/interventional treatment plan for patients with cervical radiculopathy from degenerative disorders. Trans-foraminal injections are not without risk and possible complications such as spinal cord injury and death must be considered before performing this procedure. [33][34]
Lee SH et al. researched the use of ESI (Epidural Steroid Injections) in patients diagnosed with cervical soft disc or hard disc causing nerve root compression and symptoms. In more than 80% of patients with CR who were surgical candidates, surgery was avoided using ESI. The significant factors predisposing failure of ESI were intensity of symptoms and a previous episode of CR. [35]
Physical Therapy Management[edit | edit source]
Although a definitive treatment progression for treating cervical radiculopathy has not been developed, a general consensus exists within the literature that using manual therapy techniques in conjunction with therapeutic exercise is effective in regard to increasing function, as well as active range of movement (AROM), focusing on decreasing levels of pain and disability will most likely be the main focus of the patient[36]. Recent high level research confirms the positive outcomes of exercise therapy[27].
If the patient has had long-term pain, an element of pain sensitisation may have developed and chronic pain behaves differently to acute pain. Therefore education about pain and reconceptualisation may be necessary.
Treatment Options:
- Education and advice
- Manual Therapy - PAIVMs (Passive Assessory Intervertebral Movements) / PPIVMs (Passive Physiological Intervertebral Movements) / NAGs (Natural Apophyseal Glides) / SNAGs (Sustained Natural Apophyseal Glides)
- Exercise Therapy - AROM, stretching and strengthening
- Postural re-education
Education and Advice[edit | edit source]
Education is key to getting the patient on side and to work co-operatively with physiotherapy. If a patient understands the condition and the reason for the neck and arm pain then they are more likely to be compliant with any rehabilitation plan.
In cases of a prolapsed disc, tobacco smoking causes constriction of the vascular network surrounding the intevertebral disc (IVD), reducing the indirect exchange of nutrients and anabolic agents from the blood vessels to the disc. Nicotine down-regulates the proliferation rate and glycosaminoglycan (GAG) biosynthesis of disc cells. Nicotine mostly affects the GAG concentration at the cartilage endplate, reducing it up to 65% of the value attained in normal physiological conditions. Tabacco mostly affects the nucleus pulposus, whose cell density and GAG levels reduce up to 50% of their normal physiological levels. The effectiveness of quitting smoking on the regeneration of a degenerated IVD shows limited benefit on the health of the disc. Cell-based therapy in conjunction with smoke cessation should provide significant improvements in disc health, suggesting that, besides quitting smoking, additional treatments should be implemented in the attempt to recover the health of an IVD degenerated by tobacco smoking. [37]
Manual Therapy[edit | edit source]
There are some contradictions for using manual therapy techniques and its efficacy is questioned. Gross AR et al reported mobilisation and/or manipulation when combined with exercise was beneficial for pain relief and improvement of function for persistent mechanical neck disorders with or without headache, but as a stand alone treatment manipulation and/or mobilisation was not beneficial. This is echoed in the current literature. In a multimodal treatment model, the addition of manual therapy techniques (thought to increase the size of the intervertebral foramen of the affected nerve root) has no significant additional benefits [38][39][40] Compared to one another, neither was superior either.[41] At best manipulations may also only provide short term pain relief [42]
Furthermore, cervical spine manipulation carries a risk of complications like vertebral dissection and spinal cord compression because of massive disc herniation. Therefore, this intervention should be discouraged in cervical radiculopathy, especially if imaging of the spine has not yet been performed. [11] Aware of any potential risk factors such as arterial insufficiency, Hypertension, Craniovertebral ligament insufficiency and upper motor neurone disorders is also essential[43].
Fritz JM et al examined the effectiveness of cervical traction in addition to exercise in patients with cervical radiculopathy. Adding mechanical traction to exercise for patients with cervical radiculopathy resulted in lower disability and pain, particularly at long-term follow-ups. [44][45]
Boyles et al (2011) [46] however found that manual therapy consisting of thrust mobilisations of the cervical or thoracic spine and cervical non-thrust mobilisations (PA glides/Lateral Glides in ULTT1 position/Rotations/Retractions) was shown to be effective at reducing pain levels, improving function and increasing joint ROM. When combined with exercise therapy it was more effective than the control group of manual therapy or exercise therapy however both control groups were effective at reducing signs and symptoms[47].
Persson et al [31] highlighted that there was no significant difference between outcome measures of patients who had had surgery, physiotherapy or cervical collar explaining that physiotherapy is at least as effective as surgery.
