Platelet-Rich Plasma (PRP) Therapy
Original Editor - Patti Cavaleri
Top Contributors - Patti Cavaleri, Aminat Abolade and Candace Goh
Description
[edit | edit source]
Platelet-rich plasma (PRP) is a type of cellular therapy that falls under regenerative medicine. There has been growing interest and research in using PRP injections to treat pain and promote tissue healing for musculoskeletal conditions, as well as skin rejuvenation, treatment for hair loss, breast augmentation, and wound rejuvenation[1][2]. The addition of PRP to a site is believed to initiate tissue repair through a natural healing response to tissue stimulation, synthesis of new connective tissues, and revascularisation. Due to the use of autologous blood, there are limited adverse reactions compared to other injection-based therapies, such as corticosteroid injections[1].
PRP is typically classified into 3 groups[1]:
- Pure platelet-rich fibrin (P-PRF)
- Leukocyte-rich PRP (LR-PRP): pro-inflammatory with high concentration of growth factors[3]
- Leukocyte-poor PRP (LP-PRP): anti-inflammatory[3]
Indication
[edit | edit source]
Some studies have found PRP to be more beneficial in the treatment of osteoarthritis (OA) compared to saline, hyaluronic acid, or corticosteroids[2]. Tendinopathy disorders that have also demonstrated good results from PRP in clinical trials for rotator cuff disorders, gluteal tendinopathy, and lateral epicondylalgia[2].
Achilles Tendinopathy: A 2019 meta-analysis assessed 5 randomised controlled trials that examined the effect of PRP on Achilles tendinopathy compared to placebo treatment. The only significant difference was found at 6 weeks post-treatment for higher function in the PRP group compared to the placebo group. However, further follow-ups showed no significant difference between groups[4].
Knee Osteoarthritis: A 2019 systematic review and meta-analysis examined the effects of PRP and hyaluronic acid treatments in knee OA[3]. The review compared 18 randomised controlled trials. The PRP groups found larger improvements in short term and long term outcome measures compared to the hyaluronic acid groups. The amount of injections and formulas used varied between trials. LP-PRP injections are recommended in some systematic reviews as the preferred type of injection[1].
A randomised controlled trial was done in Australia to evaluate the effects of intra-articular PRP injections on symptoms and joint structure in 288 patients with symptomatic mild to moderate radiographic medial knee OA [5]. The findings did not support the use of PRP for the management of knee OA. In patients experiencing mild to moderate knee osteoarthritis with symptoms, the injection of platelet-rich plasma (PRP) into the joint, when compared to a saline placebo injection, did not lead to a notable disparity in symptoms or the condition of the joint after 12 months.
Ankle Osteoarthritis: A randomised controlled trial was done in 2018-2020 in the Netherlands to investigate the effects of intra-articular PRP injections on improving ankle symptoms and function in 100 patients with ankle osteoarthritis. The study found that intra-articular PRP injections, compared with placebo injections, did not significantly improve ankle symptoms and function over 26 weeks [6].
Lateral Epicondylalgia: Randomised control trials show better improvements in pain and function for long term results from PRP injections compared to steroid injections[7].
Ulnar Collateral Ligament Tear (UCL): Partial and complete tears of the UCL are commonly seen in overhead athlete sports, such as baseball. Case series report good functional outcomes and return to sport with the combination of PRP and physical therapies[8].
Contraindications[edit | edit source]
Contraindications for PRP therapy include[7]:
- Immunocompromised state
- Active infection
- Inability to understand and comply with post-procedure modifications
- Coagulopathy or anticoagulation
- Prosthetic joints
- Prosthetic hardware infection
- Severe cases of advanced OA
Procedure[edit | edit source]
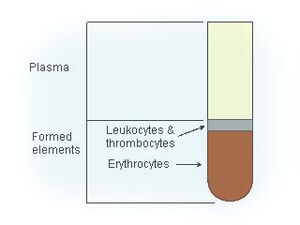
For the procedure, blood is collected from a patient and placed into a centrifuge to separate the blood into its components. A portion of the sample is then injected into the targeted site. There is not currently a recognized standard for the ideal formula of PRP, platelets, white blood cells, and other growth factors in the final concentration used[2].
Post-Procedure[edit | edit source]
Depending on the location of the PRP injection, physicians may have a specific post-procedure protocol depending on the location and type of injection. This can include periods of immobilization or altered weight-bearing status before gradual progression back to function and/or sport. Post-procedure protocols have not been addressed in the available research.
Patients may be recommended to stop taking NSAIDS in the initial post-procedure healing phase to not hinder the pro-inflammatory goal of PRP injections.[7]
Resources
[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Everts P, Onishi K, Jayaram P, Lana JF, Mautner K. Platelet-rich plasma: new performance understandings and therapeutic considerations in 2020. International journal of molecular sciences. 2020 Oct 21;21(20):7794.
- ↑ 2.0 2.1 2.2 2.3 Samadi P, Sheykhhasan M, Khoshinani HM. The use of platelet-rich plasma in aesthetic and regenerative medicine: a comprehensive review. Aesthetic plastic surgery. 2019 Jun 15;43:803-14.
- ↑ 3.0 3.1 3.2 Belk JW, Kraeutler MJ, Houck DA, Goodrich JA, Dragoo JL, McCarty EC. Platelet-rich plasma versus hyaluronic acid for knee osteoarthritis: a systematic review and meta-analysis of randomized controlled trials. The American journal of sports medicine. 2021 Jan;49(1):249-60.
- ↑ Liu CJ, Yu KL, Bai JB, Tian DH, Liu GL. Platelet-rich plasma injection for the treatment of chronic Achilles tendinopathy: a meta-analysis. Medicine. 2019 Apr;98(16).
- ↑ Bennell KL, Paterson KL, Metcalf BR, Duong V, Eyles J, Kasza J, Wang Y, Cicuttini F, Buchbinder R, Forbes A, Harris A. Effect of intra-articular platelet-rich plasma vs placebo injection on pain and medial tibial cartilage volume in patients with knee osteoarthritis: the RESTORE randomized clinical trial. Jama. 2021 Nov 23;326(20).
- ↑ Paget LD, Reurink G, de Vos RJ, Weir A, Moen MH, Bierma-Zeinstra SM, Stufkens SA, Kerkhoffs GM, Tol JL, Goedegebuure S, Krips R. Effect of platelet-rich plasma injections vs placebo on ankle symptoms and function in patients with ankle osteoarthritis: a randomized clinical trial. Jama. 2021 Oct 26;326(16):1595-605.
- ↑ 7.0 7.1 7.2 Peter I, Wu K, Diaz R, Borg-Stein J. Platelet-rich plasma. Physical Medicine and Rehabilitation Clinics. 2016 Nov 1;27(4):825-53.
- ↑ Mlynarek RA, Kuhn AW, Bedi A. Platelet-rich plasma (PRP) in orthopedic sports medicine. Am J Orthop. 2016 Jul;45(5):290-326.
- ↑ Johns Hopkins Medicine. Platelet-Rich Plasma (PRP) Injections | Q&A. Available from: https://www.youtube.com/watch?v=NxW4dPcNRBM [last accessed 13/2/2022]