Ovarian Cancer
Original Editors - Trisha Counce & Brandy Hirsch from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Brandy Hirsch, Trisha Counce, Lucinda hampton, Aminat Abolade, Vidya Acharya, WikiSysop, Kim Jackson, Elaine Lonnemann, Wendy Walker, Rishika Babburu and 127.0.0.1
Definition/Description[edit | edit source]
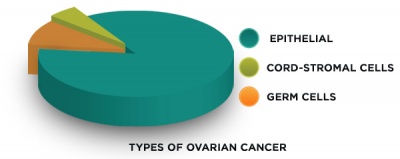
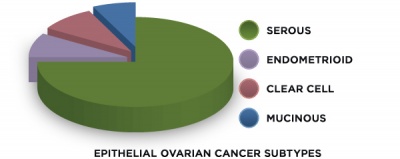
The term "ovarian cancer" encompasses several types of cancer that all arise from the cells of the ovaries in the female reproductive system.[1] Ovarian cancer commonly manifests as three different types including epithelial, germ cell, and cord-stromal cell. Epithelial ovarian cancer accounts for about 70% of all ovarian cancers, making it the most common type.[1] The four subtypes of epithelial ovarian cancer are serous, mucinous, clear cell, and endometrioid, with serous being the most common variety.[1] Ovarian cancer is believed to occur due to changes in cell DNA. Unfortunately, ovarian cancer often goes undiagnosed until advanced stages of the disease when it is hardest to identify the initial source.
The three main types of ovarian cancer are distinguished by the type of ovarian cells in which they originate:[2]
• Epithelial ovarian tumors are derived from the cells on the surface of the ovary or fallopian tube
• Germ cell ovarian tumors are derived from the cells that produce eggs
• Cord-stromal cell ovarian tumors are derived from the connective tissue within the ovary
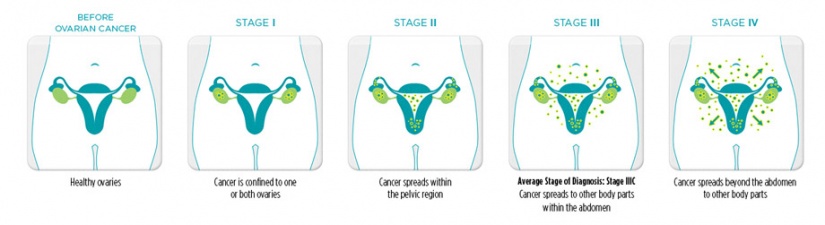
STAGES [2]
Stage I - Growth of the cancer is limited to the ovary or ovaries.
- Stage IA - Growth is limited to one ovary and the tumor is confined to the inside of the ovary. There is no cancer on the outer surface of the ovary. There are no ascites present containing malignant cells. The capsule is intact.
- Stage IB - Growth is limited to both ovaries without any tumor on their outer surfaces. There are no ascites present containing malignant cells. The capsule is intact.
- Stage IC - The tumor is classified as either Stage IA or IB and one or more of the following are present: (1) tumor is present on the outer surface of one or both ovaries; (2) the capsule has ruptured; and (3) there are ascites containing malignant cells or with positive peritoneal washings.
Stage II - Growth of the cancer involves one or both ovaries with pelvic extension.
- Stage IIA - The cancer has extended to and/or involves the uterus or the fallopian tubes, or both.
- Stage IIB - The cancer has extended to other pelvic organs.
- Stage IIC - The tumor is classified as either Stage IIA or IIB and one or more of the following are present: (1) tumor is present on the outer surface of one or both ovaries; (2) the capsule has ruptured; and (3) there are ascites containing malignant cells or with positive peritoneal washings.
Stage III - Growth of the cancer involves one or both ovaries, and one or both of the following are present: (1) the cancer has spread beyond the pelvis to the lining of the abdomen; and (2) the cancer has spread to lymph nodes. The tumor is limited to the true pelvis but with histologically proven malignant extension to the small bowel or omentum.
- Stage IIIA - During the staging operation, the practitioner can see cancer involving one or both of the ovaries, but no cancer is grossly visible in the abdomen and it has not spread to lymph nodes. However, when biopsies are checked under a microscope, very small deposits of cancer are found in the abdominal peritoneal surfaces.
- Stage IIIB - The tumor is in one or both ovaries, and deposits of cancer are present in the abdomen that are large enough for the surgeon to see but not exceeding 2 cm in diameter. The cancer has not spread to the lymph nodes.
