Systemic Lupus Erythematosus: Difference between revisions
Lotte Vonck (talk | contribs) (level of evidence) |
Kim Jackson (talk | contribs) (Formatting and updating references) |
||
| Line 4: | Line 4: | ||
'''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}} - Elaine Lonnemann | '''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}} - Elaine Lonnemann | ||
</div> | </div> | ||
== Definition/Description | == Definition/Description == | ||
Lupus erythematosus is an autoimmune disease that can manifest itself in several different ways including: discoid lupus erythematosus (DLE), systemic lupus erythematosus (SLE), drug-induced lupus, late-state lupus, and antiphopholipid antibody syndrome. | Lupus erythematosus is an autoimmune disease that can manifest itself in several different ways including: discoid lupus erythematosus (DLE), systemic lupus erythematosus (SLE), drug-induced lupus, late-state lupus, and antiphopholipid antibody syndrome. Systemic lupus erythematosus (SLE) is a chronic, rheumatic, <u>inflammatory</u> disease that can affect a person’s skin, joints, kidneys, lungs, heart, nervous system, blood, and mucous membranes. It does not affect all patients in the same way, so patients experience variable organ involvement after being diagnosed with SLE.<ref name="Goodman et al">Goodman CC, Fuller KS. Pathology: Implications for the Physical Therapist. 3rd edition. St. Louis, Missouri: Saunders Elsevier, 2009. (Level of evidence 5)</ref> <ref name="Goodman cc et al">Goodman CC and Synder TK. Differential Diagnosis for Physical Therapists: Screening for Referral. 4th edition. St. Louis, Missouri: Saunders Elsevier, 2007.</ref> | ||
Systemic lupus erythematosus (SLE) is a chronic, rheumatic, <u>inflammatory</u> disease that can affect a person’s skin, joints, kidneys, lungs, heart, nervous system, blood, and mucous membranes. It does not affect all patients in the same way, so patients experience variable organ involvement after being diagnosed with SLE.<ref name="Goodman et al" /> <ref name="Goodman cc et al">Goodman CC and Synder TK. Differential Diagnosis for Physical Therapists: Screening for Referral. 4th edition. St. Louis, Missouri: Saunders Elsevier, 2007.</ref> | |||
== Prevalence == | == Prevalence == | ||
| Line 34: | Line 32: | ||
*Occurs in 10-20/100,000 children (depends on the population) | *Occurs in 10-20/100,000 children (depends on the population) | ||
*About 15% of people diagnosed with SLE are younger than 18 years old, and when a person is diagnosed at an early age, the disease progresses more quickly and severely than if diagnosed after the age of 18.<ref name="Tucker et al">Tucker LB. Making the diagnosis of systemic lupus erythematosus in children and adolescents. Lupus; 16: 546-549. 2007.</ref> | *About 15% of people diagnosed with SLE are younger than 18 years old, and when a person is diagnosed at an early age, the disease progresses more quickly and severely than if diagnosed after the age of 18.<ref name="Tucker et al">Tucker LB. Making the diagnosis of systemic lupus erythematosus in children and adolescents. Lupus; 16: 546-549. 2007.</ref> | ||
*More prevalent in those who have a family history of SLE than it is in the general population | *More prevalent in those who have a family history of SLE than it is in the general population<ref name="Goodman et al" /> | ||
< | == Pathological Process == | ||
The exact cause of SLE is unknown but research suggests that genetics may be a contributing factor, but not the only factor.<ref name=":0">[http://www.niams.nih.gov/health_info/Lupus/default.asp "Handout on Health: Systemic Lupus Erythematosus"]. ''www.niams.nih.gov''. June 2016.(Accessed 28 April 2019).</ref> Hormonal and environmental factors have also been identified as playing a role in the onset of the condition.<ref name=":0" /><ref name=":1">Lisnevskaia, L., Murphy, G., & Isenberg, D. (2014). ''Systemic lupus erythematosus. The Lancet, 384(9957), 1878–1888.''</ref> The consensus however is that autoimmunity is thought to be the primary causative factor of SLE. The following are some of the factors that can predispose a person to SLE:<ref name=":1" /> | |||
*Heredity- There is a high prevalence of SLE in first-degree relatives. The immune abnormalities associated with SLE can be triggered by both internal and external factors. | |||
*Stress- It has been determined that stress can provoke changes in the neuroendocrine system causing changes in the function of immune system cells. | |||
*Smoking | |||
*Bacterial or viral infection- The Epstein-Barr virus has been found to be a risk factor for the development of SLE. | |||
*Sunlight or UV exposure | |||
*Immunizations | |||
*Pregnancy- The evidence about whether or not pregnancy can cause exacerbations of SLE is very inconclusive because some studies state that pregnancy does affect the course of SLE, while others state that it has no affect on the course of the disease. | |||
*Abnormal levels of estrogen | |||