Muscle Energy Techniques[edit | edit source]
Cleland et al [48] utilised muscle energy techniques (MET) in 28 patients, 46% receiving positive outcomes. However details of the techniques used were insufficient and a variety of techniques were used as it was down to the practitioner to decide which technique would be used.
The quality of research related to testing the effectiveness of MET is poor. Studies are generally small and at high risk of bias due to methodological deficiencies.[49]
Neurodynamics - Gliding and Sliding/Tensioning[edit | edit source]
Ragonese (2009)[47] performed the neurodynamics sliding and tensioning techniques, outlined by Butler[50], whilst having the patient in an upper limb tension positions described by Magee[51] conducted in a slow and oscillatory manner. With improvement in symptoms, the technique was progressed to a ‘tension’ technique, also described by Butler. Again, positive outcomes were observed in regards to pain and function, although treatment duration was not recorded.
Exercise Therapy[edit | edit source]
Exercise therapy has the most positive and lasting effects for the condition.[27] Exercises targeted at opening the intervertebral foramen are the best choice for reducing the impact of radiculopathy. Exercises such as contralateral rotation and sideflexion are amongst the simplest forms of exercises which are effective against signs and symptons, given in the form of active ROM[38]. Due to the intricate and close relationship of muscles on the intervertebral foramen and the likely presentation of reduced ROM, stretching is also an effective form of treatment to regain ROM[52]
Once ROM increases strengthening exercises can be performed to develop stability and reduce the risk of developing nerve root irritation in the future, as long as it is not caused by a structure which cannot be influenced by physical therapy. During the initial stages of treatment, strengthening should be limited to isometric exercises in the involved upper limb. Once the radicular symptoms have been resolved, progressive isotonic strengthening can begin. This should initially involve low weight and high repetitions (15-20 repetitions). Closed kinetic chain activities can be very helpful in rehabilitating weak shoulder girdle muscles. However, Griffiths et al found no significant difference with the addition of specific neck stabilisation exercises to a program of general neck advice and exercise [53].
Patient should be instructed to remain as active as possible and perform exercises daily on the days between therapy sessions. Written exercise instructions should therefore be available. We suggest a 2 components program, as suggested by Fritz JM et al. 2 components: scapula strengthening and cervical strengthening.
Cervical strengthening exercises should include supine craniocervical flexion to elicit contraction of the deep neck flexor muscles without contraction of superficial neck muscles [54]. Feedback using an air-filled pressure sensor or tactile cues can be useful. Patient should perform three sets of 10 contractions of 10 seconds with proper muscle activation. Craniocervical flexion contractions were also performed with the patient seated, with the goal of 30 repetitions of 10-second contractions.
Scapular retraction against resistance using elastic bands or pulleys can be added. Scapular-strengthening exercises included prone horizontal abduction, sidelying forward flexion, prone extension of each shoulder, as well as prone push-ups with emphasis on shoulder protraction. The goal was 3 sets of 10 repetitions, with resistance added as tolerated.
Prognosis[edit | edit source]
Regarding physical therapy interventions, in 2007 Joshua Cleland and colleagues[48] examined the predictors of positive short-term outcomes in people with a clinical diagnosis of cervical radiculopathy. The following clinical features were found to be most predictive of a positive short-term outcome:
- Age <54
- Dominant arm not affected
- Looking down does not worsen symptoms
- Treatment involves manual therapy, cervical traction, and deep neck flexor strengthening for at least 50% of visits
If 3 of these features are present, the probability of success is 85%, and increases to 90% if all 4 are present[55]
Clinical Bottom Line[edit | edit source]
Cervical radiculopathy is defined as a disorder (compression, traction, irritation, herniated disk) affecting a spinal nerve root in the cervical Spine. Cervical radiculopathy typically produces neck and radiating arm pain, numbness, sensory deficits, or motor dysfunction in the neck and upper extremities. It is important to have knowledge of the cervical anatomy, because it is the key to effective physiotherapy practice and treatment.
Because there are other pathologies that have the same signs and symptoms of radiculopathy, it’s recommended to do a good examination. You can use imaging studies (MRI) or electro physiologic studies(EMG + Nerve Conduction Studies) [56][1][39]. Better, is to use these 4 clinical tests: Spurlings Test, Upper limb tension-1 Distraction test and Cervical Flexion Rotation Test. When all 4 of these clinical test are positive, the post-test probability of cervical radiculopathy is 90%.