- Stage IIIC - The tumor is in one or both ovaries, and one or both of the following is present: (1) the cancer has spread to lymph nodes; and/or (2) the deposits of cancer exceed 2 cm in diameter and are found in the abdomen.
Stage IV - This is the most advanced stage of ovarian cancer. Growth of the cancer involves one or both ovaries and distant metastases (spread of the cancer to organs located outside of the peritoneal cavity) have occurred. Finding ovarian cancer cells in pleural fluid (from the cavity which surrounds the lungs) is also evidence of stage IV disease.
Prevalence and Incidence
[edit | edit source]
Statistics [2]
- Over 22,000 new cases of ovarian cancer will be diagnosed this year
- Ovarian cancer will cause over 15,000 deaths this year
- In women age 35-74, ovarian cancer is the fifth leading cause of cancer-related deaths
- 1 woman in every 71 will develop ovarian cancer in her lifetime
- The 5-year survival rate is over 90% if treated in the earliest stages, however, only 19% of all cases are found at this stage
- If caught in stage III or higher, the survival rate can be as low as 30.6%
- Ovarian cancer is the leading cause of death from gynecological malignancies [3]
- 2nd most common reproductive cancer in women [3]
Risk of Recurrence:[4]
- Patients diagnosed in stage I have a 10 percent chance of recurrence.
- Patients diagnosed in stage II have a 30 percent chance of recurrence.
- Patients diagnosed in stage III have a 70 to 90 percent chance of recurrence.
- Patients diagnosed in stage IV have a 90 to 95 percent chance of recurrence.
Characteristics/Clinical Presentation[edit | edit source]
Epithelial ovarian cancer presents with a wide variety of vague and nonspecific symptoms.[5] Ovarian cancer may cause one or more of these signs and symptoms--
- Bloating, which is when the area below your stomach swells or feels full [5][6][7]
- Vaginal bleeding or discharge (not normal for individual) [6][5]
- Pain in the pelvic or abdominal area, abdominal distension or discomfort, abdominal mass [6][5]
- Back pain [6][7]
- Feeling full quickly while eating [6][5][7]
- Painful urinination or frequent urges, constipation, or diarrhea [6][7]
- Indigestion and acid reflux [5]
- Shortness of breath (SOB) [5]
- Weight Loss
- Persistent lack of energy [7]
Physical findings are uncommon in patients with early disease, but the more advanced the disease one may present with ovarian or pelvic mass, ascites, pleural effusion, or abdominal mass or bowel obstruction. [5] Pay attention to your body, and know what is normal for you. If you have vaginal bleedingand/or an abnormal menstral cycle that is not normal for you, see a physician right away. The key is early intervention so the earlier ovarian cancer is found and treated, the more likely treatment will be effective. [6]
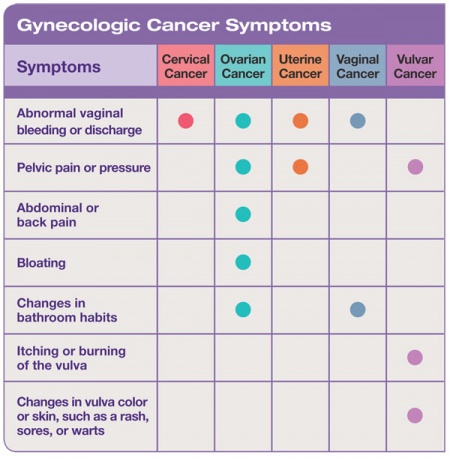
Below is chart outlining the symptoms of different gynecological cancers:
Associated Co-morbidities[edit | edit source]
Breast cancer
- Women who have had breast cancer also have a higher risk of developing ovarian cancer. The risk is even higher in women who have had breast cancer and also have a family history of breast cancer. [8]
Additional co-morbidities associated with ovarian cancer: [9]
- Hypertension
- Cerebrovascular Disease
- Osteoarthritis
- Infection
- Anemia
Medications
[edit | edit source]
Common Drugs & Drug Combinations Used in Chemotherapy [1]
- Carboplatin & Paclitaxel
- Cisplatin & Paclitaxel
- Bevacizumab
- Paclitaxel & Bevacizumab
If it is not the first time a patient has received chemotherapy, the type of drugs used are determined by how long it has been since the last time they took a drug containing platinum.[2] If it has been less than 6 months, the patient is termed platinum resistant. If it has been more than 6 months since the last day of platinum-based chemotherapy, then often a platinum-containing drug will be used again.[4]
In patients who are platinum resistant, a single drug is often used. Some of these include:[2][1]
Pegylated liposomal doxoruicin, Docetaxel, Paclitaxel, Topotecan, Gemcitabine, Etoposide, or Bevacizumab
Other Drugs Approved for Ovarian Cancer [1][2][4]
Adriamycin PFS
Adriamycin RDF
Carboplatin
Clafen
Cisplatin
Cyclophosphamide
Cytoxan
Doxorubic in Hydrochloride
Dox-SL
DOXIL
Doxorubicin Hydrochloride Liposome
Evacet
Gemcitabine Hydrochloride
Gemzar
Hycamtin
LipoDox
Neosar
Paclitaxel
Paraplat
Paraplatin
Platinol
Platinol-AQ
Taxol
Topotecan Hydrochloride
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
There are currently no reliable screening tools available to diagnose ovarian cancer. Annual pap smears will detect cervical cancer but NOT ovarian varieties. The current recommendations include an annual pelvic exam, transvaginal ultrasound, and CA-125 blood test.[10] These are the best options for screening but even in combination, results have been found to be unreliable.