*Certain drugs- Drugs such as hydralazin, anticonvulsants, penicillin, sulfa drugs, and oral contraceptives can change the cellular responsiveness and immunogenicity of self-antigens and therefore make a person more susceptible to SLE.<ref name="Goodman et al" /> | |||
*Biological agents | |||
*Pesticides | |||
*Phthalates (a chemical used to soften and increase the flexibility of plastics) | |||
Although the cause of this condition is unknown the process is fully understood "the body creates antibodies against its own cells." These antibodies can be formed against many different tissues and components of the body including red blood cells, neutrophils, platelets, lymphocytes. This accounts for the fact that SLE can affect almost any area of a person's body.<ref name="Goodman et al" /> | |||
= | === Systemic Involvement === | ||
== Systemic Involvement == | |||
There are many visceral systems can be affected from SLE, but the extent of the body's involvement differs from person to person. Some people diagnosed with SLE have only few visceral systems involved, while others have numerous systems that have been affected by the disease. | There are many visceral systems can be affected from SLE, but the extent of the body's involvement differs from person to person. Some people diagnosed with SLE have only few visceral systems involved, while others have numerous systems that have been affected by the disease. | ||
==== Musculoskeletal System: ==== | |||
*Arthritis- typically affects hand, wrists, and knees | *Arthritis- typically affects hand, wrists, and knees | ||
*Arthralgia | *Arthralgia | ||
| Line 143: | Line 63: | ||
*Ulnar drift | *Ulnar drift | ||
==== Cardiopulmonary/Cardiovascular System: ==== | |||
*Pleuritis | *Pleuritis | ||
*Pericarditis | *Pericarditis | ||
| Line 159: | Line 78: | ||
#Arterial Thrombosis | #Arterial Thrombosis | ||
==== Central Nervous System: ==== | |||
*Emotional instability | *Emotional instability | ||
*Psychosis | *Psychosis | ||
| Line 169: | Line 87: | ||
*Organic brain syndrome | *Organic brain syndrome | ||
==== Renal System: ==== | |||
*Glomerulonephritis -inflammatory disease of the kidneys | |||
*Glomerulonephritis | |||
*Hematuria | *Hematuria | ||
| Line 177: | Line 94: | ||
*Kidney failure<ref name="Goodman et al" /> | *Kidney failure<ref name="Goodman et al" /> | ||
==== Cutaneous System: ==== | |||
*Calcinosis | *Calcinosis | ||
*Cutaneous vasculitis | *Cutaneous vasculitis | ||
| Line 186: | Line 102: | ||
*Petechiae | *Petechiae | ||
==== Blood Disorders: ==== | |||
*Anemia | *Anemia | ||
*Thrombocytopenia | *Thrombocytopenia | ||
| Line 194: | Line 109: | ||
*Thrombosis | *Thrombosis | ||
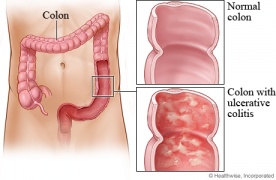
==== Gastrointestinal System: ==== | |||
[[Image:Ulcerative Colitis.jpg|right|276x180px|This picture was included courtesy of http://www.health.com]] | |||
*Ulcers--Throat & Mouth | *Ulcers--Throat & Mouth | ||
| Line 204: | Line 120: | ||
*Autoimmune Hepatitis <ref name="Lupus Foundation">Lupus Foundation of America. How lupus affects the body page. Website updated: 2010. Website accessed: February 17, 2010.</ref> | *Autoimmune Hepatitis <ref name="Lupus Foundation">Lupus Foundation of America. How lupus affects the body page. Website updated: 2010. Website accessed: February 17, 2010.</ref> | ||
== | == Clinical Presentation == | ||
[[Image:SLE rash.jpg|right|135x99px|This image illustrates the typical distribution pattern of the butterfly (malar) rash that can be a characteristic of SLE. This picture was included courtesy of: http://images.google.com.]]SLE can affect many organs of the body, but it rarely affects them all. The following list includes common signs and symptoms of SLE in order of the most to least prevalent. All of the below symptoms might not be present at the initial diagnosis of SLE, but as the disease progresses more of a person’s organ systems become involved.<ref name=":0" /> The most common symptoms associated with SLE are: | |||
*Constitutional symptoms (fever, malaise, fatigue, weight loss): most commonly fatigue and a low-grade fever | |||
*Achy joints (arthralgia) | |||
*Arthritis (inflamed joints) | |||
*Skin rashes | |||
*Pulmonary involvement (symptoms include: chest pain, difficulty breathing, and cough) | |||
*Anemia | |||
*Kidney involvement (lupus nephritis) | |||
*Sensitivity to the sun or light (photosensitivity) | |||
*Hair loss | |||
*Raynaud’s phenomenon | |||
*CNS involvement (seizures, headaches, peripheral neuropathy, cranial neuropathy, cerebrovascular accidents, organic brain syndrome, psychosis) | |||
*Mouth, nose, or vaginal ulcers”<ref name="Goodman et al" /> | |||
*The most common signs and symptoms of SLE in children and adolescents are: "fever, fatigue, weight loss, arthritis, rash, and renal disease."<ref name="Tucker et al" /> | |||
=== Associated Co-morbidities === | |||
< | *About 30% of people diagnosed with SLE are also diagnosed with fibromyalgia.<ref name="Goodman cc et al" /> | ||