The main focus for physical therapy or medical management of cervical radiculopathy, is decreasing the pain and disability. Once the treatment is started, it’s important to choose the right tool to evaluate your patient. The Neck disability index is a good option.
References[edit | edit source]
- ↑ 1.0 1.1 Eubanks J. Cervical Radiculopathy: Nonoperative Management of Neck Pain and Radicular Symptoms. Am Fam Physician. 2010 Jan 1;81(1):33-40.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 2.9 Eubanks, JD.Cervical Radiculopathy:Nonoperative Management of Neck Pain and Radicular Symptoms.American Family Physician 2010;81,33-40
- ↑ 3.0 3.1 3.2 Kenneth A. Olson. Manual physical therapy of the spine.Saunders Elsevier 2009.p 253, 257, 258
- ↑ Tanaka N. et al, The anatomic relation among the nerve roots, intervertebral foramina, and intervertebral discs ofthe cervical spine. Spine. 2000 February; 25(3): 286-291
- ↑ 5.0 5.1 5.2 Lipetz, JS. Pathophysiology of inflammatory, degenerative, and compressive radiculopathies. Phys Med Rehabil Clin N Am. 2002. 13: 439–449
- ↑ 6.0 6.1 6.2 6.3 Young IA,Michener LA,Cleland JA,Aguilera AJ,Snyder AR.Manual therapy, exercise, and traction for patients with cervical radiculopathy: a randomize clinical trial.Physical Therapy 2009;89:632-642
- ↑ Radhakrishnan K, Litchy WJ, O'Fallon M, et al. Epidemiology of cervical radiculopathy: A population-based study from Rochester, Minnesota, 1976 through 1990. Brain 1994; 117:325-335.
- ↑ 8.0 8.1 Bogduk N. Twomey CT. Clinically Relevant Anatomy for the Lumbar Spine. 2ed. Edinburgh UK: Churchill Livingston. 1991
- ↑ 9.0 9.1 9.2 Barrett I. et al. Cervical Radiculopathy Epidemiology, Etiology, Diagnosis, and Treatment. Journal of Spinal Disorders &Techniques. April 2015; 28:5.
- ↑ Radhaknshnank et al. Epidemiology of Cervical Radiculopathy. A Population Based Study. Brain. 1994: 117; 325-335
- ↑ 11.0 11.1 11.2 11.3 11.4 11.5 Kuijper B. et al. Degenerative cervical radiculopathy: diagnosis and conservative treatment: A review. European journal of neurology. 2009; 16(1): 15-20
- ↑ Ellenberg M, Honet J, Treanor W. Cervical Radiculopathy. Arch Phys Med Rehabil. 1994; 75:342-352.
- ↑ Kenneth W. Lindsay, Ian Bone.Neurology and neurosurgery illustrated.4th ed. Churchill Livingstone.p408
- ↑ Kuijper B, Tans JT, Beelen A, Nollet F, de Visser M.Cervical collar or physiotherapy versus wait and see policy for recent onset cervical radiculopathy : randomised trial.BMJ 2009;p1-7
- ↑ Rainville J, Laxer E, Keel J, Pena E, Kim D, Milam RA, Carkner E. Exploration of sensory impairments associated with C6 and C7 radiculopathies. The Spine Journal. 2016 Jan 1;16(1):49-54. Available:https://pubmed.ncbi.nlm.nih.gov/26253986/ (accessed 26.9.2022)
- ↑ Gu R., et al. Differential diagnosis of cervical radiculopathy and superior pulmonary sulcus tumor. Chinese medical journal. 2012 August; 125(15): 2755-2757
- ↑ C: R. Erhard et al. Cervical Radiculopathy or Parsonage-Turner Syndrome: Differential Diagnosis of a Patient With Neck and Upper Extremity Symptoms. JOSPT. OCTOBER 2005fckLRVolume 35, No. 10
- ↑ Partanen J, Partanen K, Oikarinen H, et al. Preoperative electroneuromyography and myelography in cervical root compression. Electromyogr Clin Neurophysiol. 1991; 31:21-26.
- ↑ 19.0 19.1 Wainner RS, Fritz JM, Irrgang JJ, et al. Reliability and diagnostic accuracy of the clinical examination and patient self-report measures for cervical radiculopathy. Spine. 2003;28(1):52-62.
- ↑ C: Wainner et al. Reliability and diagnostic accuracy of the clinical examination and patient self-report measures for cervical radiculopathy. Spine 2003 Jan 1. 28(1):52-62.
