Pelvic Organ Prolapse Quantification (POP-Q) System
Original Editor - Jacintha McGahan
Top Contributors - Jacintha McGahan, Mila Andreew and Kim Jackson
Objective[edit | edit source]
The International Continence Society (ICS), the American Urogynecologic Society (AUGS) and the Society of Gynecologic Surgeons came to agreement in 1996, for a graded objective measure to be used in the assessment of female pelvic organ prolapse[1][2]. This system provides characterisation of a woman's prolapse and allows a uniform recording method to be used by clinicians that enables contrast and disclosure of findings[2]. This system was named the 'Pelvic Organ Prolapse Quantification (POP-Q) System' and is generally used in clinical setting [3]. POP-Q is the more routinely used staging system[4] seen in published research[4].
Intended Population[edit | edit source]
A woman may present in primary care with symptoms of a 'bulge' or 'heaviness' in her vagina with or without incontinence[1][5]. Other symptoms may include urge incontinence, sexual dysfunction, problems with voiding or defecation[1]. On visual inspection a prolapse may be observed but this patient group can also be asymptotic and are identified through other routine procedures, for instance a smear test[5]. A reduction in vaginal or uterine integrity is observed in up to 30-70%[6] of women presenting for usual gynaecology procedures with 3-6% of these women reporting a drop pass the vaginal opening[6].
Method of Use[edit | edit source]
Pre-examination[edit | edit source]
Foregoing the procedure ensure the patient has an empty bladder and if feasible an empty rectum[2]. A full bladder during this examination could risk undervaluing the POP-Q score and therefore, miscalculate the staging[7]. The patient is then positioned where the utmost magnitude of the prolapse is shown and can be confirmed by the patient[2]. Positions may include supine, standing or in a birthing chair at 45 degree angle[8]. A Sim's speculum can be used if needed to draw back the anterior and posterior vaginal walls during the examination. All methods and positions utilised during the examination should be documented so that they can be reproduced[2].
Measurement Parameters[edit | edit source]
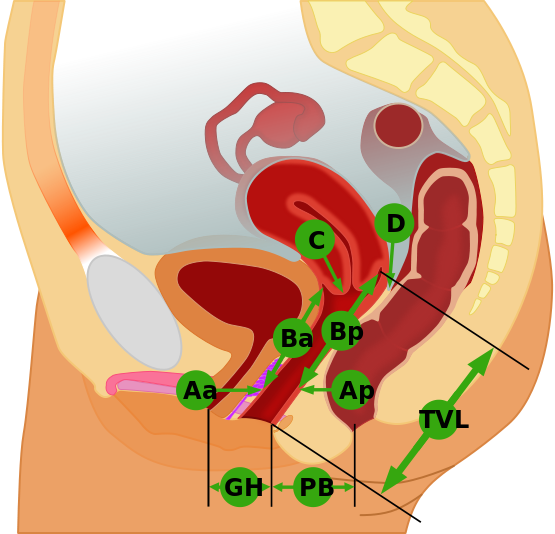
The measurement parameters are made up of six distinct locations (Aa, Ba, C, D, Ap, Bp) and three anatomical markers (GH, PB, TVL):
- Point Aa is at the midline of anterior vaginal wall. Where no prolapse is present this location is 3cm up from the hymen (merely interior to the vaginal opening). Parameters from the hymen can be -3cm indicating no anterior vaginal prolapse or +3cm, which is a full prolapse.
- Point Ba refers to the most superior location of the front vaginal wall . This location coexists with Aa (-3cm) in a woman with no anterior prolapse. However, in a woman with full prolapse this location coexists with point C.
- Point C is the lowest edge of the cervix or the vaginal cuff (i.e. hysterectomy scar). This location identifies if the cervix is descending.
- Point D is the topmost point of the posterior vaginal wall. This location can be contrasted with Point C to assess if the entry to the cervix has been extended.
- Point Ap is located midline of posterior vaginal wall 3cm proximal to hymen. The parameters for this point can range from -3cm to +3cm relative to hymen.
- Point Bp is the uppermost point of the posterior vaginal wall.
- GH is the 'Genital hiatus' that records the length from the urethral opening to the posterior vaginal opening/ hymen. The hiatus refers to the opening in puborectalis muscle, a component of the levator ani muscle group. A larger distance here may indicate laxity in this area.
- PB is the 'perineal body' and is recorded from the posterior aspect of hymen to the mid-anal opening. This will give an insight to the tonicity of superficial pelvic floor. Through vaginal birth the perineal body can be injuried via tears or by an episiotomy.
- TVL refers to 'total vaginal length' measured from hymen to the most distal point[2][9]. Knowing this allows the depth of prolapse to be assessed and reassessed post surgical repair.