*Atherosclerosis<ref name="Becker-Merok et al">Becker-Merok A, Nossent JC. Prevalence, predictors, and outcomes of vascular damamge in systemic lupus erythematosus. Lupus; 18: 508-515. 2009.</ref> <ref name="Bertsias et al">Bertsias G, Gordon C, Boumpas DT. Clinical trials in systemic lupus erythematosus (SLE): lessons from the past as we proceed to the future- the EULAR recommendations for the management of SLE and the use of end-points in clinical trials. Lupus; 17: 437-442. 2008.</ref> | |||
*Lupus Nephritis- leads to End Stage Renal Disease (ESRD) | |||
*Anemia<ref name="Windgard">Wingard R. Increased risk of anemia in dialysis patients with comorbid diseases. Nephrology Nursing Journal; 31 (2): 211-214. 2004.</ref> | |||
*Some types of cancers (especially non-Hodgkin's lymphoma and lung cancer) <ref name="Bertsias et al" /><ref name="Mayo Clinic" /> <ref name="Bernatsky - SLE">Bernatsky S, Boivin JF, Joseph L, et al. An international cohort study of cancer in systemic lupus erythematosus.Arthritis & Rheumatism 2005;52(5):1481–90.</ref> | |||
*Infections | |||
*Hypertension | |||
*Dyslipidemia | |||
*Diabetes Mellitus | |||
*Osteoporosis | |||
*Avascular Necrosis <ref name="Bertsias et al" /> | |||
*<br> | |||
== Diagnosis == | |||
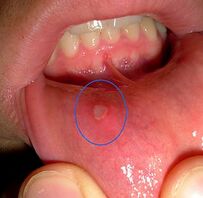
[[Image:Oral Ulcers.jpg|203x200px|This could be how an oral ulceration looks in a person with SLE. This image was included courtesy of http://www.thedailystar.net/photo.|right]]Because of the many different symptoms and manifestations of SLE early detection can often be difficult. According to the American Rheumatism Association, a patient must exhibit at least 4 of the following criteria concurrently or successively to be diagnosed with systemic lupus erythematosus. | |||
*Abnormal titer of antinuclear antibodies (ANAs) | |||
*Butterfly (malar) rash | |||
*Discoid rash | |||
*Hemolytic anemia, leukopenia, lymphopenia, thrombocytopenia | |||
*Neurologic disorder: seizures or psychosis | |||
*Non-erosive arthritis of two or more peripheral joints characterized by tenderness, swelling, or effusion | |||
*Oral or nasopharyngeal ulcerations [[Image:Discoid rash.png|right|198x249px|This is an illustration of a discoid rash that is characteristic of a patient with SLE. It is included in this project courtesy of www.googleimages.com]] | |||
*Photosensitivity | |||
*Pleuritis or pericarditis | |||
*Positive lupus erythematosus cell preparations, anti DNA, or anti-splice sosomal test or chronic false-positive serologic test for syphilis<span id="fck_dom_range_temp_1269546309419_582" /> | |||
*Renal disorder: profuse proteinuria (>0.5 grams/day) or excessive cellular casts in urine."<span style="display: none" id="1269546151699E"> </span><ref name="Goodman et al" /> | |||
''' | <br>Although laboratory tests along cannot diagnose SLE the following tests may show abnormal results if SLE is suspected: | ||
*Complete Blood Count: This blood test reveals a patient's total number of red blood cells, white blood cells, platelets, and hemoglobin. Low white blood cell or platelet counts can be indicative of SLE, whereas low red blood cell counts can be indicate of anemia which commonly occurs in conjunction with SLE. | |||
*Erythrocyte Sedimentation Rate: An elevated erythrocyte sedimentation rate can reveal a systemic problem. This test is not specific to SLE, but a postitive test could reveal that the patient could potentially have SLE. | |||
*Kidney and Liver Tests: These tests are completed to determine if a patient's kidneys and liver are functioning properly since SLE can affect these systemic organs. | |||
*Urinalysis: This test is performed to determine if there are proteins or red blood cells present in a patient's urine. If so, this could indicate that the kidneys are damaged, potentially from SLE. | |||
*ANA test: A positive test reveals that a patient could potentially have SLE, but other infections and diseases can cause this test to be positive as well. If positive, further testing is necessary to determine if the positive results occurred due to SLE. | |||
*Chest X-ray: This test is performed to determine if there is inflammation present in the patient's lungs or excessive fluid surrounding his/her heart. | |||
*Syphilis Test: A false-positive syphilis test can reveal that a patient has anti-phospholipids present, and this false-positive test result is indicative that the patient could have SLE.<ref name="Mayo Clinic">Medical Foundation for Medical Education and Research. Mayo Clinic: Lupus Page. www.mayoclinic.com. Updated October 20, 2009. Accessed February 17, 2010.</ref> <u></u><u></u> | |||
== Medical Management == | |||
'' | The medical management for SLE is primarily drug therapy and is based upon the patients symptoms and systemic involvement. The most widely used medications are: | ||
*[http://www.drugs.com/search.php?searchterm=analgesics&is_main_search=1 Analgesics][http://www.drugs.com/search.php?searchterm=analgesics&is_main_search=1]: These medications are used to control the pain associated with arthralgia, arthritis, and ulcers that are caused by SLE.<ref name="Laranzo et al" /> | |||