- ↑ Sidney M. et al. A systematic review of the diagnostic accuracy of provocative tests of the neck for diagnosing cervical radiculopathy. European Spine Journal. April 2006; 16(3): 307-319 LoE: 2A
- ↑ Tong HC, Haig AJ, Yamakawa K.. The spurling test and cervical radiculopathy. Spine. 2002 January;27(2):156-159. LoE: 2B
- ↑ Gumina, S., Carbone, S., Albino, P., Gurzi, M., & Postacchini, F. (2013). Arm Squeeze Test: a new clinical test to distinguish neck from shoulder pain. European Spine Journal, 22(7), 1558–1563. http://doi.org/10.1007/s00586-013-2788-3
- ↑ Viikari-Juntura E, Porras M, Laasonen EM. Validity of clinical tests in the diagnosis of root compression in cervical disc disease. Spine (Phila Pa 1976) 1989;14(3):253–257. LoE: 2B
- ↑ John M. Caridi. Cervical Radiculopathy: A Review. HSS journal, 2011. 7: 265 - 272. LoE: 2A
- ↑ Heckmann J, Lang J, Zobelein I, et al. Herniated cervical intervertebral discs with radiculopathy: an outcome study of conservatively or surgically treated patients. J Spinal Disord. 1999;12:396-401.
- ↑ 27.0 27.1 27.2 Cheng CH, Tsai LC, Chung HC, Hsu WL, Wang SF, Wang JL, Lai DM, Chien A. Exercise training for non-operative and post-operative patient with cervical radiculopathy: a literature review. 2015 Sep. J Phys Ther Sci. 27(9): 3011-8.
- ↑ 28.0 28.1 Leveque JC. Diagnosis and treatment of Cervical Radiculopathy and Myelopathy. 2015. Physical medicine and rehabilitation clinics of North America 26(3): 491-511.
- ↑ 29.0 29.1 29.2 Matz PG1 et al., Indications for anterior cervical decompression for the treatment of cervical degenerative radiculopathy, J Neurosurg Spine. 2009 Aug;11(2):174-82. LoE: 2A
- ↑ 30.0 30.1 Engquist M et al., Surgery Versus Nonsurgical Treatment of Cervical Radiculopathy: A Prospective, Randomized Study Comparing Surgery Plus Physiotherapy With Physiotherapy Alone With a 2-Year Follow-up. 15 september 2013. Spine, 38(20): 1715–1722.
- ↑ 31.0 31.1 Persson LC1, Moritz U, Brandt L, Carlsson CA. Cervical radiculopathy: pain, muscle weakness and sensory loss in patients with cervical radiculopathy treated with surgery, physiotherapy or cervical collar. A prospective, controlled study. Eur Spine J. 1997;6(4):256-66.
- ↑ Peolsson A et al. Physical Function Outcome in Cervical Radiculopathy Patients After Physiotherapy Alone Compared With Anterior Surgery Followed by Physiotherapy: A Prospective Randomized Study With a 2-Year Follow-up. 15 February 2013. Spine 38(4): 300-307
- ↑ Kim H, Lee SH, Kim MH. Multislice CT fluoroscopy-assisted cervical transforaminal injection of steroids: technical note. J Spinal Disord Tech 2007;20:456–61.
- ↑ Anderberg L, Annertz M, Persson L, et al. Transforaminal steroid injections for the treatment of cervical radiculopathy: a prospective and randomised study. Eur Spine J 2007;16:321–8
- ↑ Lee SH et al. Clinical Outcomes of Cervical Radiculopathy Following Epidural Steroid Injection: A Prospective Study With Follow-up for More Than 2 Years. 20 May 2012. Spine 37(12): 1041-1047.
- ↑ Boyles, Robert; Toy, Patrick; Mellon, James; Hayes, Margaret; Hammer, Bradley.Effectiveness of manual physical therapy in the treatment of cervical radiculopathy: a systematic review Journal of Manual and Manipulative Therapy 19 (2011) 135-142.
- ↑ Elmasry S, Asfour S, de Rivero Vaccari JP, Travascio F. Effects of Tobacco Smoking on the Degeneration of the Intervertebral Disc: A Finite Element Study. PLoS One. 2015 Aug 24;10(8):e0136137. LoE: 4
- ↑ 38.0 38.1 Langevin P, Desmeules F, Lamothe M, Robitaille S, Roy JS. Comparison of 2 manual therapy and exercise protocols for cervical radiculopathy: a randomized clinical trial evaluating short-term effects. 2015 Jan. J Orthop Sports Phys Ther 45(1):4-17.