Screening Tools [2]
- Pelvic Exam: Women age 18 and above should have a mandatory annual vaginal exam. Women age 35 and above should receive an annual rectovaginal exam (physician inserts fingers in the rectum and vagina simultaneously to feel for abnormal swelling and to detect tenderness).
- Transvaginal Ultrasound: This ultrasound, performed with a small instrument placed in the vagina, is appropriate especially for women at high risk for ovarian cancer or for those with an abnormal pelvic exam.
- CA-125 Test: This blood test determines if the level of CA-125, a protein produced by ovarian cancer cells, has increased in the blood of a woman at high risk for ovarian cancer or with an abnormal pelvic examination. Some non-cancerous diseases of the ovaries also increase the CA-125 levels, and some ovarian cancers may not produce enough CA-125 levels to cause a positive test.
It is also important to have a comprehensive family history taken by a physician who can identify risk factors associated with ovarian cancer since 5-10% of cases have a familial link.[2] If a women is considered to be at high risk for ovarian cancer, the following tool can also be used:
- Genetic testing: This testing identifies mutations in BRCA1 and BRCA2. Mutations in these proteins increased a womans risk of ovarian cancer greatly. About 1.4 percent of women in the general population will develop ovarian cancer sometime during their lives.[4] By contrast, approximately 39 percent of women who inherit a harmful BRCA1 mutation and 11 to 17 percent of women who inherit a harmful BRCA2 mutation will develop ovarian cancer by age 70 years.[4]
Positive Tests [10]
If any of these tests are positive, a woman should consult with a gynecologic oncologist who may conduct a CT scan and X-Rays and study the results. However, the only way to more accurately confirm ovarian cancer is with a biopsy, a procedure in which the doctor takes a sample of the tumor and examines it under a microscope.
Etiology/Causes[edit | edit source]
Typically cancer begins when healthy cells acquire a genetic mutation that turns normal cells into abnormal cells. Healthy cells grow and multiply at a set rate, eventually dying at a set time. Unlike normal, healthy cells, cancerous cells grow and multiply at an abnomally high rate, and they don't die-off when they should. These abnormal cells come together to form a mass or tumor. Cancer cells invade nearby tissues and can break off from an initial tumor to spread elsewhere in the body which is called metastasizing. [7]
There is no way to know for sure if you will get ovarian cancer because the causes remain unclear. [6][7] Most women get ovarian cancer without being at high risk. However, several factors may increase a woman’s risk for ovarian cancer, including the following:
- Middle-aged (50) or older [6]
- Close family members (such as your mother, sister, aunt, or grandmother) on either your mother's or your father's side, who have had ovarian cancer [6][7]
- Genetic mutation (abnormality) called BRCA1 or BRCA2, or one associated with Lynch syndrome [6][7]
- History of breast, uterine, colorectal (colon), or cervical cancer, or melanoma. [6]
- Eastern European (Ashkenazi) Jewish background [6]
- Never given birth or have had trouble getting pregnant [6][7]
- Diagnosed with endometriosis [6]
Although you may have one or more of the above risk factors, it does not mean you will get ovarian cancer. [6] Besides the above mentioned risk factors it is important to know certain facts as well:1) All women are at risk for ovarian cancer, 2) although vague, symptoms exist and increase over time, 3) early detection increases survival rate, 4) and a Pap test DOES NOT detect ovarian cancer. [2]Therefore, speaking with your physician about your risk is always in your best interest.