*[http://www.drugs.com/search.php?searchterm=Non-steroidal%20antiinflammatory%20&is_main_search=1 Non-Steroidal Anti-inflammatory Drugs (NSAIDS):] These medications help to decrease tissue inflammation, and therefore decrease the patient’s joint and muscle pain. | |||
*Anti-malarials: These medications are used to treat a patient's arthritic, musculocutaneous, and renal symptoms associated with SLE. <br> - [http://www.drugs.com/search.php?searchterm=Chloroquine%20&is_main_search=1 Chloroquine (Aralen)]<ref name="Goodman et al" /><ref name="Laranzo et al" /><br> - [http://www.drugs.com/search.php?searchterm=Hydroxychloroquine%20&is_main_search=1 Hydroxychloroquine (Plaquenil)]<ref name="Laranzo et al" /> | |||
*[http://www.drugs.com/search.php?searchterm=corticosteroids&is_main_search=1 Corticosteroids][http://www.drugs.com/search.php?searchterm=corticosteroids&is_main_search=1]: These drugs are only prescribed to patients with severe SLE who experience signs and symptoms that are not improving with any other drug therapy. Corticosteroids can give the patient relief from constitutional symptoms, arthritis, and cutaneous problems caused from SLE. | |||
*Immunosuppressant Agents: These drugs are used to decrease inflammation, treat lupus nephritis, and suppress the patient's immune system. <br> - [http://www.drugs.com/search.php?searchterm=Azathioprine%20&is_main_search=1 Azathioprine (Imuran)]<br> - [http://www.drugs.com/search.php?searchterm=Cyclophosphamide%20&is_main_search=1 Cyclophosphamide (Cytoxan)]<ref name="Goodman et al" /><ref name="Laranzo et al" /> | |||
*Topical medications | |||
In addition to drug therapy, prevention is also very important when dealing with SLE. For patients with photosensitivities, flare-ups can be reduced if patients are cautious about the amount of sunlight or UV light that they are exposed to. Patients with SLE are also encouraged to lead a healthy lifestyle that includes: smoking cessation, controlling alcohol consumption, weight management, and regular exercise.<ref name="Goodman et al" /><ref name="Bertsias et al" /> Patients with SLE are also encouraged to participate in support groups, ensure they are taking the correct dosages and amounts of medications, and ensure they visit medical professionals regularly.<ref name="Goodman et al" /> There are also other therapies that claim to have a positive effect on symptoms, such as: | |||
* Hormonal Intervention | |||
* Immunosupressant Therapy | |||
* IV Gamma Globulin | |||
* Apheresis | |||
* Stem-Cell Transplantation | |||
* Biological Therapy<ref name="Solsky SLE Treatment">Solsky M, Wallace D. New therapies in systemic lupus erythematosus. Best Practice & Res Clin Rheum: 2002; 16; 293-312</ref> | |||
== Physical Therapy Management == | |||
Exercise is beneficial for patients with SLE because it decreases their muscle weakness while simultaneously increases their muscle endurance. Physical therapists can play an important role for patients with SLE during and between exacerbations. The patient's need for physical therapy will vary greatly depending on the systems involved. | |||
*Education: It is essential for patients with skin lesions to have appropriate education on the best way to care for their skin and to ensure they do not experience additional skin breakdown. | |||
*Aerobic Exercise: One of the most common impairments that patients with SLE experience is generalized fatigue that can limit their activities throughout the day.<ref name="Goodman et al" /> In a study by Tench et al., it was determined that graded aerobic exercise programs are more successful than relaxation techniques in decreasing the fatigue levels of patients with SLE. Aerobic activity caused many of the participants with SLE to feel "much better" or "very much better" at the conclusion of the study. The aerobic exercise program consisted of 30-50 minutes of aerobic activity (walking/swimming/cycling) with a heart rate corresponding to 60% of the patient's peak oxygen consumption.<ref name="Tench et al">Tench CM, McCarthy J, McCurdie I, White PD, D'Cruz DP. Fatigue in systemic lupus erythematosus: a randomized control trial of exercise. Rheumatology; 42: 1050-1054. 2003. (Level of evidence 1B)</ref> Another study, completed by Ramsey- Goldman et al., concluded that both aerobic exercise and range of motion/muscle strengthening exercises can increase the energy level, cardiovascular fitness, functional status, and muscle strength in patients with SLE. In this study, the patients completed aerobic exercise for 20-30 minutes at 70-80% of their maximum heart rate. The patients who completed range of motion and muscle strengthening activities met 3 times a week for 50 minutes sessions.<ref name="Ramsey-Goldman et al">Ramsey-Goldman GR, Schilling EM, Dunlop D, Langman C, Greenland P, Thomas RJ, Chang RW. A pilot study on the effects of exercise in patients with systemic lupus erythematosus. Arthritis Care and Research; 13(5): 262-269. 2000. (Level of evidence 2B)</ref> | |||