- ↑ 39.0 39.1 Young IA. et al. Reliability, Construct Validity, and Responsiveness of the Neck Disability Index, Patient-Specific Functional Scale, and Numeric Pain Rating Scale in Patients with Cervical Radiculopathy. American Journal of Physical Medicine & Rehabilitation. October 2010; 89(10): 831-839
- ↑ Fredin K, Lorås H, Manual therapy, exercise therapy or combined treatment in the management of adult neck pain – A systematic review and meta-analysis, Musculoskeletal Science and Practice, Volume 31, October 2017, Pages 62-71
- ↑ Anita AR et al. A Cochrane Review of Manipulation and Mobilization for Mechanical Neck Disorders. Spine. 2004; 29(14): 1541-1548
- ↑ Cross KM, Kuenze C, Grindstaff TL, Hertel J.Thoracic spine thrust manipulation improves pain, range of motion, and self-reported function in patients with mechanical neck pain: a systematic review.J Orthop Sports Phys Ther. 2011 Sep;41(9):633-42.
- ↑ Rushton A, Rivett D, Carlesso L, Flynn T, Hing W, Kerry R. International Framework for Examination of the Cervical Region http://www.physio-pedia.com/Section_5:_Physical_examination
- ↑ Fritz JM, Thackeray A, Brennan GP, Childs JD.Exercise only, exercise with mechanical traction, or exercise with over-door traction for patients with cervical radiculopathy, with or without consideration of status on a previously described subgrouping rule: a randomized clinical trial. J Orthop Sports Phys Ther. 2014 Feb;44(2):45-57.
- ↑ Jellad A, Ben Salah Z, Boudokhane S, Migaou H, Bahri I, Rejeb N.The value of intermittent cervical traction in recent cervical radiculopathy.Ann Phys Rehabil Med. 2009 Nov;52(9):638-52.
- ↑ Boyles R. Toy P. Mellon J. Hayes M.Hammer B. Effectiveness of manual physical therapy in the treatment of cervical radiculopathy a systematic review. Journal of Manipulative therapy. 19 (3) 2011
- ↑ 47.0 47.1 Ragonese J. A randomized trial comparing manual physical therapy to therapeutic exercises, to a combination of therapies,for the treatment of cervical radiculopathy. Orthop Prac 2009;21(3):71–7.
- ↑ 48.0 48.1 Cleland JA, Whitman JM, Fritz JM, Palmer JA. Manual physical therapy, cervical traction, and strengthening exercises in patients with cervical radiculopathy: a case series. J Ortho Sports Phys Ther 2005;35:802–11.
- ↑ Franke H, Fryer G, Ostelo RW, Kamper SJ .Muscle energy technique for non-specific low-back pain. Cochrane Database Syst Rev. 2015 Feb 27;2:CD009852. LoE: 1A.
- ↑ Butler, 0 (1991). Mobilisation of the Nervous System, Churchill Livingstone, Edinburgh
- ↑ Magee DJ. Orthopedic physical assessment. 5th ed. St. Louis,MO: Saunders Elsevier; 2008.
- ↑ Malanga G. Sherwin SW.Cervical Radiculopathy Treatment & Management 2013 [ONLINE]fckLRAvailable from http://emedicine.medscape.com/article/94118-treatment#aw2aab6b6b2
- ↑ Griffiths C, Dziedzic K, Waterfield J, Sim J. Effectiveness of specific neck stabilization exercises or a general neck exercise program for chronic neck disorders: a randomized controlled trial. J Rheumatol. Feb 2009;36(2):390-7
- ↑ Falla D, Lindstrøm R, Rechter L, Boudreau S, Petzke F. Effectiveness of an 8-week exercise programme on pain and specificity of neck muscle activity in patients with chronic neck pain: a randomized controlled study. Eur J Pain. 2013; 17: 1517– 1528. LoE: 1B
- ↑ Cleland JA, Fritz JM, Whitman JM, et al. Predictors of short-term outcomes in people with a clinical diagnosis of cervical radiculopathy. Phys Ther. 2007;87(12):1619-1632.
- ↑ Partanen J, Partanen K, Oikarinen H, et al. Preoperative electroneuromyography and myelography in cervical root compression. Electromyogr Clin Neurophysiol. 1991; 31:21-26.