Systemic Involvement[edit | edit source]
Ovarian cancer can effect several different systems including the gastrointestinal, urogenital, cardiovascular, pulmonary, and musculoskeletal. Systemic issues that can occur with ovarian cancer consist of abdominal bloating, discomfort, pain, distension, indigestion, and acid reflux. Pelvic pain or discomfort, back pain, painful urination, constipation, and/or diarrhea are additional symptoms that may acovarian cancer. A sensation of shortness of breath can also occur which can be confused with a cardiopulmonary dysfunction. [6][7][5] In addition, it has been found that patients with ovarian cancer demonstrate an altered lipid metabolism. This condition may lead to a future epidemiological finding. [11]
Medical Management (current best evidence)
[edit | edit source]
There are three main treatment types for ovarian cancer:[2]
1) Surgery - Surgery to remove the cancerous growth is the most common method of diagnosis and therapy for ovarian cancer. It is best performed by a qualified gynecologic oncologist.
2) Chemotherapy - Chemotherapy is the treatment of cancer using chemicals (medications) that travel through the bloodstream to destroy cancer cells or stop them from growing both in and outside the ovaries. Chemotherapy is used in the majority of cases as a follow-up therapy to surgery.
- Intraperitoneal - medicine is placed directly into the peritoneal area through a surgically implanted port and catheter. New advances have combined it with intravenous (IV) therapy, using chemotherapy agents that work best for treating ovarian cancer. The National Cancer Institute recommends that, for select ovarian cancer patients, chemotherapy be given by both IV and IP. This combination has been found to increase survival for women with advanced stage ovarian cancer.[10]
- Neoadjuvant - a patient may receive chemotherapy before having surgery to remove their tumor.[10]
3) Radiation Therapy - Radiation therapy uses high-energy X-rays to kill cancer cells and shrink tumors (only rarely used in the treatment of ovarian cancer in the United States).
Side effects of Chemotherapy:[10]
- Hair loss
- Nausea & Vomiting
- Fatigue
- Diarrhea & Constipation
- Nerve Problems
- Mouth Issues
- Sexual & Intimacy Issues
- "Chemobrain"
Physical Therapy Management (current best evidence)[edit | edit source]
Although there are no specific physical therapy protocols for ovarian cancer, evidence supports the benefits of physical therapy in improving daily function, quality of life, and health in patients with cancer. As part of your cancer treatment, physical therapists can help you design an individualized exercise program. There are many reasons for being physically active during cancer treatment, but each person’s exercise program should be based on what is safe and what works best for them. It should also be something you like doing. Your exercise plan should take into account any exercise program you already follow, what you can do now, and any physical problems or limits you have. [12] These therapeutic exercises aim to reduce fatigue and optimize physical function, safety and well-being. [13]
An exercises regimen could include:
- Range-of-motion training with [14]
- Light resistance exercises [14]
- Cardiovascular activity [15]
- Flexibility exercises [15]
- Strength training [15]
Exercise, even minimal physical exertion, increases heart rate and muscle flexion while boosting your body’s tolerance to chemotherapy and radiation treatments. Participating in daily exercise programs will enable you to gain a sense of physical control over your condition, and will provide an outlet for stress and anxiety. In addition, exercise will instill you with the motivation and the drive for optimal wellness. [14]
Physical therapy also provides:
- Massage Therapy, which recent studies show can decrease stress, anxiety, depression, and pain, and increase alertness [15]
- Lymphedema Therapy
- Self-Care Managment to improve an individuals ability to return to their home
The American Cancer Society outlines the following for physical activity after cancer treatment. [8]
When you are recovering from cancer treatment
- Many side effects get better within a few weeks after cancer treatment ends, but some can last much longer or even emerge later. Most people are able to slowly increase exercise time and intensity.
- What may be a low- or moderate-intensity activity for a healthy person may seem like a high-intensity activity for some cancer survivors.
When you are living disease-free or with stable disease
- During this phase, physical activity is important to your overall health and quality of life. It may even help some people live longer. There’s some evidence that getting to and staying at a healthy weight, eating right, and being physically active may help reduce risk of second cancer as well as other serious chronic diseases. More research is needed to be sure about these possible benefits.
The American Cancer Society recommends that cancer survivors take these actions
- Take part in regular physical activity.
- Avoid inactivity and return to normal daily activities as soon as possible after diagnosis.