* | *Energy Conservation: Physical therapists can educate patients on appropriate energy conservation techniques and the best ways to protect joints that are susceptible to damage. | ||
* | *Additionally, physical therapists and patients with SLE should be aware of signs and symptoms that suggest a progression of SLE including those associated with avascular necrosis, kidney involvement, and neurological involvement.<ref name="Goodman et al" /> | ||
* | |||
*Additionally, physical therapists and patients with SLE should be aware of signs and symptoms that suggest a progression of SLE including those associated with avascular necrosis, kidney involvement, and neurological involvement.<ref name="Goodman et al" /> | |||
== Differential Diagnosis == | == Differential Diagnosis == | ||
{| border="1" cellspacing="1" cellpadding="1" width="220" align="center" | {| border="1" cellspacing="1" cellpadding="1" width="220" align="center" | ||
|+ + [http://www.rheumatology.org/publications/classification/SLE/sle.asp?aud=mem ACR Diagnostic Criteria SLE] | |+ + [http://www.rheumatology.org/publications/classification/SLE/sle.asp?aud=mem ACR Diagnostic Criteria SLE] | ||
| Line 291: | Line 257: | ||
Vasculitis <ref name="Tucker et al" /> | Vasculitis <ref name="Tucker et al" /> | ||
[[MS Multiple Sclerosis|Multiple Sclerosis]] <ref name="Bhiglee et al">Bhiglee AI, Bill PL. Case Report: Multiple sclerosis and SLE revisited. Medical Journal of Islamic Academy of Sciences; 12 (3): 79-84. 1999.</ref> | [[MS Multiple Sclerosis|Multiple Sclerosis]] <ref name="Bhiglee et al">Bhiglee AI, Bill PL. Case Report: Multiple sclerosis and SLE revisited. Medical Journal of Islamic Academy of Sciences; 12 (3): 79-84. 1999.</ref><div class="researchbox"></div> | ||
== Resources == | |||
<div class="researchbox" | |||
== Resources | |||
Lupus Foundation of America [http://www.lupus.org www.lupus.org] | |||
Medline Plus: Lupus http://www.nlm.nih.gov/medlineplus/lupus.html | |||
WebMD: Lupus http://lupus.webmd.com/ | |||
== References == | == References == | ||
| Line 319: | Line 272: | ||
<span style="line-height: 1.5em;"> </span><span style="line-height: 1.5em;"> </span> | <span style="line-height: 1.5em;"> </span><span style="line-height: 1.5em;"> </span> | ||
[[Category:Rheumatology]] [[Category:Autoimmune_Disorders]] [[Category:Videos]] [[Category:Bellarmine_Student_Project]] | [[Category:Rheumatology]] | ||
[[Category:Autoimmune_Disorders]] | |||
[[Category:Videos]] | |||
[[Category:Bellarmine_Student_Project]] | |||
Revision as of 21:56, 28 April 2019
Original Editors - Alli Christian from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Alli Christian, Elaine Lonnemann, Admin, Kim Jackson, Lucinda hampton, Rachael Lowe, Lotte Vonck, Khloud Shreif, 127.0.0.1, WikiSysop, Laura Ritchie and Wendy Walker - Elaine Lonnemann
Definition/Description[edit | edit source]
Lupus erythematosus is an autoimmune disease that can manifest itself in several different ways including: discoid lupus erythematosus (DLE), systemic lupus erythematosus (SLE), drug-induced lupus, late-state lupus, and antiphopholipid antibody syndrome. Systemic lupus erythematosus (SLE) is a chronic, rheumatic, inflammatory disease that can affect a person’s skin, joints, kidneys, lungs, heart, nervous system, blood, and mucous membranes. It does not affect all patients in the same way, so patients experience variable organ involvement after being diagnosed with SLE.[1] [2]
Prevalence[edit | edit source]
| 20/100,000 | World Prevalence |
| 9:1 | Female: Male |
| Ages of Diagnosis | 15-40 Years |
- Occurs in 15-24/100,000 people throughout the world[3]
- Large variation depending on country and location--high prevalence in Sweden. 14.6/100,000 in NY vs 78.5/100,000 in WI
- Most likely to occur in women of child-bearing age
- More common in those of African American, Hispanic, Asian, and Native American decent than in Caucasians[1]
- 9 times more likely in women compared to men[4]
- Most people are diagnosed with the disease between the ages of 15 and 40[2]
- Rarely diagnosed in the elderly [3]
- Occurs in 10-20/100,000 children (depends on the population)
- About 15% of people diagnosed with SLE are younger than 18 years old, and when a person is diagnosed at an early age, the disease progresses more quickly and severely than if diagnosed after the age of 18.[5]
- More prevalent in those who have a family history of SLE than it is in the general population[1]
Pathological Process[edit | edit source]
The exact cause of SLE is unknown but research suggests that genetics may be a contributing factor, but not the only factor.[6] Hormonal and environmental factors have also been identified as playing a role in the onset of the condition.[6][7] The consensus however is that autoimmunity is thought to be the primary causative factor of SLE. The following are some of the factors that can predispose a person to SLE:[7]
- Heredity- There is a high prevalence of SLE in first-degree relatives. The immune abnormalities associated with SLE can be triggered by both internal and external factors.