Recording Measurements[edit | edit source]
The position of the six distinct locations are measured during a maximum Valsalva or cough with regard to the hymen (that is defined as 0cm). The only exception to this is the measurement of TVL, which is to be recorded at rest when the prolapse is decreased[2].
If a point drops to the hymen it measured as 0cm, if it stays higher than the hymen it is recorded as a negative and if it protrudes past the hymen it is recorded as a positive. All measurements are recorded in centimeters using a ruler or tape measure.
All measurements for each location are recorded on a grid as shown below;
| Anterior Wall (Aa) | Anterior Wall (Ba) | Cervix or cuff (C) |
|---|---|---|
| Genital hiatus (gh) | Perineal body (pb) | Total vaginal length (TVL) |
| Posterior Wall (Ap) | Posterior wall (Bp) | Posterior Fornix (D) |
Staging of Prolapse[edit | edit source]
Once all measurements have been made the stage of the prolapse can be identified in relation to hymen;
- Stage 0: No prolapse is observed (points Aa, Ba, C, D, Ap and Bp are all < / = -3cm).
- Stage 1: The most proximal portion of prolapse is greater than 1 cm above the level of the hymen (points Aa, Ba, C, D, Ap and Bp are all < -1cm).
- Stage 2: The most proximal portion of prolapse is found between 1 cm higher than hymen and 1cm beneath hymen (points Aa, Ba, C, D, Ap and Bp can set at -1cm and +1cm).
- Stage 3: The most distal part of the prolapse extends more than 1cm beneath the hymen but no further than 2 cm, resulting in no measurement larger than TVL (points Aa, Ba, C, D, Ap and Bp can be >/= +2cm and </= TVL -3cm).
- Stage 4: vaginal eversion has taken place or eversion to with 2cm of TVL (points Aa, Ba, C, D, Ap and Bp can be >/= to TVL -2cm)[1][2].
Evidence[edit | edit source]
Reliability[edit | edit source]
The POP-Q is a criterion and clearly defined inspection system that is verifiable, uses anatomical landmarks and is reproducible[10][12]. For this reason it is used in clinical research[8]. This system was the initial examination tool in it's field to be comprehensively tested and has attested to show high interobserver and intraobserver reliability[1] in four studies involving 240 participants[12].
Validity[edit | edit source]
NICE conducted an evidence review for examining pelvic organ prolapse, in which a physical exam and/or POP-Q was compared to index tests;
- Dynamic cystoproctography
- Barium suspension
- Pelvic floor ultrasound
- International Consultation on Incontinence Modular Questionnaire vaginal symptoms (ICIQ-VS)
- Standardised pelvic floor dysfunction questionnaire.
The evidence in this review showed that not any of the index tests attained 'the diagnostic accuracy of the POP-Q reference standard'[5] and recommends that the POP-Q is the examination of preference to assess women suspected of pelvic organ prolapse[5].
Technique Variables[edit | edit source]
It is important to note that patient position utilised during the POP-Q exam can affect the outcome. For instance a POP-Q exam performed with the patient in a birthing chair at a 45 degree angle will demonstrate a higher stage POP than a patient in supine. Additionally, the full extent of POP is better seen in standing, as a dissimilarity of up to 6cm between a standing and supine exam has been viewed[8].
It has been uncertain whether all the external locations, namely GH and PB, should be recorded at rest or during the patient straining. Testing revealed a marked rise in GH and PB measurements with Valsalva. This is queried to be related to a broadening of levator hiatus, with greater intraabdominal pressure[8]. As a result it is not clear if this broadening with strain is a natural occurrence or due to pelvic floor dysfunction. Therefore, it is advised to record both measurements for GH and PB at rest and with straining, to highlight all aspects of pelvic floor performance[8].
The POP-Q system should be conducted on a patient who has emptied their bladder beforehand. It is found that an empty bladder aids in magnifying a better representation of a prolapse in the six specific locations (Aa, Ba, C, D, Ap, and Bp). However, no influence is seen on GH, PB and TVL with an empty bladder[7].
Despite the POP-Q system being recommended as the reference standard[5], in clinical practice it is found to be time consuming (2-3 minutes in trained professionals) and requires skillfulness in it's application[12]. Associates of ICS and AUGS were surveyed and approximately on one-third of those taking part did not use the POP-Q system routinely in their clinical practice[13]. The main reasons for this is that the POP-Q is considered a complex system and not user friendly. This results in the system not being customary in it's clinical use by specialists globally[13]. A simplified version of the POP-Q has been devised, by The IUGA Standardization of Terminology Committee, to aid in addressing these issues for clinical use[14]. However, for research and urogynecologists, POP-Q will continue to be the benchmark[12].