- Aim to exercise at least 150 minutes per week.
- Include strength training exercises at least 2 days per week.
A growing number of studies have looked at the impact of physical activity on cancer recurrence and long-term survival. Exercise has been shown to improve cardiovascular fitness, muscle strength, body composition, fatigue, anxiety, depression, self-esteem, happiness, and several quality of life factors in cancer survivors. At least 20 studies of people with breast, colorectal, prostate, and ovarian cancer have suggested that physically active cancer survivors have a lower risk of cancer recurrence and improved survival compared with those who are inactive. Randomized clinical trials are still needed to better define the impact of exercise on such outcomes.
Those who are overweight or obese after treatment should limit high-calorie foods and drinks, and increase physical activity to promote weight loss. Those who have been treated for digestive or lung cancers may be underweight. They may need to increase their body weight to a healthier range, but exercise and nutrition are still important. Both groups should emphasize vegetables, fruits, and whole grains. It’s well known that obesity is linked with a higher risk of developing some cancers. It’s also linked with breast cancer recurrence, and it might be related to the recurrence of other types of cancer, too. Exercise can help you get to and stay at a healthy weight.
Living with advanced cancer
- Some level of physical activity can improve quality of life for people with certain types of cancer, even if the disease is advanced (has spread to many places and/or is no longer responding to treatment). But this varies by cancer type, physical ability, health problems related to the cancer or cancer treatment, and other illnesses. The situation can also change quickly for a person with advanced cancer, and physical activity should be based on the person’s goals, abilities, and preferences.
Differential Diagnosis[edit | edit source]
Ovarian cancer presents with few diagnostic dilemmas yet it is commonly misdiagnosed as Extraovarian Primary Peritoneal Carcinoma (EOPPC) and adnexal masses (ovarian cysts). The differential diagnosis for these two diagnosis are extensive, with most masses representing benign processes. [3][5] EOPPC is an abdominal cancer without ovarian involvement. It mimics the signs and symptoms of ovarian cancer as well as the microscopic appearance and pattern of spread. Ovarian cysts are difficult to differentiate without histopathologic tissue diagnosis, a definitive diagnosis is generally precluded. Physicians must evaluate the likelihood of a pathologic process using clinical and radiologic information and balance the risk of surgical intervention for a benign versus malignant process. [5]
In addition, ovarian carcinoma will sometimes present first with a paraneoplastic syndrome such as polyarthritis syndrome, carpal tunnel, myopathy, plantar fasciitis, or palmar fasciitis (swelling, digital stiffness or contractures, palmar erythema). The condition may be misdiagnosed as chronic regional pain syndrome (CRPS), Dupuytren’s contracture, or a rheumatologic disorder. Hand and upper extremity manifestations often appear before the tumor is clinically evident. [3]
Additional Differential Diagnosis: [5]
Malignant gastric tumors
Anovulation
Appendiceal tumors
Appendicitis, Acute
Ascites
Benign lesions of the uterine corpus
Bladder distention/urinary retention
Borderline Ovarian Cancer
Cervicitis
Colon cancer
Embryologic remnants
Endometriosis
Gastric Cancer
Irritable Bowel Syndrome
Low-lying cecum
Metastatic gastrointestinal carcinoma
Ovarian torsion
Pancreatic Cancer
Pelvic abscess
Pelvic Inflammatory Disease
Pelvic kidney
Peritoneal Cancer
Peritoneal cyst
Rectal Cancer
Retroperitoneal mass
Urachal cyst
Urinary Tract Obstruction
Uterine Cancer
Uterine fibroids
Case Reports/ Case Studies[edit | edit source]
Physical Activity and Ovarian Cancer
Early Symptoms of Ovarian Cancer In Young Patients
Recreational Activity and Ovarian Cancer
Fertility Drugs and Ovarian Cancer
Resources
[edit | edit source]
Stages of Ovarian Cancer Video
National Ovarian Cancer Coalition Clinical Trials
Womens Health Website--Ovarian Cancer Fact Sheet
Social Media Support Group Healthheo
Ovarian Cancer National Alliance
Gilda Radner Familial Ovarian Cancer Registry
Daily Rx Website--Ovarian Cancer
More information about complementary and alternative treatments can be found in the Ovarian Cancer Guide to Quality of Life Issues and can be ordered by calling 1-888-OVARIAN (1-888-682-7426).