- Stress- It has been determined that stress can provoke changes in the neuroendocrine system causing changes in the function of immune system cells.
- Smoking
- Bacterial or viral infection- The Epstein-Barr virus has been found to be a risk factor for the development of SLE.
- Sunlight or UV exposure
- Immunizations
- Pregnancy- The evidence about whether or not pregnancy can cause exacerbations of SLE is very inconclusive because some studies state that pregnancy does affect the course of SLE, while others state that it has no affect on the course of the disease.
- Abnormal levels of estrogen
- Certain drugs- Drugs such as hydralazin, anticonvulsants, penicillin, sulfa drugs, and oral contraceptives can change the cellular responsiveness and immunogenicity of self-antigens and therefore make a person more susceptible to SLE.[1]
- Biological agents
- Pesticides
- Phthalates (a chemical used to soften and increase the flexibility of plastics)
Although the cause of this condition is unknown the process is fully understood "the body creates antibodies against its own cells." These antibodies can be formed against many different tissues and components of the body including red blood cells, neutrophils, platelets, lymphocytes. This accounts for the fact that SLE can affect almost any area of a person's body.[1]
Systemic Involvement[edit | edit source]
There are many visceral systems can be affected from SLE, but the extent of the body's involvement differs from person to person. Some people diagnosed with SLE have only few visceral systems involved, while others have numerous systems that have been affected by the disease.
Musculoskeletal System:[edit | edit source]
- Arthritis- typically affects hand, wrists, and knees
- Arthralgia
- Tenosynovitis
- Tendon ruptures
- Swan-neck deformity
- Ulnar drift
Cardiopulmonary/Cardiovascular System:[edit | edit source]
- Pleuritis
- Pericarditis
- Dyspnea
- Hypertension
- Myocarditis
- Endocarditis
- Tachycarditis
- Pneumonitis
- Vasculitis
- Small Vessels Purpura
- Large Vessels Papular Lesions
- Arterial Thrombosis
Central Nervous System:[edit | edit source]
- Emotional instability
- Psychosis
- Seizures
- Cerebrovascular accidents
- Cranial neuropathy
- Peripheral neuropathy
- Organic brain syndrome
Renal System:[edit | edit source]
- Glomerulonephritis -inflammatory disease of the kidneys
- Hematuria
- Proteinuria
- Kidney failure[1]
Cutaneous System:[edit | edit source]
- Calcinosis
- Cutaneous vasculitis
- Hair loss
- Raynaud's phenomenon
- Mucosal ulcers
- Petechiae
Blood Disorders:[edit | edit source]
- Anemia
- Thrombocytopenia
- Leukopenia
- Neutropenia
- Thrombosis
Gastrointestinal System:[edit | edit source]
- Ulcers--Throat & Mouth
- Ulcerative colitis/Crohn's disease
- Peritonitis
- Ascites
- Pancreatitis
- Peptic ulcers
- Autoimmune Hepatitis [8]
Clinical Presentation [edit | edit source]
SLE can affect many organs of the body, but it rarely affects them all. The following list includes common signs and symptoms of SLE in order of the most to least prevalent. All of the below symptoms might not be present at the initial diagnosis of SLE, but as the disease progresses more of a person’s organ systems become involved.[6] The most common symptoms associated with SLE are:
- Constitutional symptoms (fever, malaise, fatigue, weight loss): most commonly fatigue and a low-grade fever
- Achy joints (arthralgia)
- Arthritis (inflamed joints)
- Skin rashes
- Pulmonary involvement (symptoms include: chest pain, difficulty breathing, and cough)
- Anemia
- Kidney involvement (lupus nephritis)
- Sensitivity to the sun or light (photosensitivity)
- Hair loss
- Raynaud’s phenomenon
- CNS involvement (seizures, headaches, peripheral neuropathy, cranial neuropathy, cerebrovascular accidents, organic brain syndrome, psychosis)
- Mouth, nose, or vaginal ulcers”[1]
- The most common signs and symptoms of SLE in children and adolescents are: "fever, fatigue, weight loss, arthritis, rash, and renal disease."[5]
Associated Co-morbidities[edit | edit source]
- About 30% of people diagnosed with SLE are also diagnosed with fibromyalgia.[2]
- Atherosclerosis[9] [10]
- Lupus Nephritis- leads to End Stage Renal Disease (ESRD)
- Anemia[11]
- Some types of cancers (especially non-Hodgkin's lymphoma and lung cancer) [10][12] [13]
- Infections
- Hypertension
- Dyslipidemia
- Diabetes Mellitus
- Osteoporosis
- Avascular Necrosis [10]
Diagnosis[edit | edit source]
Because of the many different symptoms and manifestations of SLE early detection can often be difficult. According to the American Rheumatism Association, a patient must exhibit at least 4 of the following criteria concurrently or successively to be diagnosed with systemic lupus erythematosus.