Clinical Relevance[edit | edit source]
A pelvic organ prolapse is marked as symptomatic when the foremost border of the prolapse is level or past the level of the hymen (>/= stage 2 POP-Q)[2][15]. This needs to be considered when prescribing a patient's treatment. Physiotherapy aims to manage and maintain a stage 2. However, stage 3 and 4 require further assessment and treatment.
Genital hiatus (GH) measurement of >/= 3.75cm is correlated with and is prognostic of 'apical vaginal support loss'[16]. The GH measurement can check for and identify if further assessment of apical vaginal support is warranted prior planning other treatment such as a hysterectomy or POP repair surgery[16].
Links[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Persu C, Chapple CR, Cauni V, Gutue S, Geavlete P. Pelvic Organ Prolapse Quantification System (POP–Q)–a new era in pelvic prolapse staging. Journal of medicine and life. 2011 Feb 15;4(1):75.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 Madhu C, Swift S, Moloney‐Geany S, Drake MJ. How to use the Pelvic Organ Prolapse Quantification (POP‐Q) system?. Neurourology and Urodynamics. 2018 Aug;37(S6):S39-43.
- ↑ Muir TW, Stepp KJ, Barber MD. Adoption of the pelvic organ prolapse quantification system in peer-reviewed literature. American journal of obstetrics and gynecology. 2003 Dec 1;189(6):1632-5.
- ↑ 4.0 4.1 Boyd SS, O'Sullivan DM, Tulikangas P. 29: Implementation of the pelvic organ prolapse quantification system in peer-reviewed journals. American Journal of Obstetrics & Gynecology. 2017 Mar 1;216(3):S591.
- ↑ 5.0 5.1 5.2 5.3 5.4 Guidance NI. Urinary incontinence and pelvic organ prolapse in women: management:© NICE (2019) Urinary incontinence and pelvic organ prolapse in women: Management. BJU Int. 2019;123(5):777-803.
- ↑ 6.0 6.1 Barber MD. Pelvic organ prolapse. Bmj. 2016 Jul 20;354:i3853.
- ↑ 7.0 7.1 Reich A, Kohorst F, Kreienberg R, Flock F. Influence of bladder volume on pelvic organ prolapse quantification results. Gynecologic and obstetric investigation. 2010;70(2):82-6.
- ↑ 8.0 8.1 8.2 8.3 8.4 Visco AG, Wei JT, McClure LA, Handa VL, Nygaard IE. Effects of examination technique modifications on pelvic organ prolapse quantification (POP-Q) results. International Urogynecology Journal. 2003 Jun 1;14(2):136-40.
- ↑ Haylen BT, De Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J, Monga A, Petri E, Rizk DE, Sand PK, Schaer GN. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Neurourology and Urodynamics: Official Journal of the International Continence Society. 2010 Jan;29(1):4-20.
- ↑ 10.0 10.1 Bump RC, Mattiasson A, Bø K, Brubaker LP, DeLancey JO, Klarskov P, Shull BL, Smith AR. The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. American journal of obstetrics and gynecology. 1996 Jul 1;175(1):10-7.
- ↑ Dr Fiona Bach. POP-Q for the MRCOG by ACE Courses. Available from: https://www.youtube.com/watch?v=UyIzjiuUoAs [last accessed 17/09/2020]
- ↑ 12.0 12.1 12.2 12.3 Raizada N, Mittal P, Suri J, Puri A, Sharma V. Comparative Study to Evaluate the Intersystem Association and Reliability Between Standard Pelvic Organ Prolapse Quantification System and Simplified Pelvic Organ Prolapse Scoring System. The Journal of Obstetrics and Gynecology of India. 2014 Dec 1;64(6):421-4.
- ↑ 13.0 13.1 Auwad W, Freeman RM, Swift S. Is the pelvic organ prolapse quantification system (POPQ) being used? A survey of members of the International Continence Society (ICS) and the American Urogynecologic Society (AUGS). International Urogynecology Journal. 2004 Oct 1;15(5):324-7.
- ↑ Swift S, Morris S, McKinnie V, Freeman R, Petri E, Scotti RJ, Dwyer P. Validation of a simplified technique for using the POPQ pelvic organ prolapse classification system. International Urogynecology Journal. 2006 Nov 1;17(6):615-20.
- ↑ Swift SE, Tate SB, Nicholas J. Correlation of symptoms with degree of pelvic organ support in a general population of women: what is pelvic organ prolapse?. American journal of obstetrics and gynecology. 2003 Aug 1;189(2):372-7.
- ↑ 16.0 16.1 Lowder JL, Oliphant SS, Shepherd JP, Ghetti C, Sutkin G. Genital hiatus size is associated with and predictive of apical vaginal support loss. American journal of obstetrics and gynecology. 2016 Jun 1;214(6):718-e1.