Recent Related Research (from Pubmed)
see tutorial on Adding PubMed Feed
Failed to load RSS feed from http://www.ncbi.nlm.nih.gov/entrez/eutils/erss.cgi?rss_guid=1HAC9OLsDE6OY4USvjAEKUKqCrQGbzf7lTXYS: Error parsing XML for RSS
References[edit | edit source]
see adding references tutorial.
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Green A. Ovarian Cancer (Cancer of the Ovaries). MedicineNet.com. http://www.medicinenet.com/ovarian_cancer/article.htm. Updated September 24, 2013. Accessed March 12, 2014.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 2.9 Medical Information. National Ovarian Cancer Coalition. http://ovarian.org/what_is_ovarian_cancer.php. Accessed March 12, 2014.
- ↑ 3.0 3.1 3.2 3.3 1. Goodman CC, Snyder TE. Differential Diagnosis for Physical Therapists, Screening for Referral. Saunders; 2012.
- ↑ 4.0 4.1 4.2 4.3 4.4 Ovarian Cancer. National Cancer Institute. http://www.cancer.gov/cancertopics/types/ovarian. Accessed March 12, 2014.
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 Green A. Ovarian Cancer. Medscape. http://emedicine.medscape.com/article/255771-overview#a0101. Published 1994-2014. Updated March 10, 2014. Accessed March 12, 2014.
- ↑ 6.00 6.01 6.02 6.03 6.04 6.05 6.06 6.07 6.08 6.09 6.10 6.11 6.12 6.13 6.14 6.15 6.16 Ovarian Cancer. Center for Disease Control and Prevention. http://www.cdc.gov/cancer/ovarian/index.htm. Updated June 17, 2013. Accessed March 12, 2014.</ref>
- ↑ 7.00 7.01 7.02 7.03 7.04 7.05 7.06 7.07 7.08 7.09 7.10 Mayo Clinic Staff. Diseases and Conditions Ovarian Cancer. http://www.mayoclinic.org/diseases-conditions/ovarian-cancer/basics/definition/con-20028096. Published 1998-2014. Updated November 10, 2012. Accessed March 12, 2014.
- ↑ 8.0 8.1 Ovarian Cancer Overview. American Cancer Society. http://www.cancer.org/acs/groups/cid/documents/webcontent/003070-pdf.pdf. Published 2013. Updated February 6, 2014. Accessed March 12, 2014.fckLRfckLRfckLRfckLR<span>Additional co-morbidities associated with ovarian cancer: <ref>Chia V, O'Malley C, Griffiths R, et al. Prevalence and incidence of comorbidities in elderly women with ovarian cancer. Gynecologic Oncology [serial online]. May 2013;129(2):346-352. Available from: MEDLINE, Ipswich, MA. Accessed March 12, 2014.
- ↑ Chia V, O'Malley C, Griffiths R, et al. Prevalence and incidence of comorbidities in elderly women with ovarian cancer. Gynecologic Oncology [serial online]. May 2013;129(2):346-352. Available from: MEDLINE, Ipswich, MA. Accessed March 12, 2014.
- ↑ 10.0 10.1 10.2 10.3 10.4 Ovarian Cancer Institute. http://ovariancancerinstitute.org. Published 2014. Accessed March 12, 2014.
- ↑ Gercel-Taylor C, Doering D, Kraemer F, Taylor D. Aberrations in normal systemic lipid metabolism in ovarian cancer patients.Gynecologic Oncology. January 1996;60(1):35-41. Available from: MEDLINE, Ipswich, MA. Accessed March 12, 2014.
- ↑ Physical Activity and the Cancer Patient. American Cancer Society. http://www.cancer.org/treatment/survivorshipduringandaftertreatment/stayingactive/physical-activity-and-the-cancer-patient. Published 2014. Updated February 6, 2013. Accessed March 12, 2014.
- ↑ Oncology Rehabilitation for Ovarian Cancer. Cancer Treatment Centers of America. http://www.cancercenter.com/ovarian-cancer/oncology-rehabilitation/. Published 2014. Accessed March 12, 2014.
- ↑ 14.0 14.1 14.2 Oncology Rehabilitation for Ovarian Cancer. Cancer Treatment Centers of America. http://www.cancercenter.com/ovarian-cancer/oncology-rehabilitation/. Published 2014. Accessed March 12, 2014.
- ↑ 15.0 15.1 15.2 15.3 Physical Therapy. Cancer Compass. http://www.cancercompass.com/cancer-treatment/physical-therapy.htm. Published 2014. Accessed March 12, 2014.