- Abnormal titer of antinuclear antibodies (ANAs)
- Butterfly (malar) rash
- Discoid rash
- Hemolytic anemia, leukopenia, lymphopenia, thrombocytopenia
- Neurologic disorder: seizures or psychosis
- Non-erosive arthritis of two or more peripheral joints characterized by tenderness, swelling, or effusion
- Oral or nasopharyngeal ulcerations
- Photosensitivity
- Pleuritis or pericarditis
- Positive lupus erythematosus cell preparations, anti DNA, or anti-splice sosomal test or chronic false-positive serologic test for syphilis<span id="fck_dom_range_temp_1269546309419_582" />
- Renal disorder: profuse proteinuria (>0.5 grams/day) or excessive cellular casts in urine."[1]
Although laboratory tests along cannot diagnose SLE the following tests may show abnormal results if SLE is suspected:
- Complete Blood Count: This blood test reveals a patient's total number of red blood cells, white blood cells, platelets, and hemoglobin. Low white blood cell or platelet counts can be indicative of SLE, whereas low red blood cell counts can be indicate of anemia which commonly occurs in conjunction with SLE.
- Erythrocyte Sedimentation Rate: An elevated erythrocyte sedimentation rate can reveal a systemic problem. This test is not specific to SLE, but a postitive test could reveal that the patient could potentially have SLE.
- Kidney and Liver Tests: These tests are completed to determine if a patient's kidneys and liver are functioning properly since SLE can affect these systemic organs.
- Urinalysis: This test is performed to determine if there are proteins or red blood cells present in a patient's urine. If so, this could indicate that the kidneys are damaged, potentially from SLE.
- ANA test: A positive test reveals that a patient could potentially have SLE, but other infections and diseases can cause this test to be positive as well. If positive, further testing is necessary to determine if the positive results occurred due to SLE.
- Chest X-ray: This test is performed to determine if there is inflammation present in the patient's lungs or excessive fluid surrounding his/her heart.
- Syphilis Test: A false-positive syphilis test can reveal that a patient has anti-phospholipids present, and this false-positive test result is indicative that the patient could have SLE.[12]
Medical Management[edit | edit source]
The medical management for SLE is primarily drug therapy and is based upon the patients symptoms and systemic involvement. The most widely used medications are:
- Analgesics[1]: These medications are used to control the pain associated with arthralgia, arthritis, and ulcers that are caused by SLE.[3]
- Non-Steroidal Anti-inflammatory Drugs (NSAIDS): These medications help to decrease tissue inflammation, and therefore decrease the patient’s joint and muscle pain.
- Anti-malarials: These medications are used to treat a patient's arthritic, musculocutaneous, and renal symptoms associated with SLE.
- Chloroquine (Aralen)[1][3]
- Hydroxychloroquine (Plaquenil)[3] - Corticosteroids[2]: These drugs are only prescribed to patients with severe SLE who experience signs and symptoms that are not improving with any other drug therapy. Corticosteroids can give the patient relief from constitutional symptoms, arthritis, and cutaneous problems caused from SLE.
- Immunosuppressant Agents: These drugs are used to decrease inflammation, treat lupus nephritis, and suppress the patient's immune system.
- Azathioprine (Imuran)
- Cyclophosphamide (Cytoxan)[1][3] - Topical medications
In addition to drug therapy, prevention is also very important when dealing with SLE. For patients with photosensitivities, flare-ups can be reduced if patients are cautious about the amount of sunlight or UV light that they are exposed to. Patients with SLE are also encouraged to lead a healthy lifestyle that includes: smoking cessation, controlling alcohol consumption, weight management, and regular exercise.[1][10] Patients with SLE are also encouraged to participate in support groups, ensure they are taking the correct dosages and amounts of medications, and ensure they visit medical professionals regularly.[1] There are also other therapies that claim to have a positive effect on symptoms, such as:
- Hormonal Intervention
- Immunosupressant Therapy
- IV Gamma Globulin
- Apheresis
- Stem-Cell Transplantation
- Biological Therapy[14]
Physical Therapy Management[edit | edit source]
Exercise is beneficial for patients with SLE because it decreases their muscle weakness while simultaneously increases their muscle endurance. Physical therapists can play an important role for patients with SLE during and between exacerbations. The patient's need for physical therapy will vary greatly depending on the systems involved.
- Education: It is essential for patients with skin lesions to have appropriate education on the best way to care for their skin and to ensure they do not experience additional skin breakdown.
- Aerobic Exercise: One of the most common impairments that patients with SLE experience is generalized fatigue that can limit their activities throughout the day.[1] In a study by Tench et al., it was determined that graded aerobic exercise programs are more successful than relaxation techniques in decreasing the fatigue levels of patients with SLE. Aerobic activity caused many of the participants with SLE to feel "much better" or "very much better" at the conclusion of the study. The aerobic exercise program consisted of 30-50 minutes of aerobic activity (walking/swimming/cycling) with a heart rate corresponding to 60% of the patient's peak oxygen consumption.[15] Another study, completed by Ramsey- Goldman et al., concluded that both aerobic exercise and range of motion/muscle strengthening exercises can increase the energy level, cardiovascular fitness, functional status, and muscle strength in patients with SLE. In this study, the patients completed aerobic exercise for 20-30 minutes at 70-80% of their maximum heart rate. The patients who completed range of motion and muscle strengthening activities met 3 times a week for 50 minutes sessions.[16]
- Energy Conservation: Physical therapists can educate patients on appropriate energy conservation techniques and the best ways to protect joints that are susceptible to damage.
