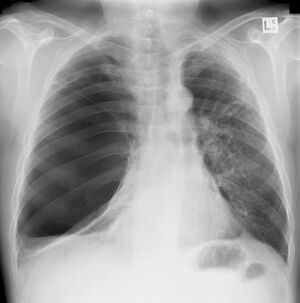
Pulmonary Bullae
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton
Introduction[edit | edit source]
A pulmonary bulla is an air-filled space, greater than 1 cm in diameter, that develops within the lung due to emphysematous damage of the lung. Pulmonary emphysema itself causes destruction of the distal lung design with lasting expansion of the alveolar space distal to the terminal bronchiole. Significantly 80% percent of patients presenting with bullae suffer from emphysema, a subset of chronic obstructive pulmonary disease (COPD).
Pathology[edit | edit source]
The development of lung bullae is heterogenis.
- Most commonly they are COPD-related emphysematous bullae,
- Pulmonary bulla may adjoin primary lung cancer and usually the prognosis is poor, no mater the size.[1]
- Primary spontaneous pneumothoraces (a pneumothorax without underlying lung disease), occur in those under 35 , (predominantly occurs in young, thin males). secondary spontaneous pneumothoraces occur usually in patients over 45[2].
- Ventilator-associated lung bullae are a rarity.
Treatment[edit | edit source]
Management options are manifold, for example; simply treating the underlying disease; ventilation strategies to prevent progression of the bullous lung disease; bronchoscopic intervention; when medical management is not enough, surgery is an option eg lung volume reduction surgery (LVRS) and lung transplantation. Finding from research indicate that elastic recoil of the lungs can improve post LVRS, improving the lungs functional expiratory airflow.[3][4]
Physiotherapy[edit | edit source]
Treatment will involve a respiratory/physiotherapist therapists. Physiotherapy management for pulmonary bullae is commonly associated with similar management of COPD.
- Clients need to be educated on the correct use of inhaler and the use of spacers in conjunction with inhalers.
- Pulmonary rehabilitation is also an important element of treatment.
- Telehealth may have a role as a cost-effectiveness resource, however this still requires further evaluation.[4]
References[edit | edit source]
- ↑ Kaneda M, Tarukawa T, Watanabe F, Adachi K, Sakai T, Nakabayashi H. Clinical features of primary lung cancer adjoining pulmonary bulla. Interactive CardioVascular and Thoracic Surgery. 2010 Jun 1;10(6):940-4.Available: https://academic.oup.com/icvts/article/10/6/940/776078?login=false#102034279 (accessed 28.4.2023)
- ↑ Luh SP. Diagnosis and treatment of primary spontaneous pneumothorax. Journal of Zhejiang University SCIENCE B. 2010 Oct;11:735-44.Available: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2950234/(accessed 29.4.2023)
- ↑ Ruan SY, Huang CT, Chien JY, Kuo YW, Yu CJ. Non-surgical management of giant lung bullae during mechanical ventilation. Respiratory care. 2011 Oct 1;56(10):1614-6.Available:https://rc.rcjournal.com/content/56/10/1614 (accessed 28.4.2023)
- ↑ 4.0 4.1 Siddiqui NA, Mansour MK, Nookala V. Bullous emphysema. InStatPearls [Internet] 2021 Jul 26. StatPearls Publishing.Available:https://www.ncbi.nlm.nih.gov/books/NBK537243/ (accessed 28.4.2023)