- Additionally, physical therapists and patients with SLE should be aware of signs and symptoms that suggest a progression of SLE including those associated with avascular necrosis, kidney involvement, and neurological involvement.[1]
Differential Diagnosis[edit | edit source]
| > 4 Present 96% Sensitive; 96% Specific[17] |
|
Diagnostic Procedures[edit | edit source]
if the ANA test is negative, unlikely to have the diagnosis of SLE
the Lupus Band Test can assist in confirming the diagnosis of SLE with inconsistent clnical findings and can assist in excluding diseases similiar to SLE[18] [19]
sensitivity: 93% specificity:87%
PPV: 64% NPV: 98%
Other Differential Diagnoses
Fibromyalgia
Undifferentiated Connective Tissue Disease
Auto-immune Rheumatic Disease
Viral Infections-Epstein-Barr, Cytomegalovirus
Bacterial Infections
HIV
TB
Malignancies
Vasculitis [5]
Resources[edit | edit source]
Lupus Foundation of America www.lupus.org
Medline Plus: Lupus http://www.nlm.nih.gov/medlineplus/lupus.html
WebMD: Lupus http://lupus.webmd.com/
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 Goodman CC, Fuller KS. Pathology: Implications for the Physical Therapist. 3rd edition. St. Louis, Missouri: Saunders Elsevier, 2009. (Level of evidence 5)
- ↑ 2.0 2.1 2.2 Goodman CC and Synder TK. Differential Diagnosis for Physical Therapists: Screening for Referral. 4th edition. St. Louis, Missouri: Saunders Elsevier, 2007.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Laranzo D. Elderly-onset systemic lupus erythematosus. Drugs and Aging; 24 (9):701-715. 2007.
- ↑ O'Neill S, Cervera R. systemic Lupus Erythematosus. Best Practice & Res Clin Rheu 24 (2010) 841-855
- ↑ 5.0 5.1 5.2 Tucker LB. Making the diagnosis of systemic lupus erythematosus in children and adolescents. Lupus; 16: 546-549. 2007.
- ↑ 6.0 6.1 6.2 "Handout on Health: Systemic Lupus Erythematosus". www.niams.nih.gov. June 2016.(Accessed 28 April 2019).
- ↑ 7.0 7.1 Lisnevskaia, L., Murphy, G., & Isenberg, D. (2014). Systemic lupus erythematosus. The Lancet, 384(9957), 1878–1888.
- ↑ Lupus Foundation of America. How lupus affects the body page. Website updated: 2010. Website accessed: February 17, 2010.
- ↑ Becker-Merok A, Nossent JC. Prevalence, predictors, and outcomes of vascular damamge in systemic lupus erythematosus. Lupus; 18: 508-515. 2009.
- ↑ 10.0 10.1 10.2 10.3 Bertsias G, Gordon C, Boumpas DT. Clinical trials in systemic lupus erythematosus (SLE): lessons from the past as we proceed to the future- the EULAR recommendations for the management of SLE and the use of end-points in clinical trials. Lupus; 17: 437-442. 2008.
- ↑ Wingard R. Increased risk of anemia in dialysis patients with comorbid diseases. Nephrology Nursing Journal; 31 (2): 211-214. 2004.
- ↑ 12.0 12.1 Medical Foundation for Medical Education and Research. Mayo Clinic: Lupus Page. www.mayoclinic.com. Updated October 20, 2009. Accessed February 17, 2010.
- ↑ Bernatsky S, Boivin JF, Joseph L, et al. An international cohort study of cancer in systemic lupus erythematosus.Arthritis & Rheumatism 2005;52(5):1481–90.
- ↑ Solsky M, Wallace D. New therapies in systemic lupus erythematosus. Best Practice & Res Clin Rheum: 2002; 16; 293-312
- ↑ Tench CM, McCarthy J, McCurdie I, White PD, D'Cruz DP. Fatigue in systemic lupus erythematosus: a randomized control trial of exercise. Rheumatology; 42: 1050-1054. 2003. (Level of evidence 1B)
- ↑ Ramsey-Goldman GR, Schilling EM, Dunlop D, Langman C, Greenland P, Thomas RJ, Chang RW. A pilot study on the effects of exercise in patients with systemic lupus erythematosus. Arthritis Care and Research; 13(5): 262-269. 2000. (Level of evidence 2B)
- ↑ Hochberg MC. Updating the American College of Rehumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis and Rheumatism 1997; 40: 1725-1734
- ↑ George R, Kurian S, jacob M, Thomas K. Diagnostic evaluation of the lupus band test in discoid and systemic lupus erythematosus. Int J Dermatol. 1995 34: 170-173
- ↑ Mehta V, Sarda A, Balachandran C. Lupus band test. Indian J Dermatol Venereol Leprol [serial online] 2010 [cited 2012 Mar 6];76:298-300. Available from: http://www.ijdvl.com/text.asp?2010/76/3/298/62983
- ↑ Bhiglee AI, Bill PL. Case Report: Multiple sclerosis and SLE revisited. Medical Journal of Islamic Academy of Sciences; 12 (3): 79-84. 1999.